
Figure 1: 50 Y Woman CT Scan: Coffee Bean Sign


Danilo Coco1* Silvana Leanza2
1Madre Teresa of Calcutta Hospital, Schiavonia, Padova, Italy*Corresponding author: Danilo Coco MD, Madre Teresa of Calcutta Hospital, Schiavonia, Padova, Italy, E-mail: webcostruction@msn.com
Caecum volvulus (CV) is defined as an axial twisting that causes an inversion position of the caecum, ascending colon and terminal ileum. These anatomical findings are responsible for some clinical features. Obstruction and strangulation are the most important and life-threatening. We present the case of 50 years old woman with sudden acute severe abdominal pain and distension of about 24 hours.
Caecum volvulus, Acute severe abdominal pain
Caecum volvulus is considered as the torsion of the caecum around its own mesentery [1]. The incidence of CV account 1%-1.5% of intestinal obstruction with female predominance and account 25% of colonic volvulus with highly variable age presentation between 30 years to 60 years making it a difficult pathology to identify [1,2]. That causes strange diagnosis and delay decision making [3].
A 50 years old woman presented to the hospital with sudden acute severe abdominal pain and distension of about 24 hours associated with vomiting and no flatus. In her clinical history, she has had a hysterectomy for myomatosis. She denied other medical problems. On physical examination, we found altered vital signs and hemodynamic instability. Abdominal examination noticed diffuse abdominal distension, tympanic sound, and positive Blumberg sign. Laboratory studies showed WBC 20 cell/mm3 and elevated PCR. Rx abdomen showed intestinal distension suggestive of Sigma volvulus. In the scout, CT scan showed coffee bean sign (Figure 1), bird beak sign (Figure 2) and whirl sign (Figure 3). So we performed an urgent colonoscopy to view mucosa and to possible sigma volvulus untwisting. Colonoscopy showed normal mucosa and no sigma volvulus. The patient was under went an urgent laparotomy with findings at the operation showing axial rotation of the caecum and terminal ileum with ischemia extended from the terminal ileum to right colon flexure (Figure 4). We performed a classical right colectomy with ileocecal mechanic side to side anastomosis for good patient status. The patient was discharged in seven postoperative days with no medical problems.

Figure 1: 50 Y Woman CT Scan: Coffee Bean Sign
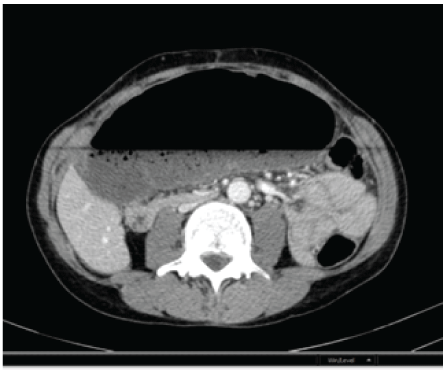
Figure 2: 50 Y Woman TC Scan: Bird Beak Sign

Figure 3: 50 Y Woman Ct Scan: Whirl Sign
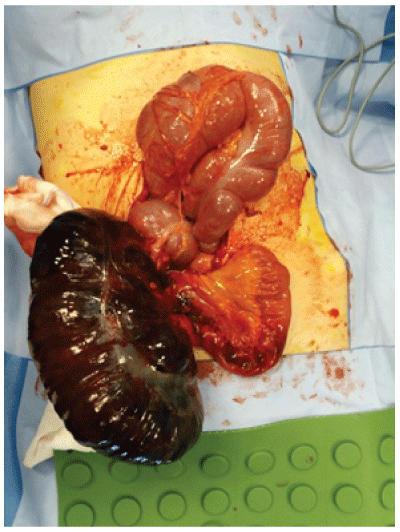
Figure 4: 50 y old woman: caecum volvulus
Caecum volvulus is a clear result of incomplete intestinal rotation during embryogenesis featured by an inadequate right colon fixation to retroperitoneal structures during the final clockwise step of colon embryogenesis [1]. Parietocolic ligaments laxity is a main cause of improve caecum motility up and down or right and left and axial rotation. Clinical reports suggest that 40% of caecum strangulation is found in patients with prior abdominal and pelvic surgery. Prior surgery causes adhesions and a new fulcrum of rotation [1]. Laxity of ligaments associated with pelvic surgery are the most important etiologies [3,4].
The most urgent clinical features are acute obstruction and strangulation associated with sharp pain, no flatus, vomiting, abdominal distension. Differential diagnosis with left colon obstruction, small bowel obstruction, mesenteric ischemia, aortic aneurism, acute pancreatitis makes the diagnosis difficult. Untreated CV may progress in strangulation, ischemia, and perforation with peritoneal irritation and hemodynamic instability presentation [3].
It is recommended that these patients must undergo early laboratory and radiological evaluations. Laboratory findings are nonspecific. Advanced obstruction may show high WBC, high PCR, and fluid or electrolytes changes. Abdominal X-ray shows intestinal dilatation in 100% of cases but, for the rarity of this pathology, many of patients are erroneously given the diagnosis of small bowel obstruction or sigma volvulus [5]. CT scan has 80%-90% sensibility/specificity. There are three clinical findings: “Coffee bean”, “bird beak” and “whirl” signs. Coffee bean sign demonstrates an axial view of dilated cecum with air. The loop may resemble a coffee bean, which has an appearance similar to that of the well-known radiographic sign of sigmoid volvulus (Figure 1) [6]. Bird beaks sign shows bowel loops (Figure 2). Whirl sign shows fat attenuation of a soft tissue mass (Figure 3) [7]. Colonoscopy may exclude sigma volvulus [8]. Barium enema CT may confirm the colon site of occlusion with 88% of accuracy [2,3]. Advances in knowledge show: two defined transition points are seen in the minority of cases of caecum volvulus; a single transition point is more sensitive for caecum volvulus. CT findings of a whirl, ileocecal twist, the X-marks-thespot sign and the split-wall sign are specific. The coffee bean sign and a distended cecum directed toward the left upper quadrant on CT images are insensitive but specific. Distal colonic decompression on CT images is relatively sensitive and specific [6,9].
Treatment choice is surgery. The most appropriate strategy depends on patient’s status, the timing of volvulus treatment (early or delayed) and surgical team expertise. The clinical review recommended: manual or laparoscopic untwisting with caecopexy in the viable intestine [2]. Caecostomy in the viable intestine but in low-grade patient status. Laparoscopic or open right colectomy is recommended in no viable ischemic or perforated colon in good performance status patient [2,3,10].
Caecum volvulus is a rare colonic obstruction. Diagnosis is strange for the rarity and nonspecific presentation: acute severe abdominal pain is the main clinical feature associated with abdominal distension. CT scan has more accuracy. Surgical Treatment is the best choice [11] Mortality can be kept near 10%-12% if operative intervention is accomplished before caecum strangulation [12-14].
Download Provisional PDF Here
Article Type: Case Report
Citation: Coco D, Leanza S (2017) Caecum Volvulus: A Rare Diagnosis for Surgeon. Case Report and Key Points Review. J Clin Case Stu 2(4): doi http://dx.doi.org/10.16966/2471-4925.147
Copyright: © 2017 Coco D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access