Abstract
A 37 year old Senegalese male presented with lower back pain and flank pain. The pain was described as sudden in onset and unresponsive to analgesics. Computed tomography (CT) was performed and suggested diskitis osteomyelitis with possible abscess formation. Magnetic resonance imaging (MRI) confirmed these findings. The patient underwent laminectomy and biopsy, which confirmed tuberculosis of the spine (Pott’s disease). The patient was started on a regimen of anti-tuberculosis medications and monitored for improvement of symptoms.
Case Report
A 37 year old Senegalese male presented with lower back and flank pain. The pain was described by the patient as both sharp and dull and sudden in onset starting one month prior to presentation, progressively worsening each day. The pain was not relieved by analgesics. The patient denied significant weight loss, subjective fever, night sweats as well as any other respiratory symptoms. No sensory or motor abnormalities were noted; however patient did report constipation for 3 weeks. The patient was referred for abdominal CT scan without intravenous contrast to evaluate for renal calculi. Significant imaging findings included diskitisosteomyelitis, possible epidural abscess, spinal cord compression, and para-aortic and paracrural lymphadenopathy. No renal calculus or hydroureteronephrosis was seen (Figure1). Shortly thereafter, an MRI of the thoracic spine without and with intravenous contrast was obtained which demonstrated findings consistent with diskitis osteomyelitis and epidural abscess causing severe spinal cord compression and flattening (Figure 2).
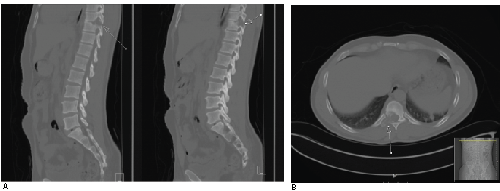
Figure 1: Sagittal (A) Axial (B) CT scan without contrast showing lytic destruction of the posterior superior endplate of the T10 vertebral body with extension to involve the right pedicle, lamina and transverse process. There is narrowing of the T9-T10 disc space and mild destruction of the inferior endplate of the T9 vertebral body. There is an epidural component with mass effect on the spinal cord
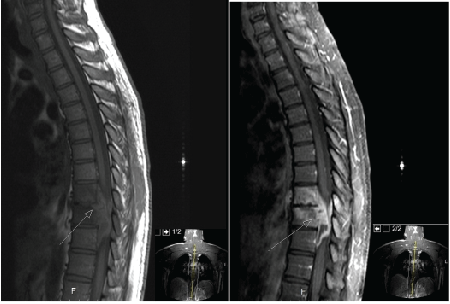
Figure 2: Sagittal of T1 weighted MR pre-contrast (left) and postcontrast (right) images. The post contrast image demonstrate abnormal enhancement with the T9 and T10 vertebral bodies, rim enhancing soft tissue component in the right intervertebral disk with extension into the right pedicle and posterior elements at T10 level
The top differential diagnoses included indolent infection such as tuberculosis versus neoplastic process. Of note, the patient reported HIV positive status with his recent medical records demonstrating a CD4+ counts >200/mm3, and he was treated with highly active antiretroviral therapy (HAART therapy) in the past. On physical examination no spinal tenderness was appreciated.
Thoracic laminectomy from T9 to T11 was performed for decompression, at which time a biopsy of the epidural tissue was obtained. The tissue was sent for pathologic analysis, which showed granulomatous inflammation with caseation necrosis (Figure 3). QuantiFERON test was positive. Of note, acid-fast bacilli (AFB) stain was negative but culture of the lesion tested positive, confirming the diagnosis of tuberculosis (TB). A diagnosis of Pott’s disease with associated abscess was determined. Subsequently, the patient was started on a regimen of rifampin, isoniazid, ethambutol and pyrazinamide for 6 months. The patient recovered well from surgery without any major complications. The patient’s consent for reporting this case was obtained.
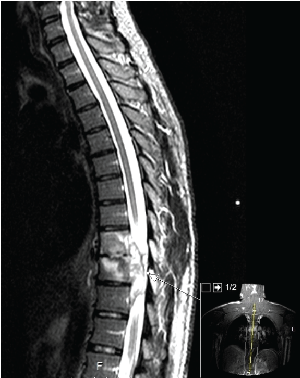
Figure 3: Sagittal STIR MRI demonstrating large rim enhancing epidural abscess from T9 to T11 levels extending into the spinal canal causing severe cord compression and flattening
Discussion
Diskitis osteomyelitis
Diskitis or vertebral osteomyelitis usually arises from hematogenous spread of an infection in children. However, in adults it usually arises as a secondary infection to an open injury to bone and its surrounding soft tissue. Staphylococcus aureus is most commonly implicated in subacute osteomyelitis [1]. The pathophysiology of vertebral osteomyelitis in adults varies from that in children. In children, the bacteria can spread to adjacent vertebrae through persisting vascular channels in the disc space. In adults, however, the disc is avascular and the bacteria invade the end-arterial arcades in the subchondral region near the disc space [2]. Plain radiography, technetium-99 bone scintigraphy and MRI are the most common modalities used in the diagnosis of osteomyelitis [1]. For definitive diagnosis, culture of the lesion must be taken and depending on the organism responsible, antibiotic treatment should be geared toward the isolated organism or organisms.
In 2014, 9.6 million people were diagnosed with tuberculosis worldwide; 1.2 million were human immunodeficiency virus (HIV) positive patients and 1.5 million people died from tuberculosis in that year, according to the World Health Organization (WHO). The vast majority of these cases occurred in Asia with incidence in the Americas comprising 3% of all cases. The incidence of new extra-pulmonary tuberculosis cases in Senegal in 2014 was 212,057 [3]. According to the Center for Disease Control and Prevention the United States has experienced a steady decline in the rate of tuberculosis since the 1950s from a rate of 52.6 in 1953 to a rate of 3.1 in 2014 [4]. The decline in tuberculosis in the United States can largely be attributed to aggressive screening and prophylactic treatments for at risk populations such as health care workers and immunocompromised individuals as well as aggressive multi-drug regimens for those infected with tuberculosis to prevent further spread.
Tuberculosis is largely considered a pulmonary disease with screening tests aimed at analyzing chest x-rays in the high risk population. We tend to not consider extra-pulmonary manifestations of TB as often as other modalities of infectious disease when dealing with non-pulmonary disease. However, in 2006 there were 13,779 cases of reported tuberculosis and 2,889 (21.0%) were extra-pulmonary tuberculosis. Additionally, while there is a decline in tuberculosis overall, proportionally, there has been an increase in extra-pulmonary tuberculosis from 15.7% in 1962 to 21% in 2006 [5].
Osteomyelitis can occur as a complication of tuberculosis. Usually, it is secondary to pulmonary manifestations, but the absence of pulmonary TB does not rule out tuberculous osteomyelitis when a lesion is present and tuberculosis is suspected [6]. Of the cases of tuberculous osteomyelitis, the spine is the most common area affected [7].
Before the advent of anti-tuberculosis medications, this complication was so common and ubiquitous earning it the eponymous entity known as Pott’s disease. Tuberculous osteomyelitis generally begins at the anterior portion of the vertebral body near the end-plate and can extend to adjacent vertebrae, encompassing the intervertebral disk and can manifest as intervertebral disk space collapse [8]. The anterior region of the vertebrae is one of the most frequently affected parts of the vertebrae [9].
Diagnosis of solitary tuberculous osteomyelitis can be difficult if the index of suspicion is low. A patient with no pulmonary manifestation and bone pain may be assumed to have a more likely bone lesion or even ligamentous strain. Initial radiographic imaging may appear benign and after failing a trial of non-steroidal anti-inflammatory drugs (NSAIDs), a more sensitive imaging modality such as CT or MRI should be employed to rule out neoplasia or infection [10]. The gold standard for diagnosis is culture of the lesion. Once a solitary lesion of tuberculous osteomyelitis is confirmed, it is recommended to perform a full body scan to search for any other possible extra-pulmonary manifestations of tuberculosis. However, since in most cases of tuberculous diskitis, there are no other extra-pulmonary lesions, a full body scan is not always required.
Screening patients, especially those at increased risk of infection, plays a tremendous role in finding tuberculosis and treating early. A popular screening test is the tuberculin skin test, which can have sensitivity up to 95%. However in immunosuppressed patients, such as those with HIV, the test has a much lower sensitivity (less than 70%) due to skin anergy, according to a recent study [11]. Therefore, the WHO recommends that screening HIV patients for tuberculosis infection should include questions about a combination of symptoms, such as chronic cough, weight loss, fever and night sweats. This will increase awareness of risk of tuberculosis infection and may indicate more specific testing and imaging in order to catch the disease as early as possible in HIV patients.
Download Provisional PDF Here
Article Information
Article Type: Case Report
Citation: Knoll A, Wiesel S, Portal D, Gold E, Kim S (2016) Tuberculous Diskitis Osteomyelitis: A Case Report. J Clin Case Stu 1(5): doi http://dx.doi. org/10.16966/2471-4925.132
Copyright: © 2016 Knoll A, et al. This is an openaccess article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Received date: 27 Apr 2016
Accepted date: 05 Nov 2016
Published date: 10 Nov 2016




