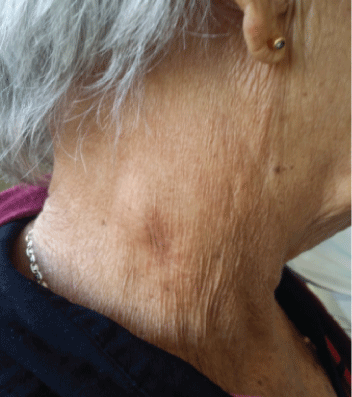
Figure 1: Cervical ganglion.

Anel Pérez de Alejo Alemán1 Claribel Plain Pazos2* Carmen Rosa Carmona Pentón2 Anisbel Pérez de Alejo Plain3 Lázaro Roque Pérez4 Leonardo Domínguez Plain5
1Specialist of I Degree in Internal Medicine, Assistant Professor, Teaching General Teaching Hospital “Mártires del 9 de Abril,” Sagua la Grande,Villa Clara, Cuba*Corresponding author: Claribel Plain Pazos, Specialist of II Degree in Integral General Medicine, Assistant Professor, Faculty of Medical Sciences of Sagua la Grande, Villa Clara, Cuba, E-mail: claribelpp@infomed.sld.cu
Castleman’s disease is a very rare lymphoproliferative disorder. There are two Clinical forms: the unicentric, which is usually benign, and the multicentric progressive course. There are three described histological patterns: hyali neovascular of unicentric presentation, of plasma cells of multicentric presentation and the mixed one. The aim of this paper is to present a clinical case of multicentric Castleman’s disease of hyaline vascular histology very little described in the literature. The patient started with asthenia, anorexia, profuse nocturnal sweating, weight loss, generalized lymphadenopathy, splenomegaly and respiratory episodes. At physical examination: multiple cervical, axillary and bilateral inguinal adenopathies. The diagnosis was made with the histopathological study of the resected ganglion, the evolution after the treatment has been favorable. Because there are no specific clinical and radiographic features, a high degree of diagnostic suspicion and the experience of the pathologist are required to diagnose this rare disease.
Castleman; Disorder lymphoproliferative; Hyaline-vascular
Castleman’s disease is a lymphoproliferative disorder and was first described in 1954, by Dr. Benjamin Castleman [1,2]. Castleman Disease (CD) encompasses several clinicopathologic disorders at the intersection of hematology, oncology, rheumatology, and virology, with overlap in histopathologic and clinical features. Castleman disease (CD) encompasses several clinicopathologic disorders at the intersection of hematology, oncology, rheumatology, and virology, with overlap in histopathologic and clinical features [3]. It is believed to be caused by an antigenic stimulation of probably viral etiology or as a consequence of a proliferation of plasma cells due to the alteration in the regulation of the decreasing factors [4]. There are two clinical forms: the localized or unicentric, which is usually benign, and the generalized or multicentric which as a worse and progressive course [2]. Occurs with equal frequency in both sexes and at any age, predominantly between the third and fifth decade of life and can affect any ganglionar site in the body in the, although mostly in the thorax (70%), followed by the neck (15%) and the abdomen-pelvis (15%) [5]. There are three described histological patterns: hyalinovascular of unicentric presentation, of plasma cells of multicentric presentationwhich is manifested by generalized peripheral lymphadenopathy, hepatosplenomegaly, fever and nocturnal sweating- and the mixed one [2]. Unicentric form as a good prognosis while multicentric, which commonly occurs in a scenario of immunocompromised patients, as a high morbidity and mortality with few therapeutic options [6]. The following is the case of an immunocompetent patient who developed the disease, which is striking in itself, with an atypical clinical presentation. The illustrative of the case is reinforced with microscopy images, which are enriching. Despite not being a common disease in patients without compromise of the immune system, the doctor should always be aware of its presence and take it into account within the differential diagnoses. In addition, the case exemplifies the importance of pathological anatomy in the diagnostic process.
MRB patient 74 years of age, female, with a history of arterial hypertension treated and controlled with Atenolol (100 mg) 1/2 tablet daily. Which has been hospitalized repeatedly for presenting asthenia, anorexia, profuse nocturnal sweating, weight loss, generalized lymphadenopathy, splenomegaly and respiratory episodes of an infectious nature, for which antibiotic treatment has been needed? The most prominent feature in the physical examination was the presence of multiple cervical, axillary and bilateral inguinal adenopathies (Figure 1) in blood cytometry at admission, anemia (Hb 6.6 g/dL) was noted Peripheral Lamina: Hypochromia XXX, Roleaux Phenomenon, red blood cells in target. Anisopoikilocytosis, normal platelets in number and aggregation, slightly increased leukocytes. Blood chemistry without alterations, protein electrophoresis without alterations, coagulogram and normal fibrinogen. Abdominal US showed Liver with changes in the ecotexture at the level of the costal margin, thin-walled vesicle without lithiasis, both kidneys with good medullary cortical relation without lithiasis or dilatation, moderate splenomegaly, normal pancreas, no free liquid in cavity. Medulogram where the myelodysplastic process reported. Treatment started with Hydroxyurea and support with erythropoietin. Faced with an unfavorable evolution, it I decided to send Hermanos Ameijeiras Hospital where she admitted to carry out further studies.

Figure 1: Cervical ganglion.
Hemoglobin 8.0 g/dl
Erythro Sedimentation (ESR) 132 mm/h
Studies for Surface Antigen for Hepatitis B (HBV), Surface antigen for Hepatitis C (HCV), Human Immunodeficiency Virus (HIV), Serology for Syphilis (VRDL), Human T-cell lymphotropic virus (HTLV-I): Negatives
Medullogram with megakaryocytic and erythropoietic hypoplasia with some dimorphic granule changes, no tumor infiltrate.
Bone marrow biopsy with reactive process and hypoplasia of the systems with a hypercellular medulla.
Lymph node excision from the neck, with anatomopathological study, showed the architecture of the modified lymph node due to the presence of secondary lymphoid follicles that go beyond the cortex (Figure 2), the secondary lymphoid follicle presents increased thickness in the blood vessels whose wall presents hyalines changes, the so-called vascular hyaline center or lollipop image (Figure 3) compatible with Castleman’s disease hyaline vascular variety.
The patient discharged with cyclophosphamide treatment with prednisone. After starting treatment, the patient followed was monthly in the internal medicine and oncology office where her clinical improvement verified for one year.
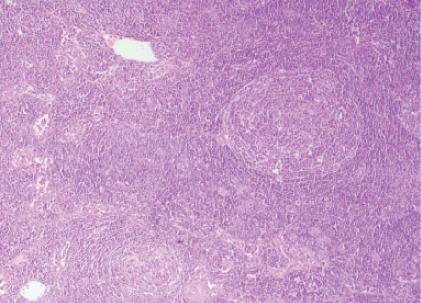
Figure 2: The architecture of the lymph node.
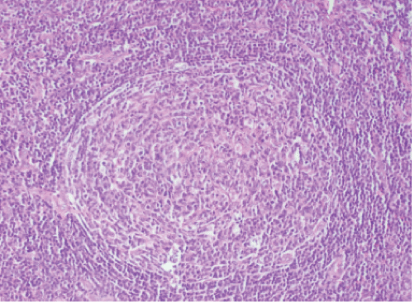
Figure 3: The secondary lymphoid follicle.
Castleman’s disease usually appears in young adults, without gender predominance, but can affect people of any age. It is an infrequent disorder, there is little information about its epidemiology and its incidence is unknown [1,5]. The presence of masses in this disease commonly triggers futile investigations in search of other types of tumors or other diseases of infectious or inflammatory origin, all of which were discarded prior to the diagnosis in our case. Because it is a rare disease, a high degree of diagnostic suspicion is required and, because there are no specific clinical and radiographic data, the diagnosis is anatomopathological [5,7]. This requires a complete resection of the affected ganglion [8]. As it happened in our case. Fine needle aspiration biopsy is not useful for diagnosis [8].
The unicentric form that represents 90% of the cases and that only includes a lymphatic ganglion, is generally benign, and usually corresponds to the vascular hyaline type, commonly appears in adults. Young, and most are asymptomatic. The multicentric form represents less than 10% of cases of Castleman’s disease. This form appears mostly in older adults and associated with the variety of plasma cells, with generalized multiple adenopathy and systemic manifestations. Within systemic manifestations may appear fever, night sweats, adynamia, hyporexia and weight loss. It can also be verified immunological and hematological abnormalities, such as anemia, or accompanied by pulmonary symptoms: cough, dyspnea or hemoptysis, as well as skin lesions [5]. In the present case, the clinical data coincide with the systemic manifestations of the multicentric form. However, the histological data show the vascular hyaline type that is the predominant pathological subtype in the unicentric variant, which is not frequent. This histological type only appears in 10% of cases of multicentric Castleman’s disease [9], the treatment of the unicentric vascular hyaline type is usually resolved by surgery and radiotherapy [1], in this case it could not be possible since the disease affected multiple ganglion behaving systemic way, making it more difficult its treatment and evolution. Multicentric Castleman’s disease requires systemic treatment [10], multiple therapeutic lines have been tried without reaching consensus on the guideline of choice. Monotherapy has been used with chlorambucil, corticosteroids, cyclophosphamide, vincristine and bleomycin [11]. In the present case, the patient, for a year, is receiving treatment with Dexametazone 4 milligrams tablet, four weekly tablets and cyclophosphamide tablet of fifty milligrams, four tablets weekly, staying stable without relapses. The prognosis of the disease, without treatment, is serious. The main causes of death in patients with multicentric CAD are due to infections, renal failure and neoplasms, including lymphoma and Kaposi’s sarcoma [5].
This represents the first case published in our institution. Because there are no specific clinical and radiographic data, a high degree of diagnostic suspicion is required and the pathologist’s experience is important. If the complete exceresis of the lymph node with biopsy not performed, it is impossible to make the diagnosis. Treatment depends on the clinical variety and type.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: de Alejo Alemán AP, Pazos CP, Pentón CRC, de Alejo Plain AP, Pérez LR, et al. (2019) Castleman’s Disease about a Case. J Clin Lab Med 4(2): dx.doi.org/10.16966/2572-9578.131
Copyright: © 2019 de Alejo Alemán AP, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access