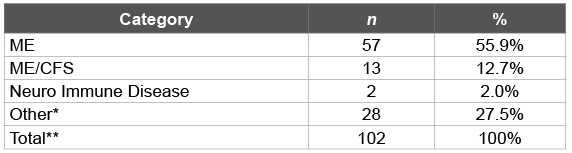
Table 1: First preference for the name
*All preferences in this category had one vote each.
**Skipped or No preference were taken out of this analysis (n=40)
Laura Nicholson* Abigail Brown Leonard A Jason Diana Ohanian Kelly O’Connor
Center for Community Research, DePaul University, Chicago, USA*Corresponding author: Laura Nicholson, Center for Community Research, DePaul University, Chicago, USA, Tel/Fax: 773-325-4154; E-mail: Lnicho10@depaul.edu
Surveys over the past two decades found that patients, advocates, and researchers want the name chronic fatigue syndrome (CFS) to be changed because this label minimizes the severity of the illness (Taylor, Friedberg, & Jason, 2001). The present study sought to qualitatively investigate patient views on the illness label CFS and healthcare providers’ knowledge of CFS. A patient-research organization asked members two open-ended questions regarding preferences for specific illness labels and educational suggestions for healthcare providers. Responses to both questions were coded thematically by multiple, trained research assistants. Findings suggested that 96% of participants disliked/ strongly disliked CFS. Myalgic encephalomyelitis (ME) was the majority’s first preference (55%) and was chosen four times more than any other name given. Four themes emerged for educational concerns: attitudes of healthcare providers, symptomatology, research, and implications of inadequate education. The most frequent subtheme (37%) was patients wanting healthcare providers to acknowledge that this is a real/serious illness. Diagnostic labels can influence providers’ perceptions of diseases and affect quality of care and communication between providers and patients. Therefore patients should be stakeholders in the process of name change. Understanding patient perspectives on educational priorities and illness labels will facilitate improved communication between providers and patients.
ME; CFS; ME/CFS; Diagnostic label; Patient perspectives; Physician attitudes
Chronic fatigue syndrome (CFS) is a debilitating disease that affects many systems in the body [1]. It has been suggested that patients with CFS are more impaired than those with type 2 diabetes mellitus, congestive heart failure, multiple sclerosis, and end-stage renal disease [2]. Given the severity of patients’ symptomatology, it is therefore, not surprising that many patients feel that the diagnostic label places too much emphasis on the symptom of fatigue [3]. Further, fatigue is experienced by many healthy individuals who gives the impression that CFS is not serious, and thus trivializes the illness [3]. The term CFS was coined by researchers at the Centers for Disease Control and Prevention in 1988 [4]. However, the syndrome was previously referred to as myalgic encephalomyelitis (ME) in Great Britain [5,6].
Illness labels for misunderstood diseases, such as CFS, can stigmatize affected individuals [7,8]. For instance, HIV/AIDS was originally referred to as “gay disease”,” gay cancer”, and “gay plague,” before it was established that the disease did not impact gay men only [9]. Multiple sclerosis (MS), which was originally thought to have been caused by oedipal fixations, was once called “hysterical paralysis” [10]. Once MS was better understood by the scientific community, the name was changed to reflect its’ physiological basis and less stigma was associated with the illness [10]. The etiology of CFS is still not well understood by the scientific community and consequently, the healthcare that patients receive has been considered unsatisfactory [11]. Several studies have elucidated this by examining the healthcare providers’ beliefs and knowledge about CFS. Bowen and colleagues found that about half of physicians were ignorant of diagnostic criteria for the illness and 28% did not accept this illness as a clinical diagnosis [12]. Another survey of healthcare providers found that 20% agreed with the statement, “I believe that CFS is all in a patient’s head” [13].
To successfully treat and manage chronic illnesses, productive relationships between patients and healthcare providers are necessary [14]. However, these relationships may be more difficult to establish and maintain when a disease is stigmatized or trivialized. Between 1998 and 2013, a number of studies were conducted to explore the ways in which the name CFS influences perceptions of the illness. In two studies, one surveying medical trainees [15] and the other surveying undergraduate students [16], participants were given a case description of a patient with prototypic symptoms of CFS. Participants were randomly assigned to different groups, with the only difference between groups being the type of diagnostic label given [e.g., CFS, ME, etc.]. Results of both studies indicated that college undergraduates’ [16] and medical trainees’ [15] attributions about CFS changed as a function of which diagnostic labels were used to characterize persons with this illness. In both studies the more medically-sounding term, ME, received the poorest prognosis and was more likely to be thought of as physiological rather than psychological in nature [15,16]. These results indicate that the diagnostic label ME elicited a more serious interpretation of this illness.
However, agreeing on an illness label has been problematic. The Name Change Workgroup (NCW) was a committee made up of scientists, clinicians, and patient representatives who distributed a questionnaire in January 2001 which assessed several possible names, including ME, neuro-immune endocrine disorder, polyalgicasthenia, and Ramsay’s Disorder. Results of this survey indicated that 92% of patients wanted a name change. Specifically, respondents favored two names: ME and neuro-immune endocrine disorder. However, less than 30% of researchers supported changing the name to either of these [17].
In 2014 the Solve ME/CFS Initiative distributed a survey to inform the Institute of Medicine (IOM) Committee of patients’ opinions on the name of this illness, as well as what they believed should be considered educational priorities for healthcare providers [18]. Within the final report, the IOM acknowledged that CFS is a trivializing name and suggested systemic exertion intolerance disease (SEID) to replace CFS [19]. Notably, this label has never appeared in results from previous studies. The present study analyzed the results of Solve ME/CFS Initiative’s survey with the intention to offer a patient-focused perspective on the name change issue. Previous research suggests that illness labels influence health care professionals’ opinions on etiology, severity, and ultimately on treatment decision-making. Therefore, it is appropriate to include patients’ perspectives on a matter that affects the care they receive from professionals.
IOM Committee – Cognitive, Sleep, and Diagnostic Issues Patient Survey was developed to inform a 2015 IOM Committee on patients’ opinions on two open ended questions: “In your opinion, what are the most important issues that healthcare providers should be educated about when it comes to diagnosis of ME/CFS? What are your thoughts on the current terminology used to describe this disease: Myalgic Encephalomyelitis/ Chronic Fatigue Syndrome? If you could suggest new terminology, what would you suggest and why?” [19].
For brevity, this survey did not ask any demographic information, but did record the IP address of the computer participants completed the survey on. The Solve ME/CFS Initiative distributed the survey on their website which was shared by other patient advocacy organizations so patient advocates from different perspectives could have taken the survey. In addition, the survey was named “IOM Committee-Cognitive, Sleep, and Diagnostic Issues Patient Survey” clearly demonstrating that the target population was patients.
The survey was created by the Solve ME/CFS Initiative and distributed on their website as well as on various internet bulletin boards in April 2014. Responses were collected over a twelve day period. The survey was anonymous and was made publically available to the research team after all data collection was complete.
Using a thematic analysis, a research assistant read through 50 unique responses to develop an initial set of themes for coding. After themes were selected, operational definitions were given to each theme to ensure reliability between coders. Two coders went through all responses and marked for the presence of each theme relying on these operational definitions. Only themes that appeared in at least five responses were included in the present analysis. After coding was completed, the two coders’ data sets were compared to establish Kappa values. Themes that had a Kappa level of at least .8 indicated that the correlation was reliable. Themes that were below a .8 Kappa were reviewed by a third coder who was considered a tie breaker. Themes were then grouped together based on similarities to create major categories.
For the second question, preferences for the name were coded. The first illness term individuals listed was categorized as their first preference by the researchers. The second, third, fourth, fifth, and sixth preferences were also recorded based on the order listed. Additionally, patient attitudes about the terminology most commonly used to describe this illness (ME, CFS, & ME/CFS) were coded using a 5-point scale (strongly dislike, dislike, indifferent, like, strongly like) which was developed by the researchers. If any of these three illness labels were mentioned in a response, they were coded using this scale by two coders. Similar to above, a third coder was utilized if the Kappa value fell below .8.
A total of 143 participants completed the survey, but no demographic information was collected. There were 2 duplicate IP addresses and the second response was excluded to ensure that the data could not have been filled out by the same participant multiple times.1.5% (n=2) of the sample skipped the first question and 1.5% (n=2) of the sample skipped the second. Since a substantial amount of participant responses were used in analysis (n=142), the authors reported the findings in percentages to highlight the frequency of the themes.
Question 1 stated, “In your opinion, what are the most important issues that healthcare providers should be educated about when it comes to diagnosis of ME/CFS?” [19]. There were 15 unique subthemes that were mentioned at least five times by respondents in response to this question. These subthemes were organized into four major themes: (a) attitudes of healthcare providers, (b) symptomatology and its impact on patients, (c) research, and (d) implications of inadequate education. However, each participant’s response could be coded into multiple themes if they brought up multiple issues or concerns, thus many participants’ responses were coded into all four categories.
Attitudes of health care providers: The first grouping of subthemes addressed patients’ concerns about healthcare providers’ attitudes and the subsequent treatment they receive. Many of the educational suggestions in this thematic group spoke to the stigma or disbelief patients experienced when engaging with providers. About 55% (n=78) of the sample expressed concerns within this category.
Real and serious illness: Notably, of all the observed subthemes, patients cited most often that this is a real and/or serious illness.37% (n=53) of participants brought up this subtheme. Common responses included, “How serious the illness actually is” and “That it’s REAL”
Not psychological: A quarter of the sample, 25% (n=36), stated healthcare providers should not attribute their symptoms to psychiatric causes (i.e., depression). Similarly, many respondents stressed that this illness was not “all in their head.”The most common phrases for this theme were, “That it is NOT depression” or “that doctors should know that CFS is not a psychiatric illness!”
Poor treatment in health care settings: 11% (n=16) of participants reported that medical professionals poorly managed this condition. One participant asserted, “Doctors scorning patients who have been diagnosed, using it as a reason not to treat them for other conditions; the doctor needs to understand the danger of shunning patients.”
Listening to patients: About 6 % (n=8) of respondents felt that doctors should listen to patients:
“First they should listen to what the patient has to say. I have been stuck with the same MD for 10 yrs and [she] doesn’t say anything about CFS/ ME. I give her symptoms and she thinks I am drug seeking.”
Ignorance of this condition: Similar to the subtheme above, 6% (n=8) described how doctors or institutions were ignorant of their condition. Participants pointed out, “Pure ignorance is what surrounds our illness” and, “doctors [are] ignorant of the condition.”
Symptomatology and its impact on patients: Similar to the first thematic category, 55% (n=79) of the sample referred to at least one of these subthemes, which emphasized ME or CFS symptomatology and its impact on patients’ lives.
Severity & complexity of symptoms: 20% (n=29) of the sample stressed that health care providers should recognize the severity and/ or complexity of their symptoms. Participants often replied to question one by asserting, “How serious the illness actually is and that it affects all bodily functions.” Other participants listed many different symptoms that affected them which portrayed the complexity of this illness:
“Healthcare providers need to understand that ME/CFS is more than just one problem. It is a syndrome. They need to understand the fluidity of symptoms and how they manifest. Even if pain is well controlled, fatigue and/or cognitive function may still exist to such a degree to cause a high state of impairment.”
Post-exertional malaise: 24% (n=34) of respondents discussed the need to increase knowledge and awareness of post-exertional malaise (PEM), a cardinal feature of the illness. One participant suggested:
“Exacerbation of symptoms with activity, sometimes show very little activity, also known as PEM or PENE. They need to know what it is, how to assess it and to warn patients not to push through it or they can make themselves significantly worse.”
Debilitating lifestyle & financial strain: Often times, symptoms were mentioned with regard to how they impacted the daily lives of patients. Though these themes were not always brought up together they were considerably interrelated. 13% (n=19) of respondents explained that the symptoms are debilitating and affect their functioning. 7% (n=10) mentioned how this illness is financially disabling:
“I want everyone - including health care providers to understand how disabling the disease it and how it affects every aspect of my life. My relationships, self image/esteem, my career (or lack of one), stress levels as well as day to day living.”
Research: The third theme illustrates the need for more research or the application of already existing research in learning about biomarkers and treatment options. 35% (n=50) of the participants’ responses mentioned at least one or more themes within this category.
Treatment and testing options: 26% (n=37) of respondents stressed the need for new and effective treatment options and better diagnostic testing.
Existing research: In terms of the existing research on ME and CFS, 8% (n=12) of patients recommended that health care providers read the existing literature on this illness; “[t]o be educated about bio physiology of M.E and up to date with biomedical research studies, and to use the ICC or CCC criteria for diagnosis.”
More research and funding: Lastly, 7% (n=10) of patients stated that there needs to be more research and funding to understand ME and CFS. One participant explained, “Give ME the sort of research funding and media respect that is given to MS and MDN and they will find real treatments for the disease.”
Implications of inadequate education: In the fourth major category, 18% (n=25) of the sample endorsed one or more themes in this category. These themes demonstrated the implications of inadequate care received from medical professionals due to the lack of education surrounding this illness.
Delayed diagnosis: Due to inadequate education about CFS or ME, 4% (n=6) of patients mentioned that they had to wait a substantial amount of time to receive a diagnosis.
Ignoring other conditions: 7% (n=10) of respondents wanted doctors to recognize that a ME or CFS diagnosis in combination with other medical conditions, drug regiments, etc. may put the patients’ health at risk if not taken into consideration.
Need for specialists: Finally, 7% (n=10) of respondents brought up the need for access to a specialist or specialized care. One respondent wrote, “Medical schools should include CFS/ME as an area of specialization…so more doctors would study it and be able to effectively treat it.”
Question two asked “What are your thoughts on the current terminology used to describe this disease: Myalgic Encephalomyelitis/Chronic Fatigue Syndrome? If you could suggest new terminology, what would you suggest and why?” [19]. Participants listed as many as six preferences, however 60% (n=86) just listed one suggestion. 27% (n=38) of participants did not explicitly list a favored name for this illness. Their preference was coded as “None Listed”.
First preference: About 72% (n=102) of all participants gave a name preference (or preferences) and suggested a total of 49 different illness labels. Within this group, 56% (n=57) of respondents’ first preference for the name of the illness was ME. The next most endorsed illness label was myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), which received votes from only 13% (n=13) of respondents. The next most popular choices were neuro immune disease (n=2) and chronic fatigue syndrome (n=2)-a combined 4%. Notably, there were 28 different name suggestions that were each listed once, which collectively accounted for 27.5% of the first preferences (Table 1).

Table 1: First preference for the name
*All preferences in this category had one vote each.
**Skipped or No preference were taken out of this analysis (n=40)
All preferences: All name choices, regardless of preferential order, were subcategorized to understand the breakdown of all name suggestions (Tables 2 and 3). Results were similar to above after combining all preferences (again excluding those who skipped and gave no suggestion); ME was suggested by 49% (n=63) of the respondents and ME/CFS was still favored by 13% (n=17) of respondents. Illness labels that were under the neuro endocrine immune disease (NEID) category were listed by 10% (n=13) of respondents. Eponyms, or having the illness be named after a researcher, clinician, or patient, were selected by 5% (n=6) of participants as were illnesses that were in the ‘multi system’ category. 4% (n=5) of participants chose a name where collapse or breakdown appeared. CFIDS was chosen by 2% (n = 3) and CFS was chosen by about 2% (n=2). The ‘other’ category accounted for 10% (n=13) of the total preferences and included names like encephalomyelitic cytokine inflammatory cascade, viral immune deficiency syndrome, etc.
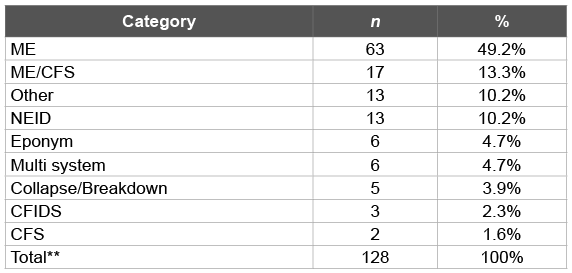
Table 2: All name preferences subcategorized. Participants could have
chosen multiple names
**Skipped or No preference were taken out of this analysis (n=40)
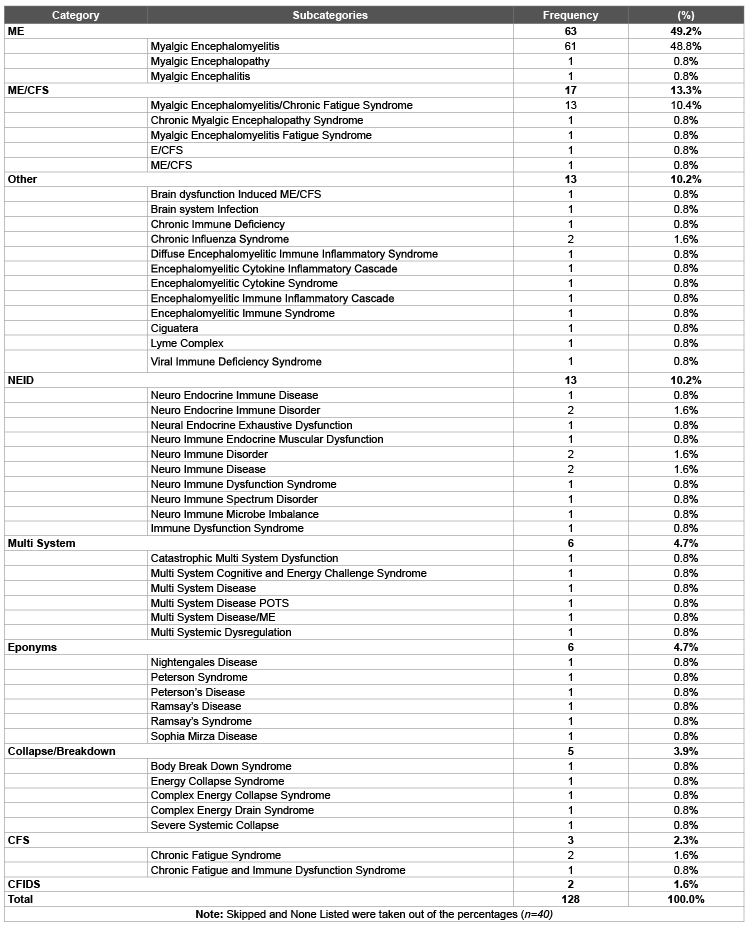
Table 3: All name preferences categorized. Participants could have chosen multiple names.
Attitudes on current illness labels: Those who did not list a name preference often still gave their opinions of other illness labels. There were respondents who exhibited frustration with this question; “You know our thoughts, this is a 20 year old question.” and “Doesn’t matter what they call it. Just find cause and cite.” Similarly, 9.8% (n=14) of participants often mentioned that more research was necessary to select an appropriate name.
Moreover, particular attitudes about the current names were coded when participants spoke of the three most currently used terms: ME, CFS, and ME/CFS. A 5-point scale was applied by the coders to determine the degree to which participants favored each name.
Chronic fatigue syndrome: 65% (n=92) of the sample gave an opinion on the illness label CFS. 53% (n=49) strongly disliked, 42% (n=39) disliked, 3% (n=3) were indifferent, and 1% (n=1) liked the label CFS. There were no participants who strongly liked the name CFS. Many respondents who strongly disliked the term spoke to how this illness label is trivializing:
“CFS should not be used alone because it is confusing. Other diseases are not typically named for a single symptom (do we call COPD “chronic coughing disease”? or diabetes “chronic peeing disease”? of course not. That would be silly and confusing, and many of the patients--and physicians--would doubtless find it trivializing.) We tend meet lots of people who say, “I hiked/stayed up late a few nights this week/work too much... I feel tired... I think I have CFS, too!” Many of them do not appear to be joking [SIC].”
8% (n=12) of the sample stated that they wanted the word fatigue to be omitted from the name; “Whatever you call it, just leave out the word fatigue and we’ll be happier about it. That word just makes us look lazy.”
Myalgic encephalomyelitis: About 54% (n=77) of our sample gave an opinion on the term ME. Of those participants, 1% (n=1) strongly disliked, 10% (n=8) disliked, 9% (n=7) were indifferent, 65% (n=50) liked and 14% (n=11) strongly liked the name ME. Notably, about 30% (n=42) of respondents in the entire sample said that ME was a better label than CFS with statements like, “I prefer ME over CFS.”
Myalgic encephalomyelitis/chronic fatigue syndrome: Finally, 13% (n=18) of participants gave an opinion on the combined name choice of ME/CFS. Of those participants, 6% (n=1) strongly disliked, 22% (n=4) disliked, 28% (n=5) were indifferent, 33% (n=6) liked and 11% (n=2) strongly liked the name. Some participants did not feel that ME/CFS was a suitable label for their illness, “Combining two medical terminologies is confusing.” Furthermore, 4% (n=5) of respondents mentioned that ME and CFS were fundamentally different illnesses and thus deciding which name was more appropriate could not be determined; “Cfs is more fatigue m.e is the illness. I think there 2 different illnesses [SIC].”
Results of the current study echo previous research demonstrating patients’ dissatisfaction with the name CFS and perceived obstacles within the health care system. This is clearly seen when comparing the 96% who disliked or strongly disliked the label CFS to the 1% who liked the name (no one strongly liked the term). One specific criticism was the use of the word “fatigue”; 8% of participants stated they wanted it omitted from the name. By placing emphasis on the symptom of fatigue, which many healthy individuals experience during their life [3], the name CFS can stigmatize patients by eliciting negative attitudes, thereby influencing how they are treated by medical professionals, work associates, and even family [20-22].
In the present survey, 55% of the sample discussed attitudes of healthcare providers when asked about educational concerns. In the most prevalent subtheme that emerged, 37% of all participants wanted healthcare providers to acknowledge that this was a real and serious illness. A previous survey by Brimmer et al. [13] found that 20% of healthcare providers agreed with the statement, “I believe that CFS is all in a patient’s head”. This finding is particularly alarming when considering that in the present survey, one quarter of respondents stressed that this illness was neither psychological nor “all in their head”. Anderson and Ferrans [23] reviewed the quality of life for those who have CFS and found that 77% reported past negative experiences with healthcare providers-another concern mentioned by our participants. While the present survey did not explicitly prompt patients to speak about negative experiences with providers, these themes still emerged.
Previous research suggests that the label CFS is harmful to the patient community as it negatively influences the opinions of healthcare providers that are responsible for providing care. The findings from the present survey raise important questions about the quality of care patients are receiving. In order to encourage better quality treatment for those with this illness, changing the illness label could be a vital first step. The majority (55.9%) of participants’ first preference was ME, and more remarkably, it was preferred four times more than any other label. 79% of those who mentioned ME in their responses liked or strongly liked the label compared to the 11.7% that disliked or strongly disliked the label. As mentioned previously, Jason et al. [15] found that medical trainees were more likely to recognize a medically sounding name (i.e. ME) as having a poorer prognosis. In line with this survey, utilizing a medically sounding label provides multiple benefits: a consensus among patients with regard to the name and a more serious appreciation of this illness by providers.
The recently published Institute of Medicine Report addressed the label ME in their report but felt there was not enough empirical support to assert this label as medically accurate [19]. Since the etiology of the disease is still debated, a number of scientists feel there is not a clear answer as to what the name should be. Yet, there are many other illnesses that do not have a medical basis to their diagnostic label (e.g. malaria means ‘bad air’) [24]. The participants that took part in the present survey suggested 49 different name choices which illustrates the willingness to find a label that is most appropriate for this illness. The IOM’s name suggestion, systemic exertion intolerance disease (SEID), has already become controversial among patients and advocates due to how the name was selected and the specific terms within this label [24]. The present survey was developed to provide name suggestions to the IOM and yet none of the patients mentioned SEID as a possible replacement in this survey.
Several limitations of the current study should be noted. Our group did not take part in the development of the survey and therefore it was not designed to be used for qualitative analysis. To allow more symptomatic participants respond to the survey, no demographic data was collected in order to make the survey brief. However this and our sample size limits our understanding of whether or not this is a representative group of patients and makes it difficult to generalize our findings. Since these analyses are retrospective in nature, we were unable to ask specific questions about our areas of interest which may have lessened the validity of the themes and preferences we did find. To this point, the five point Likert-scale scales used to measure the degree of support for the three major illness labels was created by our team and thus not a scale patients rated themselves. For these reasons, the present survey is exploratory in nature and demands a more in-depth survey to assess patient perspectives on such issues.
The results from this study show that participants’ health care providers’ attitudes and lack of knowledge about etiology/symptoms can affect the way a patient is treated. The results of this study indicate that the majority of participants’ first preference was ME and they were largely satisfied with this label. Though the 49 other diagnostic terms suggested by participants could represent an openness to finding the best label for this illness. In order to have a transparent conversation regarding the most suitable name, patients and advocates who are directly impacted by these decisions should be actively involved in the naming process. Future research should investigate patients’, researchers, and physicians opinions on such issues.
A recent study [25] found that there might be different groupings of patients who have significant limitations in energy and endurance. That study [25] suggests that CFS criteria select less impaired patients than ME criteria. In other words, these latter criteria identify a much smaller percent of patients with more sudden onset of infectious symptoms. Because the IOM clinical criteria [19] might be even broader than the CFS criteria [26], it is possible that there might be different illnesses, with some meeting clinical criteria and others that select more homogenous samples that could be used for research purposes. It is still unclear that names might be associated with these different types of conditions, but surveys and polls might help us better develop consensus on how to deal with these complex issues.
The authors declare no conflict of interest.
The authors appreciate the Solve ME/CFS Initiative, who collected the data in this study.
Download Provisional PDF Here
Article Type: Research Article
Citation: Nicholson L, Brown A, Jason LA, Ohanian D, O’Connor K (2016) Educational Priorities for Healthcare Providers and Name Suggestions for Chronic Fatigue Syndrome: Including the Patient Voice. Clin Res Open Access 2(1): doi http://dx.doi.org/10.16966/2469-6714.112
Copyright: © 2016 Nicholson L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access