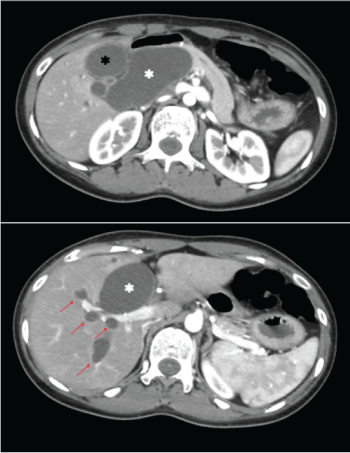
Figure 1: CT scan showing dilatated common bile duct (white asterisk) with dilatation of gallbladder (black asterisk) and intra hepatic bile ducts (red arrows).

Luigi Romeo1* Gabriele Anania1 Serena Rubino1 Cristina Bombardini1 Francesca Petrarulo1 Giorgio Ercolani2
1Department of Morphology, Surgery and Experimental Medicine, Sant’Anna University Hospital, University of Ferrara, Ferrara, Italy*Corresponding author: Romeo Luigi, Department of Surgery, Surgery 1 Unit, Sant’Anna University Hospital, Ferrara, Italy, E-mail: luigi.romeo@live.com
Choledochal cysts are congenital biliary tract diseases, which typically interest childhood. They are rarer in adults, but their incidence is getting higher in last decades according to recent reports. Their incidence is higher in Asian population and in woman. In adults, clinical manifestations include a specific symptoms and complications of the disease, such as jaundice, cholangitis, pancreatitis and biliary tract malignancies. In order to avoid these serious complications, definitive treatment is required, which consists in surgical excision of the cyst and cholecystectomy with hepaticoenterostomy. We report the case of a young woman who arrived to our attention for abdominal pain and jaundice for a choledochal cyst.
Choledochal cysts; Biliary tract cysts; Jaundice; Cyst resection
Biliary tract cysts are a rare biliary malformative pathology, accounting for 1% of benign biliary diseases [1]. Reported incidence may vary according to different series, and is higher in Asian population (1:1.000 - 1:10.000) [2] than in eastern countries, where is about 1:100.000 - 1:150.000. Female sex is more frequently interested, with a ratio of 4:1 [2,3].
Firstly classified by Alonso-Lej in 1959, nowadays the most widely accepted classification is the one provided by Todani et al., in 1977 [4]. This classification divide biliary cysts in five categories: type I, II and III involve extra-hepatic bile ducts, with differences in morphology and site, type IV involves both intra and extra-hepatic biliary tree, and type V involves only intra-hepatic ones (Caroli’s disease).
Choledochal cysts usually interest the younger ages, but in recent series are reported increasing diagnosis in adults [5]. Clinical manifestations typically include abdominal pain in upper right quadrant, obstructive jaundice, nausea and vomit, and palpable abdominal mass, especially in children. In other cases, complications such as cholecystitis, choledocholithiasis or cholangiocarcinoma represent the disease debut. Cholangitis and pancreatitis can also occur.
Early diagnosis and treatment of biliary tract cysts are very important, because they carry a malignant potential that increase with age. Surgical resection of the cyst and subsequent hepaticoenterostomy is recognised as the gold standard worldwide for extrahepatic biliary duct cysts, especially for type I and type IVa biliary cysts, while hepatic resection are indicated for localized Caroli’s disease [6]. Herein we report the case of a woman who arrived to our emergency department (ED) for abdominal pain and jaundice.
A 30-years-old woman came to the ED of the Sant’Anna hospital of Ferrara complaining pain in epigastrium and right hypochondrium without fever. Her past anamnesis was negative and she did not assume home therapies. Physical examination did not showed anything relevant. The patient underwent abdominal ultrasounds that found a 36 mm choledochal cystic dilatation, in absence of dilatation of other tracts of the biliary tree or other signs of acute pathologies. In consideration of the absence of conditions requiring hospitalization, the patient was discharged. Three days later, the woman come back to our ED referring persistence of symptoms. Serum total bilirubin was 4 mg/dL, with direct bilirubin of 2,5 mg/dL. The patient was submitted to abdominal CT scan that showed dilatation of intra and extra-hepatic bile ducts, with a maximum diameter of 5 cm at the common bile duct (CBD), which ended at the beginning of the pancreatic portion of the CBD (Figure 1). The patient was admitted in order to attempt endoscopic retrograde cholangiopancreatography (ERCP). The day after admission, ERCP showed an extra-hepatic CBD dilatation with a papillary stenosis, and a 10 Fr plastic stent was placed. The patient also underwent Magnetic Resonance Cholangiopancreatography (MRCP) that confirmed a 22 mm dilatation of CBD (Figure 2). Moreover, a revision of past imaging showed a dilatation of CBD in an abdominal ultrasounds performed in 2004, and re-evaluation of the patient anamnesis revealed a personal history of recurrent abdominal pain in paediatric age. These anamnestic findings, together with the clinical presentation and imaging, suggested Todani’s Type I CBD cyst diagnosis. In order to exclude other causes of biliary tract dilatation, the woman underwent endoscopic ultrasounds that confirmed the previous radiological investigations in absence of findings suspected for neoplasms. The patient was discharged few days later, after complete resolution of symptoms. One month later, the patient come back to ED complaining abdominal pain in right upper quadrant, nausea and vomit, and hyperpyrexia (38.5 ºC). Her blood tests showed neutrophilic leucocytosis, elevate C-reactive Protein and Procalcitonin plasma levels and a serum total bilirubin of 3 mg/dL. After admission, antimicrobial therapy started. Another ERCP found a partial dislocation of the biliary prosthesis, which was removed and substituted with a metallic one. She was discharged two days after the procedure.

Figure 1: CT scan showing dilatated common bile duct (white asterisk) with dilatation of gallbladder (black asterisk) and intra hepatic bile ducts (red arrows).
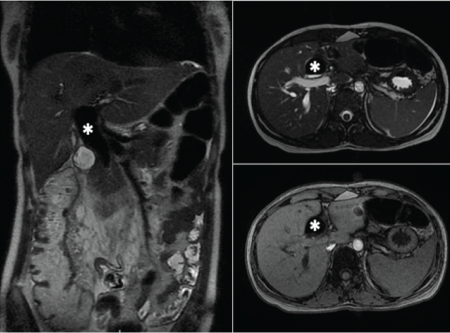
Figure 2: RM confirm common bile duct dilatation (white asterisk) after biliary drainage.
In the next months, the patient came three times to our ED for abdominal pain, but she did not required hospitalization. The patient was sent to the General and Oncologic Surgery Unit of the Morgagni-Pierantoni hospital of Forlì, which is a referral centre for hepatopancreatobiliarydiseases, where she was submitted to preoperative evaluations. Six months after diagnosis, the patient underwent cyst excision, cholecystectomy and Roux-en-Y hepaticojejunostomy (Figure 3). After surgery the patient did not developed any relevant complication and she fully recovered.
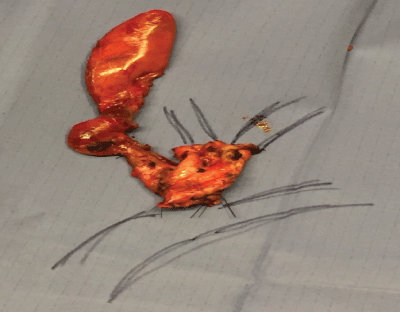
Figure 3: Resected common bile duct cyst and gallbladder.
Etiology of biliary cysts is not clear and many theories have been proposed to explain their pathogenesis. The most widely accepted one suggests that an abnormal pancreaticobiliary junction (APBJ), which consist in a union of CBD and pancreatic duct outside duodenal wall with formation of a long common duct, can lead to pancreaticobiliary reflux and subsequent activation of pancreatic enzymes in biliary ducts. Activated pancreatic enzymes deteriorate ducts wall leading to cyst formation [7]. Other theories propose that a congenital malformation of ductal plate or acquired distal biliary tract obstructions leads to development of the Biliary Ducts Cysts [8]. Despite about 80% of biliary tract cysts are diagnosed in childhood, their exordium in adult age is not infrequent. Diagnosis in adult is increasing in the last years, mainly because of spreading of modern imaging techniques [9]. The classic triad made of intermittent jaundice, right abdominal mass and pain is rarely found and is more frequent in children. Symptoms in adult are not specific and depend on complications of the cyst [10]. They include recurrent abdominal pain, nausea and vomit, dyspepsia and jaundice. Cysts can also lead to infective complications due to recurrent cholangitis, like liver abscess or sepsis and septic shock. Moreover, patient can reveal a personal history of recurrent abdominal pain, so attention on collecting anamnesis should be payed. Assesment of patients with symptomatic CC often starts from abdominal ultrasounds that demonstrate a cystic mass in right upper quadrant in continuity with biliary tree. CT scan can easily demonstrate if cystic lesions are in continuity with biliary tract and is more accurate than ultrasonography in diagnosis of biliary tract cysts, especially for intrahepatic and distal portions [10]. MRCP is considered the gold standard for diagnosis of CBD cysts, with report sensitivity of 90-100% [11]. It can also be performed with use of hepatospecific contrast agents, that can allow better visualization of biliary anatomy. In some cases, more invasive imaging techniques such as ERCP and Percutaneous Transhepatic Cholangiography should be performed. The advantage of these procedures is that they could be both diagnostic and therapeutic procedures. Biliary tract cysts can lead to severe complications related to chronic bile stasis and inflammation characterized by important mortality and morbidity. Moreover, association between CC and cholangiocarcinoma is well known. The risk of development of malignancies of the biliary tract increase with age, with reported incidence of 10-30%. Todani’s type I and type IV cysts are mostly associated with development of cholangio carcinoma. In order to avoid complications, definitive treatment of choledochal cysts is required [5]. The correct treatment depends on the cyst type. Many surgical strategies have been proposed for type I cysts. Internal drainage of the cyst through creation of a cystenterostomy was the first treatment that gained wide diffusion, but it was burdened by many long-term complications [8]. Moreover, incomplete excision of the cyst can lead to the development of malignancies. Nowadays, complete resection of the cyst with cholecistectomy and reconstruction with hepaticojejunostomy is considered the treatment of choice for Biliary Cysts [6,12]. Early postoperative complications include pancreatitis, cholangitis and anastomotic leakage, while bile ducts and anastomotic stenosis, recurrent cholangitis or pancreatitis, biliary stones and malignancies are reported as long term complications [12]. Therefore, lifelong follow up, especially for cancer surveillance, is mandatory. When required, it is advisable to send patient to a referral centre for treatment of biliary pathologies in order to concentrate resources and expertise, to reduce the risk of surgical complications, and to guarantee better outcomes to patients.
Choledochal cysts are rare in western countries and are typical of younger ages, but diagnosis in adults can also occur. Surgical treatment is required in order to avoid development of complications and consists in the excision of the cyst. Treatment should be delegated to referral centres in order to ensure the best cares to patient.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: Romeo L, Anania G, Rubino S, Bombardini C, Petrarulo F, et al. (2018) Choledochal Cyst in a Young Woman: A Rare Cause of Jaundice in Western Adults. Clin Res Open Access 4(2): dx.doi. org/10.16966/2469-6714.135
Copyright: © 2018 Romeo L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access