
Figure 1: Bioresorbable screws and plates pre-sterilized and made of polylactic acid, poly glycolic acid and poly dioxanone polymers.

Vijayendra Kumar1 Shreya Gour2 Robin K Chaube1 Rohit K Chaube1 Meenakshi Tiwari3 Shail K Chaube3*
1Department of Oral and Maxillofacial Surgery, Rama Dental College Hospital and Research Centre, Kanpur, Uttar Pradesh, India*Corresponding author: Shail K Chaube, Cell Physiology Laboratory, Department of Zoology, Institute of Science, Banaras Hindu University, Varanasi, Uttar Pradesh, India, Tel: 91-542-26702516; Fax: 91-542-2368174; E-mail: shailchaubey@gmail.com
Majority of bioresorbable plates used today are produced from synthetic semicrystailine poly-4 and its co-polymers. Though the bioresorbable plates have been extensively used in orthognathic surgery and midface trauma, the reports for their use in the mandibular fracture treatment are limited. Present study was aimed to compare the efficacy of bioresorbable plates with titanium miniplates for the treatment of mandibular fractures. For this purpose, 60 cases of fracture mandible were selected, out of which 30 were treated with bioresorbable plates and other 30 with titanium miniplates. Follow up was done after 2, 4, 8, 12 weeks and then every after 6 months. The patients were checked for pain, oedema, infection, occlusal derangement, suture dehiscence, paraesthesia, anesthesia, plate rejection, malunion, non-union and palpability of plate. Data suggest that the bioresorbable plates are easily adapted and reduction of fracture segments was better than titanium miniplates. But it is weaker than the titanium plates and resulted in cases of screw breakage, loosening of screw and decreased primary stability of the fracture segments, thus requiring longer period of IMF. The bioresorbable plates exhibit negligible complications and good handling properties. However, high cost of the material is the greatest deterrent for its wider use in treatment of mandibular fractures. On the other hand, titanium plates have shown better stability of fractured fragments.
Bioresorbable plates; Intermaxillary fixation; Mandibular fractures;
Over the past three decades, there has been extensive development of techniques used in the management of craniomaxillofacial trauma. The most significant advancement related to the management of fractures of mandible is the use of metal plates and screws [1]. These advancements are based on specific technical refinement in the rigid internal fixation methods [2]. The field of oral and maxillofacial surgery had undergone a sea of change from the closed reduction of facial fractures to the non-rigid fixation using metallic wires [3], lag screws [4]. These changes were further replaced by rigid fixation devices using dynamic compression (DCP) and eccentric dynamic compression plates (EDCP) [5]. The evolution of mini plate osteosynthesis had revolutionized the management of facial injuries and had proved to be the right alternative to DCP and EDCP. The metallic mini plates and screws currently in use for cranio maxillofacial fracture, although provide rigid internal bone fixation but have few drawbacks: (1) Once osteosynthesis is achieved, they are no longer needed and they may act as foreign body and create problems in future due to stress-shielding effect [6], (2) they may cause under-lying bone atrophy, [6] (3) interfere with computed tomography (CT) and magnetic resonance imaging (MRI) [7], (4) palpability [8], (5) sensitivity to the extremes of temperature of any oral-intake [8], (6) sometimes exposure of the plate requires removal and second surgery [6] and (7) Growth retardation and intracranial migration have also been documented with metal plates [9].
The quest to overcome the drawbacks of metal plates, researchers tried to develop the resorbable plates [10]. The interest to this increased in 1980s when use of these materials in fixation of the mandibular osteotomy [11] and fracture [12] was proposed and performed using polydioxanone-PDS screws and pins. The majority of bioresorbable plates used today are produced from synthetic semicrystailine poly-4 (alfa-hydroxy acid) and its co-polymers [13]. Though the bioresorbable plates have been extensively used in orthognathic surgery and midface trauma, the reports for their use in the mandibular fracture treatment are limited and few randomized controlled trials are available [14-16]. The use of resorbable plates in mandibular fracture treatment appears very exciting as the subsequent hydrolysis of the plates would mean no extra hardware in the facial skeleton. The better evaluation of fracture healing as PLLA plates are radiolucent and would obviate the need for second surgery at a later date [10]. Therefore, present study was aimed to use the PLLA plates as well as titanium plates in a randomized controlled trial setting to achieve the primary end point of bony union. The aim of internal fixation of traumatic and iatrogenic skeletal fracture is to achieve undisturbed fracture healing. The need for plates and screws for fixation is only temporary, until the fracture has been united.
A prospective randomized clinical study was conducted to compare the efficacy of resorbable fixation with titanium miniplate fixation in fracture of mandible. For this purpose, 60 patients who sustained fracture of mandible were selected. These patients reported at the Oral and Maxillofacial Surgery Department of our Hospital during November 2013 to August 2016. The inclusion criteria were oblique fractures and straight fractures present on one or both cortex of mandible, fractures of the symphysis, parasymphysis, body or angle region associated or unassociated with subcondylar fractures and patients with mandibular fracture who opted to have unrestricted jaw movements. The exclusion criteria were refused consent, pediatric patients, patients with associated midface fractures, patients with major systemic diseases. The 54 patients were male and only 6 cases of female patient were included. All patients were informed about the study and their consent was taken to use their information and records for this study, for ethical guidelines fulfillment.
A detailed history of each patient was carefully recorded and a thorough extra-oral as well as intra-oral examination of each patient in good light and exposure was done at the time of reporting to the department of oral and maxillofacial surgery. Radiographic assessment was carried out in regards to the site, direction of the fracture line and extent of displacement. Preoperative enrich arch bar or ivy loops were placed in maxillary and mandibular arches and elastic traction or wires were applied to bring fracture ends in reduced position and for inter maxillary stabilization.
Patients were operated either under general anesthesia or local anesthesia under strict aseptic conditions. Local anesthesia with adrenaline was infiltrated at the site of incision and a 1 to 1.5 cm Risdon’s incision was placed with 15 no. bard parker (BP) blade and layer wise dissection was done to expose the fractured segments, which was then reduced and firmly maintained in proper position. The plates and screws (Figure 1) were gamma sterilized and supplied in sterile double packing (INION INC, Weston FL, USA). The plates were activated in the water bath after which they remain contour able at room temperature for few minutes. Plate contouring and adaptation were carried out with digital pressure. Once the plate was adapted across the fracture line a screw hole was created by using appropriate drill with constant irrigation. Then screw threads were tapped manually (Figure 2). Once it reached the full depth and resistance was felt, tapping was stopped and gently the tap unscrewed. The tapped holes were irrigated to remove any bone chips and debris and plates were stabilized with minimum of two screws on either side of fracture line. Routine postoperative care was followed.

Figure 1: Bioresorbable screws and plates pre-sterilized and made of polylactic acid, poly glycolic acid and poly dioxanone polymers.
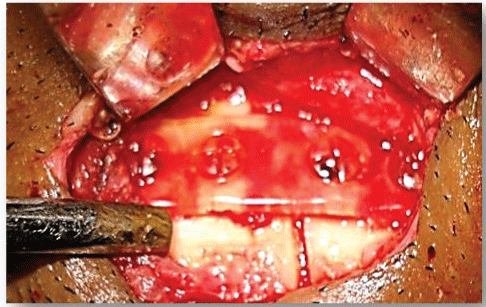
Figure 2: Resorbable plate fixations in mandibular fracture showing good adaptation of plates with contour of mandible and in ideal reduction position.
Data collection was done at the immediate post-operative period (within 72 hrs.) and at the end of 1,2,4,6 and 8 weeks. These patients were checked for pain, oedema, infection, occlusal derangement, suture dehiscence, paresthesia, anesthesia, plate rejection, malunion, non-union, palpability of plate. Radiographically orthopantomogram (OPG) was done post operatively and on routine follow up, the fracture was accessed on its reduction, changes at the fracture line, sign of osteogenesis, visibility and osteolysis around the drill holes in the case of bioresorbable group of patients. All percentage data were subjected to arcsine square-root transformation before statistical analysis. Data are analyzed statistically using SPSS version 16.0 software (SPSS Inc., Chi-cago, IL, USA). Differences between groups were examined and the significance value was set at p<0.05 level.
In the present study, maximum patients were males 90% (54 patients), while 6 patients were female 10% (6 patients). The plates and screws (Figure 1) used were gamma sterilized by the manufacturer and supplier in sterile double packing. In bioresorbable plate group, a good adaptation of the plate by digital pressure (Figure 2) was seen in all 30 patients (100%). However, titanium plate group was good only in 24 patients (80%) and fair in 4 patients (13%). The different anatomical locations of fractures revealed that parasymphysis is the most common site of fracture (28 patients, 46.6%), followed by angle (20 patients, 33.33%) and subcondylar (12 patients, 20%) (Table 1). Good reduction of fracture was achieved in all the 30 patients of bioresorbable group (100%). However, in titanium group, a good reduction was achieved in 24 patients (80%) and fair in 6 patients (20%). In bioresorbable plate group, a good primary stability was achieved in 25 patients (83%) intra operatively and fair in 5 patients (17%). In titanium plate group, a good stability was achieved in all 30 patients (100%). Screw breakage intra operatively was seen in 15 patients (50%) of bioresorbable group due to its innate property and weakness as compare to titanium screws. Loosening of screw intra operatively was noticed in 6 patients (20%) of bioresorbable group, while no loosening of screw was encountered in the titanium group (Table 2).
| Characteristic | Bioresorbable plates | Titanium plates | P value |
| Sex | |||
| Male | 28 (93.33%) | 26 (86.67%) | 0.389 |
| Female | 2 (6.67%) | 4 (13.33%) | |
| Mechanism of injury | |||
| RTA | 25 (83.33%) | 26 (86.67%) | 0.717 |
| Altercation | 5 (16.67%) | 4 (13.33%) | |
| Concomitant fracture pattern | |||
| Parasymphysis | 15 (50%) | 13 (43.33%) | |
| Angle | 11 (36.67%) | 9 (30%) | 0.435 |
| Subcondylar | 4 (13.33%) | 8 (26.67%) | |
Table 1: Preoperative demographic data.
| Variability | Bioresorbable plates | Titanium plates | P value |
| Good adaptation of plate | 30 (100%) | 24 (80%) | 0.0098 |
| Good reduction of fracture achieved | 30 (100%) | 24 (80%) | 0.0098 |
| Primary stability of fracture achieved | 25 (83%) | 30 (100%) | 0.010 |
| Screw breakage | 15 (50%) | 0 | 0.000 |
| Loosening of screw | 6 (20%) | 0 | 0.009 |
Table 2: Comparison of outcomes in bioresorbable group with titanium group.
Post-operative pain and oedema were present in both the groups. In 6 patients of titanium group, post-operative pain and oedema persisted for almost 1 week with signs of infection. In bioresorbable group, inter maxillary fixation (IMF) was kept for 4 weeks due its less ability to counter muscle and occlusal forces except in 8 patients where it was kept for 5 weeks because a proper reduction and stability of fracture segments was not achieved intra operatively. In titanium group, IMF was kept for 2 weeks except in 6 patients where it was kept for 4 weeks. Due to the presence of infection and plate rejection, the plate was removed from this patient. Rejection and palpability of plates was observed only in 6 patients in titanium group (Table 3).
| Variability | Bioresorbable plates | Titanium plates | P value | |
| Pain present in Days | 1 | 13 (43.33%) | 13 (43.33%) | 0.0262 |
| 2 | 17 (56.67%) | 11 (36.67%) | ||
| 7 | 0 (0%) | 6 (20%) | ||
| Oedema present in days | 1 | 13 (43.33%) | 13 (43.33%) | 0.0262 |
| 2 | 17 (56.67%) | 11 (36.67%) | ||
| 5 | 0 (0%) | 6 (20%) | ||
| Duration of IMF in weeks |
2 | 0 (0%) | 24 (80%) | 0 |
| 4 | 22 (73.33%) | 06 (20%) | ||
| 5 | 8 (26.67%) | 0 (0%) | ||
| Rejection of plate |
No | 30 (100%) | 24 (80%) | 0.009 |
| 0 (0%) | 6 (20%) | |||
| Palpability of plate | No | 30 (100%) | 24 (80%) | 0.009 |
| 0 (0%) | 6 (20%) |
Table 3: Comparison of post-operative criterias in bioresorbable group and titanium group.
In radiographic observations (OPG) was carried out immediate post operatively and routine follow up and apart from fracture reduction the fracture line was evaluated on various parameters such as deviation, disastasis, no change, sign of osteogenesis etc. The level of lower border of mandible was accessed. In the bioresorbable group, osteolysis around the drilled holes was checked in follow up OPG’s. Most importantly visibility of fracture line was evaluated in both the groups, showing good visibility in the bioresorbable group as compare to the titanium where it was fair (Table 4).
| Variability | Bioresorbable plates | Titanium plates | P value | |
| Visibility of fracture line | Good | 30 (100%) | 0 (0%) | 0 |
Table 4: Visibility of fracture line on OPG in bioresorbable and titanium study groups.
Rigid plate and screw fixation is the mainstay of treatment for complex fractures of the facial skeleton. The ideal implant for the fracture fixation should be rigid and biocompatible. It should have mechanical properties similar to that of bone and permit osseous union through primary bone healing. Although the metallic plates satisfy most of the criteria, there are a plethora of problems associated with their use. One of the common problems encountered with retaining metallic plates in craniofacial region is interference with the imaging techniques such as CT and MRI scans causing artifacts [17]. Apart from these complications like corrosion, electrolysis, hypersensitive and even carcinogenic potential have been reported. In an attempt to overcome these problems, there was a spur of interest in the development of bioresorbable osteofixation materials [18].
Kulkarni and his group (1966) applied bioresorbable plates for the first time to treat the maxillofacial fractures [19]. Enislidis G et al. successfully fixed zygomatic fractures with bioresorbable plate osteosynthesis found them simple and safe [20]. Landes et al. used these bioresorbable plates in sagittal split osteotomies and stated that they function as titanium in fixation for orthognathic surgery and do not impose an increase in clinical morbidity [16]. The biodegradable material is softer and weaker than titanium and requires tapping to place the screws. Unlike titanium, in which firm pressure and tight screw placement is favorable, biodegradable screws need only be finger tight and care must be taken when placing them into thin bone, if excessive torque is applied, the screw head breaks off [21].
In the present study, we compared the clinical efficacy of bioresorbable plates and titanium miniplates in management of mandibular fracture. In our study good stability was achieved in titanium plate group (100%) than in bioresorbable plate group (83%). These results are in accordance with observations that the titanium plate group gives better stability as compare to bioresorbable plate group [21]. Screw breakage and loosening of screw intra operatively was seen only in the bioresorbable group, due to its innate property and weakness as compare to titanium screws. The better performance of titanium screws has already been reported for craniofacial fractures [22]. The screw breakages are due to material failure and incorrect handling. In such cases, a new hole was easily drilled through the broken screws and a new screw was inserted without problems, fitting perfectly into the mandibular bone.
The adaptation of the bioresorbable plates to the bone surface was not complicated as with titanium miniplates. A slight grade of over bending was necessary because of the elasticity of the material. In contrast to others, bioresorbable fixation systems no healing device was necessary. The plates were easily bendable with forceps at room temperature and none of the plates broke during bending. At the bending areas, white lines occurred in the transparent plates, but this did not influence the physical quality of the devices. This phenomenon is described as microdelamination in the instruction of the manufacturer [23]. In the present study, adaptation of plates was good in all the 30 patients in bioresorbable group and 24 patients in titanium group, only in 6 patients of the titanium group; the adaptation of plate was fair. Reduction of fractured segment achieved intra operatively was good in all the 30 patients of bioresorbable group. In titanium plate group, it was good in 24 patients and fair in 6 patients.
The biodegradable fracture fixation devices are more attractive than metal ones because no removal operation is needed after bone healing. It is common practice to remove metal plate and screw after bone healing. If not removed, the metal implants may be painful and irritating. Post operatively and on routine follow up at 2, 4, 8, 12 weeks and then every after 6 months, patients were checked for pain, oedema, infection, occlusal derangement, suture dehiscenece, paraesthesia, anesthesia, plate rejection, malunion, non-union, palpability of plate. Infection was seen in 6 patients of the titanium plate, pain and infection persisted for almost 1 week with suture dehiscence, plate rejection and palpability, the plate was removed and IMF was placed for 2 weeks, except for 6 patients where it was 4 weeks as described above. The mechanical properties of the bioresorbable plates and screw applied for mandibular fracture fixation are comparable with those of metal fixation systems. The treatment goals of immobilizations, fixation and stabilization were found to be fulfilled. The skeletal stability was comparable with actual standards and sufficient for the time needed for mandibular bone healing on the basis of results of the study. Indeed, the biodegradable implants have the potential for successful use in the fixation of human mandibular fractures.
Our results suggest that biodegradable polymers exhibit negligible complications, good handling properties and less interference with craniofacial growth during the management of mandibular fracture. However, high cost of material is the greatest deterrent to its wider use and further research is required for its use in the treatment of mandibular fractures. On the other hand, the titanium miniplates are also malleable and easily adaptable to the bone in comparison with bioreabsorable plates. The titanium plates have shown the better handling properties and stability of fractured fragments. The titanium miniplates are much cheaper as compared to bioresorbable plates; hence it is being used widely for the treatment of mandibular fractures. The patients who are not able to offer bioresorbable plates, the titanium miniplates can be their choice of treatment.
VK, SG, RKC, RKC, MT and SKC declare that they have no conflicts of interest directly relevant to the content of this article.
VK, SG, RKC, RKC and MT searched the literature and drafted the manuscript under the supervision of SKC.
Download Provisional PDF Here
Article Type: REVIEW ARTICLE
Citation: Kumar V, Gour S, Chaube RK, Chaube RK, Chaube SK, et al. (2018) Comparative Efficacy and Adaptability of Bioresorbable Plates with Titanium Miniplates in the Management of Mandibular Fractures. Clin Res Open Access 4(2): dx.doi.org/10.16966/2469- 6714.137
Copyright: © 2018 Kumar V, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access