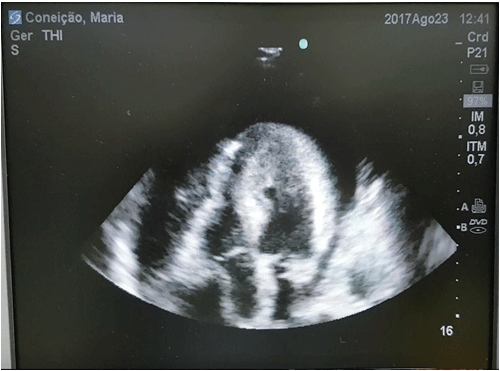
Figure 1: A large pericardial effusion with tamponade signs-Right atrial and ventricular diastolic collapse.


Emídio Lima*
Roberto Santos General Hospital, Emergency Department, Salvador, Brazil*Corresponding author: Emídio Lima, Roberto Santos General Hospital, Emergency Department, Salvador, Brazil, E-mail: emidio.lima@gmail.com
Cardiac tamponade diagnosis sometimes requires high index of clinical suspicion. It is an emergency situation whose rapid diagnosis and treatment, drainage of the pericardial effusion, can be life saving. I describe a case of cardiac tamponade whose initial diagnosis was pulmonary embolism in a 72-year-old female brought to our Hospital with shortness of breath over the last three weeks.
Cardiac tamponade; Pericardial effusion; Pericarditis; Dyspnea
Cardiac tamponade diagnosis sometimes requires high index of clinical suspicion. The three classical signs of cardiac tamponade (Beck’s triad), hypotension, jugular venous distention, and muffled heart sounds can be absent in 14% of the cases [1]. Others manifestations of hemodynamic instability such as pulmonary edema or angina may occur without hypotension [2]. Patients with severe hypovolemia and cardiac tamponade have hypotension without jugular venous distention [1].
Cardiac effusion and occasionally tamponade can complicate a broad range of conditions such as malignant disease in terminal phase, myocardial infarction, renal failure with uremia, connective tissue disorder, drug-related lupus, cardiovascular surgery or coronary intervention, thoracic trauma, pacemaker lead implantation, central venous catheter insertion, HIV, and tuberculosis [3].
Cardiac tamponade is an emergency situation requiring fast diagnosis and drainage of the pericardial effusion (pericardiocentesis or pericardial window). I describe a case of cardiac tamponade whose initial diagnosis was pulmonary embolism in a 72-year-old female brought to our Hospital with shortness of breath over the last three weeks.
A 72-year-old black female was brought to our emergency department with dyspnea. On admission, she complained of shortness of breath (SOB) over the past three weeks without others symptoms. The past medical history includes colon cancer, which was treated with uneventful colostomy. The patient had no co morbidities. Upon physical examination she had dyspnea, respiratory rate of 30 rpm, blood pressure of 100/70 mm Hg, a heart rate of 110 bpm and, jugular vein distention (JVD); she was under distress, pale and, with edema in both legs. On auscultation normal heart and pulmonary sounds; on abdominal examination there were no signs of peritoneal irritation. Laboratory workup: hemoglobin 11 g/dl, total leukocytes 12.00 × 109 /L (neutrophils 7.5 × 109 /L, lymphocytes 2.0 × 109 /L, monocytes 0.2 × 109 /L, eosinophils 0.04 × 109 /L), normal urinalysis (absent proteinuria, cellular casts or hemoglobin), urea 1.8 mmol/L, creatinine 60 µmol/L. Auto immune workup: C-reactive protein 4.0 mg/L and, absent antinuclear and antiphospholipid antibodies.
A chest CT scan showed sub segmental bilateral pulmonary embolism. Anticoagulation with Enoxaparin was initiated. The patient became progressively dyspnea even after being anticoagulated for 24 hours.
An echocardiogram showed a large pericardial effusion with tamponade signs (Figures 1,2) and lung ultrasound demonstrated bilateral B line pattern compatible with pulmonary edema. A bedside, subcostal pericardiocentesis, under local anesthesia, was made and approximately 300 ml of citrine fluid was evacuated. The patient, immediately after the pericardiocentesis, underwent a cardiac arrest with pulse less electrical activity. Basic and advanced life supports were undertaken, such as chest compression, ventilation, tracheal intubation and vasopressor. The return of spontaneous circulation occurred after 25 minutes of resuscitation and the patient, neurologically intact, was maintained under mechanical ventilation support and sedation. The day after resuscitation the patient presented with pneumonia, characterized by purulent tracheal secretions and a new pulmonary consolidation, observed in lung ultrasound. Antibiotics were started and 72 hr after a tracheostomy was made, because increased tracheal secretions and ineffective cough. The follow up was uneventfully, weaning from mechanical ventilation 24 h after tracheostomy, decannulation and discharge from the hospital took place after seven day of antibiotic therapy. An echocardiogram at the discharge showed a pericardial effusion without tamponade signs. A pericardial fluid sample sent for cytology review was negative for bacteria, fungus, virus, or malignancy. A pericardium biopsy analyzed by pathology ruled out malignancy. The patient in thirty days follow up, postdischarge, had no complains and an echocardiogram didn’t show pericardial effusion.

Figure 1: A large pericardial effusion with tamponade signs-Right atrial and ventricular diastolic collapse.
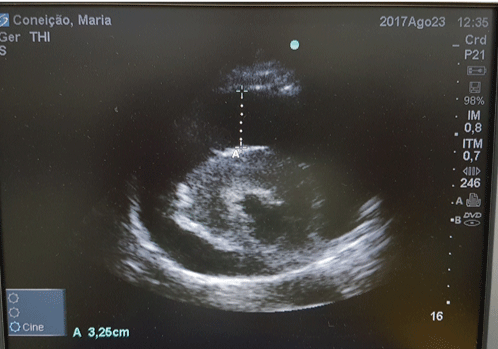
Figure 2: A large pericardial effusion (300 ml) in parasternal short axis window.
Cardiac tamponade diagnosis in non-traumatic diseases may be a great challenge for clinicians at the Emergency department. Dyspnea, hypoxemia, chest pain and hypotension, symptoms present in cardiac tamponade, are frequently observed in different critical conditions such as: pulmonary edema, pulmonary embolism, myocardial infarction and pneumonia [2,4]. The most common sign of cardiac tamponade is dyspnea (78% of cases) [2] and the most frequent presentation is dyspnea, tachycardia and elevated venous jugular pressure [3]. Our patient had dyspnea and, on CT, the sub segmental bilateral pulmonary embolism diagnosis established and she was initially treated for that pathology. The patient’s condition (dyspnea and hypoxia) deteriorated, although 24 h of anticoagulation and an echocardiogram was made disclosing an unsuspected cardiac tamponade. Echocardiography is a non-invasive method, with high accuracy for cardiac tamponade diagnosis and can be made at bedside, avoiding the risks of patient’s transference to imaging department. An echocardiogram is useful for excluding differential diagnoses such as cardiomyopathy, constrictive pericarditis, and myocardial infarction in those patients with arterial hypotension and venous hypertension [5]. The diagnosis of cardiac tamponade by echocardiography is confirmed when a pericardial effusion with right atrial and right ventricular diastolic collapse are present [3,4]. The four most frequent etiologies of cardiac tamponade are: cancer (30-60%), uremia (10-15%), idiopathic pericarditis (5-15%) and infectious disease (5-10%) [3] (Table 1). In our case the cytology review of the pericardial fluid was negative for bacteria, fungus, virus, or malignancy and a pericardium biopsy ruled out malignancy. I believe, according to cytology result (sensitivity 75%) [6-8] and the uneventful patient’s outcome, that the idiopathic pericarditis was the cause of the pericardial effusion.
| Etiology | Incidence rates (%) |
| Malignant diseases | 30 - 60 |
| Uremia | 10 - 15 |
| Idiopathic pericarditis | 5 - 15 |
| Infectious diseases | 5 - 10 |
| Anticoagulation | 5 - 10 |
| Connective tissue diseases | 2 - 6 |
| Dressler or postpericardiotomy syndrome | 1 - 2 |
Table 1: Etiologies of pericardial tamponade.
In conclusion, considering the necessity of emergency treatment and the effective result with pericardial effusion drainage, cardiac tamponade must be suspected in all cases of acute dyspnea. In those cases is echocardiogram the method of choice for the diagnosis or exclusion of cardiac tamponade. Echocardiogram is also important for guiding safety pericardial effusion drainage.
Download Provisional PDF Here
Article Type: CASE REPORT
Citation: Lima E (2018) Cardiac Tamponade as Cause of Respiratory Distress and Cardiac Arrest. J Clin Case Stu 3(3): dx.doi. org/10.16966/2471-4925.174
Copyright: © 2018 Lima E. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access