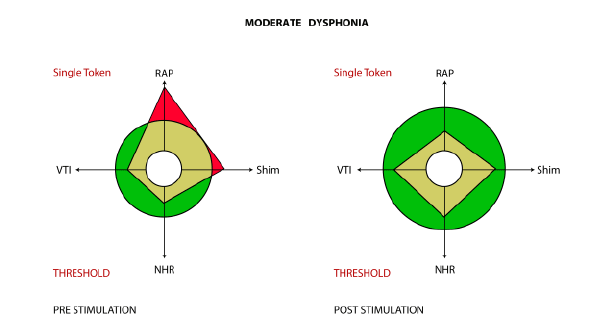
Figure 1: MDVP graphs of pre and post stimulation of moderate dysphonia.
Natalie Schaeffer*
Department of Speech Communication Arts and Sciences, Brooklyn College, Brooklyn, NY, USA*Corresponding author: Schaeffer N, Department of Speech Communication Arts and Sciences, Brooklyn College, Brooklyn, NY, USA, Tel/Fax: (718) 376-1601; E-mail: natalies@brooklyn.cuny.edu
Objective: The purpose of this study was to compare acoustic data for the following vocal parameters to assess vocal noise in dysphonic participant’s pre and post stimulability training: Relative Average Perturbations (RAP), Shimmer, and Noise-Harmonic Ratio (NHR) using the Multi-Dimensional Voice Program (MDVP) were assessed. The objective was to determine if stimulability training could improve the parameters on the MDVP and corroborate perceptual improvements in vocal quality with the acoustic data. Such data could provide evidence of the MDVP’s value as a measure of parameter changes resulting from stimulability training. There is little research on this instrument’s efficacy for documenting change after stimulability training.
Method: The investigator assessed 20 participants (male and female) between the ages of 20 and 30 (mean age=25) who were perceptually rated as dysphonic. The diagnostic team rated the participants upon listening to their monologue, conversational speech, and a reading passage. The participants prolonged the vowel /a/ on the MDVP to obtain acoustic parameters. They were subsequently stimulated to use proper coordination of respiration and phonation and actively engage their abdominal muscles upon phonation of /a/. After stimulation, the participants again phonated /a/ on the MDVP using the stimulation technique. The same parameters were compared before and after stimulability training.
Results: Results of the MDVP (before stimulation) revealed aberrant vocal parameters for all the participants, corroborating informal vocal perception of dysphonia by the diagnostic team with the MDVP results. After stimulation training, the participants’ voices were again measured on the MDVP as they used the stimulation technique. Decreased RAP, Shimmer, and NHR levels were observed for all participant, although NHRs were either minimal or within normal limits before stimulation. Perceptual improvements in vocal quality post-stimulation were also reported by the evaluators.
Conclusion and implications: The MDVP can measure parameter change with regard to vocal improvement after the present stimulability training. Acoustic improvement corroborated perceptual improvement.
MDVP; Stimulability; RAP; Shimmer; NHR; Dysphonia; Parameters; Acoustic
Traditionally, vocal quality has been assessed subjectively through auditory-perceptual means. With the introduction of computer-based acoustic instruments, clinicians can supplement subjective analysis with objective data. The Multi-Dimensional Voice Program (MDVP) is an acoustic analysis program that can effectively be used in the assessment of individuals with dysphonia. The instrument provides objective measurements of several vocal parameters, for example, Fundamental Frequency, Relative Average Perturbations (RAP), Shimmer, and NoiseHarmonic Ratio (NHR).
Previous studies have discussed the reliability of the MDVP as an assessment tool: Gonzalez et al. [1] examined the reliability of the MDVP based on test-retest measures in healthy adults. Results disclosed high stability of frequency parameters and adequate stability of frequency and amplitude perturbation, noise-harmonic ratio, and vocal irregularities. Barsties and DeBodt [2] describe the MDVP as one of the most reliable and frequently used instruments for obtaining vocal perturbation analysis. The MDVP has been compared to other acoustic instruments such as PRAAT and Dr. Speech. A recent study looked at the reliability of the MDVP when measuring normal voice. According to these authors, the MDVP provided reliable intra-day data (data derived from the same client in the same session) for jitter measurements (including RAP). This program was also found to be more reliable in terms of quantifying vocal variability and irregularity than older instrumentation such as the VisiPitch [3]. Nicastri et al. [4] stress the importance of reducing any type of variability when conducting the MDVP procedure and found that past variability factors have been significantly reduced.
Bhuta et al. [5] looked at whether there was a correlation between the vocal aspects on the GRABAS scale (grade, roughness, breathiness, asthenia, and strain, a subjective measure) and the MDVP scale. These researchers determined that certain noise parameters of the MDVP (i.e., voice turbulence index (VTI), noise harmonic ratio (NHR), and soft phonation index (SPI)) correlated with the perceptual rating system of the GRABAS scale. Vaz Freitas et al. [6] found that the MDVP required fewer numbers of acoustic measures (e.g., shimmer) to correlate objective data with audio-perceptual parameters such as the GRABAS scale.
Validity was also indicated in a study by Schaeffer et al. [7] these researchers studied participants with perceptually normal voices between 60 and 80 years of age on the MDVP and compared them with younger participants between the ages of 20 to 30. Results revealed that the older participants, whose voices were perceptually normal, showed greater levels of RAP, Shimmer, and Noise to Harmonic ratio, reflecting the thinning of the vocal folds with age in comparison to the younger participants who showed little or no parameter issues [8,9]. That is, the thinning of the vocal folds in older individuals was reflected in the MDVP’s parameters despite their perceptually normal voices.
Although the MDVP is often used to provide objective acoustic data during the initial evaluation of clients with dysphonia, the implications of this instrument extend beyond the diagnostic room. Extant literature indicates that the MDVP also allows for the quantification of progress in therapy related to surgical correction of interfering physical aspects in children such as hypertrophic tonsils and enlarged adenoids [10] and in non-linear dynamic analysis in children [11]. Tezcaner et al. [12] and Senkal and Ozer [13] are among the many researchers who have utilized the MDVP in their studies to compare vocal parameter measures before and after voice therapy; they concluded that computer-assisted voice analysis programs, such as the MDVP, are sensitive indicators for detecting changes in vocal quality.
According to Zelcer et al. [14] the MDVP may also be a useful tool in diagnosing vocal fold dysfunction that can imitate asthma, a condition which may lead to unnecessary pharmacologic treatment or intubation; therefore, the acoustic measurement may be an interim step to shed light on the problem. Additionally, Dogan et al. [15] assessed voice quality in clients with mild to moderate asthma through acoustic analysis using the MDVP, as well as with other assessments (e.g., vital capacity, s/z values) and with subjective evaluations (e.g., Voice Handicap Index and the GRB parameters of the GRABAS scale). These authors concluded that monitoring voice changes by objective measures is especially important in patients with asthma, especially those who have been on long-term inhaled steroids and need appropriate follow up of this disorder.
The MDVP has also proven to be a valuable tool in analyzing vocal parameters before and after medical and surgical treatments. Types of disorders which have been researched with this instrument include chronic cough, [16,17] Reinke’s edema, [18] and dysphonia related to endotracheal intubation [19]. These authors found that the value of shimmer gives evidence to even small intubation-induced edemas on the vocal folds. The MDVP has also been used to indicate a degree of positive change in vocal quality in people with quadriplegia after singing therapy [20]. Petrovic-Lazie et al. [21] used the MDVP to demonstrate improved vocal quality in patients after surgical and therapeutic treatments for vocal polyps, and to demonstrate the reduction on noise to harmonic ratio (NHR) after treatment of people with vocal fold lesions. Bonilha and Dawson [22] found in their study that the average NHR range of measures approximated the mean more closely.
Gillespie and Gartner-Schmidt [23] conducted pre and post stimulation research on the MDVP by having dysphonic participants use “clear speech” as their stimulation task. The participants were instructed to “use clear, crisp consonants” and “precise articulation.” The researchers found no significant difference in the results post stimulation using the MDVP technique. These same authors, however, conducted a stimulation study on an aerodynamic instrument (the Phonatory Aerodynamic System) using the same stimulus material as above and found significant positive results such as appropriate vocal intensity, airflow rate, pausing to replenish breath supply, and appropriate rate of speech with regard to aerodynamic measures. Boniha and Dawson [22] however, found that after stimulation with forward focused voice, RAP and Shimmer measures on the MDVP showed improvement. These authors contend that having clients see positive results can encourage motivation and confidence in the voice therapy. Furthermore, the results of stimulation allow the clinician to assess approaches to therapy for documentation [23].
Dejonckere and Lebacq [24] introduced a rating scale to determine vocal plasticity (i.e., how participants respond to stimulability). Participants who presented with vocal pathologies (e.g., polyps, edema, unilateral vocal fold paralysis, cysts) were graded on whether different conditions could affect vocal quality in a short period of time (e.g., changes in posture, articulatory range of motion, vocal intensity). Their results showed a significant correlation between stimulability to improve vocal quality as well as improvements in voice post-therapy. The authors, however, did not describe or rate which types of conditions were most effective in creating immediate improvements in voice.
Although there are studies examining the use of the MDVP for initial evaluations and for pre-and post- intervention measures, there is minimal research investigating its use for documenting vocal parameters before stimulability and after stimulability training. Future studies are needed to address this inquiry to determine if the MDVP can reveal (1) parameter changes with stimulability, (2) the perception of improved vocal quality, and (3) whether motivation for therapy increases if the client observes positive changes. Given these gaps in the literature, the principal investigator sought to obtain a productive training method to determine both the potential of the client and the effectiveness of the stimulation training technique. The author compared acoustic data for vocal noise parameters (i.e., RAP, Shimmer, NHR) on the MDVP pre and post stimulability training. The training consisted of supporting the voice through the coordination of respiration and phonation and actively pulling in the abdominal muscles upon phonation. As noted above, Gillespie and Gartner-Schmidt [23] found that using “clear speech” on the MDVP in a pre-post stimulation study (which they noted was the first study of this kind) did not yield significant differences. Further research on stimulability training is needed, considering the scarcity of research in this area in terms of stimulation results, the stimulation technique, and the clients’ responses and motivation.
The principle investigator used a certain stimulation technique to increase vocal fold periodicity (revealed on the MDVP), and perceptually as well, when phonating /a/, the vowel required by the MDVP instructions. Prior to being exposed to any voice stimulation techniques, each participant phonates/a/ into a microphone (three times for reliability). The computer software yields an image indicating vocal fold vibration. The clinician then stimulates the participant through modeling and feedback to obtain an improved vocal quality using the stimulation training technique, which consists of coordinating respiration and phonation and pulling in the abdominal muscles upon phonation of /a/. Once the participant improves his/her voice using the technique, he/she will repeat the MDVP method of data collection using the stimulation technique, again three times for reliability. The MDVP yields the stimulated results as an image or graph which reveals vocal fold vibration. Acoustic data will then be compared pre-and post stimulability training. It is expected that the MDVP will show improvements (greater periodicity which is reduced RAP, NHR, and Shimmer) on the post-stimulation administration. According to Georgieva and Stefanovska [25] this immediate visual feedback may serve to increase client awareness and improve motivation. It would appear that in addition to being a reliable measure of vocal fold vibration, the MDVP can be used as a source of visual feedback for clients by generating a pictorial representation of the analyzed vocal parameters.
A total of 20 dysphonic participants/students were selected to partake in the study during a voice diagnostic evaluation in Brooklyn College. These participants were Brooklyn college students who had been screened and noted to have dysphonia; therefore, a voice evaluation by the diagnostic team in the Speech and Hearing Department was recommended. The participants were between 20 and 30 years of age (mean age 25) and were perceptually rated as dysphonic (mostly moderate to severe) by the diagnostic professor and the graduate students. All these raters were experienced with diagnosing dysphonia and rated the participants upon listening to their monologue, conversational speech, and a reading passage. None of the dysphonic students had respiratory, neurological, or structural problems, nor had any of them received prior voice therapy. Additionally, they did not smoke. The diagnostic team diagnosed the participants with phonotrauma and recommended an ENT evaluation.
To obtain acoustic values which indicate vocal noise in the signal (RAP, Shimmer, and NHR), the participants prolonged the vowel /a/ on the MDVP. As instructed by the Kay Pentax Corporation manual [26], the participant sat 6 inches from the microphone (Shure SM48). For the MDVP procedure, each participant was seated in a chair which faced the investigator and asked to sit up straight with legs uncrossed and hands away from the face. Before each sustained /a/ phonation, the investigator measured the distance between the participant’s mouth and the microphone, utilizing the 6 inch measure to ensure the proper distance for phonation. Each participant was given instructions regarding the procedure, and the investigator gave instructions and an example of how to participate in the procedure (i.e., “Take a normal breath through your mouth and say /a/ when I tell you to start and stop when I ask you to stop”). The participants practiced the steps in the procedure to make certain that they were on task, using their natural or habitual voice. When the procedure started, each participant began his or her phonation at the beginning of the capture window on the computer to the end of that window, following the investigator’s instruction for that task. This procedure was repeated three times for reliability of the result.
After each trial was completed, the MDVP yielded a computergenerated image on a Dell OptiplexGX620 computer; this graphic image was printed on an HP Deskjet 6988 printer to retain the acoustic data. The MDVP also printed numerical values for all the parameters (e.g., RAP, shimmer, harmonic to noise ratio). According to Kay Pentax, numbers representing acoustic values are related to the results on the graphic read-out. Data which aligned within the threshold numbers (all green on the graphic read-out) (Figure 1) were considered to be within normal threshold limits. If red appeared in the graphic signal (Figure 2), the values were outside the threshold limits. For purposes of this investigation, the acoustical values for RAP, Shimmer, and Noise to Harmonic ratio were evaluated for this study; these parameters were chosen primarily to assess aperiodicity (noise) in the vocal signal and to compare them to normal voices.
Subsequent to the three initial trials for each participant, the principle investigator stimulated every participant (through modeling and feedback) to use a technique to increase vocal fold periodicity upon the production of /a/. As previously noted the method consisted of coordinating respiration and phonation and pulling in the abdominal muscles upon phonation of /a/. Once the participant improved his/her voice upon stimulation, he/she repeated the MDVP method of data collection using the learned stimulation technique, again three times for reliability. The MDVP yielded the stimulated results as an image or graph indicating vocal fold vibration. Acoustic data was then compared pre-and post-stimulability training. It was expected that the MDVP would show improvements (greater vocal periodicity, that is, reduced RAP, NHR, and Shimmer) on the post-stimulation administration.
Results of the MDVP data were the following: A paired sample T test revealed a significant difference at the .001 level between pre and post stimulation with regard to RAP and Shimmer, revealing a significant improvement in vocal periodicity on the MDVP as a result of the stimulation technique for both parameters (Table 1 and Figure 3). See figures 1 and 2 for examples of pre and post stimulability graphs of moderate and severe dysphonia. NHR was not significant, as this parameter was usually within threshold means or slightly elevated.

Figure 1: MDVP graphs of pre and post stimulation of moderate dysphonia.
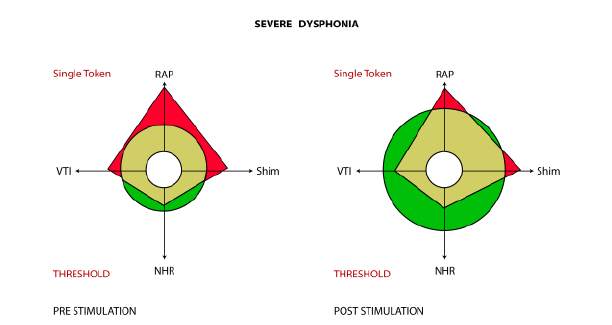
Figure 2: MDVP graphs of pre and post stimulation of severe dysphonia.
Parameter |
Pre Stimulation |
Post Stimulation |
Mean RAP |
1.274921 |
.97858 |
Mean Shimmer |
5.440 |
3.4418 |
Discussion
This investigation was undertaken to determine if stimulability training would reveal significant differences on the MDVP at an initial evaluation prior to voice therapy. In this study, the MDVP revealed aberrant vocal parameters, that is, abnormal values for RAP and Shimmer, for participants with dysphonic voices, thus corroborating the diagnostic team’s informal subjective vocal assessment of dysphonia. There were, however, minimal or no levels of NHR. After stimulability training, the diagnostic team found that the participants demonstrated perceptually improved voices upon production of /a/, supported by the significant improvement on the MDVP’s vocal parameters, particularly shimmer and RAP. Objective data confirmed subjective assessment both pre and post stimulability. It appeared that these results were reliable, especially as the literature attests to the reliability of this instrument, and that the data answered the questions asked:
It appears that the stimulability task must be appropriate for the instrument. As noted, Gillespie and Gartner-Schmidt [23] found no significant difference on the MDVP using “clear speech” as a stimulation technique. In the present study, the stimulation technique of respiratory support (the coordination of respiration and phonation) and the conscious use of abdominal support facilitated improved vocal periodicity on a single vowel. Perhaps using “clear speech” is not conducive to stimulation on an acoustic instrument. However, these authors noted significant differences pre and post stimulation when using “clear speech’ on the Phonatory Aerodynamic System, suggesting that the stimulation method needs to be appropriate for the instrument.
A pre and post stimulation procedure may also be a motivational factor. Participants viewing differences in their graphs pre and post stimulation may realize that improvement is possible. Viewing these vocal gains in vocal quality may also reduce any fears regarding therapy and increase motivation. For example, the literature indicates that client motivation tends to be low in those clients with muscle tension dysphonia (MTD) and appears related to poor adherence to voice therapy practice [27]. According to Georgieva and Stefanovska [25], visual feedback on the MDVP may serve to increase client awareness and stimulate motivation. That is, the MDVP can be used as a source of visual feedback at the outset for clients by generating a pictorial representation of the analyzed vocal parameters before and after stimulation.
The MDVP may also be used in a stimulation task for older individuals with dysphonia to compare with older individuals with perceptually normal voices [6] in terms of the parameters older non dysphonic participants obtained. Stimulation training can also be incorporated with individuals who have particular problems as chronic cough, [14,15] and dysphonia related to endotracheal intubation [17]. This training may allow clinicians to assess stimulation approaches to therapy for documentation, allow clinicians with some considerations with regard to a therapy plan, reveal the potential and motivation of clients, and allow clients to participate in evaluating their voices. In the present study, a number of clients were motivated to enroll in therapy and see an ENT doctor to examine their vocal folds. Stimulation training can allow clinicians to assess stimulation and provide them with some considerations before beginning a therapy plan. As per Mcllwaine et al. [28] it is also important to determine which types of feedback are preferable.
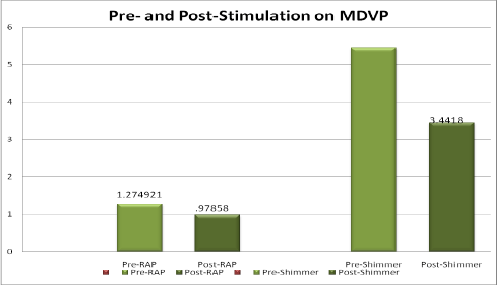
Figure 3: Results of MDVP data pre and post stimulation
The MDVP reliably measured parameter change with regard to vocal improvement after stimulability training. The present investigation’s stimulability approach, which consisted of coordination of respiration and phonation and purposely pulling in the abdominal muscles upon phonation, resulted in lower levels of RAP, shimmer, and NHR ratios to normal levels. Additionally, perceptual assessment of vocal improvement was consistent with acoustic improvement. Additionally, some participants were motivated to enroll in therapy and see an ENT doctor after viewing the results of stimulation.
I wish to acknowledge Professor Cyndi Stein and my Brooklyn College students, Erin Blatti and Dana Levine, for their contributions to this article. My deep appreciation to Howard Spivak, my statistician for his advice and input.
Download Provisional PDF Here
Article Type: Research Article
Citation: Schaeffer N (2016) Pre and Post Stimulation Results for Dysphonic Participants on the Multidimensional Voice Program. Clin Res Open Access 2(1): doi http://dx.doi.org/10.16966/2469-6714.111
Copyright: © 2016 Schaeffer N. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access