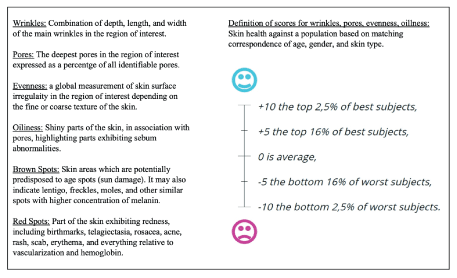
Figure 1: Quantificare skincare tests and score definitions.


Greg Chernoff, BSc, MD, FRCSC*
Department of Otolaryngology, Head and Neck Surgery, Ascencion St. Vincent Hospital, Indianapolis, Indiana, USA*Corresponding author: Chernoff G, Department of Otolaryngology, Head and Neck Surgery, Ascencion St. Vincent Hospital, Indianapolis, Indiana, USA, Tel: +1-317-573-8899; Fax: +1-317-818-2008; E-mail: greg@drchernoff.com
Introduction: The science in aesthetic medicine continues to grow and expand exponentially. With improved science comes advanced clinical therapeutics that further benefits our patients. Physicians are seeking non-surgical technologies that are capable of safely treating all Fitzpatrick skin types while yielding meticulous results.
This study examines the safety and potential efficacy of a new instrument platform offering single session sea salt exfoliation in combination with cavitating cutaneous ultrasound and high intensity LED light therapy (SaltFacial) in treating aging skin, acne, infection, edema and wound healing.
Method: The safety of each of these modalities has been established individually in the peer reviewed literature. There has not been a study comparing the efficacy of combining these technologies in a single session to traditional treatments such as microdermabrasion and hydrating facials, potentially adding benefit to the patient. This study examines performing the SaltFacial on the 20 aging skin patients, 16 acne patients, 16 patients with post-surgical infection, and 40 patients with post-surgical edema, bruising, and actively healing wounds. The treatment group was compared to an equal number of patients in a control group who were matched for sex and age, treated with what is considered “standard of care” treatment for the specific conditions studied. Patient results were objectified with standardized photography, and the Quantificare 3D Imaging System Software (Quantificare, USA), which measures depth of wrinkles, pore size, general evenness, oiliness, unwanted pigment and redness. Linear analog scores were also administered to patients measuring treatment satisfaction and pain experienced.
Results: There were no adverse reactions in any patient from the sea salt exfoliation, ultrasound therapy, or LED light treatment, alone or in combination with each other.
In the Aging Skin Population, the SaltFacial proved more efficacious than microdermabrasion or hydrating facials. Uniformly, Quantificare analysis measurements were better for wrinkle reduction, pore size reduction, improved skin evenness, reduced oiliness, reduced pigmentation, and reduction of unwanted blemishes in the SaltFacial patients than microdermabrasion or hydrating facials alone. These results were further improved when a nitric oxide generating serum (N101, Pneuma Nitric Oxide, USA) was utilized as the ultrasound “glide” primer prior to administering protein peptides. Patient Linear Analogs showed the majority of patients to be “extremely happy” or” happy” with the combination treatment results. No patients expressed “displeasure” with the combination treatment results. This combination treatment can therefore serve as a “non-thermal” form of skin rejuvenation, comparable to Fractionated CO2 or radiofrequency systems.
The Acne Patient Population showed a reduction in pustules and comedones 4 weeks after weekly SaltFacial combination treatments compared to a control population receiving oral and topical antibiotic treatment alone. Acne-induced inflammation and erythema was reduced by 72.5% in SaltFacial patients as compared to 36.8 % in the antibiotic patients.
The Post-Surgical Infection Patients showed uniform rapid resolution of infection, inflammation, erythema and pain (mean 5.8 days) subsequent to the high-intensity LED light therapy as compared to patients similarly infected in corresponding regions treated only with traditional culture-specific antibiotic therapy(11.4 days) and accepted wound care. This was shown in challenging MRSA infections which can yield devastating results if not treated promptly and appropriately .
The Post-Surgical Wound Healing SaltFacial Patient Population showed more rapid healing (mean 6.9 days) as compared to the control patient population (mean 11.1 days) receiving traditional corticosteroid therapy alone. Eighty-five percent of patients reported less edema, erythema and discomfort by day 10 as compared to 18% of control patients. The anti-prostaglandin effect of LED light therapy was also demonstrated with 76% of LED-treated patients reporting less pain as measured by linear analog scores compared to 10% of control patients.
The Wound Healing Patient Population also showed more rapid re-epithelialization, faster edema and purpura resolution as well as more aesthetically pleasing scars compared to control patients who received traditional standard of care wound care.
Conclusion: The SaltFacial shows benefit in the aging skin, acne, infection, inflammation and wound healing patient populations.
The sea salt component lends antibacterial, antifungal and antiviral benefits. Additionally, sea salt promotes healing via normal pH maintenance, barrier function protection and mineral and vitamin deposition. Ultrasound penetration is also enhanced.
The topical minerals, particularly calcium and magnesium aid in neocollagenesis and keratinocyte production improving the overall tone, quality and clarity of skin.
The cavitating ultrasound improves circulation, facilitates tissue permeability of dermal beneficial products and promotes a healthy immune cellular response.
LED phototherapy acts as an anti-bacterial, anti-fungal, and anti-viral tool. Additionally, LED light reduces inflammation, increases dermal collagen synthesis, and dramatically reduces pain by down regulating pain receptors.
This novel combination therapy yields a valuable addition to the armamentarium of the aesthetic and reconstructive physician.
The concept of “Generational Aesthetics” is important to understand in the current arena of products and services offered by aesthetic providers. The current demographic distribution of aesthetic patients in most practices includes: generation Z patients (12-25 years), millennials (26-40 years), generation X patients (41-55 years), baby boomers (56-75 years), and with improved health care, more 76-to 90-year-old patients are also seeking consultations for skin maintenance and improvement.
While the individual needs of these groups differ proportionate to genetics, age, diet, hormonal levels, environmental exposure, and degree of self-care, common to all; is the desire to obtain “preventative regimens” over “corrective regimens”. In addition to prevention, more patients are seeking non-surgical, minimally invasive alternatives to surgical intervention for aesthetic improvement. Minimal to no downtime tops the list for this reasoning.
The main signs of aging common to men and women include bone resorption, gravitational muscular decent, volume loss, and loss of elasticity, tone, quality and clarity of skin. It behooves the treating physician to recommend the safest, most efficacious treatment to yield the best, longest lasting solution. If muscular gravitational decent is the chief complaint, then surgical interventions such as brow lift, eyelidlift or face/neck lift are typically the best long-term solutions. Volume loss can be remedied with fat transfer or commercially available injectable fillers. When loss of elasticity, tone, quality and clarity of skin are more concerning than muscular gravitational descent or volume loss, then non-surgical skin improving options are realistic to achieve realistic goals.
Technological advancements have risen in skin quality improvement systems over the past decades. Both ablative and non-ablative systems have seen refinements. Light and energy-based therapies have sought higher intersecting lines of safety and efficacy. Minimally invasive treatments heralding minimal risk, minimal downtime, and minimal pain have added to the armamentarium of treating physicians. Four of these individual treatments include microdermabrasion, hydrating facials, cavitating ultrasound, and LED phototherapy
Traditional microdermabrasion systems shoot a stream of fine crystals such as aluminum oxide, sodium chloride or sodium bicarbonate with the intent of disrupting and removing all or part of the stratum corneum. With this in mind, a more accurate name would be “microepidermabrasion”, as there is little effect on the dermis. A suction device removes the dead cells and the used crystals. The act of removing the stratum corneum allows for improved absorption of topical products and the replacement by the body with younger, healthier epidermal cells.
In recent years, research has focused on refining the media used to remove the stratum corneum. This research focused on finding an exfoliation medium that could have ancillary dermal benefits in addition to exfoliative capabilities.
Salt is one of the potential candidates. Much has been written on the history of salt [1]. For hundreds of years, this substance has served as a currency, influenced the establishment of trade routes and cities, provoked and financed wars, and inspired revolutions and secured empires. There is some misunderstanding in the lay population as to the types of salt. From a health perspective, there is “bad” salt, and “good” salt. Bad salt is processed and refined. It typically contains 97.5% sodium chloride (NaCl) and 2.5% chemical additives which when overused can lead to hypertension and cardiac disease. Good salt is unrefined, typically found in ocean and sea salt, or in pristine salt mines. Sea salt is composed of 85% NaCl, and 15% of 60 trace minerals such as Mg, Ca, Na, and K.
There has been growing evidence that the well-being of our skin is strongly influenced by nutrition, particularly vitamin and mineral content [2]. Twelve vitamins and nine minerals are thought to be essential for healthy enzymatic bodily function. The vitamins include vitamins A, D, C, E K, B6, B12, thiamin, riboflavin, niacin, folate, and choline. The minerals include calcium, copper, iron, magnesium, phosphorus, selenium, zinc, potassium, and sodium. While some topical application studies exist, the benefits of topically applied mineral salts to the skin have been largely unexplored. To date, topical sea salt has been found to be antibacterial, antifungal, antiviral, and hydrophilic in protecting the hydration barrier, detoxifying and immunomodulatory [2].
Cavitating ultrasound is another modality which has shown scientific benefit to skin health [3]. Traditional topical delivery of products to tissue is limited by epidermal permeability and dependent upon the molecular size and weight of the product being applied, and the existing circulation of the recipient tissue bed. Cutaneous ultrasound has been shown to improve circulation and increase tissue permeability, thereby increasing the depth of penetration and absorption of topically applied substances [4]. When focused deeper, with higher intensity, cavitating ultrasound has been shown to successfully reduce adipocytes and improve lymphatic drainage [5].
LED therapy has also been investigated for skin health [6]. The most common and beneficial wavelengths include blue (414nm), which has been shown to be bactericidal, red (660nm), which can reduce inflammation and induce cellular proliferation, amber (590nm) which has ant-inflammatory benefits, and infrared (830nm) which improves vascularity and collagen production [6].
To date, there has not been a single instrument platform, or a study that combines, in a single treatment session, these modalities. The purpose of this study is to examine the potential efficacy of these modalities combined in a single treatment session in treating aging skin, acne, infections, and wound healing and other cutaneous problems.
This study examines combination single session therapy utilizing sea salt exfoliation, cavitating ultrasound with dermal deposition of a hyaluronic acid peptide serum containing acetyl hexapeptide, palmitoyl pentapeptide, and palmitoyl oligopeptide (Abbe Labs, New York, NY), followed by endpoint focused, wavelength specific, high-intensity LED light exposure, (SaltFacial, USA).The sea salt for the SaltFacial is harvested from the waters of the San Francisco Bay, processed, purified and re-crystallized to produce an extra-fine particle size. The sea salt is composed of 85% NaCl, and 15% of 60 trace minerals such as Mg, Ca, Na, and K.
The SaltFacial Treatment Patient Population included 20 aging skin patients, 16 acne patients, 16 patients with post-surgical infection, and 40 patients with post-surgical edema, bruising, and actively healing wounds located on the face and neck. The control group contained an equal number of patients, matched for sex and age within each subgroup above.
The Aging Skin Patients consisted of 15 females and 5 males. Ages ranged from 36-73 years. There were 6 Caucasian, 3 Asian, 4 Hispanic, 4 African American, 3 Indian, and 1 Mediterranean patient. The Acne Patients consisted of 12 females and 4 males. Ages ranged from 15 to 34 years. There were 8 Caucasian, 2 Asian, 4 Hispanic, and 2 Indian patients. The Infection Patients consisted of 16 females. Ages ranged from 42 to 73 years. All were Caucasian. The Post-op edema/bruising/ Wound Healing Patients consisted of 32 females and 8 males. All were Caucasian.
The Aging Skin Patients first received the sea salt exfoliation. This was followed by a 3-megahertz (3MHz) ultrasound application of Nitric Oxide generating serum (N101, Pneuma Nitric Oxide, USA), followed by the peptide serum. Topical nitric oxide has been shown to dramatically increase dermal vascularity, absorption, and act as a vehicle for enhanced absorption of other topicals [7]. It is generated topically subsequent to mixing Vitamin C serum and a serum containing sodium nitrite [7]. This was followed by the high intensityLED phototherapy module which consisted of 4 condition specific wavelengths. The light emitting diodes are contained in 3 panels on an articulated arm. The panels can be positioned flat or articulated at 90 degrees to each other, yielding a wrap around effect to the patient’s head and neck. The aging face patients received 20 minutes of red (660nm) / near infrared (930nm) @ 186 J/cm2, 20mW/cm2 therapy. Each patient received a full treatment at 30, 60 and 90 days. The control group was randomized, and received either traditional microdermabrasion or a hydrating facial administering the same peptide serum. Linear analogs were administered at each treatment session and finally at 120 days. Patients were given a 10 cm line, the left side representing no benefit, and the right side representing maximal benefit. They placed a mark on the line representing their perceived benefit from each respective treatment. This yielded a number out of 10, subjected to statistical analysis. Standardized color photography was performed prior to each session and at 120 days. Patient results were objectified at 30-day intervals with standardized photography, as well as the Quantificare 3D imaging system (Quantificare, USA), which measures depth of wrinkles, pore size, general evenness, oiliness, unwanted pigment and redness (Figure 1). Linear analog scores were also administered to patients measuring treatment satisfaction and pain experienced. Quantificare analysis was performed at 30 and 120 days.

Figure 1: Quantificare skincare tests and score definitions.
The Acne Patients received salt exfoliation, cavitating ultrasound, and 20 minutes of red (660nm)/blue (414nm) @ 106 J/cm2, 20 mW/cm2 LED therapy at each treatment session. Treatments were performed at 7day intervals for 21 days (3 treatments). Standardized photography and Quantificare analysis were performed prior to each session and finally on day 28. Linear analogs were administered at each session and on day 28.
The Infection Patients received 20 minutes of red (660nm)/blue (414nm) @ 106 J/cm2, 20mW/cm2 LED therapy daily for 10 days. Photography and quantificare analysis were performed prior to the initiation of treatment and on the final day of treatment.
The Wound Healing Patients received 20 minutes of red (660nm)/amber (660nm) @ 142J/cm2 , 20mW/cm2, daily for 10 days. Photography was performed prior to the initiation of treatment and on the final day of treatment. Exclusion criteria in this study included an unwillingness to avoid excessive sunlight or wear protective clothing and sunscreen, unwillingness to forgo any other topical dermatological or drug therapy, the use of topical corticosteroid, alpha and betahydroxy acids, retinoids, or vitamin-C containing topicals within 30 days before, as well as throughout the course of the study. Washout periods adhered to by subjects in this study included 6 months free from dermabrasion, deep chemical peels, ablative laser treatments, and neurotoxin or filler injections: 3 months free from non-ablative laser, light, radiofrequency or ultrasound treatments; and 1 month free from microdermabrasion, light and medium depth peels.
The Aging Skin Patients were compared to a control population undergoing traditional microdermabrasion followed by a hydrating facial treatment utilizing standard parameters for those technologies.
The Acne Patients were randomized equally into a SaltFacial treatment group, and a control group. The control group received clindamycin 150mg bid, and 1% clindamycin topical solution bid.
The Infection Patients were randomized equally into a SaltFacial treatment group and a control group. The control population received antibiotic therapy alone, specific to bacterial culture results, collected by cutaneous swab specimens before treatment and 5 days after treatment.
The Inflammation/Bruising/Wound Healing Population was randomized equally into a SaltFacial treatment group and a control group. The control population received standard postoperative corticosteroid (Medrol Dose Pack) and antibiotic therapy (Cephalexin, 500mg, po, bid for 7 days).
Data were analyzed with IBM SPSS statistics (Version 23: IBM Inc, Armonk, New York). Data was analyzed with the student’s t test, paired sample t tests and one-way analysis of variance (ANOVA). P values were assumed significant when < .05.
There were no adverse events attributable to the salt exfoliation, cavitating ultrasound, or LED therapy in the entire study patient population. In particular, there were no allergic, or hypersensitivity reactions, abrasions, or ultrasound/light burns. No patients experienced claustrophobic symptoms due to the proximity of the wrap around LED panels. No patients experienced discomfort or pain that forced cessation of treatment.
The Aging Skin Patients uniformly showed by Quantificare analysis a reduction of wrinkles, pore size, unwanted pigment, and improvement in general oiliness, texture and vascularity of their skin (Figure 2). Each category showed a greater improvement than those patients undergoing traditional microdermabrasion (Figure 3), or a hydrating facial (Figure 4). The degree of improvement increased with each subsequent treatment up to the 120 day period (Figure 5). Patient linear analog scores (Figure 6) showed progressive patient satisfaction with each consecutive treatment (Table 1). There were no unhappy patients treated in the SaltFacial Group. By day 120, 80% reported being extremely satisfied, 10% were very satisfied and 10% were satisfied.
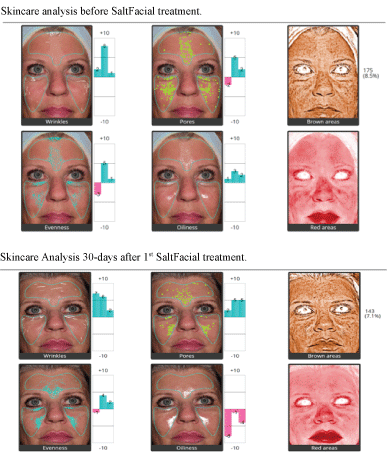
Figure 2: Aging skin patient: Note improvement in graphs after salt facial.
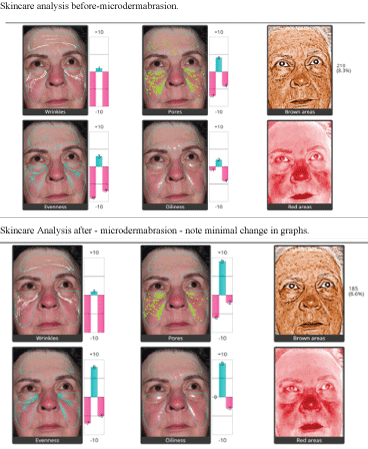
Figure 3: Skincare analysis before and after microdermabrasion.
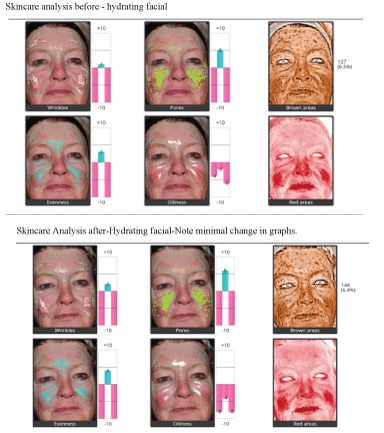
Figure 4: Skincare analysis before and after-hydrating facial
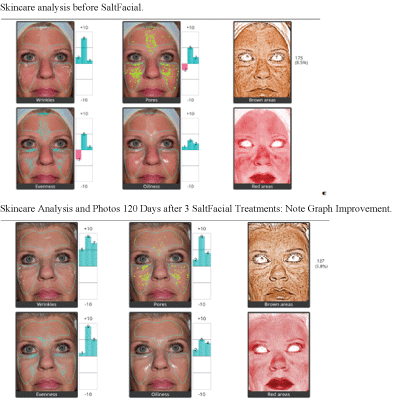
Figure 5: Aging skin patient
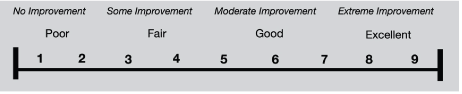
Figure 6: Linear analog
Test patient places mark on line according to perceived result.
| Satisfaction | Percent | |||
| 30 Days | 60 Days | 90 Days | 120 Days | |
| Unhappy | 0 | 0 | 0 | 0 |
| Satisfied | 75 | 50 | 10 | 10 |
| Very Satisfied | 15 | 10 | 15 | 10 |
| Extremely Happy | 10 | 40 | 75 | 80 |
Table 1: Aging Skin: Summary of the results of patient administrated linear analog tests for satisfaction.
The Acne Patients showed a 72.5% mean reduction of pustules and comedones (Table 2) compared to a 36.8 % mean reduction (p<.0001) in the control patients treated with antibiotics alone by day 28 (Figure 7). The degree of improvement increased with each subsequent treatment from Day 7 to Day 28 (Figure 8). Linear analog scores showed a progressive increase in satisfaction with each subsequent treatment (Table 3). There were no unhappy patients in the SaltFacial group. By 28 days, 87.5 % reported that they were extremely satisfied, and 12.5% reported that they were very satisfied with the treatment.
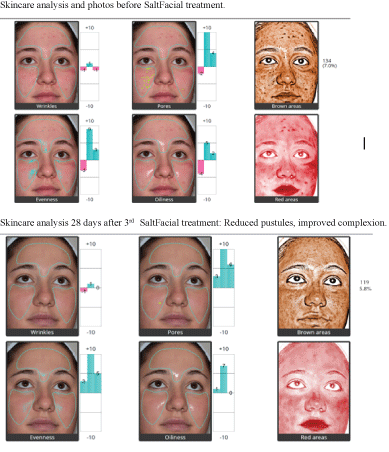
Figure 7: Acne patient.

Figure 8: Acne patient.
| Salt Facial | %Improvement-28 Days | Control | %Improvement-28 Days |
| 1 | 65 | 1 | 40 |
| 2 | 75 | 2 | 30 |
| 3 | 50 | 3 | 60 |
| 4 | 80 | 4 | 50 |
| 5 | 90 | 5 | 10 |
| 6 | 75 | 6 | 50 |
| 7 | 70 | 7 | 35 |
| 8 | 75 | 8 | 20 |
Table 2: Acne Patient: Percent improvement pustules/Comedones compared to control Antibiotic alone patients.
| Satisfaction | Percent | |||
| 7 Days | 14 Days | 21 Days | 28 Days | |
| Unhappy | 0 | 0 | 0 | 0 |
| Satisfied | 62.5 | 12.5 | 12.5 | 0 |
| Very Satisfied | 25 | 50 | 25 | 12.5 |
| Extremely Satisfied | 12.5 | 37.5 | 62.5 | 87.5 |
Table 3: Acne Patients: Summarizes the results of the patient administrated linear analog tests for satisfaction.
The Active Infection Patients (Figure 9) showed a faster time of tissue culture resolution with a mean of 5.8 days, than the control group with a mean of 11.4 days (p<.0001) on oral and topical antibiotics alone (Table 4). Linear analog scores also showed a significant reduction in pain when treated with the LED therapy compared to antibiotics alone (Table 5) with 87.5% reporting to be extremely satisfied and 12.5 5 reporting to be very satisfied. There were no patients unhappy with the treatment.
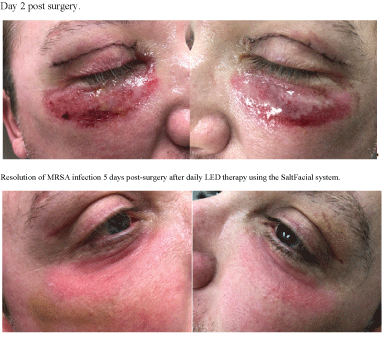
Figure 9: MRSA infected patient.
| Salt Facial | #Days | Antibiotics | #Days |
| 1 | 6 | 1 | 10 |
| 2 | 5 | 2 | 12 |
| 3 | 7 | 3 | 9 |
| 4 | 8 | 4 | 14 |
| 5 | 5 | 5 | 12 |
| 6 | 7 | 6 | 10 |
| 7 | 4 | 7 | 13 |
| 8 | 5 | 8 | 11 |
Table 4: Infection Patients: Number of days healing compared to controlAntibiotic alone patients.
| Satisfaction | Percent |
| Unhappy | 0 |
| Satisfied | 0 |
| Very Satisfied | 12.5 |
| Extremely Satisfied | 87.5 |
Table 5: Infection Patients: Summarizes the results of patient’s administrated linear analog tests for satisfaction.
The Post-Surgical Edema and Bruising Patients (Figure 10), showed a faster resolution with a mean of 6.95 days when treated with LED therapy than the control group, mean of 11.1 days (p<0001) that were treated with standardized oral corticosteroid therapy alone (Table 6). Eighty-five percent of the SaltFacial group reported less edema, bruising and discomfort by day 10 compared to only 10% of the control group. Seventy-six percent of the SaltFacial group reported less pain from the onset of treatment resulting in less pain medication consumed, compared to only 10% of the control group.
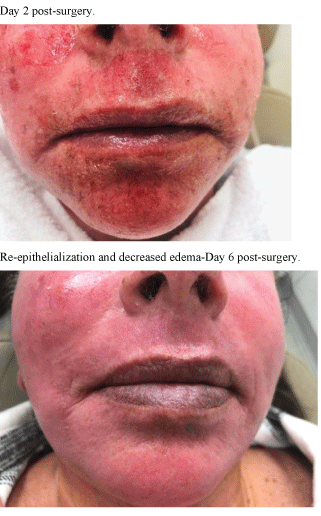
Figure 10: Wound healing patient (Facelift and skin resurfacing).
| SaltFacial | #Days | Control | #Days |
| 1 | 6 | 1 | 10 |
| 2 | 7 | 2 | 14 |
| 3 | 9 | 3 | 16 |
| 4 | 10 | 4 | 12 |
| 5 | 7 | 5 | 10 |
| 6 | 8 | 6 | 7 |
| 7 | 5 | 7 | 10 |
| 8 | 8 | 8 | 12 |
| 9 | 7 | 9 | 15 |
| 10 | 6 | 10 | 13 |
| 11 | 5 | 11 | 12 |
| 12 | 5 | 12 | 10 |
| 13 | 7 | 13 | 16 |
| 14 | 8 | 14 | 10 |
| 15 | 10 | 15 | 9 |
| 16 | 7 | 16 | 8 |
| 17 | 6 | 17 | 7 |
| 18 | 8 | 18 | 10 |
| 19 | 5 | 19 | 11 |
| 20 | 5 | 20 | 10 |
Table 6: Wound Healing: Number of days healing compared to control.
As the age demographic of patients seeking aesthetic improvement widens from Generation Z (12-25 years) to patients in their 70’s and 80’s, demand for non-surgical alternatives is also increasing. Systems having high intersecting points of safety and efficacy, providing patients with focused end-point results with minimal risk, minimal discomfort, and minimal downtime continue to see interest and implementation by treating physicians.
This study examines the combination of three modalities into a single treatment platform, as compared to microdermabrasion or hydrating facials alone. These include sea salt exfoliation, cavitating ultrasound to improve circulation and tissue permeability, and high intensity end point focused, wavelength specific LED phototherapy (SaltFacial). Each of these modalities individually have undergone scientific peer reviewed scrutiny. This is the first study examining the benefit of concomitant utilization.
Why sea salt? Historically, for thousands of years, salt has played a central role in developing civilization [1]. It has served as a currency, influenced the establishment of trade routes and cities, provoked and financed wars, and inspired revolutions and secured empires. For centuries, salt was used medically for its cleansing and healing properties, revealing it to be antibacterial, antimicrobial, a natural humectant, aiding in balancing pH, improved permeability, and reducing inflammation [1]. Sea salt and salt from pristine salt mines is comprised of 85% NaCl, and 15% trace minerals. Processed or refined salt contains 97.5% NaCl, and 2.5% toxic chemical additives which have been related to disorders such as hypertension and other cardiac diseases [1].
In 2011, the U.S. Departments of Agriculture, Health and Human Services issued their 7th edition of the Dietary Guidelines for Americans [2]. They listed twelve vitamins and nine minerals recognized as necessary for health and well-being. Sea salt contains all of these essential minerals. (Table 7) lists the mineral goals for adults based on dietary reference intakes and dietary guideline recommendations [2]. Biochemically, many enzymes require the presence of metal ions for catalytic activity. (Table 8) lists examples of several important metalloenzymes [2]. Early studies examined the oral intake benefits of the essential minerals, while more recently, the benefits of topically applied mineral salts have been studied [8]. The presence of these minerals in the sea salt contributes to the benefit of the SaltFacial over standard microdermabrasion.
| Mineral | Female | Male | Female | Male |
| 19-50 year | 19-50 year | 51+year | 51+year | |
| Calcium (mg) | 1000 | 1000 | 1200 | 1200 |
| Iron (mg) | 18 | 8 | 8 | 8 |
| Magnesium (mg) | 310-320 | 400-420 | 320 | 420 |
| Phosphorus (mg) | 700 | 700 | 700 | 700 |
| Potassium (mg) | 4700 | 4700 | 4700 | 4700 |
| Sodium (mg) | <2300 | <2300 | <2300 | <2300 |
| Zinc (mg) | 8 | 11 | 8 | 11 |
| Copper (μg) | 900 | 900 | 900 | 900 |
| Selenium (µg) | 55 | 55 | 55 | 55 |
Table 7: Mineral goals for adults based on dietary reference intakes.
Calcium is the most abundant mineral in the human body [9-13]. Its key roles include hemostasis and regulating epithelialization. It plays a large role in wound healing by regulating keratinocytes [10- 12]. Calcium is essential in maintaining skin’s barrier function, playing a major role in skin barrier repair. Barrier thickening assists skin in retaining moisture, thereby reducing visible wrinkles and dryness. This explains the improving Quantificare profiles of patients receiving the salt therapy.
Potassium [14] and sodium [15] are the bodies’ major cellular and extracellular electrolytes. In this role, they maintain cellular membrane potential. The positive electrolyte benefits to skin of bathing in the Dead Sea have been heralded for centuries [16].
Magnesium is critical for energy metabolism, cell replication, and skin barrier repair with calcium regulating keratinocyte function and production [17-25]. Two popular consumer products containing magnesium are talcum powder (magnesium silicate) and epsom salts (MgSO4). Talc is used as an astringent in baby powder, reducing wetness, in the perineal and axillary regions, while enhancing the smoothness of skin on other body areas. Epsom salts acts as a laxative internally, while enhancing keratinocyte softening and exfoliation when bathed in. It has been known as the relaxation mineral, activating the parasympathetic system and subsequently reducing oxidative stress [21].
Zinc is a prominent cofactor for many enzymes (Table 8), especially those involved in wound healing [26-29]. The use of many zinc salts is FDA-approved for treating numerous conditions [27]. Most common are sunscreens, dandruff treatments, and anti-fungal preparations.
| Element | Metalloenzyme | Function |
| Cu | Superoxide Dismutase | Superoxide decomposition (Antioxidant) |
| Lysyl Oxidase | Collagen, Elastin synthesis | |
| Collagen Proline Dioxygenase | Collagen synthesis | |
| Cytochrome Oxidase | Energy production | |
| Tyrosinase | Melanin formation | |
| Fe | Cytochrome C Reductase | Energy production |
| Aconitase | Intermediary metabolism | |
| Mg | Glucose 6-Phosphatase | Intermediary metabolism |
| Aconitase | Intermediary metabolism | |
| Hexokinase | Intermediary metabolism | |
| Mn | Catalase | Peroxide decomposition (Antioxidant) |
| Se | Glutathione Peroxidase | Peroxide decomposition (Antioxidant) |
| Zn | Matrix Metalloproteases | Matrix remodeling, Wound healing |
| Numerous Protein Kinases | Signal Transduction | |
| Numerous tRNA synthases | t RNA synthesis | |
| DNA/RNA Polymerase | DNA/RNA synthesis |
Table 8: Metalloenzymes.
Iron is one of the most abundant trace minerals in the body. It is most important in cellular oxygen transportation and oxygenreduction reactions involved with respiration [30-35]. Approximately 70% of the body’s iron is associated with hemoglobin.
Copper is an important trace mineral found throughout the body. It serves as a coenzyme for many enzymes including lysyl oxidase, responsible for cross-linking collagen, and tyrosinase, the enzyme involved in skin pigmentation. Several copper peptide complexes have been shown to calm irritated skin, improve elasticity, firmness, and accelerate wound healing [36]. Other copper compounds have shown antibacterial, anti-fungal, and antiviral properties [37].
Selenium is believed to protect the skin via it’s involvement with two antioxidant enzymes, glutathione peroxidase and thioredoxin reductase [38]. Human fibroblasts, keratinocytes and melanocytes express numerous selenoproteins essential for the well-being of skin [39].
Topical salt minerals therefore act as a nontoxic exfoliant, possessing natural antiseptic properties, killing pathogens and detoxifying skin while absorbing impurities and maintaining the normal microbiome of skin. The barrier protective function regulates transepidermal water loss preventing dryness and minimizing the appearance of wrinkles.
This unique delivery device, compared to traditional microdermabrasion devices, provides for a non-thermal customizable exfoliation and sea salt/mineral delivery, with the ability of fine tuning the intensity and depth of exfoliation from the stratum corneum to the reticular dermis. The positive pressure, no vacuum/suction handpiece eliminates the risk of suction-based adverse events, making it safe for all skin types. The handpiece angle of impact allows for efficient and uniform delivery of salt with little to no patient discomfort.
Why ultrasound? There have been many papers examining the benefits of cutaneous ultrasound for enhanced dermal delivery, stimulating neocollagenesis, elastin remodeling, as well as lipoapoptosis [40-54]. Utilizing 30MHz, pulsed delivery ultrasound provides a cavitation effect, increasing intercellular spaces thereby propelling agents through the stratum corneum and increasing passive epidermal and dermal permeability to topically applied materials.
When focused on subcutaneous tissues, the tissue can reach temperatures exceeding 60 degrees celsius yielding small coagulation points to a 5mm depth within the mid to deep reticular dermis, while leaving the epidermis and papillary dermis unaffected [55,56]. This can result in deep reticular collagen fiber denaturing, contraction, and neocollagenesis [44]. Clinically, as evidenced in this paper, this correlates with a “skin polishing” or “air brushing” effect yielding a reduction in fine lines, increased clarity and quality of skin and improved permeability with barrier restoration.
Why LED phototherapy? The past decade has seen further refinements in the utilization of light emitting diodes (LED) in the treatment of medical and aesthetic conditions [6,57-67]. LED phototherapy has been shown to have a broad utility in a wide variety of medical, aesthetic and surgical procedures. Their safety is one of the most attractive features of LED therapy. When used alone (without topical sensitizers), they are nonablative and nonthermal, and do not cause damage in the epidermis or dermis. Depending upon the desired outcome, and the target chromophore, different wavelengths of light are employed [57].
The most common wavelengths studied include blue, red, amber and infrared or near infrared. Blue light (414nm) has been widely shown to possess antibacterial properties, particularly against p. acnes, clostridium, staph aureus and MRSA [57-59]. This was shown repeatedly in this study. Red light (660nm) stimulates mitochondrial and fibroblast activity, increasing cellular proliferation, promoting healing, and reducing inflammation and erythema [60], also evidenced in our patient population. When combined together, antibacterial efficacy is improved [61]. Amber light (590nm) was also found to contribute to reducing inflammation and erythema. Further studies revealed that infrared (830nm) and near infrared (930nm) aided with vasodilation and stimulated fibroblastic activity and collagen production, further enhancing wound healing. This magnified the benefits of Red light [62-67]. This was successfully shown in our postoperative patient population.
Several technological advancements distinguish the LED system utilized in this study. The LED module features 3 large adjustable wraparound panels, each containing 1750 semi-coherent LED’s utilizing spectral power- (no scatter); with precision endpoint focused, wavelength specific, LED therapy. This yields a more concentrated, focused and powerful light emission (semi-coherent), capable of treating the face and neck simultaneously [68].
The wavelengths are pre-programmed into 4 specific treatment modes:
1. Acne therapy- combination of blue and red (20 minutes)
2. Photodynamic therapy (PDT)- blue (9 minutes)
3. Collagen restoration-combination of red and NIR (20 minutes)
4. Skin rejuvenation-combination of red and amber (20 minutes)
This paper has shown the synergistic positive effect of combining these three modalities for many aesthetic dermatological and surgical scenarios, including:
1. Maintenance of healthy skin physiology
2. Aging skin improvement
3. Acne therapy
4. “Covid 19 Era” tissue cleansing improving patient confidence
5. Pre and post procedure tissue cleansing (implants, threads)
6. Pre and post botulinum/filler injection edema reduction
7. Post-procedure reduction of edema, erythema, purpura, and pain
8. Improving scalp vascularity/hair growth
9. Reducing active infection time of healing
10.Pain mitigation
11. Successful “non-energy” form of skin rejuvenation
12.Pre- non-surgical ultrasound body sculpting (removal of stratum corneum prior, enhances ultrasound penetration and efficacy)
This study has shown the synergistic effect of combining sea salt exfoliation, cavitating dermal permeability enhancing ultrasound, and high intensity, endpoint focused, wavelength specific LED therapying in treating a variety of common aesthetic, medical, dermatological and surgical conditions. This combination therapy is a viable and valuable addition to the armamentarium of aesthetic non-surgical treatments to safely and effectively offer to patients of all ages and Fitzpatrick Skin Types 1 through 6. Additionally, it is a treatment that is performed by ancillary staff, thereby allowing the managing physician to treat other patients while this treatment is being performed.
Further study will yield enhancements in the efficacy of this valuable combination therapy.
Download Provisional PDF Here
Aritcle Type: RESEARCH ARTICLE
Citation: Chernoff G (2021) A Novel Combination Therapy in Aesthetic and Reconstructive Surgery: Sea Salt, Exfoliation, Cavitating Ultrasound, and High Intensity Multiwavelength LED Treatment: (SaltFacial). J Clin Cosmet Dermatol 5(2): dx.doi.org/10.16966/2576-2826.162
Copyright: © 2021 Chernoff G. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access