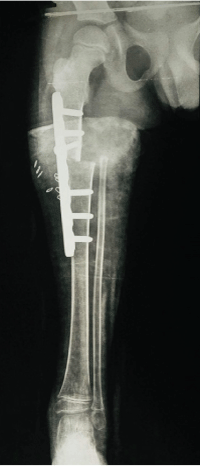
Figure 1: X-Ray showing image of Rotationplasty


Dildip Khanal1* Janith Lal Singh2
1Bachelor of Physiotherapy (BPTh) Master of Physiotherapy in Neurology (MPTh in Neurology), Department of Physiotherapy, Government of Nepal Ministry of Health National Trauma Center Mahankal, Kathmandu, Nepal*Corresponding author: Dildip Khanal, Bachelor of Physiotherapy (BPTh) Master of Physiotherapy in Neurology (MPTh in Neurology), Government of Nepal Ministry of Health National Trauma Center Mahankal, Kathmandu, Nepal, E-mail: dildip17@gmail.com
The procedure in which the distal leg and foot are rotated axially 180 degrees and grafted to the femur bone so as to create a functional joint replacing the knee joint is known as Van Nes. It has been intermittently performed as an alternative to high above knee amputation in malignant bone tumors of the lower extremity, also can be performed as a function-preserving salvage procedure for adult patients with infected knee prostheses. This chapter discusses Van Nes as one of rare surgery performed in orthopedic cases in context to Nepal.
Van Nes; Rotationplasty; Tumor; Amputation; Rehabilitation
Borggreve was the first person to introduce Rotationplasty in a patient with femoral deficiency in 1930. Then the procedure was popularized for the management of proximal femoral focal deficiency by Van Nes, whose name has become the synonyms with the procedure [1-3]. In 1981 Salzer, et al [4] first reported a reconstruction for bone deficits associated with oncologic resection using rotationplasty.
Rotationplasty have been reported to achieve superior functional outcomes in several studies compared with endoprosthesis, allografts and amputations. Regardless of this, it is rarely performed owing to concerns with the psychological effect of the abnormal cosmetic appearance of the limb [5-8].
7 years old boy was referred to Bhaktapur Cancer Hospital with the diagnosis of Ewing Sarcoma of the right femur in 2015 AD. Tumor was the size of a cricket ball which was growing rapidly. He was put on a temporary back-slab plaster as the bone looked fragile in X-rays and was advised not to bear any weight on the affected leg. Chemotherapy was started promptly with the aim of limb salvage surgery. As the days passed by, his tumor regressed in size which was very encouraging for a team and he got discharged.
When the earthquake struck on April 25th 2015, he was inside his house having a lunch. While fleeing for his life he sustained pathological fracture of his femur bone right through the cancer weakened site. After many weeks of sleeping in the open space they finally made it to hospital. While examining him, we found fracture hematoma had escaped into the back of his knee joint and had contaminated vessels and tissues. In this situation limb salvage surgery was not possible. So, the ‘practical options’ for him was a very high above knee amputation that would create a short ineffective stump or a hip disarticulation. In either situation, he would be expected to fare badly as the prosthesis is usually cumbersome and not ideal for the Nepalese terrain. Then the other possible option was what we called a ‘Rotationplasty’.
After a lot of discussion that included motivational videos of other patients in western countries who had undergone the same procedure, his parents were willing to go ahead with Rotationplasty (Figure 1). Given the stigma of having a deformed looking foot with certain religious repercussions, the decision to go ahead on their part was very courageous step. It was the first operation of Rotationplasty performed in context to Nepal.

Figure 1: X-Ray showing image of Rotationplasty
33 years old male patient came to the National Trauma Center, Mahankal, Kathmandu with the history of pain and inability to move the left knee joint since one and half month back.
3 years back he felt pain on his left knee while squatting followed by difficulty in bending knee. He consulted to local doctor who gave medication for the same. His pain was reduced little bit but as such no functional improvement was found on his condition. Then he sustained pathological fracture of the left distal femur for which he was referred from local level hospital to National Trauma Center for the further management. He underwent tibial turn-up plasty and knee arthrodesis (Figure 2). Unfortunately he developed recurrence of the disease in the form of multiple non-contiguous soft tissue deposits as well as recurrence in the left proximal tibia after 1 year of surgery. Even the lack of options, he was given a choice of either a high transfemoral amputation or a rotationplasty which would technically function as a below knee amputation. After much discussion and counseling he chose latter. Initially the patient refused to perform the surgery because of abnormal cosmetic appearance of the limb; later with the counseling and motivational videos of similar conditions he agreed to perform the Rotationplasty surgery (Figure 3). It was the second operation of Rotationplasty performed in context to Nepal.
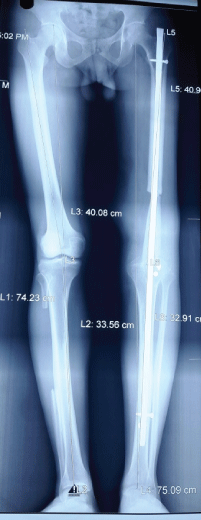
Figure 2: X-Ray image of tibial turn-up plasty and knee arthrodesis
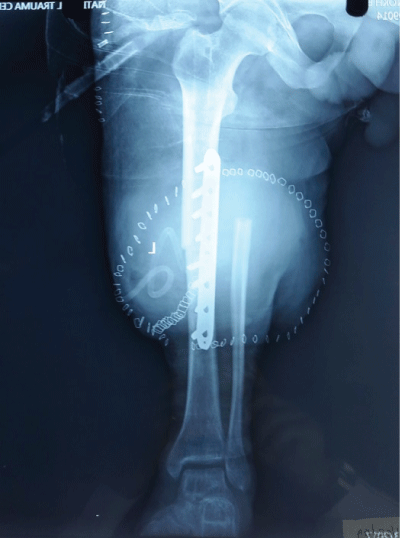
Figure 3: X-Ray showing rotationplasty of the left leg
Histopathology: Report shows features are compatible with giant cell tumor.
MRI Impression: Ill-defined eccentric heterogeneous lesion in distal femur involving meta epiphysis reaching up to the articular surface predominantly involving the medullary cavity with extension and destruction as described above with minimal joint effusion and enlarged popliteal lymph nodes-likely malignant Giant Cell Tumor. Non enhancing filling defect in distal femoral artery above the knee joint which is extending up to the proximal popliteal artery-likely thrombus. Ill-defined non-enhancing hyperintense track in medial aspect of distal thigh involving the skin, subcutaneous tissue and muscle plane reaching up to the lesion (Figures 4 and 5).
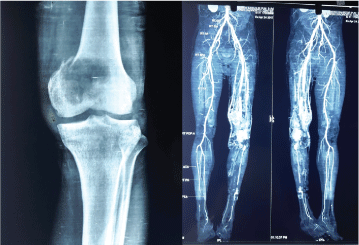
Figure 4 and 5: X-Ray and MRI Contrast Media Images
Rotationplasty that often gets overlooked due to concern about cosmesis is an alternative reconstructive strategy after sarcoma resection. Rotating a distal segment and fixing it to a proximal segment leaves a highly functional and durable reconstruction that functionally compares favorably to other limb salvage techniques [3].
In a study comparing functional outcomes, rotationplasty patients were shown to have higher Musculoskeletal Tumor Society and Toronto Extremity Salvage functional scores than patients with alternative limb sparing procedures or amputations [5]. Most encouragingly in a study, 85% who had undergone rotationplasty for a lower extremity sarcomere were actively participating in high level sports [9].
A critical issue noted after rotationplasty is psychosocial well-being as the appearance of the limb is unusual. In a study conducted by Veenstra, et al [10] used the SF-36, Social Support List, and European Organization for Research and Treatment of Cancer to create a questionnaire and they found that psychosocial functioning, general quality of life, and social support were comparable to healthy peers. Although almost half of the patients reported negative effects of the surgery on initiating social or intimate contact, body image, and sexuality, 64% of the patients had been sexually active in the month before the surgery.
Rehabilitation following limb sparing procedures such as rotationplasty or amputations focuses on retraining muscles, increasing strength and endurance, balance and range of motion as well as helping the patient return to school or work activities thus improving the quality of life of patients [11]. For this physiotherapist plays a crucial role.
Paralleled with endoprosthesis, allografts, and amputations, rotationplasty patients have been reported to achieve superior functional outcomes in several studies. Despite this, rotationplasty is rarely performed owing to concerns with the psychological effect of the abnormal cosmetic appearance of the limb and it was second operation of rotationplasty in context to Nepal.
Download Provisional PDF Here
Article Type: Case Series
Citation: Khanal D, Singh JL (2017) Van Nes: One of Rare Surgery Executed in Context to Nepal. J Clin Case Stu 3(1): doi http://dx.doi.org/10.16966/2471-4925.162
Copyright: © 2017 Khanal D, et al. This is an openaccess article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access