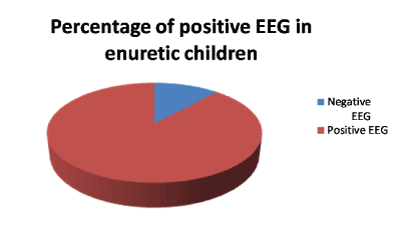
Figure 1: Showing percentage of abnormal EEG findings in patients presented with enuresis.

Maha Nada1* Mohamed A Gamal2
1Neurology department, Ain Shams University, Cairo, Egypt*Corresponding author: Maha Nada, Neurology department, Ain Shams University, Khalifa El-Maamon St El-Qobba Bridge, Cairo, Cairo Governorate 11566, Egypt. E-mail: drmahanada@yahoo.com
Abstract: Among causes of secondary enuresis, epilepsy was none of those. It was observed in 15 children with secondary enuresis whom were urologically free, that their sleep EEG showed epileptic discharge without any other manifestations of epilepsy. After receiving antiepileptics, soon they became dry. There were common manifestations between those patients and they share some EEG similarities which we will try to explain aiming to shed the light on this possible new syndrome. This can guide future research for better management of such condition.
Background: In our pediatric neurology clinic, we have seen many children with secondary nocturnal enuresis. They have been thoroughly investigated for any urological cause, and all common therapies and regimens have failed to control their problem. The patients and families were in great distress especially when those children became embarrassed in front of other siblings or strangers. We have noticed that many of those children experienced mild scholastic deterioration coincident with the start of their enuresis.
Objective: To find clinical similarities between children with epileptic enuresis and describe features of this possible syndrome.
Materials and methods: This was an observational study done on 15 enuretic children, whom were urologically free, collected within the last year. History taking, neurological examination, Sleep EEG, and MRI epilepsy protocol were done for all patients. Data were collected and reviewed by the writer.
Results: In a sample of secondary enuretic children (age: 5-14), 10 males and 5 females; 9 of them had FH of epilepsy, 10 of them had mild cognitive affection with onset of enuresis. All of them were having epileptic form activity in their Sleep EEG. All of them had Normal MRI. 12 of them improved significantly after one or two months of the use of antiepileptics.
Conclusion: The result of this study raise the possibility of the presence of Benign Childhood Epileptic Enuresis as one of the benign childhood epilepsies with characteristics as described.
Enuresis; Childhood Epilepsy; Benign Childhood Epilepsy
Normally, minimal sphincteric control starts between the 12th and 18th month of age. Normal child starts to control urine between the 24th and 30th month of age. Full sphincteric control can be achieved by the age of three. After the age of 5, the child can void urine even if a little amount is in his/her bladder [1]. The word enuresis is derived from the Greek word (enuorein) which means to void urine. The International Children’s Continence Society (ICCS) restricts the term to wetting that occurs at night. Enuresis can be divided into primary enuresis (PE) and secondary enuresis (SE). A child who has been continent for at least 6 months before the onset of bed wetting is considered to have SE. The pathogenesis of PE is similar to that of SE. Many causes for such conditions have been proposed as: slower physical development, excessive output of urine during sleep, anxiety, genetic causes, obstructive sleep apnea, structural urinary system problems, overactive bladder and infrequent voiding [2,3]. According to DSM-5 criteria, the behavior is either (a) occurs at least twice a week for at least 3 consecutive months, or (b) results in clinically significant distress or social, functional or academic impairment. The behavior occurs in a child who is at least 5 years old (or has reached the equivalent developmental level) [4].
Enuresis commonly occurs within the attack of generalized tonic clonic seizure or even tonic seizures.
Contraction of the bladder wall with full bladder, forces the urine out due to the increase in the intravesical pressure.
Theoretically speaking; any contraction of bladder wall especially with impaired awareness can cause enuresis as well.
Enuresis commonly occurs within the attack of generalized tonic clonic seizure or even tonic seizures. Contraction of the bladder wall with full bladder, forces the urine out due to the increase in the intravesical pressure. Theoretically speaking; any contraction of bladder wall especially with impaired awareness, can cause enuresis as well.
While urinary incontinence commonly accompanies generalized seizure, few studies address it to simple focal seizures or complex partial seizures [5].
Also some studies failed to find an increase in incidence of enuresis in epileptic patients more than in normal population [6].
In 2010, a 14 years old male patient presented with SE nearly 5 years before presentation, with subsequent anxiety and distress. He was investigated thoroughly for any urological cause, but all were normal. Due to the FH of epilepsy in a maternal cousin, sleep EEG was requested. The EEG showed epileptic discharge and he rapidly became dry using lamotrigine 5 mg\kg. 3 years later, medication was successfully withdrawn.
Since then; for any child presenting with SE or even prolonged PE, I always request Sleep EEG after exclusion of all possible urological causes. One year ago, I have started to collect data of enuretic children coming to our pediatric neurology clinic. Till the end of this study submission; new children with the same condition were coming to our pediatric neurology clinic.
We had 17 children with SE, we excluded 2 of them whom sleep EEGs were normal, careful history taking showed that 2 patients were mouth breathers by night and we referred them to the ENT clinic and recommended polysomnography. This study included 15 enuretic children aged (5-14 years) who presented to our pediatric neurology clinic of Neurology department, Ain shams University.

Figure 1: Showing percentage of abnormal EEG findings in patients presented with enuresis.
This was an observational study. Data were collected regarding personal data, FH of epilepsy, developmental history, onset of enuresis, results of MRI, improvement of condition with treatment and type of therapy. Improvement in the following table means that the child became completely dry or enuresis occurred less than once per month in a child less than 8 years of age. Results of Sleep EEG were reviewed by me focusing upon the site and type of epileptic discharge. Detection of seizure activity was done manually as no available automatic detection. EEGs were done in neurology department and in psychiatric department of Ain Shams University hospitals. Statistics were meaningless due to little number of patients (Table 1).
| Treatment | Improvement | EEG | Recent memory or concentration | FH of epilepsy | onset | Sex | Age | No |
| Lamot | + | CT | No | + | 7 | M | 9 | 1 |
| Oxacarb | + | CT | Yes | + | 6 | M | 10 | 2 |
| Oxacarb | + | CT / FP | Yes | + | 9 | F | 9 | 3 |
| Lamot | + | CT | Yes | + | 8 | F | 13 | 4 |
| Carbama | - | CT /FP | No | - | 7 | M | 10 | 5 |
| Levetira | + | CT / O | Yes | + | 8 | M | 9 | 6 |
| Levetira | + | Left C | Yes | - | 6 | M | 10 | 7 |
| Levetira | + | CT | No | + | 7 | M | 9 | 8 |
| Lamot | + | CT /O | Yes | - | 6 | F | 11 | 9 |
| Lamot | + | CT | No | + | 8 | F | 12 | 10 |
| Oxacarb | + | CT /FP | No | - | 5 | M | 6 | 11 |
| Valproat | - | CT /FP | Yes | + | 10 | F | 12 | 12 |
| Levetira | + | CT | Yes | - | 5 | M | 5 | 13 |
| Lamot | + | Left C /FP | Yes | - | 8 | M | 14 | 14 |
| Valproat | - | Left T /O | Yes | + | 7 | M | 13 | 15 |
Table 1: showing the results of our study.
10 of those patients were males and 5 were females.9 of them had positive FH of epilepsy.10 patients had mild decline of their scholastic performance in the form of recent memory and concentration problems. All patients had normal developmental history, normal neurological examination, and normal MRI brain. All showed rapid improvement (1-2 months) on different antiepileptics except 3 patient (two were on valproate and one on carbamazepine) for more than 3 months. These are not statistics but an observation that can raise suspicion for future research.
Sleep EEGs were reviewed by the author manually. It showed similar results as follows:
When EEG was repeated for two of the patients, same characteristics applied except for a change in the site of discharge, as foci moved slightly within the centrotemporal region (migrating spikes). (Figures 2-5)
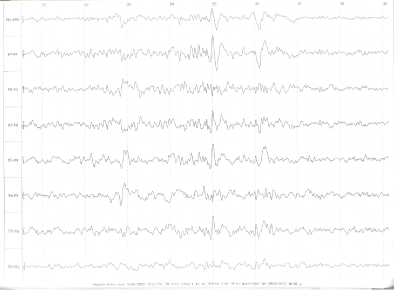
Figure 2: Sleep EEG showing multifocal bilateral temporal discharge.
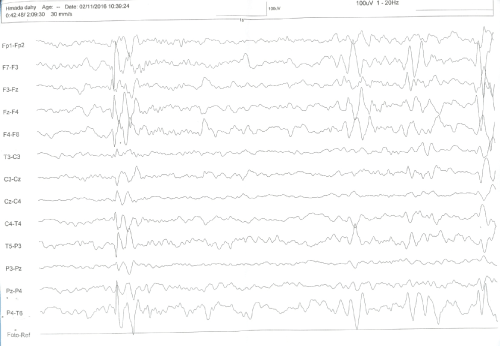
Figure 3: Sleep EEG showing simultaneous left parietotemporal and right parietal discharge.
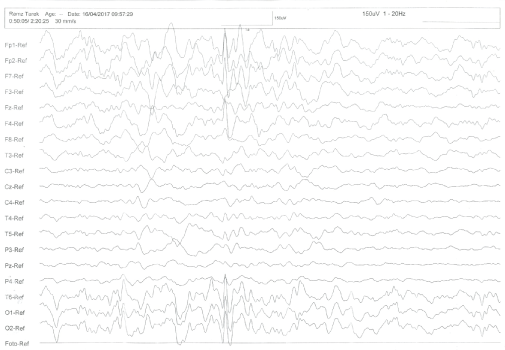
Figure 4: EEG showing multifocal simultaneous left temporal, right temporal and bilateral occipital.
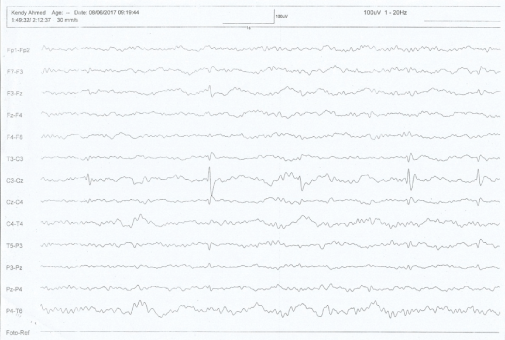
Figure 5: Sleep EEG showing left central discharge.
In this study: patients with positive FH of epilepsy, when were asked about the type of epilepsy in their known relatives and of pediatric relatives from our clinic; three of them had BRE, one had ICOE, another one had febrile seizures. For the other three we didn’t find any data.
Our patients were continent for a while (not less than 6 months) before occurrence of SE. They have normal urological investigations and no history suggestive of obstructive sleep apnea.
Most of them had minor affection of their recent memory and concentration, coincident with the start of the problem (even at day time when no enuresis is present) as those children became unable of remembering what was studied in the day before, mothers noticed that they became forgetful for what was told to them at home despite being normal before that, normal previous scholastic achievement and having normal developmental history. This could be explained by the fact that; the abnormal EEG could itself affect the normal brain functions as neurons became busy with this frequent abnormal discharge and the discharge interrupt the normal neuronal activity.
It is noticed in this study that those patients improved easily with the use of different antiepileptic drugs. This improvement couldn’t be attributed to the mere effect of those antiepileptics on sleep structure because the used antiepileptics have different effects on sleep architecture [7].
In the present work, we did not depend on the failure of other investigations to explain this condition. We depend on the positive EEG results which were frequent, repeatable, similar and treatable.
The similar EEG changes, the normal MRI, normal cognition together with the rapid improvement on antiepileptic medications; suggest this syndrome to be one of the benign childhood epileptic syndromes.
The EEG in BRE is highly similar to what we have found as regard the high amplitude waves in the centrotemporal region but in our syndrome; the EEGs showed multiple foci of epileptic discharge making it difficult to attribute the discharge to single focus and some patients showed occipital sharp-slow complexes as well.
Prior to this study; I have encountered patients with SE problem and similar to our patients but they were not diagnosed as having epilepsy. They didn’t receive any antiepileptics and there were spontaneous improvement after many years, almost by adulthood. This observation goes with the benign nature of this syndrome.
“Benign childhood epileptic enuresis” of Maha Nada is the most suitable name for such syndrome, which can be one of the groups called (Benign Childhood Seizure Susceptibility Syndrome).
The concept of BCSSS was first proposed by Panayiotopoulos in 1993 [8].
Subsequently, the original description has been expanded and its utility emphasized (Panayiotopoulos 1999, 2007; Panayiotopoulos et al, 2008) [9-11].
The concept is that these syndromes are linked by a common genetically determined functional derangement of the maturational process of the brain [12].
These disorders included in BCSSS are:
Evidence supporting this concept includes:
Panayiotopoulos stated that these syndromes almost have excellent outcome with regard to the cessation of seizures but may be associated with learning, behavior, or attention issues that cause havoc if not properly recognized and treated [13].
Murro AM et al showed that those epilepsies have normal interictal background and contain highly stereotyped spikes. Those spikes may be found in a single focus, in homologous regions or in multiple foci [21].
In some circumstances, the multifocal spikes may appear almost simultaneously. They have been referred to as “clone-like” and they appear to be driven by a primary basic generator, which is posteriorly located and often of the smallest amplitude [13].Researchers at Chung Shan Medical University in Taiwan analyzed 969 EEGs from 463 children with epilepsy to determine outcome difference over 3 years between those with fixed epileptic foci and those with migrated foci. They found that children with epilepsy and age-related migrating foci have a better prognosis than those with fixed EEG foci [22].
I think this new syndrome should be the fifth of the BCSSS, and may be the causative genes are similar but can manifest in different clinical picture between different patients. The syndrome can be added as a monosymptomatic epilepsy syndrome which I think is common but under diagnosed and under investigated. Follow up of those patients improvement on both enuresis and cognitive domains will help more understanding of this syndrome.
Secondary enuretic children with no urological abnormality may be epileptic and Sleep EEG can easily help recognition of Benign Childhood Epileptic Syndrome. EEG shows the high amplitude spike/slow or sharp slow complex, multifocal (central or centrotemporal or less frequently occipital) unilateral or bilateral discharge. The discharge is asynchronous but sometimes synchronizes in a clone like pattern. Benign refers to the normal MRI, normal cognition except for mild affection of recent memory and concentration and also refers to the easily improvement with most of the used antiepileptics preferably those with little or no cognitive side effects.
Addition of multifocal category under the Focal type of epilepsy (in the classification of ILAE) as a single entity, which might differ from the usual focal epilepsy.
Download Provisional PDF Here
Article Type: Research Article
Citation: Nada M, Gamal AM (2017) New Sole Presentation of Childhood Epilepsy, Clin Res Open Access 3(2): doi http://dx.doi.org/10.16966/2469- 6714.126
Copyright: © 2017 Nada M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access