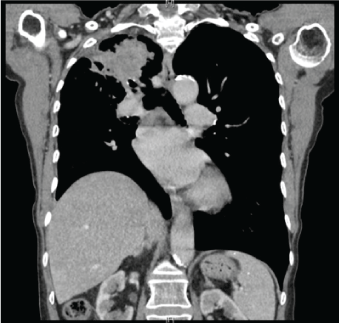
Figure 1: CT taken on initial presentation showing a RUL lesion.

Christine E Orr* Adewale Adeyinka David Good Sandip K SenGupta
Department of Pathology and Molecular Medicine, Queen’s University, Kingston, Ontario, Canada*Corresponding author: Christine E Orr, Department of Pathology and Molecular Medicine, Queen’s University, Kingston, Ontario, Canada, E-mail: christine.orr@queensu.ca
Adenosquamous bronchogenic carcinoma; Paraneoplastic pancytopenia
Adenosquamous carcinoma of the lung is a rare event comprising 0.4-4% of lung carcinomas [1]. These tumors are diagnosed both morphologically and immunohistochemically via positive staining with TTF-1* and p63* on the acinar and squamous components respectively.
Paraneoplastic syndromes are due to malignant conditions that are the result of production of endocrine, or other chemical substances, by the tumor rather than due to local or metastatic spread of the tumor. Lung carcinomas are well known to be involved with many paraneoplastic syndromes including but not limited to: Myasthenic syndromes, SIADH*, and Cushing syndrome [1]. Paraneoplastic pancytopenia is a relatively rare syndrome and the exact mechanism behind its presentation is still unknown. It is usually a diagnosis of exclusion when there is no evidence of tumor metastasis or underlying secondary disorder in the bone marrow. There are only a few cases reported of pancytopenia associated with both small cell [2] and non-small cell lung carcinoma (NSCLC) [3,4] in the literature; however, to our knowledge, there is no report specifically of it associated with adenosquamous carcinoma.
A 75 year old woman presented with a three week history of hemoptysis complicating three months of fatigue and cough. She was a previously healthy non-smoker with a history of hypertension, hyperlipidemia, and chronic back pain. She had no history of recent travel, malignancy, immune dysfunction or record of pancytopenia. Her medications included hydrochlorothiazide, irbesartan, risedronate, amlodipine, metoprolol, and rosuvastatin.
The original differential diagnosis included infectious and malignant disease. CT scan showed a 6.3cm right lung mass involving all three lobes with a second nodule in the right lower lobe, which was suggestive of a primary malignancy or necrotizing infection (Figure 1). Lab testing identified pancytopenia which was sustained throughout her seven day admission; hemoglobin 65-88g/L (120-160 reference), white blood cells 0.5-1.9 × 109 /L (4-10.5 reference) and platelets 5-85 x 109 / L (150-400 reference). Her peripheral blood smear showed occasional teardrop cells and elliptocytes with no evidence of schistocytes or blasts. Furthermore, there was no evidence of hemolysis: LDH 143 U/L (94- 250 reference), haptoglobin 2.31 g/L (0.2-2.0 reference), total bilirubin 16 umol/L (0-17 reference), direct bilirubin 5 umol/L (0-5 reference) and reticulocytes 10 × 109 /L (10-100 reference). Coagulation studies remained within normal limits throughout her stay with the exception of elevated fibrinogen: PTT* 28 seconds (21-29 reference), PT* 12.5 seconds (10.7-13.0 reference), INR* 1.1 (0.9-1.1 reference) and fibrinogen 8.25 g/L (1.8-4.1 reference). Investigations regarding her anemia ruled out folate, vitaminB12, and iron deficiencies: folate >50 nmol/L (13.5-55 reference), vitamin B12 399 pmol / L (165-740 reference), iron 33 umol/L (7-26 reference), ferritin 242 ug/L (13-150 reference), and transferrin % saturation 58% (20-55 reference).

Figure 1: CT taken on initial presentation showing a RUL lesion.
A number of investigations including lung biopsy, sputum and blood culture, bone marrow biopsy, and brush cytology revealed only pulmonary macrophages and rare fungal forms suggestive of Candida. The bone marrow biopsy was hypocellular with decreased trilineage hematopoiesis, no increase in blasts, <10% cellularity, and no dysplastic or malignant morphology (Figure 2a). A cytogenetic sample was available but not tested. Flow cytometry on the bone marrow aspirate showed 71% T lymphocytes, some NK* cells, 26% B lymphocytes, no blasts and no myeloid cells (Figure 2b).
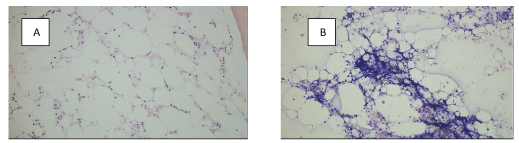
Figure 2: 20x view BM biopsy (A), 10x view BM aspirate (B).
Antibiotics, IVIG*, platelet transfusions and red cell transfusions, were ineffective. Platelets recovered marginally after a combination of IVIG and platelet transfusions but required another round of therapy within one to two days. An autoimmune work-up was negative for the following: c-ANCA*, p-ANCA*, and DAT* (Broad Spectrum Coombs, Anti-IgG Coombs, and Complement). The rest of the autoimmune workup was within normal limits with exception to ANA*: C3 complement 1.01 g/L (0.80-1.80 reference), C4 complement 0.27 g/L (0.13-0.40 reference), rheumatoid factor <20 KIU/L (0-20 reference) and ANA 1:640 positive. Further microbiology studies for acid fast bacilli, Nocardia, Pneumocystis and Legionella were all unable to identify a responsible organism. A final attempt at bronchial artery embolization failed as the process appeared to be involving the pulmonary artery. She passed away the next day.
An autopsy was performed which revealed a primary bronchogenic adenosquamous carcinoma with both acinar and squamous components. Immunohistochemicallythe tumor expressed TTF-1 and p63 staining respectively (Figure 3). The massive pulmonary hemorrhage and paraneoplastic pancytopenia were attributed to this tumor which invaded the right pulmonary artery.
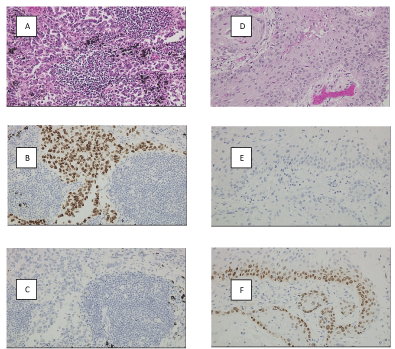
Figure 3: 20x views; Acinar component (A), with TTF1 (B) and p63 (C). Squamous component (D), with TTF1 (E) and p63 (F).
Paraneoplastic pancytopenia has been described in small cell lung cancer, adenocarcinoma and squamous cell carcinoma; but there has been no report of it in relation to bronchogenic adenosquamous carcinoma. Previous reports have found evidence of both hypercellular bone marrow and hypocellular bone marrow in the context of pancytopenia without signs of metastasis in the bone marrow [4].
Given the limitations of cytology and biopsy studies, as exemplified in this case, pancytopenia may be a diagnostic clue to suggest malignant rather than infectious causes of hemoptysis. However there are many causes of pancytopenia and, as of yet, there are no serological markers associated with paraneoplastic pancytopenia that may further aid in diagnosis. A bone marrow aspirate and biopsy must be performed to rule out metastasis into the bone marrow, or if there is another underlying disorder that could explain pancytopenia (i.e. drugs, toxins, infection or congenital disorder). Laboratory studies including an anemia, autoimmune, infectious and coagulation work-up must also be performed in the investigation of pancytopenia.
Future direction may include investigating the mechanism of paraneoplastic pancytopenia syndromes in order to provide treatment in a timely manner to critically ill patients in the context of negative cytology or biopsy results.
TTF-1 (thyroid transcription factor 1), p63 (transformationrelated protein 63), SIADH (syndrome of inappropriate anti-diuretic hormone), PTT (partial thromboplastin time), PT (prothrombin time), INR (international normalized ratio), NK cell (natural killer cell), IVIG (intravenous immunoglobulin), c-ANCA (cytoplasmic anti-neutrophil cytoplasmic antibodies), p-ANCA (perinuclear anti-neutrophil cytoplasmic antibodies), DAT (direct antiglobulin test), ANA (antinuclear antibody).
Download Provisional PDF Here
Article Type: Case Report
Citation: Orr CE, Adeyinka A, Good D, SenGupta SK (2016) Case Report: Primary Adenosquamous Bronchogenic Carcinoma Presenting with Hemoptysis and Pancytopenia. J Clin Lab Med 1(1): doi http://dx.doi.org/10.16966/2572-9578.104
Copyright: © 2016 Orr CE, This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access