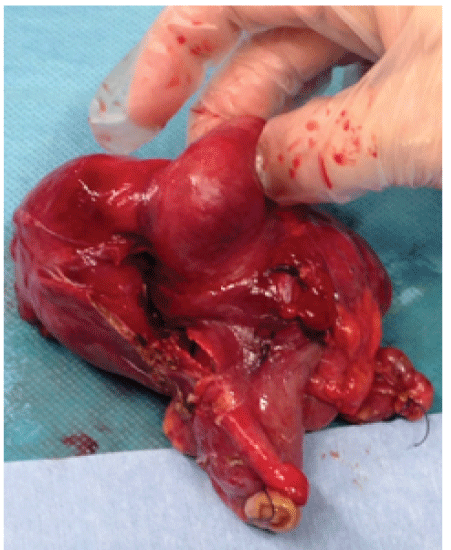
Figure 1: Surgery specimen

Monterde Álvarez ML1 Latorre Martínez E2 París Sans M3* Piñana Campón ML4 Del Castillo Déjardin D1 Queralt Escarre RA2 Feliu Rovira A3* Rius Gordillo N4 Escribano Subías J1
1Paediatric Service, Hospital Universitari Sant Joan de Reus, Reus, Tarragona, Spain*Corresponding author: Maria Laura Monterde Álvarez, Hospital Universitari Sant Joan de Reus, Reus, Tarragona, Spain, Tel: 679543434; E-mail: madchen24@hotmail.com
The presence of a tumor in the intestine should make us think of a wide group of differential diagnoses from tumour to infectious etiology. We report a 13-year-old patient with cecal tumor discovered during an emergency intervention for suspected appendicitis after a clinical and ultrasound assessment. Right hemicolectomy with an end-side anastomosis is performed during the intervention. The pathological study confirms the infectious etiology of the process after Actinomyces spp presence confirmation. Later, medical treatment is performed with oral amoxicillin for 4 months with good clinical evolution without presenting associated complications. Actinomycosis is an infectious disease that should be considered in the differential diagnosis of abdominal pain torpid, because their management and treatment are specific, and are primordial to reduce the risk of associated complications.
Actinomycosis; Appendicitis; Abdominal pain; Abdominal tumor
The presence of a tumor in the intestine is a rare-finding in children. Given this finding we must take into account a wide range of differential diagnoses, from cancer to infectious disease etiology, mainly abdominal tuberculosis, amebiasis and granuloma for Yersinia spp, Salmonella spp or Actinomyces spp. Actinomycosis is an infectious disease which must be acknowledged, because although it is relatively rare, management and treatment are specific, and will be essential to reduce the risk of associated complications.
Case exposed is related to 13-year-old male patient who presents pain at the right lower quadrant over 24 hours evolution, with no fever or symptoms. He is emergency attended at pediatric hospital service.
As unique clinical history refers gastroenteritis by Campylobacter jejuni occurred during the first month of his live, solved with any complications. Physical examination by apparatus highlights by tenderness in the right lower quadrant with positive Blumberg maneuver without other signs of peritoneal irritation. The rest of the examination does not show other pathological findings. Following values are showed by the blood test: 11,350 leukocytes/mm3 with 71% segmented neutrophils and PCR 0.5 mg/dl. Urine reactive strip give a negative result. Compressible tubular structure in the right iliac fossa is observed by abdominal ultrasound. In addition, the ultrasound shows a little quantity of free fluid and discrete inflammatory changes around it. Come from analytic and radiologic tests, emergency surgery is decided because high suspicious of acute appendicitis. By McBurney incision to approach appendix, a Cecal tumor of 50 × 40 mm without inflammatory signs is identified instead (Figure 1). Multiple lymph nodes are observed, but cecal appendix is not evident during the surgery. Due to a tumoral process suspicious, right hemicolectomy is done with an end-side anastomosis by infraumbilical midline laparotomy.

Figure 1: Surgery specimen
An infection in the surgical wound appears during the third day after surgery. Treatment is initiated by amoxicillin–clavulanic acid. After 10 days post intervention, and due to the clinical improvement, the patient is discharged with oral antibiotic therapy and under control outpatient clinic of our center.
The pathological study shows signs of acute appendicitis with necrotizing granuloma, inflammatory periappendicular plastron, necrotizing granulomatous lymphadenitis and presence of a bacterial colony in the appendicular ostium, suggestive of Actinomyces spp, visualizing the associated Splendore-Hoeppli phenomenon (Figure 2). In the rest of the colonic mucosa, small intestine and impellers, no signs of inflammatory bowel disease are found. Stains of PAS, Grocott, Gram and Ziehl-Neelsen are performed and do not show any other microorganisms presence.
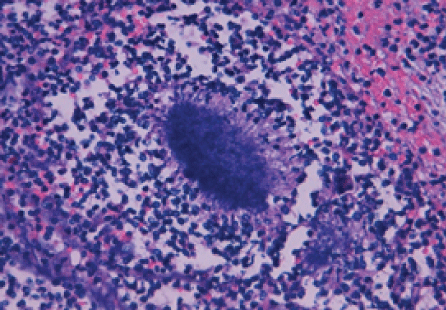
Figure 2: Splendore-Hoeppli phenomenon.
Given those results, medical treatment continues with oral amoxicillin (50 mg/kg/day) and close monitoring in outpatient of Surgery and Paediatric Infectious Diseases is performed. The basic screening of primary immunodeficiency’s (CBC and immunoglobulin’s), HIV infection and TB test are also performed with negative results.
The patient has an excellent clinical outcome, complete healing of the surgical wound and without observing the presence of fistula. After 4 months of antibiotic treatment, he remains asymptomatic at present, one year after the process.
Actinomycosis is a bacterial infection caused by various species of the family Actinomycetaceae. Those are anaerobic gram-positive filamentous bacteria’s, which the most common human species is A. israelii.
Usually it is part of the commensal flora of the gastrointestinal and genitourinary tract; however, the disruption of the mucosal barrier can produce endogenous opportunistic infection. Actinomycosis is a granulomatous infection with a highly variable latency period, which can vary from days to even years from inoculation to the onset of symptoms. This infection can show a wide type of symptoms. For that reason, together low incidence of actinomycosis, several pathologies can be wrong disseminated. Because it complexity use to have a difficult and late diagnostic that results doing preoperative diagnosis in less than 10% of patients [1]. The most common sites of this infection are cervicofacial (50-60%), mainly mandibular, abdominopelvic (20%) and thoracic (15%) [1-3].
The abdominal form is the most indolent and nonspecific presentation. In some cases it is accompanied by abdominal pain, fever, weight loss, altered bowel habit or a feeling of mass. It manifests as a firm, hard mass, attached to the abdominal wall and it is often confused with a malignant tumor lesion because, like them, the injuries seem to invade neighboring tissues. Predisposing factors in the development of the disease are usually associated with loss of mucosal integrity episodes. Appendicitis is the most common factor, although there are others such as diverticulitis and perforation of the transverse or sigmoid colon [4].
Currently, the impact of cecal actinomycosis on the general population, both adults and children, is not well known. In the more extensive series of appendectomy pieces respected by acute appendicitis clinic, appears in 1 case per 2,849 [5], however some series relate this pathology with the 5% of all appendectomies [6]. There are few reported cases of actinomycosis presenting as an abdominal mass in children, being normally the final diagnosis by pathologic examination of the surgical specimen, as in our case [2,7].
The critical to discard any risks associated factors, are as follow: poor oral hygiene, immunosuppressive therapy, HIV infection, malnutrition, previous abdominal surgery, perforated appendicitis, placement of an intrauterine device of long duration, etc. Even risks mentioned, until to 20% of cases develop with no associated co morbidity [3].
Definitive diagnosis requires bacterial isolation of the sample, either by their growth in the microbiological study or by histological assessment. Actinomyces spp colony by Methylamine silver staining or GrocottGomory, shows a typical picture denominated “sulfur granules”, as well as the associated, Splendore-Hoeppli phenomenon defined as the histological image between bacterial colony and exudate of polymorph nuclear eosinophilic material accumulation. These findings differentiate the presence of Actinomyces spp as part of the normal flora and therefore, we can attribute a pathogenic role for this bacterial colony [3,8].
The treatment of choice is intravenous penicillin G sodium (250.000 U/ kg/day) for 2-6 weeks, followed by phenoxymethylpenicillin (100 mg/kg/ day) or oral amoxicillin (50 mg/kg/day) to complete a total of 6-12 months [9,10]. In beta-lactam allergic patients, alternative treatment would be macrolides, lincosamides or tetracyclines [3].
Although the most important base of the therapy is prolonged antibiotic treatment, the majority of reported cases require combined surgical and antibiotic therapy, which is the most effective treatment, since the simultaneous surgical resection of the infected area decreases recurrence rates. In these cases the laparoscopic approach may be the best option, since it is a minimally invasive technique [1,11].
In our case we chose to perform outpatient treatment, given the perfect general condition of the patient and the realization of previous surgical resection.
The prognosis is favorable, although longer treatments (6-12 months) are needed because of the risk of associated complications, mainly the fistula. Even so, in cases with small numbers of colonies and after surgical resection, treatment duration is not well established, and shorter courses of antibiotic can offer excellent performance, as in our case [2,12].
The interest of this case is that the abdominal actinomycosis is a disease with low incidence in children and a variety of symptoms that can simulate different pathologies. For this reason the diagnosis is delayed in many cases. However, as an early diagnosis and primary treatment are essential to reduce the risk of associated complications, we suggest that actinomycosis should be considered in the differential diagnosis of abdominal mass. Abdominal actinomycosis can present as a firm mass in the intestine, being able to simulate a tumor, usually confused with a neoplastic process [4].
We have no financial conflicts of interest to disclose.
All authors have read and approved the manuscript.
For this type of study (case report) formal consent is not required.
All procedures were in accordance with the ethical standards and with the Declaration of Helsinki.
Download Provisional PDF Here
Article Type: Case Report
Citation: Álvarez MLM, Martínez EL, Sans MP, Campón MLP, Déjardin DDC, et al. (2017) Cecal Actinomycosis as an Unusual Cause of Abdominal Tumoration: Case Report. Clin Res Open Access 3(2): doi http://dx.doi.org/10.16966/2469-6714.121
Copyright: © 2017 Álvarez MLM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access