Abstract
Background: Packing a socket is a common practice to control hemostasis, promote healing and prevent complications after difficult tooth
extractions. Alvogyl is a paste composed of different substances. Active ingredients ensure antiseptic and analgesic effects, while the inactive
ingredient, the fern-derived Penghawar djambi fibers have styptic effects. It is claimed to be a resorbable and self-eliminating paste with little
complications.
Purpose: To investigate the occurrence and types of complications in postextraction nonhealing sockets after application of Alvogyl and to
determine if the fibrous component is resorbable and self-eliminating.
Methods: We performed a retrospective chart review over four years of 40 patients with a history of tooth extractions.
Results: We found seven patients with nonhealing sockets and a history of Alvogyl dental dressings. Some developed complications (alveolar
osteitis, abscess, sinus formation, bony erosion and gingivitis) that prevented subsequent tooth implants. Histologically, three cases showed
foreign body giant cell reactions with variably shaped membranous fibrous components that were initially confused as fungal hyphae or parasitic
ova.
Conclusion: Dentists and oral surgeons should be aware of these potential complications associated with Alvogyl and the fact that it is non
resorbable and not always a self-eliminating oral paste. Pathologists should also be aware of the histological appearances of this foreign material
to avoid a diagnostic pitfall and incorrect management since the history of dental dressings is not always provided.
Keywords
Alvogyl; Dental dressing; Tooth extraction; Nonhealing socket
Introduction
Dental extraction is a common procedure sometimes associated with
nonhealing dry sockets (alveolar osteitis (AO) and local complications.
Several different dental and oral medicaments are used to promote
healing in extraction sockets, treat dry sockets and prevent complications
[1-3]. Alvogyl is a well-known dental dressing that was first described
in the German literature in 1951[4,5]. The first detailed account of its
effects on the healing of extraction sockets was in 1979[6,7]. Although it
is claimed by the manufacturer to be a safe and efficient oral and dental
medicament, several studies demonstrated detrimental effects on the
healing of extracted sockets, aggravating dry sockets and encouraging
infections[6,8,9]. We report a case series of seven cases of postextraction
nonhealing sockets after application of Alvogyl. Three patients
demonstrated residual Alvogyl fibers with foreign body reaction and local
complications. Histologically, the foreign bodies were initially confused
with fungal hyphae and parasitic ova.
Materials and Methods
This descriptive histology-based case series review was approved by
the medical research committee in Rashid hospital. The patients’ medical
records were obtained and the histology specimens were retrieved. The
research has been conducted in full accordance with the World Medical
Association Declaration of Helsinki. We conducted a retrospective review
of 346 oral and dental histology specimens over four years from May 2011
to February 2015. The collected data was anonymized and de-identified
prior to analysis. Oral and dental specimens that were removed after
tooth extractions were collected. Patients with a history of extraction
sites that failed to heal or who developed complications, for example
dry sockets after tooth extractions were selected and included in the
study as cases. Patients with a history of uneventful recovery after tooth
extractions without complaints or complications were excluded from the
selected cases. A computer retrieval search was used to collect the oral
and dental specimens that were clinically labeled as nonhealing sockets,
dry sockets, postextraction complications and tooth extractions. The
history of the application of dental dressings and packing and their types
was retrieved from the patients’ files. The age and gender of each patient
was recorded. Clinical data regarding the clinical presentation, number
of extracted teeth, their location, the preoperative clinical impression,
as well as follow up data (when available) and any associated local oral
lesions or systematic diseases were collected. History of other previous
dental or oral surgical interventions or trauma was also explored. History
of smoking, alcohol drinking, diabetes mellitus and osteoporosis was
collected. Intake of oral contraceptive pills and postmenopausal status in
women was also recorded. Sections of 4-6 μm thickness were stained with
routine hematoxylin and eosin (H and E) stain for each collected case.
All of the H and E slides for each collected case were reviewed. Special
stains, for example periodic acid Schiff (PAS), PAS with diastase, Alcian
blue, Masson trichrome, von Kossa, Grocott methenamine (GMS) and
Prussian blue iron stain were performed for each case. The sections were
also examined under polarized light for the detection of any refractile
foreign materials.
Results
We found 40 patients who had a procedure for tooth extractions during
the study period. Seven patients developed nonhealing sockets and
persistent complaints after tooth extraction. The remaining 33 patients
had uneventful recovery. None of the 33 patients had a history of dental
packing or dressing. The seven patients who developed postextraction
complications had a history of application of different types of dental
dressings/materials including Alvogyl, amalgam and gutta percha (Table
1). The age range was between 23 and 50 with a mean age of 37 years. The
male to female ratio was 1.3:1. None had a history of previous trauma or
traumatic tooth extractions. Each patient had one extracted tooth, mostly
commonly a molar tooth of the upper jaw. The symptoms were mainly
pain, but some developed bleeding. Clinically, they presented as tender
nodules or lumps of variable sizes, but usually less than 2.0 cm. The clinical
impression was varied and included infection, abscess, granulation tissue
and cysts. Two cases were confused with neoplasms. All of the patients had
Alvogyl, one in combination with amalgam and another patient had gutta
percha points, as well. One patient (case 4) had her tooth extracted and
dressing placed abroad. Another patient (case 7) had his tooth extracted
in a private clinic. The remaining patients had their teeth extracted in
our institution. Three of the patients developed AO, one with abscess and
sinus formation and another one with bony erosion. Another patient had
gingivitis. The remaining three patients had no complications. All of the
patients had good oral hygiene, except one patient (case 2) who had a
poor oral condition with generalized gum recession. Two of the female
patients were married (case 1 and 4). They were being treated hormonally
and medically for infertility. One unmarried female patient (case 2)
was clinically suspected of intersex, but had not received medical or
hormonal treatment. She was sexually inactive and had no history of oral
contraceptive (OCP) intake. One patient (case 4) had a previous history of
tuberculosis with chronic sinusitis. Another patient (case 7) was medically
treated for recurrent deep vein thrombosis because of thrombophlebitis.
We lost follow up of two patients. The remaining patients had a follow
up that ranged from one year to three years. Two patients were not
suitable for tooth implants because of their oral conditions and local
complications. The patients without complications had successful tooth
implants. All of the female patients were non-smokers and did not drink
alcohol. None had OCPs intake, menopause or osteoporosis. The male
patients were smokers, but had no history of alcohol intake.
Histologically, the cases showed inflammation that varied from mild
nonspecific chronic inflammation to marked mixed inflammation with
abscess formation (Table 2). The fibrosis was generally mild. Most of the
cases showed calcifications that varied from micro calcifications to large
chunks of calcified materials. None had osteoid formation. Three cases
showed hemorrhage. None showed hemosiderin pigments deposition.
Three cases showed foreign bodies with variable intensity of foreign
body giant cell reaction. Four cases did not reveal foreign materials or
foreign body reaction. Three cases showed squamous epithelium that
was represented in the sections, two of which showed either perforated
or ulcerated hyperplastic inflamed epithelium. Cases 1, 4 and 6
showed similar foreign bodies composed of variably sized and shaped
membranous structures (Figures1 and 2). Some were elongated broad
walls, while others were smaller oval or round. Some were either partly or
completely calcified (Figure 1B). Foreign body type multinucleated giant
cells were seen adjacent to the walls of these structures or “inside” them
(Figure 1B). No eosinophils or neutrophils were seen in the vicinity of
these structures. We did not find epithelioid granulomas in the case with
a history of tuberculosis (case 4) or in the other cases. The walls of the
fibers were polarizing. Some showed septated walls arranged in vegetablelike
cell chambers. Some of these foreign materials were seen within an
abscess or perforating through the surface epithelium with transepithelial
elimination (Figure 2). These structures were positive for PAS and GMS
(Figure 3). Some sections showed calcified Schistosoma ova-like or
Trichuris ova-like structures (Figure 1B).
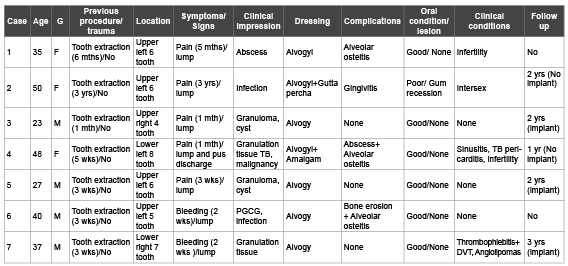
Table 1: The clinical features of the collected cases of non healing sockets after tooth extraction.
G: gender, F: female, mths: months, yrs: years, M: male, wks: weeks, TB: tuberculosis, PGCG: peripheral giant cell granuloma, DVT: deep vein
thrombosis.
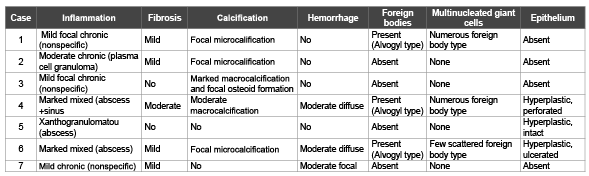
Table 2: The histological features of the collected cases.
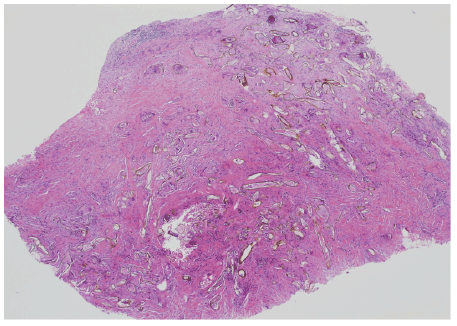
Figure 1: A) A fibrotic nodule studded with variably sized and shaped
yellow to golden elongated membranous broad hyphae-like structures.
Others were oval to round (hematoxlyin-eosin, original magnification
×20).
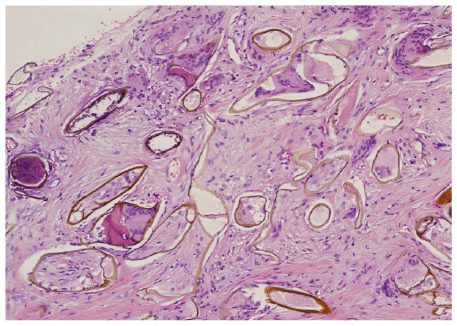
Figure 1: B) Multinucleated giant cells are seen partly engulfing the
structures; some giant cells are seen “inside” the walls of the elongated
membranous structures. Some of the structures were oval to round
and partly calcified thus resembling parasitic eggs. Not the absence of
eosinophils and neutrophils (H and E,×200).
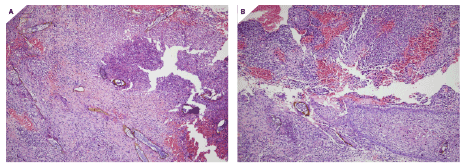
Figure 2:A) An abscess cavity filled with similar structures with scattered foreign type giant cells (H and E,×200).
B) An inflamed sinus tract with similar structures perforating through the squamous epithelium (H and E, ×200).
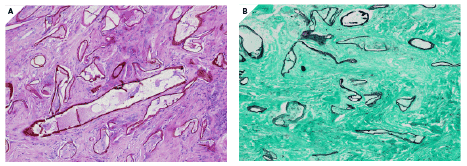
Figure 3: A) PAS special stain highlights the broad hypha-like walls, some with septae (H and E,×200).
B) GMS special stain is also positive and highlights the broad hypha-like walls (H and E, ×200).
Discussion
Alvogyl is an oral and dental dressing paste composed of various
ingredients and consists of a thick brown fibrous paste [10]. Active
ingredients include butamben, iodoform and eugenol that ensure
antiseptic and analgesic effects. Other inert ingredients include olive
oil, spearmint oil, sodium lauryl sulphate, calcium carbonate and water.
Of interest, is the fern-derived Penghawar djambi, a Malayan term for
the Fern indigenous in Indonesia. This fiber material is known to have
hemostasis styptic effects when applied to wounds and ulcers. The
dressing of extraction socket by Alvogyl is considered by some to be a
safe and effective management of dry sockets [3]. The product has been
available and used in clinical practice for a long period. It is used mainly
as a post extraction dressing in patients with a history of dry sockets and
traumatic extractions. However, there are no manufacturer instructions
of how long the paste remain in the socket since it is claimed to be selfeliminating
[10].
On the other hand, there have been reports of adverse side effects
associated with Alvogyl. A higher number of patients with infection of the
extraction sockets after application of Alvogyl have been reported [8,9].
In addition, serious complications can occur if the dressing remains in
place for a long period. One study demonstrated retarded wound healing
after application of Alvogyl compared to controls [6].This was found
within one to two weeks after extraction. Some authors claim that the
systematic application of Alvogyl after tooth extraction and treatment
of post extraction infection and complications should not be advocated
[6,11]. The treatment of non healing sockets after application of Alvogyl
is removal of the dressing, profuse irrigation of the socket, a course of
antibiotics and oral mouth wash. Some emphasized regular observation of
the healing process, as well [8]. There are many different ways of treating
dry sockets[3]. Some authors advise alternative approaches to promote
postextraction healing. Some recommend the use of broad spectrum
antibiotics supplemented with resorbable clot stabilizing substances[2].
Others endorse the use of chlorhexidine gel directly applied to the
socket[12]. Some authors have studied the use of bone graft, bioactive glass,
freeze dried gel and laser[13,14]. However, it seems there is no consensus
on the best option for treating complicated tooth extractions and AO[12].
If it is necessary to use Alvogyl or other applications, it is advisable to
regularly observe the healing process and remove any residual dressing
within days rather than weeks to ensure efficient spontaneous healing and
prevent foreign body reaction and further complications[8,9]. Several
local and systematic factors (smoking, trauma, OCPs) were found to
have negative effects on the healing process after tooth extraction[15-17].
Local factors include tooth site, traumatic extraction and multiple
extraction sites. Systematic factors might include old age, smoking, OCPs,
hypertension and diabetes mellitus. No gender differences were observed.
In this review, the patients who had Alvogyl dressings developed dry
sockets and further local complications that impeded their recovery and
future option for implants. This review suggests that possible contributory
detrimental factors could include hormonal disturbances, since two
of the patients with complications were being hormonally treated for
infertility. Our findings and other previous studies demonstrated that
the fern-derived fibers are clearly non-resorbable and not always selfeliminating.
Histologically, the large, broad and long Penghawar djambi
fibers could be confused by the unwary pathologists, particularly without
prior knowledge of a history of dental dressing, with the broad hyphae
of mucormycosis. Mucormycosis is a recognized complication in the oral
cavity in compromised patients. Hints to the correct recognition are the
presence of foreign bodies around and ‘inside” these structures, presence
of septa and absence of neutrophils around these structures. In addition,
the smaller calcified structures can mimic old calcified Schistosoma eggs.
Some noncalcified oval structures could resemble Trichuris ova. Clues
to avoid misinterpretation are the presence of foreign body reaction,
absence of eosinophils and absence of the lateral or terminal spines or
knobs. In addition, parasitic ova in the oral cavity are rare findings. Other
plant derived cellulose fibers were described in periapical lesions, cysts,
postendodontic granulomas and extraction sockets[18,19]. Pathologists
should be able to differentiate between these foreign bodies by morphology
and use of histochemical stains and polarizing microscopy. Knowledge of
a history of previous dental dressing should help.
In conclusion, Alvogyl related fibers are non-resorbable and not
always self-eliminating. If left for a long period, they may elicit a foreign
body giant cell reaction which can lead to further local complications.
Clinicians should be alert to the potential side effects of dental and oral
dressings, in particular those with non-resorbable materials. Without
a prior knowledge of a history of dental or oral dressings, pathologists
should be aware of the histomorphologic appearance of these fibers to
correctly recognize them and guide the dentists and oral surgeons to the
correct diagnosis and subsequent management.
Acknowledgment
We thank Mrs. Sybil De Costa, our department secretory, for her
assistance with papers formality and manuscript preparation and typing.
Financial and Funding Disclosure
The authors disclose no sources or grants of financial support from any
institution. No conflict of interests to be disclaimed or financial disclosure
to be declared by the authors.
Article Information
Article Type: Original Article
Citation: AbdullGaffar B, Alawadhi F, Gandour K
(2016) Alvogyl dental dressing: a potential cause of
complicated postextraction nonhealing sockets: a
clinicopathologic study of 7 cases. Int J Dent Oral
Health 2(4): doi http://dx.doi.org/10.16966/2378-7090.170
Copyright: © 2016 AbdullGaffar B, et al. This is
an open-access article distributed under the terms
of the Creative Commons Attribution License,
which permits unrestricted use, distribution, and
reproduction in any medium, provided the original
author and source are credited.
Publication history:
Received date: 29 Oct 2015
Accepted date: 07 Jan
2016
Published date: 12 Jan 2016







