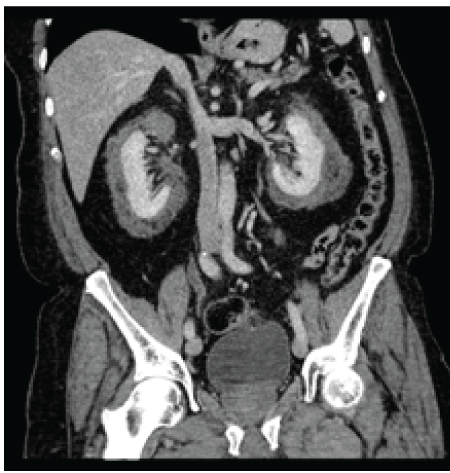
Figure 1: Coronal section of contrast enhanced CT of abdomen and pelvis demonstrating bilateral heterogeneous perinephric soft tissue rind and interspersed pararenal fat


Bruce Gao Emeka Nzekwu Shelley Jane Spaner*
University of Calgary, Canada*Corresponding author: Shelley Jane Spaner, MD, FRCP, University of Calgary, Elbow Drive SW, Calgary, Canada, E-mail: shelley.spaner@gmail.com
Erdheim-Chester disease (ECD) is a rare disease radiologically characterized by bilateral symmetric multifocal long bone osteosclerotic lesions, perinephric soft tissue rinds and smooth pleural thickening. Biopsy typically reveals foamy histiocyte sheets.
With bone pain as the most common presenting symptom, we report an atypical case of a 65-year-old male presenting solely with microscopic hematuria. Contrast enhanced CT demonstrated bilateral perinephric soft-tissue rinds and a left perinephric mass, which post-biopsy, was negative for both lymphoma and renal neoplasm, however, revealed foamy histiocytes. A skeletal survey was performed demonstrating bilateral symmetric long bone lesions with increased metabolic activity on PET CT.
The radiologic and pathological findings were congruent and suggestive of ECD. Given his rather benign presentation, it was elected to conservatively manage and radiologically monitor his condition with annual CTs and skeletal surveys with no significant medical presentation in 4 years of follow-up.
With only several hundred cases reported in the literature, Erdheim Chester is a rare disease. Multi-system involvement results in a nonspecific clinical picture frequently delaying diagnosis. Similarly, our patient underwent multiple biopsies and imaging studies prior to a successful diagnosis. To our knowledge, there are only a few cases of Erdheim-Chester disease presenting with hematuria. This case will provide the reader with a rare presentation of ECD with a review of the clinical and radiological findings.
Following a routine physical a 65-year-old male ex-smoker with medication-controlled hypertension and hypercholesterolemia was found to have microscopic hematuria on urinalysis. He was afebrile with no constitutional symptoms and reported no prior history of abnormalities to his urine, prior trauma, renal calculi, urinary tract symptoms, flank pain or visible blood in the urine.
Physical examination was unremarkable with no abdominal or lower extremity abnormalities such as constovertebral angle tenderness, masses, or edema.
Past medical history included two prior cerebrovascular accidents with medication-controlled hypertension and hypercholesterolemia. No personal or family history of malignancy or other recurring medical conditions. His medications included Aspirin, Crestor and Irbesartan.
A repeat urinalysis indicated persistent microscopic hematuria with the absence of dysmorphic red blood cells, protein and leukocytes. Ultimately presenting with painless hematuria, he was referred to urology for further workup to exclude bladder or kidney cancer.
Cystoscopy demonstrated a normal bladder and urethra. An initial limited ultrasonographic study of the abdomen including his kidney, ureters and bladder revealed suspicious perinephric masses.
Follow-up enhanced computed-tomography (CT) of the abdomen and pelvis demonstrated bilateral heterogeneous perinephric soft tissue rinds with interspersed pararenal fat (Figure 1). No renal calculi or hydronephrosis was identified. No bladder masses or aggressive lytic bone lesions were seen. A well-circumscribed heterogeneously enhancing soft tissue mass immediately anterior to the right piriformis muscle was also noted (Figure 2).

Figure 1: Coronal section of contrast enhanced CT of abdomen and pelvis demonstrating bilateral heterogeneous perinephric soft tissue rind and interspersed pararenal fat
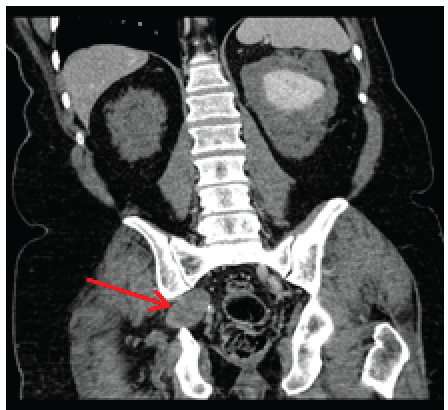
Figure 2: Coronal section of contrast enhanced CT of abdomen and pelvis demonstrating well-circumscribed heterogeneously enhancing soft tissue mass immediately anterior to the right piriformis muscle.
CT guided biopsies of the left perinephric and right piriformis masses were negative for lymphoma or renal neoplasia. The piriformis mass biopsy was non-specific, demonstrating dense fibrosclerotic tissue with organized blood clots negative for amyloid by Congo Red special stain. However, biopsy of the left perinephric mass demonstrated fibromyxoid tissue with multifocal lymphoid aggregates, plasma cells and focal foamy histiocytes concerning for Erdheim-Chester disease (ECD).
PET CT imaging demonstrated increased metabolic activity in the right piriformis mass, perinephric soft tissue and bilateral distal diametaphyseal femurs suggestive of Erdheim-Chester disease (figure 3) with subsequent skeletal survey confirming PET findings demonstrating focal areas of sclerosis in the distal femurs bilaterally, supporting the diagnosis.
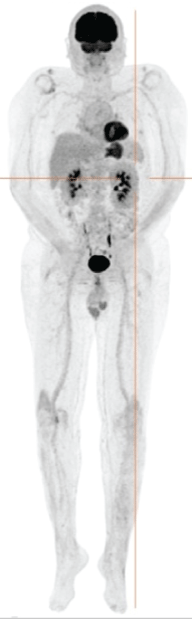
Figure 3: Coronal section of extended PET CT demonstrating low density perinephric soft tissue infiltration and a right piriformis mass with low-grade metabolic activity. Intramedullary calcification in the long bones surrounding the knees also show low-grade metabolic activity. These lesions likely relate to Erdheim-Chester disease.
With the exception of microscopic hematuria, laboratory findings were unremarkable including a complete blood count with differential, liver function tests, creatinine, serum electrolytes, ESR, CRP, urine osmolality and glomerular filtration rate
Given his rather benign presentation, it was elected to conservatively manage and radiologically monitor his condition with annual CTs and skeletal surveys with no significant findings in 4 years of follow-up.
After initial contrast enhanced CT of the abdomen and pelvis:
Lymphoma
Renal Cell Carcinoma
Metastatic Disease
Post-biopsy of left perinephric and right piriformis lesions:
Metastatic disease
Erdheim-Chester disease
Post-PET CT and skeletal survey:
Erdheim-Chester disease
The patient received no medical or surgical treatment for his diagnosis of Erdheim-Chester Disease.
Aside from occasional microscopic hematuria on urinalysis, the patient was otherwise asymptomatic. He was placed on observation with an annual CT survey of the neck, thorax and abdominopelvic region for formation of new masses, growth of the bilateral perirenal soft tissue rinds and enlargement of the mass adjacent to the piriformis muscle. Additionally, an annual skeletal survey for changes in the known sclerotic lesions in the distal femurs was performed. Due to the lack of a clear treatment for Erdheim-Chester disease, it was elected to utilize a conservative observational approach with the alternative of commencing interferon therapy deemed less favourable given the known side-effect profile of this medication.
Including very brief review of similar published cases (how many similar cases have been published?)
Erdheim-Chester Disease (ECD) is a rare form of systemic nonLangerhans cell histiocytosis of unknown etiology with fewer than 500 cases reported in the published literature [1]. The most common clinical presentations are bone pain, neurologic features (most commonly cerebellar and pyramidal syndromes), diabetes insipidus and constitutional symptoms making this gentleman’s presentation of painless microscopic hematuria atypical [1]. Extra-skeletal manifestations are seen in roughly 50% of cases [2]. Rind-like soft-tissue lesions surrounding the ureters and kidneys have potential to cause progressive renal failure secondary to compression of the renal parenchyma [3]. This gentleman had no laboratory features of renal failure or imaging features of hydronephrosis.
The pathogenesis of ECD is not well understood [4]. Pathological demonstration of foamy histiocyte sheets with surrounding fibrosis and interspersed multinucleate and inflammatory cells are diagnostic [5]. Additionally, histiocyte markers CD163, CD68 and Factor XIIIa are expressed in ECD, but not CD1a or S100 frequently seen in Langerhans cell histiocytosis [6]. These markers were not pursued as a part of our pathology workup.
Since there is no known cure for ECD, observation is suggested for asymptomatic patients. Patients with symptomatic ECD are encouraged to enrol in clinical trials or consider therapies such as interferon alpha [7]. There are no clear roles for surgical therapy except for the management of obstructive symptoms secondary to mass-like lesions, commonly seen in ECD. The prognosis for ECD is poor with a 70% overall survival rate of patients treated with interferon alpha therapy [7].
Although our patient’s presentation was highly nonspecific, a rigorous biochemical, pathological, and radiological workup lead to an uncommon diagnosis of ECD which to our knowledge, there are no similar cases with similar findings presenting solely as asymptomatic microscopic hematuria.
Erdheim-Chester disease is a rare pathology characterized by long bone multifocal osteosclerotic lesions with foamy histiocyte sheets on biopsy.
Erdheim-Chester disease can present as a rare differential of Hematuria.
Diagnostic imaging combined with pathology can be useful for diagnosis of the condition and monitoring complications.
Download Provisional PDF Here
Article Type: Case Report
Citation: Gao B, Nzekwu E, Spaner SJ (2017) Microscopic Hematuria as a Rare Presentation of Erdheim-Chester Disease. J Clin Case Stu 2(3): doi http://dx.doi.org/10.16966/2471-4925.145
Copyright: © 2017 Bruce Gao, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access