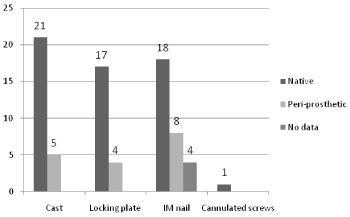
Figure 1: Graph showing fracture type and treatment

M Sajjad Athar* MA Fazal M Hassan N Ashwood
Department of Trauma & Orthopaedics, Burton Hospital NHS Foundation Trust, Burton-upon-Trent, UK*Corresponding author: M Sajjad Athar, Department of Trauma & Orthopaedics, Burton Hospital NHS Foundation Trust, Burton-upon-Trent, UK, Tel: 01283 566333; E-mail: msathar@hotmail.com
Aim: Distal femoral fractures are associated with high mortality rates in the elderly. Our aim was to evaluate the effectiveness of our management of distal femoral fractures and the mortality rates amongst various treatment modalities.
Methods: Seventy-eight patients were included in a retrospective study at our department of all distal femoral fractures between 2006 and 2012. Data was collected on: demographics, injury related data and outcomes.
Results: Demographics: Of the final study population, females constituted 81% of patients with 85% of patients older than 65 years old. Injury related data: 67% of patients underwent operative intervention of which 68% were operated on within 48 hours. Outcomes: Our overall 1 year mortality rate was 46% and the length of hospital stay was found to increase with increasing age. Both were found to be least with the use of locking plates and greatest in those treated conservatively.
Conclusion: These fractures are challenging to treat and are likely to increase given the ageing population. We propose their outcomes are improved when treated surgically particularly with the use of locking plates. We also suggest they should be managed similar to proximal femoral fractures, with early routine orthogeriatric review.
Distal femur fracture; Elderly; Mortality; Locking plates; Outcome
Distal femoral fractures occur in two population groups, the young and the elderly. The former usually resulting from high energy trauma and the latter from falls in osteoporotic individuals. They account for 1% of all fractures [1,2] and 4-6% of all femoral fractures [3]. They are the second most common type of femoral fracture in the elderly following proximal femoral fractures despite being 10 times less frequent [2,4]. These fractures usually require operative intervention to allow early mobilization and rehabilitation, where conservative management has largely fallen out of favor secondary to advances in implants and surgical technique [5]. Various techniques used to treat these fractures surgically include Dynamic condylar screw, blade plates, locking plates, intramedullary nails and knee replacement however .They are an injury type with significant morbidity and mortality particularly in this population when compounded by multiple co-morbidities. There have been reported mortality rates of up to 0.05% at 1 month, 16% at 6 months and 30% at 1 year of distal femoral fractures in the elderly, increasing with the presence of medical co-morbidities [6,7]. Better outcomes have been demonstrated through surgical management [3], however operative intervention is not without risks, which include infection, neurovascular damage, mal-union, non-union, and mortality. Stiffness and reduced range of motion is a risk with prolonged immobilization and early motion is therefore integral part of rehabilitation [8].
As with any fracture, treatment requires restoring and maintaining femoral alignment to preserve function. Treating these fractures are particularly challenging when having to consider healing potential and bone quality to achieve a satisfactory functional outcome [9]. This is further compounded when these are periprosthetic fractures making surgery even more challenging [10]. In a previous study looking at mortality after distal femoral fractures in elderly patients suggested a delay of greater than 4 days increased the 6-month and 1-year mortality risk, compared to surgery 48 hours after admission. The mortality of a native distal femoral fracture was found to be similar to that of a control hip fracture population and an important field to explore if management and outcomes can be improved [6].
Our aim was to evaluate the current effectiveness of our management of distal femoral fractures by measuring one year mortality rates amongst different treatment modalities. We also assessed time to surgery and therefore if early surgery provided better outcomes, preand post-operative mobility and complications to ascertain if improved management suggestions could be made.
We conducted a retrospective cohort analysis of all patients presenting with distal femoral fractures to our department between January 2006 and December 2012. A total of 91 patients were identified. Patients aged less than 18 years old, those who sustained osteochondral fractures, ligamentous injury through avulsion fractures and patients who required referral to tertiary centers for further treatment were excluded. A final study population of 78 patients was therefore included in our analysis. The average follow-up was 9 months.
Data was collected from a variety of sources including emergency department notes, admission assessments, radiographic imaging, operation notes, physiotherapy assessments and clinic letters. The data was subsequently divided into 3 broad categories including: demographics, injury related data and outcomes. Demographics included gender and age, which was subdivided into three groups, those younger than 65 years old, between 65 and 85 and those older than 85.
Injury related data included fracture type. Native fractures were classified according to the AO system and peri-prosthetic fractures according to the Lewis and Rorabeck classification. Treatment comprised conservative cast treatment and surgical fixation with intramedullary nailing, locking plates and cannulated screws. Time to operation in days was also recorded.
The primary outcome of the study was 1 year mortality rates which were assessed according to treatment type. Secondary outcome measures comprised length of hospital stay, complications and mobility. Length of hospital stay was calculated in days. Complications included infection, non-union, mal-union, knee stiffness and re-operation. Radiographs were analyzed digitally by a single surgeon (MH) to assess union. Radiographic union was considered when there was disappearance of the fracture line, bridging of the fracture site with callus or cortical continuity. Mal-union was defined as greater than ten degrees of angulations in each plane. Mobility outcomes were assessed by comparing pre- and post-operative mobility. Simple data analysis was conducted using descriptive statistics with the use of percentages, mean and range.
Eighty-one per cent of patients in our study were female and 48% over the age of 85, representing a population particularly vulnerable to fractures (Table 1).The average population age was 80, with a range between 22 and 101 years of age. The mean age amongst females was 83(range 56-101) and 67 in men (range 22-88).
| Characteristic | Subgroup | N = 78 |
| Gender | Male Female |
15 (19%) 63 (81%) |
| Age in years | 22 – 65 65-85Over 85 |
12 (15%) 29 (37%) 37 (48%) |
Table 1: Population demographics
Fifty-seven patients (73%) sustained native DFFs and 17 patients sustained peri-prosthetic fractures (22%). It was not possible to ascertain the type of fracture according to the AO/Lewis and Rorabeck classification in the remaining four patients (5%). Type A1 was the most common fracture configuration in the native group and type 2 in the periprosthetic fracture group. Forty-four per cent and 55% of fractures were right and left sided respectively. One patient in this group sustained bilateral DFFs. On average, 11 patients with native DFF and 3 patients with peri-prosthetic fractures were managed annually at our department. Two thirds of patients underwent operative intervention for their injury, refer to Figure 1, with 73% treated within two days 2 days, see Figure 2.

Figure 1: Graph showing fracture type and treatment
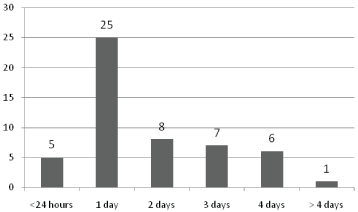
Figure 2: Graph showing time to surgery
40% of patients died in the operative group in comparison to 58% in the conservative group over the duration of the study. One year mortality rates were calculated based on those treated non-operatively, with IM nails and locking plates. Little conclusion of mortality rates in the single patient treated with cannulated screws could be drawn and therefore were excluded in Figure 3 below.
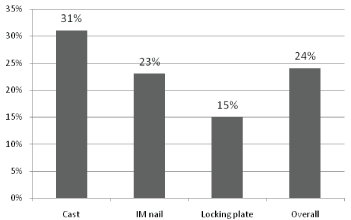
Figure 3: Graph showing one year mortality rates according to treatment modality
Length of hospital stay: Date of discharge was unavailable in three patients. 43% of patients were discharged within 2 weeks and 25% of patients were discharged beyond 6 weeks. The remaining 32% were discharged between these time frames, refer to Figure 4. A greater length of hospital stay was found with increasing age.
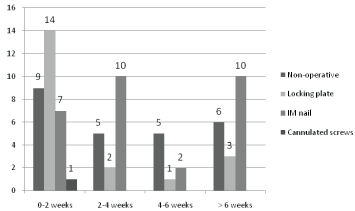
Figure 4: Graph showing hospital stay according to treatment type
Mobility: 21% of patients had either no pre- or post-operative mobility status recorded or had died. 24% of patient’s mobility had worsened post injury and management. The remaining 55% of patients regained their pre-operative mobility status.
Complications: The most commonly reported complication was stiffness in 9 patients. It is difficult to ascertain if this was related to the injury or treatment, or pre-existing stiffness from osteoarthritis. This was followed by 3 cases of non-union, two of which had reasons for nonunion including presence of secondaries and motor neuron disease. There were three further cases of mal-union, one each of metalwork failure, re-operation and on-table mortality. We had no cases of infection or neurovascular injury.
With hip fractures being a major leading public concern, development of a hip fracture care pathway has allowed care to be optimized for such a vulnerable population group by providing better functional outcomes, reduced peri-operative complications and improved healthcare expenditure. Elderly patients in comparison to the young with similar injuries have a longer hospital stay in addition to an increased mortality rate as they are frailer and require more resources particularly on discharge. This is particularly true of major long bone fractures integral to mobility. Although less common than proximal femoral fractures distal femoral fractures have similar rates of mortality in the elderly population. With an ageing population these injuries will be managed more frequently and is important they are managed adequately to reduce complication rate and improve clinical outcomes.
Our results clearly display improved outcomes with surgical management in comparison to conservative treatment, with a 7% reduction in one year mortality between the two. It has been suggested a surgical delay in the treatment of distal femoral fractures of more than 4 days increases the 1year mortality risk and suggested to be lowest when preformed within 48 hours of admission [7]. In our study population 13% of patients were operated beyond 4 days, which may contribute to our low overall mortality rate compared to the 30% suggested in the literature [7]. This stresses the importance of early surgery in such injuries, akin to the management of proximal femoral fractures, inevitably reducing risks such as chest infection and venous thromboembolism associated with prolonged immobility when confined to bed.
The most effected group of patients are elderly females as evidenced in our data, who are likely to suffer from osteoporosis. Distal femoral fractures treated with locking plates are thought to provide a safe and effective fixation that improves fracture healing and stability, allowing early mobilization in those with poor bone quality [11] and have increasingly been used in fractures involving diaphyseal and metaphyseal bone in osteoporotic individuals and as a way of bridging severely comminuted fractures [12]. However, it has also been argued that poor bone stock quality in osteoporosis can risk failure such as cutout from poor implant anchorage [13]. However, our results suggest patients treated with locking plates have better outcomes, with the lowest rates of mortality amongst the treatment options and a shorter length of hospital stay. It is suggested that plate osteosynthesis can interfere with the natural healing process of fractures due to its inherently stiff construct influencing the mechanical environment of callus formation [14] suppressing interfragmentary movement [15,16]. This is supported by non-union rates of 16-23% in recent studies with the use of locking plates in DFF [11,17,18]. Our results however showed no cases of non-union in those patients treated with locking plates.
Surgical technique may also have a bearing on outcome. Plates are popular as a minimally invasive approach can be adopted through submuscular insertion allowing for smaller incision, preservation of blood supply, minimal soft tissue damage and avoidance of disrupting the fracture haematoma [19,20]. In comparison reaming in intramedullary nailing can lead to thermal necrosis and alteration of bone architecture with increased risk of fat embolism [21]. Providing an optimal fracture healing environment will allow for earlier weight bearing again leading to a reduction in hospital stay and complications. It was not possible to ascertain if the plates in this population were inserted via a wide surgical exposure or minimally invasive approach which may have had some effect on non-union and infection rates.
Meneghini RM et al. [22] noted a greater failure rate among locking plates compared to IM nailing in periprosthetic fractures. A cadaveric study also suggested that femoral nails have better stiffness and fatigue life in comparison to non-locking nails and plates [23]. This is thought to be particularly advantageous in elderly patients with osteoporotic bone that are more likely to fail under loading [23]. In our population group, there was one case of stress fracture occurring at the proximal end of a locking plate 3 months post-operatively which required re-operation with further plating. Plate failure can occur as a result of delayed union or nonunion with loading [6] however union was achieved in this specific patient suggesting no greater failure rate. Our data supports that by Khursheed et al. [24] who describe good union rates amongst 25 patients treated with locking plates using a minimally invasive method, where the average time of union was noted in 17 weeks.
Several limitations are considered in our study. Given its retrospective design approximately 15% of the initial cohort was excluded leaving a relatively small population size, where additional studies are needed to confirm these findings. The follow-up period was relatively short, although this takes into account a number of mortalities which are likely to explain its length. We did not have any detailed data on patient comorbidities or presence of osteoporosis, which may potentially influence outcomes such as length of hospital stay and treatment modality as we know elderly patients are clinically challenging as they respond differently. Furthermore, we did not analyses the biomechanical properties of our fixations, such as working length for IM nails, implant material, screw ratio, plate length, that can also effect outcomes. Range of motion and functional knee scores are a difficult measure to get in these groups of patients however these were not the primary aim of our study.
There is ever increasing need to ensure the elderly population remain active members of society given the ageing population. Co-management by orthopaedic and geriatricians have shown to improve outcomes by reducing mortality and hospital stay [25]. With such fragility fractures, we recommend that such patients should be fast tracked to orthopaedic wards for optimization for surgery with early routine orthogeriatric review to minimize the delay to surgery. We also suggest prompt mobilization following surgery with multidisciplinary rehabilitation.
Distal femoral fractures are likely to increase given the ageing population. Our study confirms that these are challenging fractures to fix and the mortality rates are quite high. Often the fixation is needed in moribund patients in order to improve the nursing care and hygienic needs. We were able to demonstrate that a robust extramedullary fixation is better tolerated by the patients. Also early management of these fractures resulted in longer survival of these patients. Although our study was small we propose surgical management of these fractures provides better mortality outcomes amongst the elderly population, particularly when treated with locking plates. This however, does require further indepth analysis to confirm these conclusions. We also suggest patients should receive routine early orthogeriatric review to minimize delay to surgery to improve outcomes and mortality such that of the proximal hip fracture patients.
Download Provisional PDF Here
Article Type: Research Article
Citation: Athar SM, Fazal MA, Hassan M, Ashwood N (2017) Distal Femoral Fractures in the Elderly: Does Early Treatment with Locking Plates Reduce Mortality Rates? Clin Res Open Access 3(1): doi http://dx.doi.org/10.16966/2469-6714.119
Copyright: © 2017 Athar SM. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access