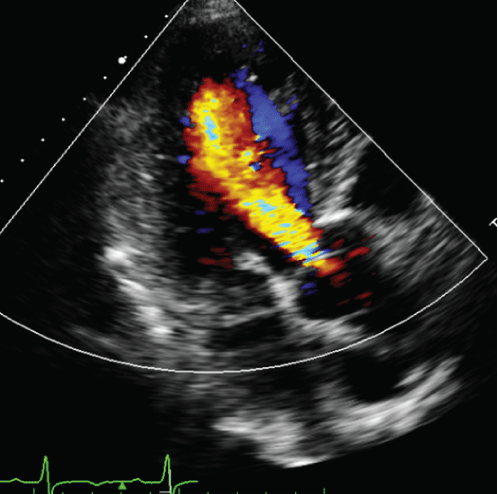
Figure 1: Preoperative echocardiogram showing a grade 3 aortic regurgitation.


Hideyuki Harada1* Hiroyuki Miyamoto1 Tomoki Nakastu1 Fumiaki Kimura1 Toshio Baba1 Kiminari Ito2
1Department of Cardiovascular Surgery, Kushiro Kojinkai Memorial Hospital, Japan*Corresponding author: Hideyuki Harada, MD, Department of Cardiovascular Surgery, Kushiro Kojinkai Memorial Hospital 191-212 Aikoku, Kushiro-shi 085-0062, Japan, Tel: 0154-39-1222; Fax: 0154-54-0330; E-mail: h_harada@kojinkai.or.jp
Reports of the clinical results of cardiac surgery in patients with Essential Thrombocythemia (ET) are rare. In addition, cases of aortic arch aneurysm in ET have not been previously reported. We present a successful aortic valve and arch replacements with the frozen elephant trunk technique using hypothermic circulatory arrest in an ET patient with grade 3 aortic regurgitation and arch aneurysms. Reducing platelet count via the administration of anagrelide and the careful balancing of antiplatelets and anticoagulants is essential in determining the outcome of surgery.
Aortic arch aneurysm; Aortic valve replacement; Hypothermic circulatory arrest; Essential thrombocythemia; Frozen elephant trunk technique
Reports of the clinical results of cardiac surgery in patients with essential thrombocythemia (ET) are rare [1-3]. In addition, cases of aortic arch aneurysm in ET have not been previously reported. We present a successful aortic valve and arch replacements with the Frozen Elephant Trunk (FET) technique using Hypothermic Circulatory Arrest (HCA) in an ET patient with grade 3 Aortic Regurgitation (AR) and arch aneurysms.
A 60-year-old male was referred to our hospital with cerebral infarction with symptoms of mild right hemiparesis and dysarthria. He accepted the conservative therapy and rehabilitation for cerebral infarction. He had been followed by a hematologist for two years with a diagnosis of ET, and had been treated with hydroxyurea and anagrelide for platelet reduction, and aspirin for preventing thrombosis. On admission, his blood pressure was 168/92mmHg and his pulse was 81/min and regular. He had a grade 4/6 systo-diastolic murmur at the left sternal border. A chest X-ray showed a slight enlarged heart (52% cardiothoracic ratio). An electrocardiogram revealed left ventricular hypertrophy and QS pattern in leads V1 to V3. Echocardiogram demonstrated a grade 3 AR (Figure 1). The Left Ventricular Diastolic Dimension (LVDs) was 64.4mm, the left ventricular systolic dimension (LVDs) 54.1mm, and the Left Ventricular Ejection Fraction (LVEF) 25% (Figure 2). The patient had a blood platelet count of 386 × 109/L. The patient was administered hydroxyurea 500mg/day and anagrelide 3mg/day. His LDL cholesterol was elevated (185mg/dL) and his HDL cholesterol was low (34mg/ dL). Computed Tomographic (CT) angiography demonstrated a saccular aortic arch aneurysm (Figure 3). Coronary angiography revealed a 95% stenosis at the Left Anterior Descending (LAD) and 90% stenosis at the Left Circumflex coronary artery (LCx) (Figure 4). PCI (Percutaneous Coronary Intervention) to LAD was performed at that time. DAPT (Dual Antiplatelet Therapy) with prasugrel and aspirin was commenced. One month later, PCI to LCx was done without complications. Despite treatment with vasodilators and diuretics, shortness of breath upon slight exertion continued. On the basis of these findings, aortic valve and arch replacements combined with FET technique was offered to the patient with ET and he selected to proceed, despite the operative risk. Hydroxyurea was discontinued 14 days before surgery and aspirin 7 days before surgery. Anagrelide and prasugrel were continued until the day before the operation. The patient presented with an immediate preoperative platelet count of 187 × 109 /L and hemoglobin concentration of 12.5g/dL.

Figure 1: Preoperative echocardiogram showing a grade 3 aortic regurgitation.
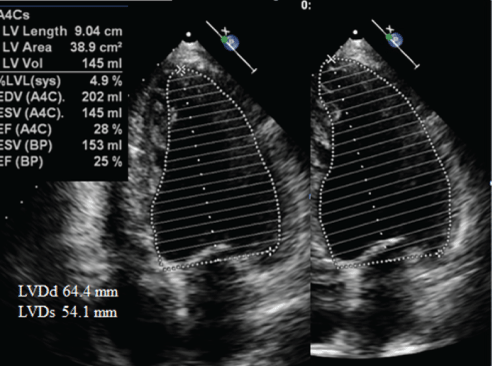
Figure 2: Preoperative echocardiogram showing that the LVDs was 64.4mm, the LVDs 54.1mm, and the LVEF 25%.
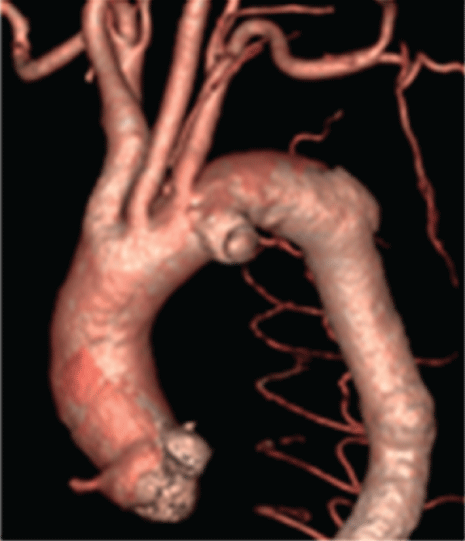
Figure 3: Preoperative computed tomographic angiography showing a saccular aortic arch aneurysm.
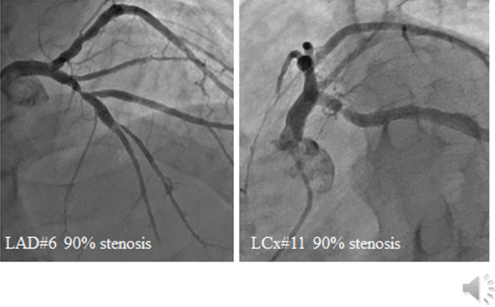
Figure 4: Coronary angiography showing a 90% stenosis at the left anterior descending and 90% stenosis at the left circumflex coronary artery.
The operation was performed under general anesthesia, and the sternum was opened. After heparin sodium 300IU per kg bodyweight had been given intravenously, the Activated Coagulation Time (ACT) increased from 130 seconds to 446 seconds. Cardiopulmonary Bypass (CPB) was commenced by Ascending Aorta (AA) blood delivery and superior and inferior vena cava blood removal and the Body Temperature (BT) was reduced to 22°C. A venting tube was inserted into the LV via the right upper pulmonary vein. The AA was crossclamped, and myocardial protection was achieved by using ante grade Cold Blood Cardioplegia (CBC). Partial bypass altered to total bypass. The right atriotomy was made. The cannula for retrograde perfusion was placed into the coronary sinus. The retrograde CBC was continued. On the other hand, an 8mm hemashield graft (Boston Scientific, Wayne, NJ, USA) was anastomosed to the left axillary artery with 5-0 polypropylene sutures. During reducing temperature, the Innominate Artery (INN), Left Common Carotid Artery (LCCA) and Left Subclavian Artery (LSA) were exposed. The AA was incised and transected about 15 mm above the sinotubular junction. The aortic valve was inspected. The aortic valve annulus was enlarged. The noncoronary cusp had been fallen into the LV. Three cusps were thin. AR was evident. Therefore, the cusps were extirpated and a 25mm CEP bioprosthetic valve (Carpentier Edwards Perimount Magna Ease, Edwards Lifesciences, Ivine, CA, USA) was fixed there. At 22°C rectal, the LSA was clamped with a 15mm metal clip and ligated with a tape near its branching from the arch. Selective Cerebral Perfusion (SCP) was started. The LSA was perfused via the 8mm hemashield graft anastomosed to the left axillary artery. After the INN and LCCA were clamped, and HCA was instituted. The aortic arch was incised and inspected. The aneurysmal sac with mural massive thrombi was seen within the aortic arch. The proximal INN and LCCA were transected and perfused via cannulae. The origin of LCCA was closed. The aortic arch was transected between the INN and LCCA. The FROZENIX delivery system (JOSG-29120570N, Japan Lifeline, Tokyo, Japan) was deployed. For the distal anastomosis, four 4-0 polypropylene stay sutures were placed with reinforcement by a felt strip. A 28-mm-fourbranched J graft (J Graft SHIELD NEO, Japan Lifeline, Tokyo, Japan) was anastomosed to the distal aortic arch with 3-0 polypropylene continuous sutures with a felt strip. The graft was clamped. Antegrade arterial perfusion was started via the branch of the graft. BT was gradually elevated. The proximal anastomosis between the graft and the AA was then made with 3-0 polypropylene continuous sutures using a felt strip. Antegrade warm blood cardioplegia was given and air was evacuated from the AA and LV. Antegrade warm blood perfusion was started and the AA was vented. The heart was defibrillated spontaneously. The AA was unclamped. The LCCA was reconstructed using one branch of the four-branched graft with 4-0 polypropylene sutures. Air was evacuated from the graft and the circulation to the LCCA was restored via the graft. The INN was also reconstructed in the same manner in turn. The left axillary artery was reconstructed using one branch of the four-branched graft through the left second intercostal space, rather than reconstruction of the LSA inside the mediastinum. SCP was terminated. The patient was weaned from CPB without the use of intraaortic balloon pumping. Protamine sulfate 200mg was administered intravenously to neutralize heparin, and the ACT returned to 143 seconds. The total CPB time was 281 minutes, and the aortic cross-clamp time was 181 minutes, and the SCP time was 80 minutes. During the operation, the patient received 3080mL of red blood cell transfusion, 720mL of frozen plasma transfusion and 800mL of platelet transfusion. The patient was extubated 15 hours later. Heparin was started with 10,000 unit intravenous injections per day. A platelet count was 144 × 109 /L on postoperative day (POD) 1. On POD 5, the platelet count increased to 428 × 109/L. A dose of anagrelide (4mg/day) was re-started. Aspirin 100mg/day, prasugrel 3.75mg/day and warfarin controlled at Prothrombin TimeInternational Normalized Ratio (PT-INR) from 1.5 to 2.5 were started on POD 6. Heparin was stopped when PT-INR level reached 1.65 on POD 9. On POD 11, the platelet count decreased to 224 × 109/L. A dose of anagrelide was decreased from 4 mg to 3 mg/day with daily monitoring of the platelet count (Figure 5). On POD 28, the patient was discharged on a regimen of anagrelide (3mg/day), aspirin, prasugrel, and warfarin, with a platelet count of 364 × 109 /L (Figure 6). On postoperative echocardiogram, the LVDd and LVEF improved to 43.1mm and 52%, respectively (Figure 7). Warfarin was discontinued 3 months after surgery, and anagrelide and DAPT with aspirin and prasugrel are currently continuing. The patient is doing well in NYHA class I for three years after surgery, with no episodes of thrombosis or bleeding.
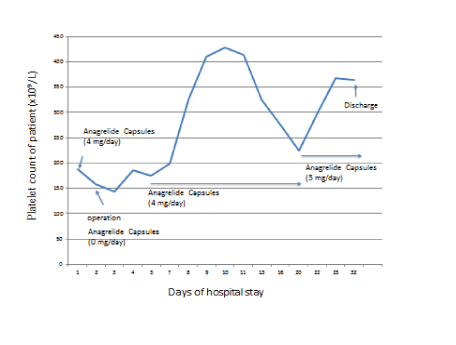
Figure 5: Transition of platelet count and dosage of anagrelide.
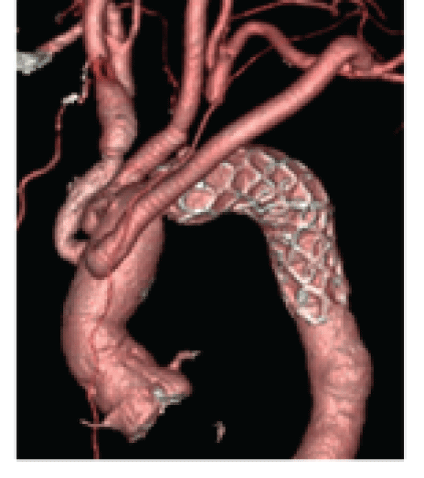
Figure 6: Postoperative CT angiography (one-month after surgery).

Figure 7: Postoperative echocardiogram showed the LVDd and LVEF improved to 43.1mm and 52%.
ET is a rare chronic myeloproliferative disease characterized by unexplained thrombocytosis (>450 × 109 /L). Patients often are asymptomatic; however, thrombosis and less frequently hemorrhage of the cerebral, coronary, and peripheral vessels are reported complications [1]. Hydroxyurea, anagrelide, alpha interferon, and plateletpheresis are the most common cytoreductive therapies, with the goal of maintaining platelet counts less than 400 × 109 /L [1]. Especially, high-risk ET patients (age ≥ 60 years, or history of thrombosis, or platelet count ≥ 1500 × 109 /L) should be treated with a cytoreductive therapy and low-dose aspirin [3]. Reports of the clinical results of cardiac surgery in patients with ET are rare [3]. There are no brief guidelines for patients with ET undergoing cardiac surgery [4,5]. Gurrieri C, et al. [6] investigated 25 ET patients who underwent cardiac operations and 18 patients identified in available literature related to this population. They concluded that it was reasonable for patients presenting for cardiac operations to undergo cytoreduction targeting a platelet count of less than 800 × 109 /L, and perhaps lower, to reduce the risk of catastrophic thrombotic or hemorrhagic complications, or both, in the preoperative period.
Although there has been a report of AVR with graft replacement for aortic valve stenosis with ascending aortic enlargement in a patient with ET [3], to our knowledge, there have been no reports of AVR with graft replacement for AR with arch aortic aneurysm, and the present case report seems to be the first one.
Concerning the surgical procedure in the present case, since the invasion is large in the one-staged operation for AR with severely impaired LV function and the aortic arch aneurysm, hybrid debranching surgery might be considered. Hybrid debranching surgery has the advantages of avoiding HCA, reducing the time of aortic cross-clamp and reducing intraoperative bleeding [7]. Its short-term and long-term mortality are similar to TAR with FET. However, there are reports that the hybrid debranching procedure has more permanent neurological complications in results than TAR with FET [8]. Permanent neurological complications after hybrid surgery are considered to be related to aortic atherosclerosis. The surgical operation in the aortic arch and the delivery and release of stents may cause the rupture of atherosclerotic plaques and cause neurological complications. Sideclamping of the ascending aorta may cause the atherosclerotic plaque of the AA to rupture and cause neurological complications [8]. On the other hand, HCA is an effective brain protection technique, and the FET technique has been used worldwide in recent years [9]. But a major concern caused by HCA is hypothermia-induced coagulopathy [10]. Before and after the operation, anagrelide was administered in the present case. Anagrelide reduces platelets without increasing platelet coagulation activity markers such as platelet factor 4 compared to hydroxyurea, and there is no difference in the frequency of thrombosis or bleeding [11]. Anagrelide is useful for performing perioperative platelet reduction therapy in cardiac surgery, such as using heparin [12].
In the present case, aspirin in addition to a P2Y12 platelet receptor inhibitor was administered after PCI. In the post-PCI population in general, dual therapy with aspirin in addition to a P2Y12 platelet receptor inhibitor has become increasingly common [1,13], although there are no consensus guidelines regarding antiplatelet therapy in patients with ET undergoing PCI. P2Y12 blockade prevents platelet activation during CPB and hypothermia. Owing to its short half-life, platelet inhibition can be well controlled, thus potentially reducing bleeding complications. This novel pharmacological strategy has the potential to reduce complications associated with CPB and hypothermia [14].
Although the present case had a high-risk ET, and his cardiac function had been severely impaired, good results were obtained by appropriate administration of anagrelide, aspirin and prasugrel in the perioperative period. Before the operation, an anarelide treatment by a hematologist controlled his platelet count to around 400 × 109/L. His cardiac function was remarkably improved by AVR following PCI. The patient has a good progress at the present three years after surgery, but it seems important to continue to follow up closely in cooperation with a hematologist in the future.
We presented a successful aortic valve and arch replacement with the FET in a high-risk ET patient with grade 3 AR and arch aneurysms. Reducing platelet count via the administration of anagrelide and the careful balancing of antiplatelets and anticoagulants is essential in determining the outcome of surgery
Written informed consent was obtained from the patient for the publication of this case report.
All authors have no conflict of interest.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: Harada H, Miyamoto H, Nakastu T, Kimura F, Baba T, et al. (2022) Aortic Valve and Arch Replacements in a High-Risk Patient with Essential Thrombocythemia. J Clin Case Stu 7(1): dx.doi.org/10.16966/2471-4925.251
Copyright: © 2022 Harada H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access