Abstract
Dissecting cellulitis of the scalp is a rare inflammatory disorder of unknown etiology. It is clinically characterized by the formation of painful suppurative chronic nodules and abscesses, which are connected by fistulae that, although they can be cured, as a consequence leave patients with irreversible alopecia. Currently, there are only a few cases reported in the literature. Here we present the case of a 45-year-old patient with dissecting cellulitis of the scalp, focusing on the histopathological findings and clinicopathologic correlation.
Keywords
Dissecting cellulitis of the scalp; Perifolliculitis capitis abscedens et suffodiens; Alopecia cicatrisata; Isotretinoin
Introduction
Dissecting cellulitis of the scalp is a rare inflammatory disease. It is one of three skin conditions presenting follicular occlusion, of which dissecting folliculitis is the least commonly found [1]. This condition is clinically characterized by the formation of chronic suppurative nodules and abscesses that are connected by fistulae and leave hypertrophic or keloid alopecic scars [1]. We report the case of a 45-year-old male patient presenting perifolliculitis capitis abscedens et suffodiens, and we provide a review of the literature.
Case synopsis
A 45-year-old African descent male presented to our clinic with a lesion in the scalp, in the occipital region, that originated five years ago as a small “pimple” that began to gradually extend, and had not responded to standard established treatments. There was no previous history of trauma, surgery, or other relevant medical conditions. Upon clinical examination, dermatosis of the scalp was identified, characterized by fluctuating and suppurative nodules that were soft to the touch and of keloid appearance (Figure 1).
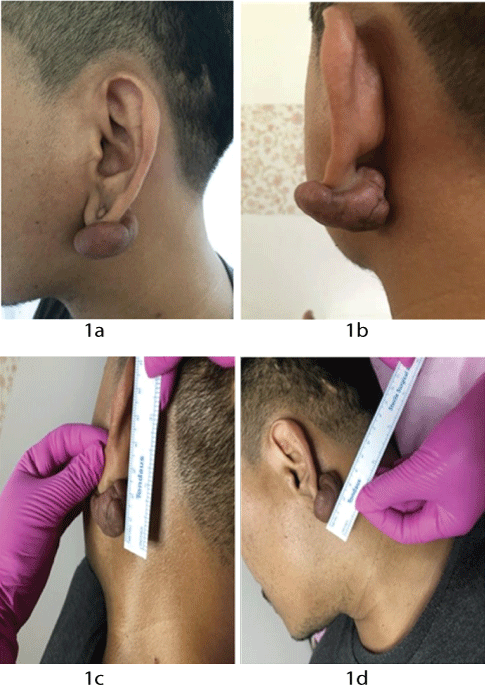
Figure 1: A) Occipital-parietal inflammatory nodules converge and generate extensive alopecic areas. B) Nodules of keloid appearance in the bilateral parietal región. C) Coalescing fluctuating nodules forming fistulous tracts and discharging purulent material are shown at higher magnification.
Test results: Staphylococcus aureus culture was positive. NMR studies showed no bone compromise. Skin biopsy revealed an intense inflammatory reaction in the deep layer of the dermis, with presence of neutrophils, lymphocytes, plasma cells, and histiocytes. In addition, frank abscesses interconnecting by sinuous fistulae, and discharging to the exterior (Figure 2) were also observed. These findings are consistent with histopathological findings in dissecting cellulitis of the scalp. Treatment with 1 mg/kg isotretinoin was initiated, and incision and drainage of the largest nodules with notable improvement in scalp lesions (Figure 3). Biological therapy was not used.
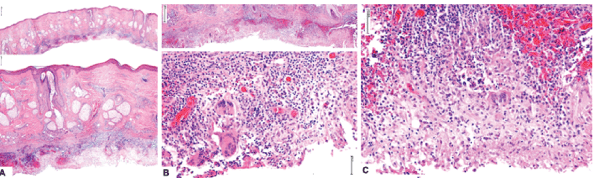
Figure 2: A) H&E staining micrograph from occipital lesion. Upper panel: 10X, panoramic view of entire dermis thickness including a deep fistulous tract indicated by arrow. Lower panel: 40X, epidermis, superficial, and middle dermis of normal appearance. A dense inflammatory infiltrate is observed in the deeper dermis, indicated by asterisk. B) H&E staining micrograph from occipital lesion. Upper panel: 40X, deep fistulous tract formation lined by inflammatory cells. Lower: 200X, multinucleate giant cells and mixed inflammatory infiltrate. C) H&E staining micrograph from occipital lesion. 200X: intense dermal inflammatory reaction constituted mainly by neutrophils, lymphocytes, and plasma cells.
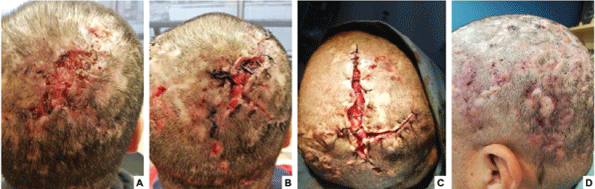
Figure 3: Marked improvement of occipital scalp lesions after surgical treatment. (A) First intervention: Incision, drainage of nodules and secondary intention healing. (B) Second intervention: curettage and resections of the fistulous tracts 12 months later. (C) Third intervention: correction of hypertrophic scars and subcutaneous tracts 24 months later. (D) Nodules, cysts and hypertrophic scar had remarkably improved after 36 months of treatment.
Case discussion
Dissecting cellulitis of the scalp was first described by Spitz in 1903, referring to it as “dermatitis folicularis capitis et perifolliculitis conglobata” [2]. Later, in 1908, Hoffman introduced the name of “Hoffman’s perifoliculitis capitis abscedens et suffodiens”, the name by which it is currently identified [3]. This is a rare disorder that belongs to the group of neutrophilic cicatricial alopecia, and represents 1% to 2% of cases of primary cicatricial alopecia. Patients more frequently affected by this disorder are young black males between 18 and 40 years of age, however a few cases in white males, even among family members and children, have also been described [4-10].
Currently, etiopathogenesis of dissecting cellulitis of the scalp remains to be fully elucidated. Nonetheless, it is commonly associated with acne, hidradenitis suppurativa, and occasionally with pilonidal disease. This suggests that it may be secondary to follicular hyperkeratosis, which leads to hair follicle occlusion and dilation [5,7]. Clinically, it’s characterized by the formation of painful nodules and abscesses that are more frequently found in the vertex and occiput. Nodules and abscesses can be firm, fluctuating, and some even suppurative, which drain purulent material. In the majority of cases, such nodules may coalesce and form fistulous intercommunicating tracts that dissect the scalp, and in consequence leave cicatricial alopecia as a scar, which may be extensive [4,8].
Regarding histopathology, it may be non-specific and varied, as it depends on the stage of the disease. In early lesions, histological sections may exhibit numerous intact hair follicles, and simultaneously an acneiform distention of the follicular infundibulum with intra and perilesional neutrophilic infiltration with its consequent inflammation, and subsequent formation of deep abscesses, which will destroy the pilosebaceous unit [1,5,7]. Unlike other types of cicatricial alopecia, the inflammatory infiltrate is located in the deepest part of the hair follicle, and even of subcutaneous tissue [7].
As disease progresses, and as a consequence of hair follicle destruction, foreign body granulomas begin to form, associated to abscess and sinuous tract formation. In the late or healing stage, hair follicles and sebaceous glands are completely destroyed and replaced by fibrous tissue [9]. Diagnosis is established with an adequate clinicopathological correlation [5].
The differential diagnosis for dissecting cellulitis of the scalp includes other types of cicatricial alopecia that also exhibit inflammation in the deep portion of the hair follicle and/or of the perifolicular region such as keloid folliculitis, which although has specific clinical features, shares similar histopathologic findings with dissecting cellulitis [9]. Subtle changes may favor their identification, since dissecting cellulitis is characterized by severe purulent inflammation and intense neutrophil infiltration and abscess formation [10], and, on the other hand, keloid folliculitis may present more fibrosis and greater number of plasma cells [11]. Nonetheless, distinct histological features may not be identified between these clinically different lesions [9].
As a general rule, the presence of any type of microorganisms including parasites, bacteria, and fungus, must be ruled out, since it may mimic folliculitis decalvans. However, it must be taken into account that although cultures and special stains may indicate presence of microorganisms at the level of the dilated follicular ostium, this finding may not be pathological. Lesions caused by dissecting cellulitis of the scalp are persistent and do not usually respond to treatment [12]. To date, there is no specific treatment for this condition, however variable results have been achieved using several therapeutic approaches that range from antibiotics, oral retinoids, and corticosteroids, to radiotherapy, biological therapy, and surgery [1,13,14].
Conclusion
We report a typical case of dissecting cellulitis of the scalp, which is a rare disorder with few cases available in the literature. We emphasize on histopathological findings since this is a type of cicatricial alopecia that, as such, shares many histological findings with other disorders belonging to the same group, and exhibits subtle differences with other types of neutrophilic and mixed cicatricial alopecia. Therefore, clinicopathologic correlation is of pivotal importance in this type of cases.
Article Information
Aritcle Type: CASE REPORT
Citation: Valencia VG, Malliquinga MS, Molina RR, Santamaria FEP (2021) Perifolliculitis Capitis Abscedens Et Suffodiens: A Case Report and Literature Review. J Clin Cosmet Dermatol 5(2): dx.doi.org/10.16966/2576-2826.167
Copyright: © 2021 Valencia VG, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Received date: 20 Sep, 2021
Accepted date: 08 Oct, 2021
Published date: 19 Oct, 2021




