Abstract
Aim: To demonstrate that stage 1 caries lesions in a moderate-to-high-risk young adult can be successfully remineralized with a customized protocol
Background: While some clinicians respond immediately to demineralized enamel with surgical procedures (e.g. sealants, microabrasion,
restorations), holistic or minimally invasive approaches preserve tooth structure while achieving remineralization of such lesions.
Case description: We report on the application of a tray-based protocol that prolongs contact between a multi-mineral NaF dentifrice and the
teeth of a young adult manifesting stage 1 caries lesions.
Conclusion: Instead of invoking procedures that generate tissue loss (no matter how minimal), reversible conditions of a moderate-to-highrisk
patient demonstrating stage 1 caries can be addressed via creative, minimally invasive approaches, such as delivery of a multi-mineral
dentifrice via mouth trays.
Clinical significance: The minimal interventional approach we used required patience and creativity, and produced remineralization of
incipient caries lesions in a moderate-to-high-risk patient. Importantly, this case study also demonstrates the importance of understanding the
psychology of the patient, acquiring a detailed history of habits, and devising a customized, preventive-focused protocol to match the patient’s
needs.
Introduction
Dental caries is a disease afflicting mankind since time immemorial
[1]. Considered a lifestyle disease, dental caries is not only caused by
an excessive intake of sugar-rich foodstuffs but also is related to the
environment of the oral cavity, including the number and type of bacteria,
salivary flow and buffer capacity, frequency of dietary exposures, age,
medical treatments, psychology, dental knowledge, and oral hygiene
habits [2]. Despite much research in the field of clinical and preventive
dentistry, dental caries continues, unabatedly, challenging us to think of
creative methods to prevent, manage and treat it.
Fluoride remains a clinically effective agent in preventive dentistry but
its efficacy can be limited in certain clinical scenarios, leading to frustration
of both the patient and the clinicians [2]. One method of improving
fluoride’s effect may be through supplementation with calcium phosphate
materials. Other techniques include devising formulations, such as
fluoride varnishes, that extend the contact time of fluoride with the tooth
surface and while some clinicians respond immediately to demineralized
enamel with surgical procedures (e.g. sealants, microabrasion, and
restorations), which may increase the risk of future complications (e.g.
secondary caries), holistic or minimally invasive approaches can preserve
tooth structure while achieving long-lasting remineralization.
In this Case Report, we report on a novel method of prolonging the
duration of a multi-mineral dentifrice on the tooth surface. This
method is designed to remineralize stage 1 caries lesions while also
improving periodontal health, and is therefore intended for moderateto-high-risk
caries individuals.
Case Report
A 16-year-old boy was brought to the dental office for a routine checkup
by his parents. Upon inspection, his maxillary anteriors showed breaks
in enamel and loss of tooth structure on the labial surface (Figure 1). The
dental caries lesions (as indicated with black arrows) were excavated and
the four teeth manifesting irreversible damage were restored with Ketac®
N100, a resin glass ionomer having good esthetics and the ability to attain
a high polish. Despite instructions and requests, the patient however
never came back for a follow-up appointment.
Four years later, the patient returned for a routine prophylaxis. All
four restorations appeared clinically sound (maxillary anteriors in
Figure 2), plaque control was reinforced and a basic prophylaxis was
performed. Noticeably, the mandibular anteriors showed white chalky
demineralized enamel on the labial surface (mandibular anteriors
in Figure 2). The demineralization had not yet progressed to dentin
and as such we recommended topical fluoride application to help
remineralize the affected enamel.
Fluoride varnish (3M Clinpro® White Varnish with 5% NaF plus
TCP) was applied as per the manufacturer’s instructions on day one to
the maxillary and mandibular teeth (Figure 3). Patient was instructed
to brush lightly on the teeth, as vigorous brushing could remove the soft
white chalky enamel. He was asked to return to the dental clinic every
week for an assessment of his oral hygiene and to monitor the status of
the white chalky lesion. Unlike the experience four years ago, the patient
returned each week as instructed.
After a month, however, there was no improvement in the lesions on
the mandibular anteriors (Figure 4). In attempting to identify factors
contributing to the resistance of remineralization, it was realized that the
patient’s personal habits history had not been recorded; when asked about
his habits, he reported that he was a smoker.
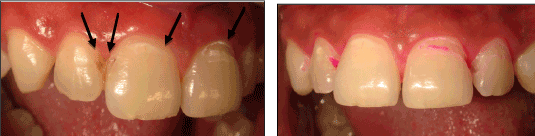
Figure 1: Baseline photos of the 16-year-old patient’s upper anterior
teeth demonstrating presence of enamel breaks and/or loss of tooth
structure. Photo on left is off-center to demonstrate location of the four
restorations (denoted with black arrows). Breaks in the enamel are further
resolved with the caries detector purple dye, as shown in the right-hand
photo. All four teeth were restored with a Resin Modified glass-ionomer.
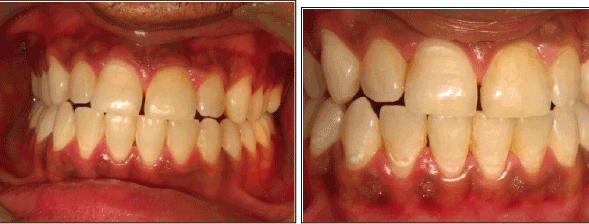
Figure 2: Panoramic and close-up views of the upper and lower anterior
teeth four years later (patient was 20 years old). The four restorations
were in sound condition, but the lower anteriors manifested stage 1
caries lesions accompanied with irritated gingival tissue.
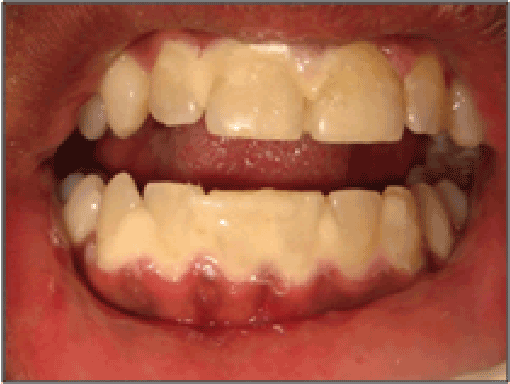
Figure 3: View of the anteriors after a fluoride varnish treatment.
Treatment
Given the prevalence of demineralization on the mandibular anteriors,
an opportunity presented to devise a protocol that increased the level of
preventive therapy as discussed below.
Alginate impressions of the maxillary and mandibular arches were
taken, and using the vacuum former, silicon trays were prepared. These
trays were used as carriers for the Clinpro® Tooth Crème. A pea-sized
amount of Tooth Crème was dispensed and spread in each tray and then
positioned on the teeth (Figure 5). The patient was instructed to brush his
teeth after dinner and then wear the tray for 15 minutes while maintaining
reasonable pressure to ensure the dentifrice contacted the tooth surfaces.
If any dentifrice managed to spill over into his mouth from the tray, he was
instructed to spit it out. After 15 minutes he was asked to remove the tray,
expectorate any residual paste and not to rinse his mouth. The patient was
supplied a tube of Clinpro® Tooth Crème and the silicon mouth trays for
take-home use, and was instructed to perform the tray-based procedure
before bedtime every night until the assigned toothpaste was exhausted.
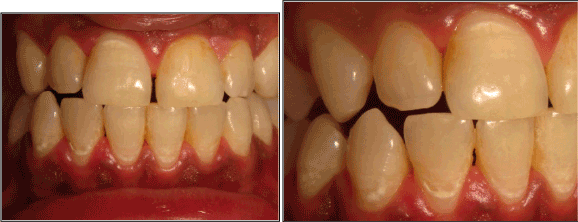
Figure 4: Panoramic and close-up views of the anterior teeth one month
after the fluoride varnish treatment. Notice the presence of enamel
lesions along the lower anteriors.
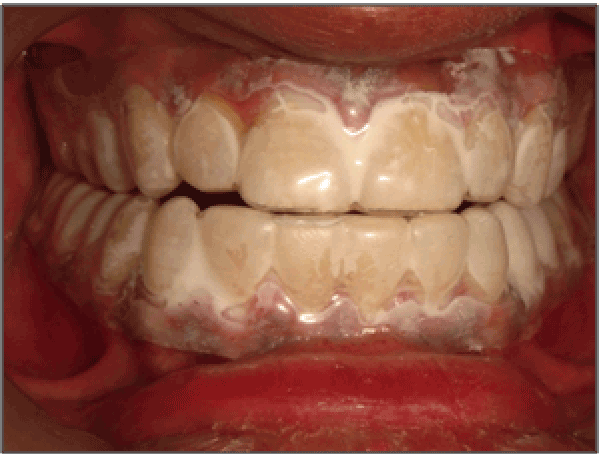
Figure 5: Appearance of the teeth fitted with a silicon-based mouth tray
with a pea-sized amount of Tooth Crème applied to the upper and lower
tray and positioned on the teeth. The patient was instructed to brush his
teeth after dinner with the Clinpro® dentifrice, followed by placement of
the tray for 15 minutes.
Additionally, the patient was asked to cease smoking and return for
a follow-up visit. Unfortunately, the patient could not maintain the
scheduled appointment because he had plans to leave the country for the
purpose of attending university.
The patient returned after 22 months for a prophylaxis and follow-up
appointment. The patient had accumulated heavy plaque build-up on the
teeth (Figure 6), and this was gently removed to reduce the potential for
damage to possible underlying soft, chalky enamel. Afterwards, the teeth
were dried with air and inspected for regions exhibiting demineralization.
Noticeably, all mandibular anteriors previously manifesting white-spot
lesions had remineralized, with light scar tissue being visible (Figure 7).
Discussion
The design of any preventive protocol must consider the patient’s habits,
drug use (over-the-counter, prescription and recreational, if possible),
medical conditions or psychology, as these are some of the causative
factors that can tilt the equilibrium (including the nature of the oral
biofilms) of the mouth from a healthy to a pathogenic environment [3]. A
16 year old young man having dental caries on the labial surface of upper
anteriors is somewhat unusual among the many patients seen and treated
at our three Thaper Dental Clinics, and was considered to be at higher
risk for dental caries. We comment that a favorable mindset is critical to a
patient’s outlook and compliance not only with their oral health but also
to their overall health. The 16-year-old patient begrudgingly came to our
clinic at the insistence of his mother. He had matured during the four year
time period, allowing him to take full responsibility for his own dental
health, without the insistence of his mother.
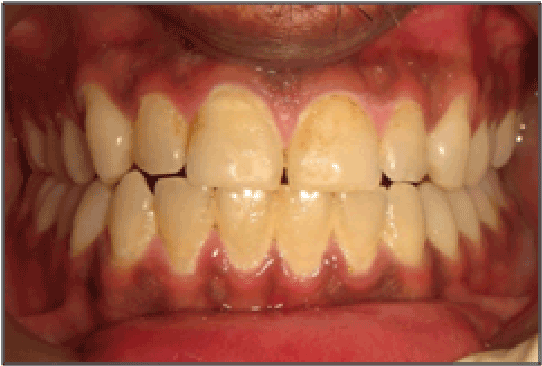
Figure 6: Appearance of the anterior teeth 22 months since the patient’s
last visit. The teeth manifested heavy plaque accumulations.
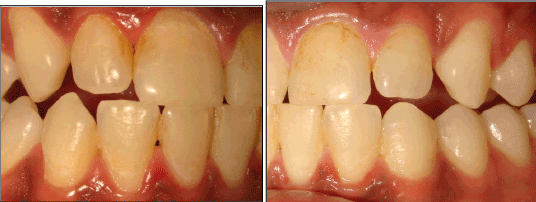
Figure 7: Close-up of anterior teeth on each side after gentle removal of
plaque and air-drying the teeth. The previously hypomineralized regions
on the lower anterior teeth have remineralized, the teeth are in stable
condition and the gingival tissue appears healthy Presence of scar tissue
inherent to remineralization processes is visible on some of the teeth.
At the patient’s first visit, it was necessary to immediately restore specific
lesions in the mouth and this was performed with the fluoride-recharging
and fluoride-releasing glass-ionomer in order to provide protection to
the adjoining surface and the neighboring teeth. However, a number of
tooth surfaces, especially the mandibular anteriors, exhibited significant
decalcification, that were not yet too soft to break, posed concerns for lesion
progression and aesthetic concerns. There are several clinical approaches
to addressing these decalcifications. One approach may include limited
surface etching followed by the application of either a sealant to the lesion
surface or lesion-infiltration with resins [4]. Microabrasion techniques can
be clinically effective in addressing hypocalcification [5]. But for clinicians
opting for less invasive intervention without acid pre-treatments, topical
applications of mineralizing therapies may be appealing. For example,
fluoride varnishes are recommended as a clinically effective cariesinhibition
measure, especially for children with developing dentition [6].
In this particular case, treatment with a fluoride varnish treatment
failed to provide sufficient remineralization of hypomineralized enamel
after a one-month period. The use of Clinpro® fluoride varnish was chosen
based on its inclusion of functionalized tricalcium phosphate (fTCP) and
its demonstrated clinical efficacy [7-9]. However, it became clear that
application of a single fluoride varnish treatment to complement the
patient’s oral care regimen was not sufficient in remineralizing the lesions.
This demonstrates the limitations of topical fluorides, including fluoride
varnishes, in certain instances [2]. Additionally, poor remineralization
may be related to the patient’s habit of smoking, which has been shown
to reduce saliva flow as well as increase the accumulation of periodontal
pathogens [10,11].
Maintaining the perspective that minimally invasive interventions is
key, a more intense level of therapy was devised that utilized tray-based
delivery of Clinpro® Tooth Crème, a low-abrasive dentifrice that contains
sodium fluoride (950 ppm F-) and fTCP. The purpose of fTCP is to
support fluoride-based remineralization and deliver functional forms of
bioavailable calcium and phosphate that help incorporate fluoride deeper
into enamel; in doing so, acid-resistant, enamel-like remineralization
is achieved not only at the tooth surface but also within the subsurface
lesions [7]. Although the dentifrice is formally designed to deliver fluoride,
calcium and phosphate in a toothbrushing event, we have adapted its
remineralizing capability by delivering these mineralizing ions via a traybased
application. The use of the custom mouth-tray extends the contact
time of these minerals with the demineralized enamel, and subsequently
works with the patient’s saliva to generate improved remineralization
as shown in Figure 7. The extended contact time allows fluoride to
exert a response on both the enamel and the gingival tissue, thereby
strengthening the enamel (in conjunction with calcium and phosphate)
while limiting the activity of microbial pathogens. As salivary flow and
clearance becomes minimal at nighttime, an environment rich in fluoride,
calcium and phosphate accomplished via the tray-based treatment helps
to prolong the dental benefits beyond the 15-minute application period.
When the demineralized regions remineralize with the aid of fluoride,
less-soluble mineral layers are formed, resulting in improved stability
against acid attacks. This helped to explain the observation that when the
patient returned after 22 months he was without caries. Furthermore, the
demineralized regions had sufficiently healed, with the natural formation
of scar tissue that developed during the remineralization process. Such
scar tissue is a component of the healthy tooth structure and has only
cosmetic importance for some patients.
We note the success of this technique is dependent upon the patient’s
compliance. Importantly, instead of using a multi-step treatment plan, the
dentifrice comprising both fluoride and fTCP in this single-step procedure
was critical to maintaining an easy-to-use regimen for the patient. It
appears the patient’s use of the dentifrice-tray combination for six months
achieved the desired remineralization; subsequent use of standard
toothpaste was sufficient to maintain the achieved remineralization of
the hypomineralized lesions. Also, this technique may find application in
reducing dental hypersensitivity from localized exposed root surfaces, or
from generalized post-bleaching tooth sensitivity. Finally, the technique
can also be used to improve gingival health.
Clinicians utilizing preventive approaches to manage reversible oral
health conditions must be confident that prevention therapy is effective
and that remineralization can be achieved. A major key to implementing
a preventive-based approach is the customized treatment protocol for the
need of the patient: the higher the decay-risk, the more aggressive and/
or creative prevention-focused protocol might be required. As always,
the patient’s desire to care for his/her own oral health and maintain
compliance to a recommended regimen is critical to the success of a
treatment plan. As clinicians, we need to remain open to increasing or
decreasing the level of prevention as per the patient’s progress. Through
judicious and intelligent adaptation of the tools available to both the
clinicians and the patients, we can effectively address reversible oral health
conditions that might otherwise develop into future decay problems (e.g.
secondary caries).
Conclusion
Instead of utilizing procedures that may result in tissue loss (no
matter how minimal), reversible conditions in moderate-to-high-risk
patients can be addressed via creative approaches, such as delivery of a
multi-mineral dentifrice via mouth trays. The simplicity of a dentifrice
comprising fluoride, calcium and phosphate helps to enable a creative,
straightforward and effective remineralization protocol for a moderateto-high-risk
patient with initial caries lesions.
Clinical Relevance
Minimally invasive approaches for reversible oral health conditions can
be successful but require a commitment from the patient and clinician.
Even though such approaches likely involve patience and creativity, the
successful remineralization of initial caries lesions of this patient is an
example of the importance of understanding the psychology of the patient,
acquiring a detailed history of habits, and devising custom, preventivefocused
protocols to fit the patient.
Article Information
Aritcle Type: Case Report
Citation: Thaper R, Karlinsey RL (2015) Clinical
Observations on the Remineralization of Stage
1 Enamel Caries Lesions Using a Tray-Based
Protocol: A Case Report. Int Dent Oral Health 2(1):
doi http://dx.doi.org/10.16966/2378-7090.151
Copyright: © 2015 Thaper R, et al. This is an
open-access article distributed under the terms
of the Creative Commons Attribution License,
which permits unrestricted use, distribution, and
reproduction in any medium, provided the original
author and source are credited.
Publication history:
Received date: 28 July 2015
Accepted date: 31
October 2015
Published date: 3 Nov 2015








