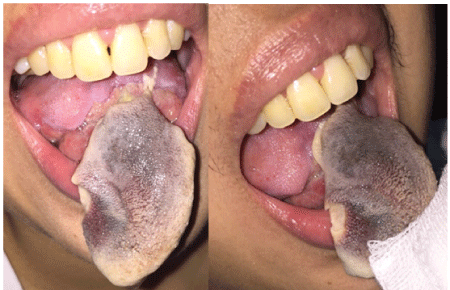
Figure 1: pre-operative photograph showing self-amputation of the tongue


Adel Alenazi*
Department of Oral and Maxillofacial Surgery and Diagnostic Science, Prince Sattam University, Al Kharj, Saudi Arabia*Corresponding author: Adel Alenazi, Department of Oral and Maxillofacial Surgery and Diagnostic Science, Prince Sattam University, P.O. Box 173, Prince Sattam Street, Al Kharj 16278, Saudi Arabia, Tel: 00966115886200; E-mail: a.alenazi@psau.edu.sa
Vasculitis is a condition that can affect any organ of the body and is caused by an inflammation of the walls of large and small blood vessels of the body. It has a complex classification and is idiopathic in nature or occurs secondary to systemic disorders. Extensive history taking is key to diagnosis of this condition as it helps the clinician establish whether the vasculitis is idiopathic or secondary in nature. ESR is considered the gold standard lab investigation along with CRP, liver function tests and definitive diagnosis is established by tissue biopsy and angiogram where required.
This report describes a case of vasculitis of the tongue. The patient had existing vasculitis of the toes and was referred from general surgery department to examine and manage tongue necrosis which led to the partial self-amputation of the tongue. Surgical debridement of the necrotic tissue was carried out under local anesthesia while aspirin and systemic corticosteroids prescribed by the general surgeon led to a reduction of toe discoloration.
Necrosis of the tongue is a rare occurrence due to high vascularity of the organ. Oral health practitioners must be aware of this condition so that they are able to recognize and consider giant cell arteritis or temporal arteritis as a differential diagnosis of any ischemic or necrotic changes that appear in the tongue.
Vasculitis; Necrosis; Tongue; Inflammation; Arteries
Vasculitis is a disease which is considered to have a simple definition but complex classification, pathogenesis, and prognosis. It refers to a heterogeneous group of disorders characterized by inflammation of vessel walls which leads to their weakening, obstructs the vascular lumen and their subsequent necrosis and oedema [1]. Although it can affect any blood vessel present in the human body, it is known to affect arteries more than veins. Histological examination of the necrotic site usually displays an infiltration of inflammatory cells while histopathologically there exist patterns of necrotizing vasculitis, granulomatous disease, giant cells and immune complex deposition [2]. It usually involves multiple organs in the body but single organ involvement is also observed. The disease has a sudden onset, has varied presentations and very diverse sites of occurrence which makes it difficult to diagnose and treat [3,4].
The classification of vasculitis is not straightforward. It can be primary which is idiopathic in nature or secondary to infectious and inflammatory connective tissue diseases. Due to the difficulty in classifying vasculitis, the international chapel hill consensus conference (CHCC) 2012 publish a nomenclature system to simplify the communications between the specialists (Table 1) [5]. Each form of vasculitis presents with its unique clinical manifestations and histopathologic findings. Diagnosis is made by recording extensive history, clinical examination, preliminary screening tests which include ESR, CRP, liver function tests etc. and finally angiography and tissue biopsy to detect and define the nature of the vasculitis process [6]. This report describes a case of tongue vasculitis and its management.
| Large vessel vasculitis (LVV) |
|
| Medium Vessel Arteritis |
|
| Small vessel Arteritis | Antineutrophil cytoplasmic antibody(ANCA)- associated vasculitis (AAV)
|
| Variable vessel vasculitis (VVV) |
|
| Single-organ vasculitis (SOV) |
|
| Vasculitis associated with systemic disease |
|
| Vasculitis associated with probable etiology |
|
Table 1: Names for vasculitides adopted by the 2012 International Chapel Hill Consensus Conference on the Nomenclature of Vasculitides [10]
A 33-year-old female patient. She was not known to have any chronic medical illness with a negative history of pregnancy, abortion, vasculitis or malignancy. she was referred to the department of oral and maxillofacial surgery from general surgery to evaluate the oral presentation of an already diagnosed vasculitis of the lower limb (toes).The sudden lower limb discoloration was seen 8 days before the referral to the oral surgeon. Angiogram to the lower limb showed severe narrowing of the lateral plantar artery. The patient presented to the oral surgeon with difficulty in tongue movements, speech, and discoloration of the anterior third of the tongue. Oral examination revealed a grayish black discoloration and partial self-amputation of the anterior part of the tongue (Figure 1). Mouth opening was normal and other oral tissues appeared to be normal. On the basis of clinical presentation and existing diagnosis from the general surgery department, a diagnosis of vasculitis of the tongue was made.

Figure 1: pre-operative photograph showing self-amputation of the tongue
The patient was already prescribed aspirin 325 mg and corticosteroids (prednisone 80 mg) daily by the consulting general surgeon. It allowed recovery of blood supply and color of the tissues. Surgical debridement of the necrotic tissue was carried out under local anesthesia and the necrotic tissue was sent for histopathologic examination (Figure 2). The result of the histopathology exam came with a necrotic tissue with inflammatory infiltrates. Clinical evaluation of tongue functional ability did not mandate reconstruction procedure as the remaining tongue size was adequate to maintain function. An oral care regimen was established for the patient by prescribing 0.2% chlorhexidine gluconate three to four times daily. Follow-up visits were divided to one week, 4 weeks, 12 weeks and 6 months post-operative check-up. Follow-up visits focused on assessment of tongue function, swallowing ability and healing of the debrided area. Good healing with normal colored tissues, efficient swallowing, and good tongue movement was observed.
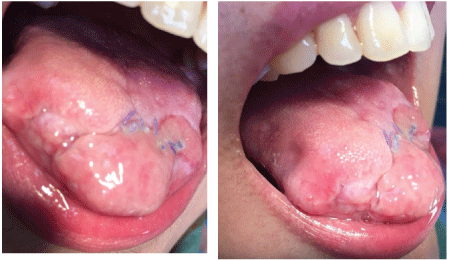
Figure 2: post operative photograph
Tongue necrosis is a very rare occurrence due to high vascularity of the organ and may be caused by a plethora of other reasons like the use of vasoconstrictors, radiation therapy and cancer (Table 2) [7]. Impairment of venous drainage of the tongue or ischemic occlusion of the arteries can result in circulatory disturbances in the tongue [8]. In this case, the diagnosis of the lower limb vasculitis and the negative history of radiation, chemotherapy, vasoconstrictor medications intake and cardiac arrest exclude the possible other causes of tongue necrosis. No systemic or local signs of malignancy were seen and the microscopic examination of the debride tissues didn’t show any dysplastic changes at the periphery of the necrotic tissue.As discussed earlier by Sharma et al. [3] diagnosis of vasculitis begins with a thorough history taking in order to determine an underlying cause and ascertain in the diagnosis whether the vasculitis is primary or secondary to any other systemic condition or drug use. In the present case, no underlying systemic cause was detected and the vasculitis was of idiopathic origin i.e. primary vasculitis.There are various cases in the literature which report tongue necrosis due to different forms of vasculitic conditions. Zaragoza et.al reported lingual necrosis as a result of giant cell arteritis in a 68-year-old female patient [6]. In this case, similar to our present case, necrosis was severe which eventually led to self-amputation of the tongue. No surgery was required in that case. Ekman-Joelsson et al. [9] reported another case of a 7-year-old boy with generalized vasculitis with symptoms of polyarteritis nodosa and streptococcal infection leading to tongue necrosis. In this case, the anterior one-third of the tongue had to be extirpated. Another 68-year-old woman who presented with anterior tongue necrosis was diagnosed with temporal arteritis [10].
| Differential Diagnosis of lingual necrosis | |
| 1 | Malignancy (carcinoma, lymphoma, sarcoma) |
| 2 | Vasoconstrictor drugs (vasopressin, ergotamine), chemotherapy |
| 3 | Radiation therapy |
| 4 | Cardiovascular – haemorrhage, embolism, cardiac arrest |
| 5 | Infection (tuberculosis, syphilis) |
| 6 | Systemic vasculitis (ACNA positive vasculitis, giant cell arteritis) |
Table 2: Differential Diagnosis of Lingual Necrosis (adapted from Zaragoza et.al) [6]
When a patient presents with signs and symptoms of atypical vasculitis, the first course of action is to initiate corticosteroids in order to reduce the inflammatory process within the affected organ. Investigations are simultaneously carried to rule out other causes. Angiogram and biopsy of the artery in the affected area or of the affected tissue are used to confirm the diagnosis. No angiogram was conducted for the head and neck area due to the clear diagnosis of this case as discussed earlier. The distal part of the deep lingual artery is the expected inflamed and narrowed part of the lingual blood supply. It was clear that the middle and posterior parts of the tongue were normal in color and function without changes due to the sufficient blood supply
Necrosis secondary to vasculitis can affect even the most highly vascularized organs within the body such as the tongue. Early detection of vasculitis in any portion of the oral cavity is critical to avoid radical resection of tissues. The oral health practitioners should be vigilant in identifying signs and symptoms of all forms of vasculitis which have oral manifestations in order to be able to efficiently diagnose this condition and may sometimes be the first line of healthcare practitioners to identify this disease. It is important to have temporal arteritis or giant cell arteritis as a differential diagnosis if a patient presents with any evidence of tongue ischemia and necrosis.
Download Provisional PDF Here
Article Type: Case Report
Citation: Alenazi A (2017) Primary Vasculitis of the Tongue - A Case Report. J Clin Case Stu 2(5): doi http://dx.doi.org/10.16966/2471-4925.151
Copyright: © 2017 Alenazi A. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access