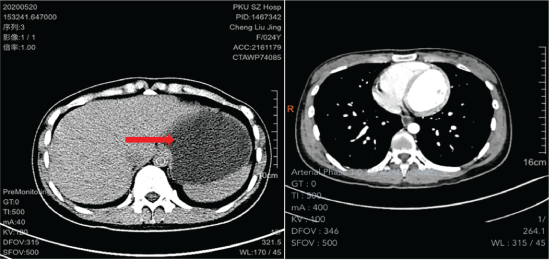
Figure 1: Computed Tomography (CT) showed the left retroperitoneal tumor, with a size of 65.3mm × 55.4mm × 99mm, clear border, single room, and cystic mass.


Liusheng Wu1,2 Xiaoqiang Li1,2* Jian Li3 Yanwei Lai4*
1Peking University Shenzhen Hospital, Clinical College of Anhui Medical University, Shenzhen, Guangdong, 518036, China*Corresponding author: Yanwei Lai, PhD, Professor, Department of Pharmacy, Peking University Shenzhen Hospital, Shenzhen, Guangdong, 518036, China, E-mail: 505272751@qq.com
Xiaoqiang Li, PhD, Professor, Department of Thoracic surgery, Peking University Shenzhen Hospital, Shenzhen, Guangdong, 518036, China, E-mail: dr.lixiaoqiang@gmail.com
Background: PRMC is a very rare benign tumor of the abdominal cavity that usually occurs in women, and PRMC demonstrate no specific findings on CT. There are many reports on the differential diagnosis and discussion of PRMC imaging, but there are few reports on the treatment of dedifferentiated PRMC using laparoscopic resection and postoperative follow-up.
Case summary: A mass was discovered in the left abdomen of a 24-year-old woman during a physical examination 6 years ago, and she suddenly developed paroxysmal pain in her left middle abdomen 4 months prior. The imaging examination revealed that a large cystic lesion on the left abdomen and part of the small intestine had a slight dilation of the liquid-gas plane in the left middle and lower abdomen. Besides, she also had incomplete obstruction of the small intestine, and it was not clear whether this was caused by the mass in the left abdomen. Following multidisciplinary team discussion, we finally decided to perform laparoscopic exploration and those of cancer antigen (CA) 19-9 and 125 (CA125) were elevated. Pathological examination results: dedifferentiated PRMC.
Conclusion: Laparoscopy can effectively treat giant retroperitoneal mucinous cystadenoma with obvious therapeutic effects, and there is no tumor recurrence.
Primary retroperitoneal mucinous cystadenoma (PRMC); Laparoscopic surgery; Large adenomas; Retroperitoneal tumor; Case report; Surgery
PRMC was first described by Calo PG, et al. in 1924 [1]. PRMC is an extremely rare disease, and its biological behavior still lacks sufficient evidence-based medical evidence. The clinical manifestation of patients is an abdominal mass with paroxysmal pain in the mid-abdomen, and its symptoms are not specific and are often misdiagnosed by doctors, so attention needs to be paid. Interestingly, relevant literature reports that PRMC almost always occurs in female patients, and its pathogenesis is unclear [2]. In many discussions, whether sex differences are a key factor in the pathogenesis of PRMC is still unknown. This article reports a case of a young woman with a giant retroperitoneal mucinous cystadenoma successfully resected under laparoscopic surgery and reviews the literature.
A 24-year-old woman had intermittent left abdominal pain for 4 months.
The patient had no previous medical history.
Computed tomography (CT) showed an oval low-density shadow on the left paracolic sulcus, with clear edges, a size of 65.3mm × 55.4mm × 99mm, uniform internal density and a CT value of 4.6Hu (Figure 1). Because part of the small intestine was compressed by the tumor, the patient developed incomplete intestinal obstruction and intermittent abdominal pain. The performance of the patient’s intestinal obstruction and abdominal pain was exacerbated, so we planned to use laparoscopic exploration to relieve tumor compression. To avoid damaging the blood vessels of important organs during the operation, we needed to know the blood supply of the tumor and its adhesion to adjacent tissues (Figure 2).

Figure 1: Computed Tomography (CT) showed the left retroperitoneal tumor, with a size of 65.3mm × 55.4mm × 99mm, clear border, single room, and cystic mass.
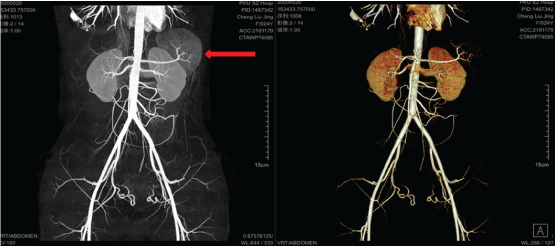
Figure 2: The vascular reconstruction image showed that there was less blood supply in the cyst and that it contained clearer fluid.
Under laparoscopy, we observed that the inner and outer walls of the tumor were smooth, and adhesion to the surrounding tissues was not tight (Figure 3). Because the phrenic nerve was stimulated when the top of the tumor was surgically stripped, the patient had respiratory depression during the operation.
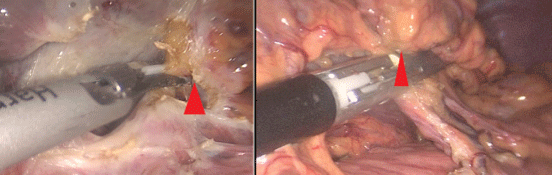
Figure 3: The intraoperative image showed the large, smooth outer wall of the posterior peritoneum on the left side, which did not adhere closely to the surrounding tissues, and A small amount of fat tissue can be seen on the surface of the mass and the surrounding area under laparoscopy.
The pathology report showed that the retroperitoneal cyst was a large vesicle with a size of 11.5cm × 8.5cm × 3.5cm, and it contained clear liquid, had a smooth outer wall with a size of 0.1cm-0.2cm and had a small amount of adipose tissue attached to the local surface (Figure 4). The results of immune histochemical examination showed that part of the cyst had a single layer of cubic or flat glandular epithelium. Some mucous columnar epithelial cells were positive for CDK7, ER, AB (Alcian Blue) and PAS (Figure 5).
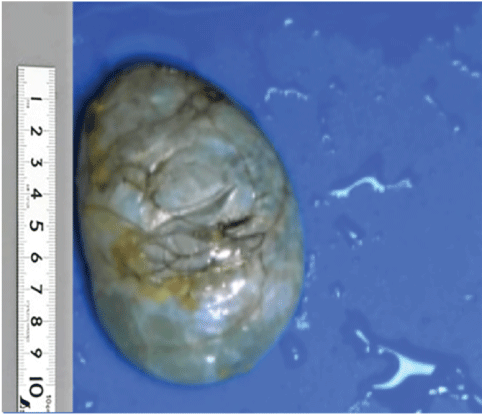
Figure 4: The excised specimens were found to be unilateral cysts, mostly fibrous cystic lesions, with little calcification on the cyst wall, smooth inner and outer walls, and clear and transparent liquid inside.
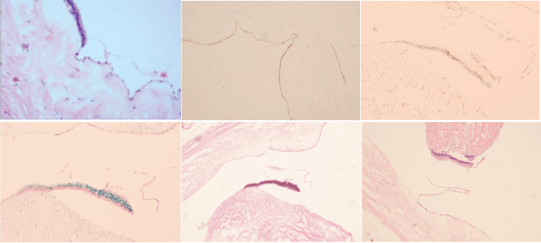
Figure 5: The tumor cyst wall is composed of single cuboidal and flat glandular epithelial cells. Immuno histochemical examination revealed CDK7 (+), ER (+), AB (Alcian Blue) (+) and PAS (+).
Pathologists in Peking University-Hong Kong University of Science and Technology Medical Center Biocell Research Laboratory suspected that the tumor was a PRMC.
After informing the patient and her families of the surgical plan and risks, we recommended expanding the scope of tumor resection or adjuvant treatment.
The patient did not complain of obvious discomfort 1 week after the operation, and the symptoms of abdominal pain and intestinal obstruction disappeared. She refused further treatment but agreed to return to our hospital for review 3 months after the operation, and the patient’s last abdominal CT examinations did not show any signs of recurrence or other complications.
The early diagnosis and treatment of primary retroperitoneal mucinous cystadenoma present great challenges to surgical doctors, and Imaging examinations are difficult to diagnose and differentiate. We need to differentiate PRMCs from mesangial lymphatic cysts, cystic teratomas and retroperitoneal neurogenic tumors [3-5]. Laparoscopy is used frequently and has shown great clinical value in the treatment of PRMC, and we found that laparoscopic resection of retroperitoneal cystadenoma is a very good minimally invasive surgical method, and there are patients [6-9] with small incision, less trauma, better postoperative prognosis. There are several reports on the use of laparoscopy for PRMC resection, but there are more reports on the transabdominal approach and less on the retroperitoneal approach [10]. In the open resection approach, and surgeons have a greater operating space, the intestine and peritoneal tissue need to be separated, and the operation time will be extended [11]. Although laparoscopy does not require separation of too much tissue and the greatly shortened operation time, but the disadvantage is that the operation space is only the retroperitoneal space, and the tumor cyst wall is easily broken when the tumor is removed, causing the contents of the cyst to disseminate into the peritoneal cavity [12]. Therefore, this type of posterior peritoneal surgery has a higher risk and higher surgical requirements for surgical doctors. However, regardless of which surgical method is used, the use of laparoscopy for PRMC resection is currently the most effective treatment [13,14]. In short, when patients with suspected PRMC lesions are identified and there are no related contraindications, laparoscopic abdominal mass resection is the first choice for the treatment of PRMC.
In our study, we reviewed 14 literatures on surgical treatment of PRMC, and summarized the clinical characteristics, pathological and imaging manifestations, potential malignant tendency of tumors, and surgical mode selection of PRMC (Table 1).
| Study | Years of reports | Gender | Age | Area | Symptom | Size(mm) | Treatment |
| Koyama R, et al. [15] | 2019 | Female | 39 | Japan | Tension and pain in the left flank | 20 | Laparotomy |
| Pesapane F, et al. [16] | 2018 | Female | 52 | Italy | Abdominal pain and a palpable mass | 121 × 81 | Laparotomy |
| Tokai H, et al. [14] | 2017 | Female | 29 | Japan | Abdominal pain and a cystic mass | 85 × 80 | Laparotomy |
| Zanoni D, et al. [17] | 2015 | Female | N/A | Italy | Abdominal mass | N/A | Radiotherapy and chemotherapy |
| Dong A, et al. [18] | 2015 | Female | 52 | China | N/A | 38 × 34 | N/A |
| Hanlian HM, et al. [19] | 2014 | Pregnant Female | 37 | Turkey | Cystic mass | 220 × 130 × 110 | Laparotomy |
| Kurita T, et al. [20] | 2014 | Female | 30 | Japan | Abdominal tumor | N/A | Laparoscopic surgery and chemotherapy |
| Feng JF, et al. [21] | 2013 | Male | 63 | China | Clironic lower back pain | 40 × 30 × 40 | Laparotomy |
| Sliiau JP, et al. [22] | 2013 | Male | 59 | Taiwan | A left retroperitoneal cystic mass | 75 × 30 × 70 | Laparotomy |
| Demirel D, et al. [23] | 2013 | Female | 34 | Turkey | Retroperitoneal cystic mass | 140 × 10 × 80 | Laparotomy |
| Kanayama T, et al. [24] | 2012 | Female | 40 | Japan | A progressive abdominal distension | 250 | Open surgery |
| Fiijita N, et al. [25] | 2012 | Male | 71 | Japan | Abdominal tumor | 100 | Open surgery |
| Kasliima K, et al. [26] | 2008 | Female | 28 | Japan | Abdominal tumor | 170 | Laparotomy |
| Thamboo TP, et al. [27] | 2006 | Male | 64 | Singapore | A large retroperitoneal cystic tumor | 240 × 200 × 160 | Open surgery |
| Carabias E, et al. [28] | 1995 | Female | 43 | Spain | A palpable right-sided abdominal mass | 150 | N/A |
Table 1: Cases of primary retroperitoneal mucinous cystadenoma reported in the literature [14-28].
N/A: Not Applicable
Our study reviewed the literature for nearly 20 years and found that cases of PRMC were mostly reported in women, but rarely in men. Feng JF, et al. [21], Shiau JP, et al. [22] and Thamboo TP, et al. [18] reported cases of male PRMC. Afzal Z, et al. [25] once counted 50 female patients with PRMC, most of them were young women and middle-aged women (90% ± 1%), and the age was mainly (33.5 ± 5.0). However, we found that male patients were mostly elderly, and the age was mainly (62.0 ± 2.0). We can’t help but wonder if there is the difference of gender and age in the incidence of PRMC [15].
Hanhan HM, et al. [16] reported cases of PRMC in pregnant female, which is extremely rare. At present, no more than 10 cases have been reported in the world [3,17]. Hanhan HM, et al. also found that pregnant women of tumor size: 220mm × 130mm × 110mm, and they planned to perform laparoscopic surgery to remove the PRMC in order to minimize the harm of the pregnant woman. This minimally invasive surgical approach has obvious advantages in the treatment of cystadenomas [19-23].
With the development of medical equipment technology, more and more laparoscopy techniques are used in surgical operation. At present, laparoscopic resection is the main treatment in the surgical treatment of PRMC. However, Kanayama T, et al. [24] adopted Open surgery in consideration of the tumor size ≥ 250mm, and Thamboo TP, et al. [18] and Fujita N, et al. [27] changed the surgical method from laparoscopic surgery to open surgery due to the malignant transformation of the tumor in the PRMC patients.
Yanwei Lai designed the research; Xiaoqiang Li performed the research; Jian Li contributed to pathologic diagnosis; Liusheng Wu wrote the paper.
The authors declare that they have no conflict of interest.
This work was supported by grants from the National Natural Science Foundation of China (81972829), the Science and Technology Innovation Committee of Shenzhen Municipality (Grant No. JCYJ20180228162607111, JCYJ20190809104601662), the Health and Family Planning Commission of Shenzhen Municipality Research Project (Grant No. SZBC2018018), China Scholarship Council (CSC, 201908440124).
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: Wu L, Li X, Li J, Lai Y (2021) Laparoscopic Resection of a Giant Dedifferentiated Primary Retroperitoneal Mucinous Cystadenoma (PRMC) in a Young Woman: A Case Report and Literature Review. J Clin Case Stu 6(1): dx.doi.org/10.16966/2471-4925.215
Copyright: © 2021 Wu L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access