Abstract
Case report: A 10-year-old patient was referred by her orthodontist with agenesis of teeth 14, 13, 12, 22, 23, 24, 25, and 45 (N=8). Initial treatment started with transplantation of primary teeth 73 22, 83 12 and the premolar 35 24 to create a balanced number of premolars in all four quadrants. The primary tooth transplant was performed with the technique as described previously [1-3]. The dental arches in the upper and lower jaws were reformed and developed by the orthodontist. Eleven years later, the patient presented again aged 21 to replace the primary tooth transplants with endosseous implants.
Result: The transplanted primary teeth in position12 and 22 were in place for 11 years and helped to ensure good co-development of soft and bone tissue. The definite care of the patient with implants in positions 12 and 22 was performed without the need for extensive bone-augmenting measures. The premolar transplant in position 24 remained undisturbed in place. The bite-raising by the orthodontist in the meantime achieved an aesthetically pleasing result.
Conclusion: The combination of autogenous tooth transplants in childhood and endosseous implants in late adolescence yields reliable aesthetic and functional rehabilitation of patients with agenesis of multiple teeth. Early detection of these patients is crucial for this treatment option.
Keywords
Autogenous tooth transplant; Primary tooth transplant; Premolar transplant; Endosseous implant; agenesis; Two-phase transplantation concept
Introduction
Treatment of patients with agenesis of multiple teeth presents a major challenge to doctors working in implantology. Due to the lack of tooth eruption in multiple areas of the jaw, patients experience decreased jaw growth on both the vertical and sagittal planes with the well-known consequences of deep overbite and the associated physiognomic changes of the outer facial contours (dish face) [4].
A recently published systematic review for the treatment of patients with agenesis of multiple teeth (oligodontia) analyzed different treatment options (implant vs. transplant vs. leaving primary teeth vs. dentures) in terms of survival and success rates [5]. The authors found that, for patients under the age of 13, autogenous tooth transplantation and leaving primary teeth represents a reliable and above all costeffective way of treating young patients, with average survival rates of 94%. Furthermore, in patients over the age of 13 endosseous implantations is a reliable alternative therapy with average survival rates of 95%. Leaving primary teeth achieved average survival rates of 90% while providing conventional prosthetic measures had survival rates of only 60% [5].
This case report describes the clinical course of a 10-year-old patient, who was given definitive treatment using the technique of autogenous tooth transplantation in early mixed dentition as well as endosseous implants in late adolescence at the age of 21. It confirms that the combination of these two treatment options within an opportune treatment window can deliver very good results for the patient’s occlusal rehabilitation.
Case Report
A 10-year-old patient was referred to us by her orthodontist for consultation due to agenesis of eight teeth in total (Figure 1A-1C) with lack of three permanent teeth in quadrant I, of four permanent teeth in quadrant II, of one permanent tooth in quadrant IV, and no lack in quadrant III. Due to the patient being at a young age at the time of the appointment, primary teeth 73 and 83 were still present (Figure 1C). Due to the large number of missing teeth in the upper jaw (N=7), we decided upon the following orthodontic surgical concept, which included the following four key measures (Figure 2):
- First, the broad diastema in positions 11/21 should be closed by the orthodontist as quickly as possible to create space in positions 12 and 22 for the primary teeth transplants in the area of the agenesis.
- The ankylosed primary molars 55, 54, 64, 65, 75, 74, 84 and 85 in a significant infraposition should be removed to resolve their vertical growth-inhibiting effect.
- As part of the procedure, the lower primary canines 73 and 83 will be transplanted into space previously created in positions 12 and 22, where possible before they have been completely exfoliated naturally by the lower permanent canines erupting normally.
- In addition, the premolar 35 should be transplanted into position 24 as balancing transplant, so that all quadrants have at least one premolar.
After the closure of the diastema by the orthodontist, the surgical measures can begin promptly. Figures 3A and 3B show the clinical and radiological situation one week after surgery and suture removal. The flexible splinting of the transplants were performed with a TTS splint (titanium trauma splint, Medartis, Basel, Switzerland and composite, Ivoclar Vivadent, Schaan, Liechtenstein), which remained in situ for another six weeks. The primary tooth transplants were placed in the newly created tooth spaces in positions 12 and 22, while the premolar transplant was set in position 24 in slight infraocclusion due to an extensive lack of vertical bone growth (Figure 3B): The white arrow indicates the considerable vertical bone loss in positions 24 and 25, due to the infraposition of the ankylosed primary molars. The yellow arrows indicate the positions of the three transplants within the splint. Both primary tooth transplants in positions 12 and 22, as well as the premolar transplant in position 24, did not display any complications six weeks later when removing the splint (Figure 4). The teeth were fluoridated during regular aftercare and the patient was discharged into further orthodontic treatment. A recommendation was made to move the transplanted teeth no earlier than three months after the transplant with only half of the usually applied forces.
Results
The patient presented 1.5 years later under concomitant treatment by the orthodontist, now 11.5 years old, with normal and stable teeth (Figure 5A). Marked shortening of the root lengths can be seen in the post-OP orthopantomogram, indicating physiological exfoliation (Figure 5B). Obliteration of the pulp cavity is visible in all transplants. Significant vertical bone growth was seen in position 24 with the premolar transplant, now reaching the cement-enamel junction (white arrow). In addition, increasing apexification and similar to the primary tooth transplants-obliteration of the pulp cavity is detectable, which is believed to be a vital reaction in the healing process of transplants [6].
Figure 6 shows the patient 5.5 years later, now at the age of 17 years. Orthodontic treatment has advanced since then, with the aim of leveling the dental arches. The primary teeth are now in slight supra-position. No attempt to extrude the primary teeth was made by the orthodontist, in order to spare the patient from premature loss. The primary tooth transplants in positions 12 and 22 now show significant signs of apical resorption, meaning that, from a surgical perspective, implantology measures should be introduced immediately if the teeth are lost prematurely.
Another four years later, at the age of 21, the patient returned once her primary teeth transplants had become loose. The patient was thereafter promptly provided with implants. During the extraction of the loosened primary teeth, only minor alveoplastic measures had to be performed by filling of the extraction wounds with bone replacement material (Bio-Oss, Fa. Geistlich, Baden-Baden, Germany). The implants were inserted eight weeks later (2 × Nobel Active implants 3.0 × 11.5, Nobel Biocare Services AG, Zurich, Switzerland) and prosthetics were given another 2.5 months later. Figure 7 shows the clinical and X-ray situation following prosthetic care of the implants with all-ceramic crowns. Highly effective bite raising could be achieved (Figure 7A), associated with an aesthetically pleasing parodontal result in the area around the implants (Figure 7A and B). The OPG shows a stable crestal bone condition (Figure 7C). The remaining smaller gaps in positions 35 and 45 were not viewed to be problematic by the patient. Prosthetic measures in these gaps were advised upon request, as these gaps were too small for implants.
Discussion
This case of a patient with agenesis of seven teeth in total in the upper jaw and one agenesis in the lower jaw illustrates that satisfying clinical results can be achieved for patients in early mixed dentition with the methods of autogenous tooth transplantation and, in later adolescence, with the techniques of endosseous implantation. The methods underlying this treatment, which had already been used in combination in as early as 2006 [1], were confirmed in a recently published systematic review [5]. The authors concluded from their results that implants delivered very good survival rates overall, but not in the age group of children under the age of 13. In these cases, the autogenous transplantation of teeth and leaving primary teeth achieved better results in terms of survival and success. Conventional prosthetic measures, such as adhesive bridges or dentures, had lower survival and success rates than other treatment options. This case report therefore once more highlights how important the “time window” is in the success of treatment measures in patients with agenesis of multiple teeth. It was a happy coincidence that the then 10-year-old patient still had her lower primary canines available for autogenous transplants, thus allowing for the co-development of bone and soft tissue growth in the upper jaw.
Autogenous primary tooth transplantation is a method hardly reported in the literature. Scientifically substantiated data for success rates of autogenous primary tooth transplantation have since become available [3,7]. Based on our clinical experience and that of other working groups, the time window most important for jawbone development between 9 and 13 years of age can be successfully bridged using the technique of autogenous primary tooth transplantation as stable tooth replacement in the case of agenesis or traumatic loss of remaining upper incisors. Tschammler et al. provided quantitative evidence for the first time that autogenous primary tooth transplantation can achieve a significant increase in bone and soft tissue growth. The average five-year survival rate for the method was 87% [3]. In this case report, both primary tooth transplants were functionally in place for 11 years in total, until they had to be extracted selectively due to increasing looseness. To date, this represents the first description in the literature worldwide reporting such long survival times of primary tooth transplant. The aesthetically promising bite raising by the orthodontist as well as the subsequent successful implantation in positions 12 and 22 confirm that this is associated with the reliable bone formation in the agenesis area (Figure 7A-7C). It was not necessary to carry out major bone-augmenting measures during the implantation. The only technical challenge during implantation was the limited interdental space demanding for diameter-reduced implants.
Since first being described by Bjercke and Slagsvold some fifty years ago [8-10], premolar autotransplantation has become a long established technique with recorded ten-year survival rates of over 90% [11-14]. It has since become common knowledge that the method of autogenous tooth transplantation has favorable effects on the development of bone and soft tissue in the area of the transplant. This observation has recently been proven quantitatively [15]. In this case report, it is impressively documented that, after transplantation of premolar 35 into the agenesis position 24, where there was previously a primary molar in significant vertical infraposition (Figure 1C), a significant increase in bone height could be achieved. This vertical bone growth is clearly to be seen in figures 3B versus 5B: The vertical bone deficit has been completely resolved within 1.5 years following the premolar transplantation (Figure 5B, white arrow). The premolar transplant displayed a positive vitality probing 11 years after surgery. The obliteration of the pulp cavity may be interpreted as a vital reaction following the healing process (Figure 7C) [4]. Esthetics and function after the final insertion of endosseous implants as compared to the basic situation before treatment yielded a highly pleasing result (Figure 7A-7C).
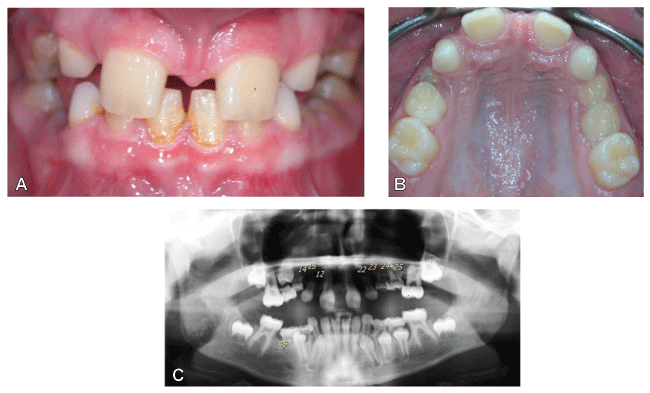
Figure 1: Intraoral clinical view of ten-year old girl at first sight.
A. Frontal view of both jaws in centric occlusion (clearly visible diastema and infrapositioned primary molars).
B. Occlusal view of teeth in the upper dental arch.
C. Orthopantomogram (agenesis of 14,13,12,22,23,24,25,45).
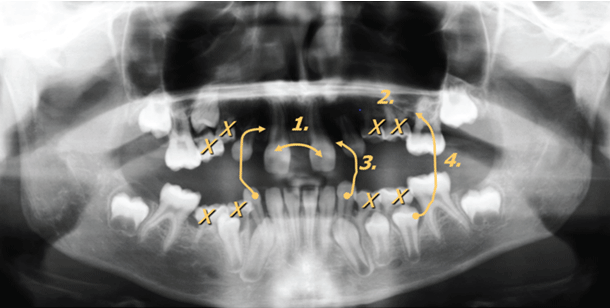
Figure 2: Orthodontic and surgical planning (for detail see text)
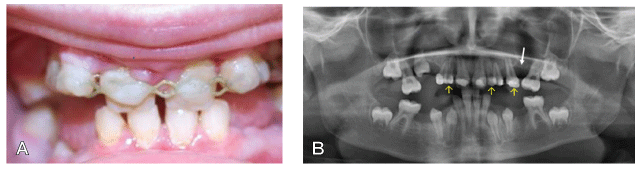
Figure 3: Clinical and radiographic situation after autotransplantation of 35 → 24, 73 → 22 and 83 → 12.
A. Clinical view one week after removal of stitches with titanium trauma splint still in situ which was left for another six weeks.
B. Post-OP orthopantomogram with transplant positions indicated by yellow marked arrows. White arrow indicates the initial vertical bony deficit in the area of the premolar transplant.
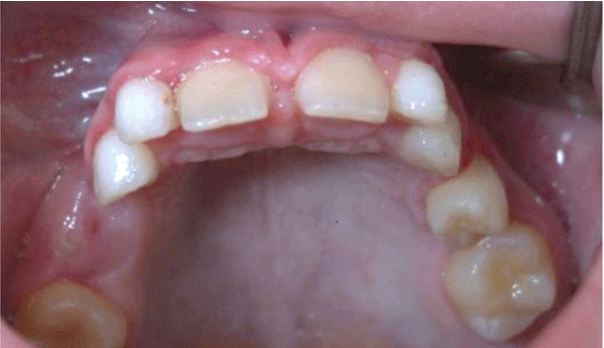
Figure 4: Clinical view six weeks after removal of titanium trauma splint. The three transplants in positons 12, 22 and 24 are found stable in situ without any gingival irritation.
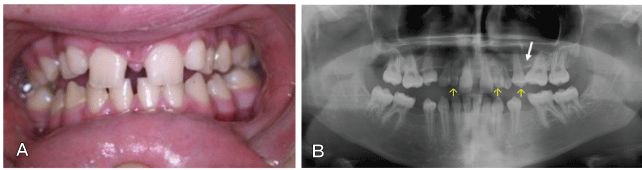
Figure 5: Clinical and X-ray findings 1.5 years after autotransplantation.
A. The bite has meanwhile been raised by the orthodontist, the diastema has slightly relapsed.
B. The transplanted primary teeth and the transplanted premolar are marked by the yellow arrows. In both primary tooth transplants apical resorption of root length is visible without inflammatory signs. Compared to the early post-OP X-ray examination (Figure 2), there is a significant increase in vertical bone height in region 24 (white arrow), now achieving the height of the non-transplanted healthy side.
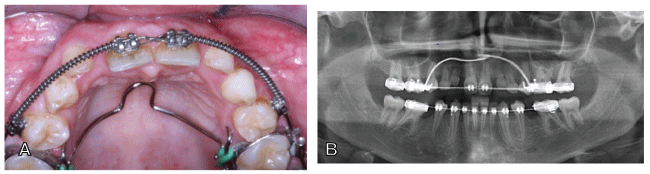
Figure 6: Clinical and X-ray findings 7 years post-OP.
A. Orthodontic alignment has continued in the meanwhile 17 years old girl. Transplanted and non-transplanted primary teeth in positons 13, 12 and 22, 23 were excluded from orthodontic therapy.
B. Progressive apical resorption of transplanted primary teeth is visible.
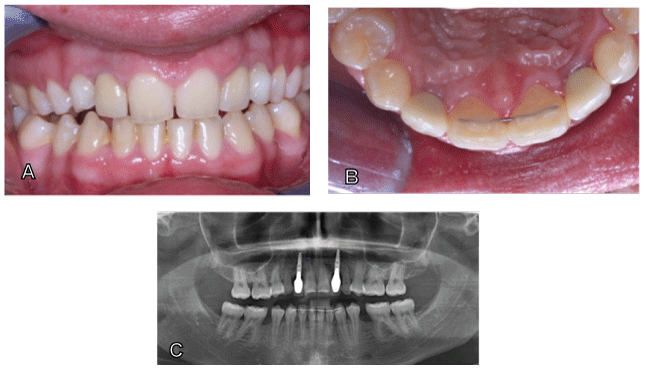
Figure 7: Clinical and X-ray findings 11 years post-OP in the meanwhile 21 year old patient.
A. Facial view
B. Occlusal view, both revealing a pleasing clinical situation after orthodontic bite raising.
C. Primary transplants have been removed and been replaced by endosseous implants without the necessity of elaborate bone augmentation procedures.
In light of this case report, the term “time window” is gaining an entirely new meaning for interdisciplinary cooperation between orthodontists, dentists, and maxillofacial surgeons. Primary tooth transplantation, which is only possible if primary teeth have not yet fully exfoliated, requires the patient to have primary teeth in situ as given in early mixed dentition. Thereafter, it is necessary to wait patiently for premolar transplantation due to the later eruption of the second dentition. We have addressed this issue of right timing with primary tooth transplantation in early mixed dentition (age 6-10) and premolar transplantation in late mixed dentition (age 10-14) under the term of the “two-phase transplantation concept” [16]. This concept was originally developed for traumatic tooth loss in children and adolescents. It allows children with traumatic loss of teeth in childhood (aged 6-10) to receive fixed prosthetic rehabilitation by means of a primary tooth transplant (phase I). The only alternative treatment options available at this age so far are prosthetic structures like removable dentures or adhesive bridges, representing often a significant psychosocial burden for the patients and their parents [17,18]. Patient satisfaction with both types of autotransplantation was excellent as assessed by questionnaires [3,15,19].
In the case of traumatic tooth loss after the age of 10, premolar transplantation is a long-established option for tooth replacement in young patients aged 10 to 16 in the late mixed dentition (phase II) [8- 14]. Whether or not the consecutive transplantation of primary teeth in phase I followed by premolar transplants in phase II should take place [16], crucially depends on the decision-making by and experience of the treating team of orthodontist, dentist and maxillofacial surgeon in close consultation with the patient’s parents. Ultimately, the decision as to whether to carry out premolar transplantation at the age of 12 to 14 or to permanently insert an implant later in life at the age of 18 at the earliest in the aesthetically challenging area of the upper front remains a challenging multidisciplinary task.
Summary
Children with agenesis of multiple teeth can be reliably treated with the techniques of autogenous tooth transplantation of both primary and secondary teeth and endosseous implantation. It is important that doctors know about the optimal timing for each type of autogenous tooth transplantation. Therefore, early interdisciplinary planning between orthodontist, dentist and maxillofacial surgeon is mandatory, as autogenous primary tooth transplantation can only take place prior to complete exfoliation of the deciduous teeth. Autogenous tooth transplantation reliably supports bone and soft tissue growth and therefore spares the children from wearing removable dentures, which is associated with a high acceptance by children and parents alike.
Article Information
Article Type: CASE REPORT
Citation: Nolte D, Braikeh S, Kurfurst B, Krause A, Linsenmann R (2018) Case Report: Multiple Tooth Agenesis-A Re-Update after 11 Years. Int J Dent Oral Health 4(4): dx.doi.org/10.16966/2378-7090.266
Copyright: © 2018 Nolte D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Received date: 22 Jun, 2018
Accepted date: 18 Jul, 2018
Published date: 25 Jul, 2018








