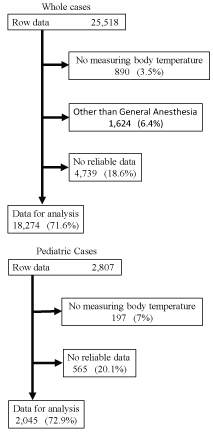
Figure 1: Flowchart of the process of excluding cases according to the exclusion criteria and case grouping.

Mikiko Yumoto Nobutada Morioka* Maho Kinoshita Makoto Ozaki
Department of Anesthesiology, Tokyo Women’s Medical University, Kawadachou Shinjuku, Tokyo, Japan*Corresponding author: Nobutada Morioka, Department of Anesthesiology, Yachiyo Medical Center, Tokyo Women’s Medical University, Yachiyo City Chiba, Japan, Tel: +81-47-450-6000; Fax: +81-47-458-7047; E-mail: nmorioka@twmu.ac.jp
Article Type: Research Article
Citation: Yumoto M, Morioka N, Kinoshita M, Ozaki M (2017) Incidence of Inadvertent Intraoperative Hypothermia with Continuous Air Forced Active Warming. Single Center, Retrospective Study. J Clin Anesth Manag 2(2): doi http://dx.doi.org/10.16966/2470-9956.131
Copyright: © 2017 Yumoto M. This is an openaccess article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Intraoperative hypothermia has been clearly shown in numerous studies to influence various postoperative outcomes. Therefore, body temperature maintenance is performed throughout operations. However, the incidence of hypothermia during surgery with active warming is as yet unknown. We determined the incidence of hypothermia during surgery with active warming at our hospital.
Methods: We reviewed 25,518 anesthesia records in our hospital. There were 5,620 casesin which intraoperative body temperature had not been measured and thus lacked reliable body temperature data. These cases were manually excluded. After exclusion of these cases, we divided the remaining patients into two groups; hypothermia with body temperatures less than 36°C and normothermia with body temperatures of 36°C to 38°C.
Results: Hypothermia occurred in 9,970 of 18,274 cases. There were 8,276 normothermic cases. As to the type of surgery, head and neck operations, including neurosurgeries, and also pediatric surgery, were associated with a low incidence of hypothermia.
Discussion: Although all of these cases received active warming employing an air forced warmer, the hypothermia incidence was still 54.5%. Abdominal and thoracic surgeries were associated with higher incidences of hypothermia than other procedure categories, while the incidence was lower with head and neck surgery. This is attributable to the body being mostly covered during head and neck surgery. The low incidence of hypothermia during pediatric surgery was attributed to higher room temperature and more continuous active warming than during other surgical procedures. In this study, although there were some problems with analysis of the data, due to variability in measuring sites and lack of accurately measured data in several cases, the data presented herein highlight the importance of payingstrict attention to maintaining body temperature intraoperatively and to continue warming patients.
Inadvertent perioperative hypothermia; Active warming; Core temperature; Forced air warming
It has been observed in a number of randomized trials that hypothermia is associated with three major risks, increased incidence rates of cardiovascular events, increased occurrence of wound infection, and greater blood loss in patients undergoing various types of surgery [1-3]. In addition, prolongations of the recovery period and hospital stay after surgery have also been reported [1].These findings indicate that hypothermia has major involvement in the serious mortality rates which can impact surgical patients. Despite the employment of active warming measures, hypothermia is currently a very significant clinical issue, affecting both the safety of surgery and the quality of anesthesia [4]. Although the necessity of preventing hypothermia has long been well known to many anesthesiologists, this important issue has yet to be thoroughly investigated [5,6]. The occurrence of shivering in a hypothermic state might be clinically encountered even if active warning measures are taken. Currently, the use of a forced air warming device is common, and this is a simple and effective procedure [7]. Active warming is not necessarily performed in every institution. The extent that active warming contributes to hypothermia prevention, when performed routinely using forced air in institutions that have an aggressive attitude toward control of body temperature, remains unclear. In our hospital, forced air warming is aggressively performed before and during elective surgery. In order to investigate the actual status of forced air warming for body temperature control, the efficacy of this procedure for hypothermia prevention, in terms of its incidence rates and measuring methods, body temperature control, and awareness of hypothermia among surgeons, was investigated in a single institution employing a retrospective observational study design.
This study was approved by the ethics committee of Tokyo Women’s Medical University, and included patients who underwent surgery under general anesthesia in our hospital. Surgeries performed between February 1, 2008, and March 31, 2010, was covered. Data on intraoperative body temperature were the values measured during surgery extracted in 1-minute intervals from measurements obtained with AIMS (Metavision®, FUKUDA DENNSHI Tokyo, JAPAN). The following cases were excluded, 1. No body temperature measurements were obtained, 2. Body temperature data were of low reliability; and 3. The procedure performed was cardiovascular surgery. As for the low-reliability body temperature data, cases with a minimum intraoperative body temperature of less than 30° C and those with a mean intraoperative body temperature of 34°C or less were manually identified, and excluded due to obvious deviations in the body temperature data. The patient profile parameters extracted were age, height, weight, gender, body mass index, the American Society of Anesthesiologists Physical Status, operative time, and duration of anesthesia.
Based on the data excluded according to the aforementioned exclusion criteria, a minimum body temperature of less than 36°C during surgery was defined as hypothermia. A body temperature of 36°C or higher and less than 38°C was defined as normal, and a body temperature of 38°C or higher as hyperthermia. The incidence rates of hypothermia were compared among patients undergoing thoracic surgery, abdominal surgery, head and neck surgery, and neurosurgery. From the data other than those excluded for the aforementioned reasons, the incidence rate of hypothermia was calculated for a separate group of pediatric patients 16 years of age or younger and for the following subdivided age groups:
For statistical analysis, the incidence rates were expressed as percentages, each of the patient attributes as the mean with standard deviation, and body temperature as a median value. The incidence rates of hypothermia and hyperthermia according to the type of surgery were analyzed employing the chi-square test. Statistical processing was performed using the statistical software JMP (Tokyo, Japan).
Table 1 shows the profiles of patients overall. The total number of patients was 25,518. Excluding 890 patients for whom no body temperature data were obtained during surgery, 1,624 who did not receive general anesthesia, and 4,730 with low-reliability data, a total of 18,274 patients were included in the analysis. Among 2,807 patients 16 years of age or younger, 197 for whom no body temperature measurements had been obtained intraoperatively and 565 who had low-reliability data were excluded, and the remaining 2,045 were included in the analysis (Figure 1). The overall incidence rate of hypothermia was 54.5%. In relation to the type of surgery, the hypothermia incidence rate was 60.8% in patients undergoing thoracic or abdominal surgery, 41.4% in head and neck surgery cases, and, similarly, 41.6% in those receiving craniotomy (Table 2). Among pediatric cases, the overall incidence rate of hypothermia was 42.4%, and the results differed minimally among age groups of pediatric patients (Table 3).

Figure 1: Flowchart of the process of excluding cases according to the exclusion criteria and case grouping.
| Whole | Hypothermia | Normothermia | P-value Hypothermia vs Normothermia | |
| Cases | 18274 | 9970 | 8276 | |
| Age | 56.1 ± 16.8 | 56.7 ± 16.7 | 55.3 ± 16.9 | p < 0.001 |
| Weight (kg) | 58.2 ± 12.1 | 57.2 ± 11.7 | 59.3 ± 12.3 | p < 0.001 |
| Height (cm) | 161.0 ± 9.1 | 160.7 ± 9.0 | 161.5 ± 9.2 | p < 0.001 |
| BMI (kg/m2) | 22.3 ± 3.7 | 22.1 ± 3.6 | 22.7 ± 3.8 | p < 0.001 |
| Blood Loss (ml) | 197.1 ± 600.7 | 238.2 ± 710.0 | 147.8 ± 429.6 | p < 0.001 |
| Operation Time (min) | 166 ± 110 | 180 ± 113 | 148 ± 103 | p < 0.001 |
| Anesthesia Time (min) | 233 ± 120 | 250 ± 124 | 212 ± 112 | p < 0.001 |
Table 1: Background and Profiles of All Patients.
| Cases | less than 36 °C | 36-37.9 °C | more than 38 °C | |
| Total | 18274 | 9970 (54.6%) | 8276 (45.3%) | 28 (0.2%) |
| Chest & Abdominal Surgery | 9053 | 5505 (60.8%) | 3528 (39.0%) | 20 (0.2%) |
| Neurosurgery | 2270 | 944 (41.6%) | 1323 (58.3%) | 3 (0.1%) |
| Head & Neck Surgery | 2575 | 1067 (41.4%) | 1508 (58.6%) | 0 (0.0%) |
| others | 4376 | 2454 (56.1%) | 1917 (43.8%) | 5 (0.1%) |
| elderly patients | 522 | 224 (42.9%) | 298 (57.1%) | 0 (0.0%) |
| ( more than 65 years old) | ||||
| pediatric patients | 2045 | 868 (42.4%) | 1164 (56.9%) | 13 (0.6%) |
| ( less than 16 years old) |
Table 2: Comparison of Overall and Surgical Site-Related Incidence Rates of Hypothermia
| Cases | less than 35.9 °C | 36-37.9 °C | more than 38 °C | |
Total |
2045 | 868 (42.4%) | 1164 (56.9%) | 13 (0.6%) |
| 0 - 1 yrs | 256 | 108 (42.2%) | 146 (57.0%) | 2 (0.8%) |
| 1 - 5 yrs | 854 | 357 (41.8%) | 487 (57.0%) | 10 (1.2%) |
| 6 - 10 yrs | 457 | 196 (42.9%) | 261 (57.1%) | 0 (0.0%) |
| 11 - 16 yrs | 478 | 207 (43.3%) | 270 (56.5%) | 1 (0.2%) |
Table 3: Comparison of overall and age-related incidence rates of hypothermia in pediatric surgery.
Active warming using forced air was employed in all patients after they were brought into the operating room. However, hypothermia occurred in more than 50% of patients as a whole. Although it is unclear whether this figure is entirely accurate, we believe that it serves as a useful reference for the hypothermia incidence in patients who undergo active warming with a forced air device. However, the results must be interpreted with caution as doubt remains regarding the accuracy of the data obtained herein. First, those in whom no intraoperative body temperature measurements had been obtained accounted for nearly 4% of all patients, and those with low-reliability data accounted for 20%. Thus, when combined, these patients, with meaningless data in terms of body temperature measurements, constituted nearly 25% of all potential study subjects. The necessity of excluding nearly a quarter of all potential subjects proves that staff members, as a whole, including anesthesiologists, surgeons, and co-medical professionals did not pay sufficient attention to the patients’ body temperatures [8]. In our hospital, anesthesiology specialists are involved in all surgical cases. However, the presence of so many cases with data deviations may indicate inadequate awareness of body temperature control. Even if active warming using forced air is performed in every patient, the actual effect of active warming cannot be achieved without body temperature monitoring. Therefore, further examination of the efficacy of and support for the importance of active warming with a forced air device or by other means might be necessary, and education on this matter may also be required. In addition, there are variations in the site of body temperature measurement. Rectal temperature is often used in patients undergoing craniotomy, while pharyngeal temperature or bladder temperature might be used in other cases. The reliability of data also varies among temperature monitors, and the characteristic features of surgery are likewise contributory.
Overall, hypothermia occurred in more than 50% of patients. In relation to the type of surgery, hypothermia occurred in at least 60% of patients undergoing thoracic or abdominal surgery. The influence of heat loss from the surgical field seems to be substantial, as described in previous reports. Because laparoscopic or thoracoscopic operations have become more common in recent years, heat loss from the surgical field may be less overt than in the past. It is also possible that the use of bladder temperature produces a stronger tendency for hypothermia [6]. In patients receiving head and neck surgery and craniotomy, the patient’s whole body is covered with a surgical drape [9]. Therefore, it is presumed that heat loss would be minimal, and that the body temperature would be maintained via heat retention. The incidence rate of hypothermia was lower in pediatric surgery cases than in patients overall, who had a higher mean incidence rate [10]. This is probably because the temperature of the operating room is maintained aggressively at higher levels in pediatric surgery cases than in other surgical cases. While heat loss and heat gain are generally regarded as occurring easily in pediatric patients, no marked age-related changes were found in children up to 16 years of age in this study. Although data on postoperative shivering were examined in this study, the presence of shivering in neurosurgery, even in patients whose body temperatures were well maintained, might be attributable to craniotomy [7,11]. Strict implementation of active warming may not be sufficient to prevent hypothermia in all patients, but active warming must always be employed. However, it is necessary to ensure that efforts are made to avoid hypothermia employing various procedures, while always bearing in mind body temperature maintenance. For this purpose, accurate body temperature monitoring is essential. The results of this study revealed that many anesthesiologists actually do not implement close body temperature monitoring and control, despite their knowledge of the importance of body temperature maintenance. We believe that the findings of this study provide an extremely valuable reminder to all anesthesiologists that maintaining body temperature control is clinically essential.
This study has limitations including differences in the sites of measurement, variable accuracies of the measuring methods employed, and the single-center design.
Therefore, further investigation using a prospective design is necessary
While the raw data in this article have already been published [12], the analysis and its purpose are entirely novel.
The incidence rate of hypothermia defined by an intraoperative minimum body temperature of less than 36° C during surgery was more than 50% in an institution where active warming was performed in all surgical patients. Nonetheless, body temperature measurements were lacking or inaccurate in nearly 25% of otherwise eligible study subjects.
There were no conflicts of interest associated with this study
Download Provisional pdf here
All Sci Forschen Journals are Open Access