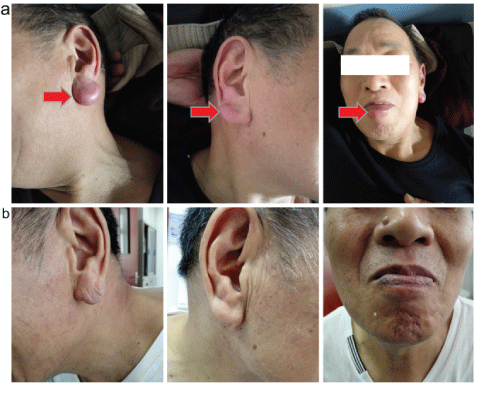
Figure 1: a) Multiple cutaneous lesions at diagnosis and b) after treatment.


Teng Yu* Qiaohong Ying Xuzhao Zhang
Department of Hematology, the Second Affiliated Hospital of Zhejiang University School of Medicine, Hangzhou, Zhejiang, China*Corresponding author: Teng Yu, Department of Hematology, the Second Affiliated Hospital of Zhejiang University School of Medicine, No.88, Jiefang Road, Hangzhou, Zhejiang 310009, PR, China, E-mail: yutengzju@zju.edu.cn
Introduction: Skin involvement is less common in chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL) than that of aggressive lymphoma such as diffuse large B cell lymphoma and T cell lymphoma. Cutaneous lesion as an initial presentation of CLL/SLL is even more rarely. While CLL/SLL presenting in the skin has been reported, to our knowledge it has never been described in the context of such as earlobes.
Patient concerns: Here we report a case of a CLL/SLL patient with multiple cutaneous lesions as initial presentation. This patient had cutaneous lesions before the typical elevated lymphocyte in peripheral blood.
Diagnosis: Cutaneous lesion pathology test diagnosed the patient as SLL. PET-CT scan shows elevated SUV value in these cutaneous lesions instead of lymph nodes.
Interventions: There is lack of guideline for treatment of CLL/SLL with cutaneous involvement. The patient received 5 cycles of fludarabine plus cyclophosphamide.
Outcomes: The patient got complete response and having been well during following up.
Conclusion: Cutaneous involvement could be present at early stage, although it is very rare, in CLL/SLL patient. This rare presentation sometimes maybe confuses the diagnosis at the beginning. The differential diagnosis depends on high quality pathology diagnosis. Cutaneous lesions are more sensitive than lymph nodes to PET-CT scan. Cutaneous involvement maybe is not a poor predicative factor for CLL/SLL.
Cutaneous involvement; CLL/SLL; Initial presentation; PET-CT
CLL/SLL: Chronic Lymphocytic Leukemia/Small Lymphocytic Lymphoma; CBC: Complete Blood Count; PET-CT: Positron Emission Tomography-Computed tomography; 18F-FDP: 18F-Fluorodipalmitin; HBsAg: Hepatitis B Surface Antigen; HBeAb: Hepatitis B e Antibody; HBcAb: Hepatitis B Core Antibody; LDH: Lactate Dehydrogenase; FISH: Fluorescent In Situ Hybridization; IGHV: Immunoglobulin Heavy Chain Variable Region; CTCLs: Cutaneous T-Cell Lymphomas; CBCLs: Cutaneous B-Cell Lymphomas; NK/T Cell Lymphoma: Natural Killer/T Cell Lymphoma; DLBCL: Diffuse Large B-cell Lymphoma; NCCN National Comprehensive Cancer Network; MCL: Mantle Cell Lymphoma; MBL: Monoclonal B-cell Lymphocytosis; PLL: Prolymphocytic Leukemia; HCL: Hairy Cell Leukemia; FL: Follicular Lymphoma; LPL Lymphoplasmacytic Lymphoma
Chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL) is a common hematological malignant over through the world, especially in elder population [1]. The usual presentations of CLL/SLL are elevated clonal CD5+CD23+ B lymphocytes in peripheral blood and/or enlarged lymph nodes [2]. Cutaneous involvement is not common in CLL/SLL compared with that of aggressive lymphoma such as diffuse large B cell lymphoma and T cell lymphoma. But there are some rare cases that reported as uncommon presentations including cutaneous lesion, which may increase the difficulties for differential diagnosis or induce misdiagnosis. Here we report a rare case that initially presents multiple cutaneous lesions.
A 63-year old man present with continuing enlarged left earlobe and lower lip for over 1 years, enlarged right earlobe for two months. This patient is a farmer and has been well until 1 year ago he found his left earlobe and lower lip enlarged with slightly rash and pruritus. At that time, he felt well except the above symptoms. He went to see the doctor in the local hospital and blood tests including complete blood count (CBC) were normal. He accepted anti-inflammation and anti-allergic therapies but has no response. Because traditionally Chinese people believe that large earlobe indicates lucky, so this patient regarded his enlarge earlobe as a sigh of lucky and did not see more doctors for help. Two months before admission, his right earlobe was also enlarged with significant pruritus (Figure 1). Then the patient went to see the dermatologist, a biopsy of enlarged left earlobe was performed. Pathology image showed that corium layer was infiltrated with smeared nodular lymphocytes, epidermal layer was not infiltrated obviously (Figure 2A). Majority of the infiltrated cell were small lymphocytes, which is a little bigger than normal lymphocyte, with circular nuclear, lumpy chromatin, very little small nucleolus and rare mitotic (Figure 2B, 2C). Then the diagnosis was made as a small lymphocytic lymphoma, immunohistochemistry showed CD5+, CD20+++, CD79a+++, CD23+, CD10-, Bcl-6-, Bcl-2- ,CD3 background+, CK (AE1/AE3)-, EMA-, Ki-67 30%+, Kappa(k) focal+, Lambda focal+, CD21 focal+, CyclinD1 background+, TdT -, CD99 -, CD38 -(Figure 2 and FigureS1). He has history of chronic hepatitis B virus carrying for over 20 years. The family history and personal history are negative.

Figure 1: a) Multiple cutaneous lesions at diagnosis and b) after treatment.
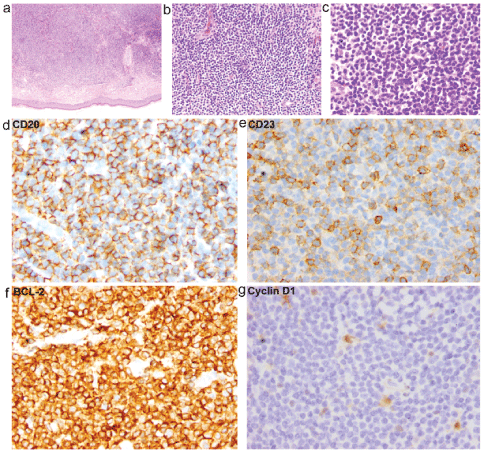
Figure 2: a) Corium layer was infiltrated with smeared nodular lymphoid cells, epidermal layer was not infiltrated obviously. b, c) Majority of the infiltrated cell were small lymphocytes, which is a little bigger than normal lymphocyte, with circular nuclear, lumpy chromatin, very little small nucleolus and rare mitotic. d) Immunophenotype of the cutaneous infiltrate CD20 positive, e) CD23 positive, f) BCL-2 positive, and g) Cyclin D1 negative.
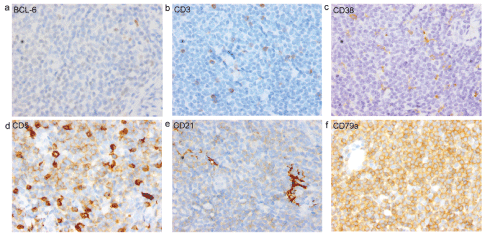
Figure S1: a) Immunophenotype of the cutaneous infiltrate BCL-6 negative, b) CD3 negative, c) CD 38 negative, d) CD5 positive, e) CD21 negative, and f) CD79a positive.
After admission, the CBC test showed elevated peripheral blood white blood cells of 12.2 × 10 ^ 9/L, lymphocyte count was 8.72 × 10 ^ 9/L, B lymphocyte count was 6.8 × 10 ^ 9/L, Hemoglobin and platelet were normal. Hepatitis B surface antigen (HBsAg), antiHepatitis B e antibody (HBeAb) and Hepatitis B core antibody (HBcAb) were positive. Hepatitis B virus (HBV)-DNA was 812 IU/ mL. Tumor markers were normal. Direct and indirect Coomb’s test were both negative. B ultra sound showed slightly splenomegaly (5.2 cm thick) and no enlarged lymph node. Peripheral blood cell flow cytometry showed clonal population of lymphocyte positive for HLADR, CD19, CD22 (dim), CD5, CD23 and sLambda (dim), partial cell positive CD11c, CD20(dim), considering for CLL/SLL. Bone marrow smear showed elevated lymphocyte of 75.5%. Fluorescent in situ hybridization (FISH) analysis of bone marrow showed loss of 13q14.3 (favorable marker), immunoglobulin heavy chain variable region (IGHV) mutation >2% (favorable marker) and no lost of TP53/CEP17 (poor prognostic marker). ZAP-70 positive was 3%. Karyotype was normal. PET/CT showed left earlobe and lower lip soft tissue SUV value elevated considering lymphoma, both sides of neck and mediastinum lymph nodes SUV elevated considering lymphoma possible (Figure 3 and Figure S2). LDH was normal. After evaluation this patient was considering stage Binet B with symptom of pruritus. The patient had no fatigue, bodyweight loss nor night sweat. According to iwCLL guideline for treatment criteria, this patient had symptomatic extranodal involvement of skin [3]. And this patient had a vision to accept chemotherapy because of pruritus. Therefore, this patient meets the indication for CLL treatment.
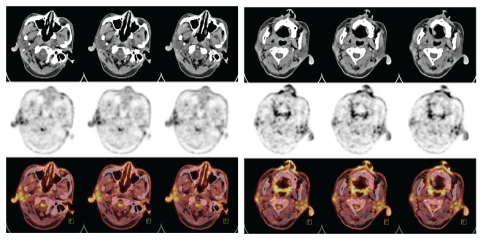
Figure 3: Both earlobes were showed positive under PET-CT.
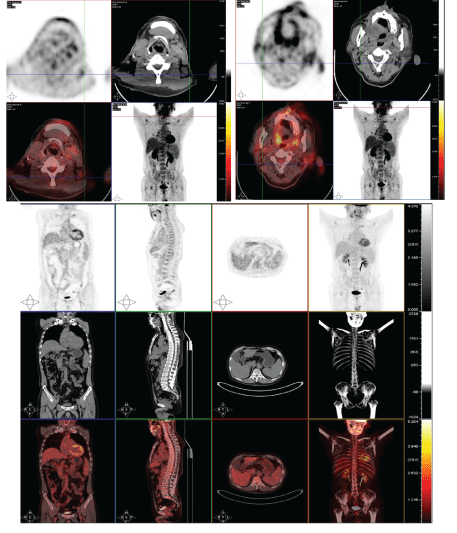
Figure S2: PET-CT.
After excluding contraindication for chemotherapy, this patient refused to rituximab for worrying about the risk of HBV reactivation and accepted fludarabine plus cyclophosphamide (FC) chemotherapy. After finishing 5 cycles of FC chemotherapy, this patient’s lymphocyte in peripheral blood was normal, both earlobes and lower lip were nearly normal size and no rash or pruritus (Figure 1). This patient achieved complete response and having been well during the regular following up.
CLL/SLL is the most common indolent lymphoma characterized by clonal expansion of B lymphocytes with distinct morphology and Immunophenotype [3]. CLL/SLL patient usually has an insidious onset during the early course and may only be recognized when leukocytosis is found on routine complete blood cell count or continuing enlarged lymph node that diagnosed by pathology test. Cutaneous involvement in CLL/SLL is less common comparing with T-cell leukemia or lymphomas but increasing in the later stages of the disease. Cutaneous lesion could be seen in up to 25% of patients with CLL, which is regarded as a relatively good prognosis [4,5], and may be expressed in a spectrum of lesions including erythematous plaques, papules, nodules, erosions, telangiectasias and papulovesicles [6-8]. But cutaneous involvement still is a rare initially present especially in asyptomatic CLL/SLL patients. Only few cases were reported with an initial cutaneous plaque [9]. This fact increases the difficulty for differential diagnosis of this kind of cutaneous lesion. So review of the characters of cutaneous involvement of CLL/SLL will help for diagnosis and differential diagnosis.
Cutaneous lesions should be differential diagnosis among inflammation, allergenic disease, connective tissue disease, solid tumor malignance and hematologic malignance including lymphoma. A population-based study of 3884 cutaneous lymphomas cases in the United States during 2001-2005, shows that cutaneous T-cell lymphomas (CTCLs) accounted for 71%, whereas cutaneous B-cell lymphomas (CBCLs) accounted for 29% and SLL accounted only 0.8% [10]. Another review of 517 cutenous lymphoma patients from Korea shows that the trunk area is the preferentially affected area(40.2%), the most frequent subtypes in order of decreasing prevalence were mycosis fungoides (22.2%), peripheral T-cell lymphoma (17.2%), CD30+ T-cell lymphoproliferative disorder (13.7%), and extranodal natural killer/T (NK/T) cell lymphoma, nasal type (12.0%). Diffuse large B-cell lymphoma (DLBCL) accounted for 11.2% of cases, other types of B-cell lymphoma accounted for less than 1% of cases [11]. These data prove that cutaneous involvement is not a common present for CLL/SLL, which increases the difficulty for diagnosis. There are no distinguished clinic characters of cutaneous small lymphocytic lymphoma. Differential diagnosis should depend on pathology. Cutaneous small lymphocytic lymphoma usually present as a painless nodules sometimes with rash and/or pruritus. Because CLL/SLL usually could cause allergenic reaction, the major of these cutaneous nodules were initially treated as allergenic disease and could have some response at first but relapse repeatedly.
The diagnosis of skin involvement depends on pathology test. Typical pathology characters of cutaneous CLL/SLL are nodular-diffuse and band-like infiltrates of small, monomorphous CD19+, CD20+ (dim), CD5+, CD23+ lymphocytes. Besides this typical immune pattern, CyclinD1 and/or Sox11 also should be involved to different with mantle cell lymphoma (MCL). For peripheral white blood cell increased cases, CLL also should differential with monoclonal B-cell lymphocytosis (MBL), prolymphocytic leukemia (PLL), Hairy Cell Leukemia (HCL), Follicular Lymphoma (FL) and lymphoplasmacytic lymphoma (LPL). For some rare CD5- CLL/SLL cases the diagnosis should be very carefully. If patient has previous CLL/SLL history or accelerate very quickly, the richet syndrome (CLL transform) should be considered because skin involvement in DLBCL is more common than that of CLL/SLL.
According the national comprehensive cancer network (NCCN) guideline for CLL/SLL evaluations for staging and treatment are slightly different from aggressive lymphoma. The common evaluation test for CLL/SLL include blood test for clonal B lymphocyte, CBC, direct coomb’s test and LDH and B ultra sound for lymph node and abdomen, enhanced CT for chest and abdomen. PET/CT scan is not recommended for CLL but can assist in directing nodal biopsy if richter’s transformation is suspected. In the present case, the PET-CT scan shows the multiple skin involvement which indicates that skin lesions maybe more sensitive than lymph nodes for 18F-fluorodipalmitin (18F-FDP) intake. Presently, there is lack of recommendation for staging and treatment of CLL/SLL with cutaneous involvement. When and how these patients with cutaneous lesions should be treated is still undefined. In present case, the patient had isolated three part of cutaneous involvement, as well as obvious symptom of pruritus. Also, the patient had a strong vision to be treated. So, we staged this patient with CLL Bient B or SLL staging system (Lugano Modification of Ann Arbor Staging System) stage IV, and treated this patient with FC and got a good response. But whether it was a right time for the treatment and if there were other suitable treatment strategies for this kind of patients still need to be further discussed.
This case is unique for having an initial presentation of non-trunk skin multiple involvements before lymphocyte increase in peripheral blood. This initial presentation is very rare for CLL/SLL patient. To our knowledge, there are rare cases with initial body skin involvement had been reported [12], which is different from the non-trunk skin involvement of this case. This kind of rare presentation sometimes could confuse the diagnosis and need to be pay attention to. The skin involvements do not influence the out-come, and the cutaneous lesions seem to be more sensitive for 18F-FDG intake than lymph nodes. More cases are needed to be collected for more comprehensive characters of this kind of disease.
This case study was approved by the ethics committee of the second affiliated hospital of Zhejiang University School of Medicine.
This case was consent by the patient for publication.
Pathology pictures and PET-CT pictures as supplemental materials.
The authors declare that they have no competing interests.
This work was supported by a grant from Zhejiang Provincial Natural Science Foundation of China (LY21H08005 to Yang Xu, Teng Yu).
Yu T and Ying Q designed the study and collect the data, Yu T. and Zhang X. wrote the manuscript. All authors have read and approve the final manuscript.
We thank Dr. Jinfan Li, from the Department of Pathology the second affiliated hospital of Zhejiang University School of Medicine, for the kindly help in preparing the pathology pictures and drafting the manuscript. We also thank Dr. Lin Chen, from the Medical PET Center of the Second affiliated hospital of Zhejiang University School of Medicine, for the kindly help in preparing the PET-CT.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: Yu T, Ying Q, Zhang X (2022) An unlucky Man with “Lucky” Earlobes: A Case Report of CLL/SLL with Cutaneous Lesions as the Initial Presentation. J Clin Case Stu 7(1): dx.doi.org/10.16966/2471-4925.246
Copyright: © 2022 Yu T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access