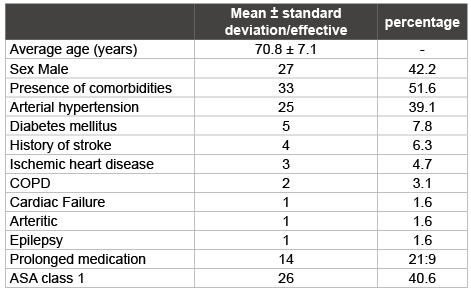
Table 1: Demographic and clinical characteristics of patients

Mahoungou Guimbi KC1,2 Biez U2 Monka M1 Ngatsé-Oko A1 Elombila M2 Moyikoua A1
1Department of Surgery and maternity, University of Marien Ngouabi, Brazzaville, Congo*Corresponding author:Mahoungou Guimbi Kryste Chancel, Department of Surgery and Maternity, University of Marien Ngouabi, Brazzaville, Congo, Tel: 00242055233281; E-mail: mahoungouguimbi@yahoo.fr
Aritcle Type: Review Article
Citation: Mahoungou Guimbi KC, Biez U, Monka M, Ngatsé-Oko A, Elombila M, et al. (2016) Incidence, Clinical Characteristics and Blood Transfusion Factors of Elderly Patients undergoing Orthopedic Surgery in a Tropics University Hospital. J Clin Anesth Manag 1(2): doi http://dx.doi.org/10.16966/2470- 9956.107
Copyright: © 2016 Mahoungou Guimbi KC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Purpose: Identify clinical factors associated with blood transfusion with older patients undergoing orthopedic surgery.
Patients and methods: This is a retrospective study of patients undergoing orthopedic surgery over a period of 24 months.
Results: In total, 64 (21%) of patients aged 60 and older were included in the study. Males (42.2%) were the minority. Comorbidities were dominated by arterial hypertension (39.1%), diabetes mellitus (7.8%) and previous cerebrovascular events (strokes) (6.3%). Thirty-seven (57.8%) patients were ASA class 2-3. Loco-regional anesthesia (75%) was the most used anesthetic technique. This was combined with sedation in 5 cases (10.4%). Arterial hypotension (29.7%) and intra-operative bleeding (4.7%) were the main intra-operative incidents. The incidence of blood transfusion was 37.5%. Multiple logistic regression identified age ≥ 60 years (OR=5.33, 95% CI: 2.11 to 13.42, P=0.0004), duration of surgery (OR=1.02, 95% CI: 1.01 to 1.03, p<0.0001) and the presence of intra-operative events (OR=5.07, 95% CI: 2.34 to 11.00, p<0.0001) as risk factors associated with blood transfusion.
Conclusion: This study shows a reconciliation of the clinical characteristics of elderly patients in the tropics from patients in developed countries. Clinical factors of transfusion are not specific of anesthetic and surgical practice in the tropics.
Anesthesia; Orthopedic surgery; Elderly patients; Blood transfusion
The decline in world poverty is accompanied by an increase in life expectancy in both the so-called rich countries and in developing countries. This correlates to the presence of more and more elderly people in the general population. It is then becoming more common to see anesthesia and surgery for the elderly. In the West, orthopedic and trauma surgery is primarily interested in the elderly [1-4]. In developing countries this surgery focuses on young subjects, the share of activity assigned to the elderly is often misjudged [5,6]. The purpose of this work is to highlight the clinical features of elderly underwent orthopedic surgery and identifies clinical factors associated with blood transfusion for them.
This is a retrospective study over 24 months among patients undergoing orthopaedic surgery after local ethics committee approval. Of this group, we excluded patients under 60 years old, according to the definition of the elderly in our environment [7]. Thus, of the 305 patients involved in the orthopedic surgery, 64 (21%) were of an age ≥ 60 years. The variables studied initially focused on demographic and clinical characteristics of patients, and in a second step we analyzed the influence that these variables could exert on blood transfusion. For statistical analysis, quantitative variables were expressed as mean ± standard deviation and categorical variables as numbers and percentages. Transfusion clinical determinants were sought from the set of clinical factors that could lead to blood transfusion, by simple logistic regression. Then, in a second step, all the factors were included in the same statistical model for multiple logistic regression to identify independent clinical risk factors for intra-operative blood transfusion. The conditions of validity of the multiple logistic regression were established on the basis of seven events by explanatory variables. The statistical significance was set at 5%.
The average age of patients was 70.8 ± 7.1 years (range 60-88 years). Twenty-two (34.4%) patients were aged 75 and over. The sex ratio [M/F] was 0.73. The presence of comorbidities concerned 33 (51.6%) patients. These were dominated by hypertension, diabetes mellitus and a previous stroke with a respective frequency of 39.1%, 7.8% and 6.3%. In addition, 14 (21.9%) patients were receiving long-term treatment for chronic conditions (Table 1). Treatment with calcium channel blockers (10.9%) and vasodilators (4.7%) were at the forefront.

Table 1: Demographic and clinical characteristics of patients
According to ASA (American Society of Anesthesiologists) classification, 27 (42.2%) patients were class 1, whereas class 2 and 3 accounted respectively 32 (50%) and 5 (7.8%) patients. Loco-regional anesthesia was the most used technique (52 cases, 81.2%). Spinal anesthesia (68.8%) and plexus and nerve block (6.2%) were the main techniques used. Three cases of failure (6.2%) were noted in spinal anesthesia. In 5 cases (9.6%), the loco-regional anesthesia was accompanied with sedation. A hypnotic was used in an isolated or associated manner, ketamine (4 cases), diazepam (2 cases) and midazolam (1 case). General anesthesia after the first time or after loco-regional anesthesia failure was used in 16 (25%) patients. Propofol (62.5%) and thiopental (25%) were the main hypnotic drug for anesthesia induction. For myorelaxation vecuronium (68.7%), pancuronium (12.5%) and suxamethonium (12.5%) were used. Fentanyl was the only opioid available. Anesthesia maintenance was provided mainly by halogenated anesthetics including halothane (nine cases or 56.2%) and isoflurane (five cases, 31.2%). The portion of intra-venous maintenance of anesthesia was marginal (two cases or 12.5%). Twentythree intra-operative incidents were reported with 35.9% of incidence. Arterial hypotension and intra-operative hemorrhage constituted the bulk of these incidents, with a respective frequency of 29.7% and 4.7%. Furthermore, lower limb surgery was predominant and involved 55 (85.9%) patients. Among the surgical indications, osteosynthesis (37 cases, 57.8%) and the osteosynthesis material ablation (9 cases or 14.1%) were in the top two places. The blood transfusion rate was 37.5%. The average quantity of whole blood transfused was 1.9 (range 1-3). The simple logistic regression showed that age ≥ 60 years (OR=2.04, 95% CI: 1.13 to 3.68, p=0.01), duration of surgery (OR=1.02, 95% CI: 1.01 to 1.03, p<0.0001), intra-operative events (OR=6.69, 95% CI: 3.77 to 11.90, p<0.0001) and loco-regional anesthesia (OR=2.19, 95% CI: 1.10 to 4.34, p=0.02) were the factors promoting blood transfusion; while general anesthesia (OR=0.43, 95% CI: 0.22 to 0.82, p=0.01) had a protective effect (Table 2). Finally, multiple logistic regression was used to identify independent factors determining intra-operative blood transfusion. These notably included age ≥ 60 years (OR=5.33, 95% CI: 2.11-13.42, p=0.0004), duration of the surgery (OR=1.02, 95% CI: 1.01 to 1.03, p<0.0001) and intra-operative events (OR=5.07, 95% CI: 2.34 to 11.00, p<0.0001) (Table 3).
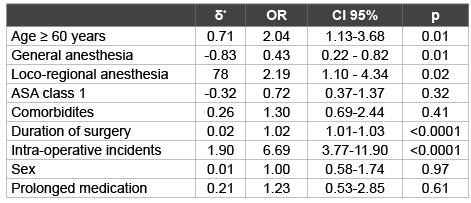
Table 2: Simple logistic regression risk factors of blood transfusion
δ* represents the logistic regression coefficient; OR: odds ratio; CI:
confidence interval of 95%
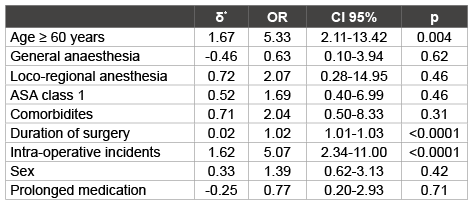
Table 3: Multiple logistic regression factors beyond blood transfusion
δ* represents the logistic regression coefficient; OR: odds ratio; CI:
confidence interval of 95%
The incidence of orthopedic surgery in the elderly aged 60 years-old or more in our study was 21%. This rate varies in developed countries between 18 and 70% [8-10]. This confirms the progressive aging of the population in developing countries. This population aging phenomenon correlated to the emergence of chronic diseases within it. Thus, 51.6% of patients in our study have at least one chronic disease. Hypertension (39.1%), diabetes mellitus (7.8%) and history of stroke (6.3%) were at the forefront (Table 1). Similar results were reported in the literature. For Herrera et al. [11], chronic underlying disease was mainly vascular (69.2%), endocrine and metabolic (50.8%), heart (38.3%) and neurological (35.8%); whereas Brauer et al. [12] chronic heart failure, chronic obstructive pulmonary disease and diabetes mellitus were the main comorbidities.
Patients of ASA class 2-3 numbered 37 (57.8%) while ASA class 1 included 27 (42.2%). The distribution of patients according to the ASA classification could influence long term treatment frequency, class 2-3 was associated with comorbidities will explains the observed rate of these treatments. Similar distribution rates relative to similar classes ASA have been reported in literature [10-15]; whereas for Martinez et al. [2] the median age of patients was 61.6 years and ASA class 1 with 213 (70.5%) patients was predominant. Regarding anesthetic techniques, loco-regional anesthesia was administered to 48 (75%) patients, with 91.6% of cases of spinal anesthesia. The use of nerve blocks was marginal at 8.3% of cases. Sedation accompanied loco-regional anesthesia in 5 (10.4%) of cases. General anesthesia was applied to 16 (25%) patients. Propofol (62.5%) was the main hypnotic and vecuronium (68.7%) the main myorelaxant agent. In the literature, the frequency of general and loco-regional anesthesia in orthopedic surgery varies. Many authors observed the same distribution between loco-regional and general anesthesia as us, in contrast other authors reported a greater propensity for general anesthesia [10,16,17]. Intra-operative hypotension (29.7%) and hemorrhage (4.7%) as major intra-operative incidents identified in this study have also been identified by a number of other authors [11-13]. As the top surgical indication, the majority of patients were operated on lower limbs (85.9%) and osteosynthesis (57.8%). In a study conducted in Spain involving patients of 65 years and older admitted for orthopedic hip surgery, DHS (Dynamic Hip System) plate and intermediate hip prosthesis were the most commonly used techniques. The incidence of bone synthesis was low, 5% of all indications [11].
The blood transfusion rate was high, 37.5%. This rate, however, appears high compared to those reported in the United States [3]. Blood conserving technologies are highly developed in these countries and this could justify these lower transfusion rates. Moreover, in this US study, the age of 60 years, female gender, comorbidities and other criteria within the hospital structure were presented as risk factors for blood transfusion [3]. Older age and female sex were considered as factors increasing the risk of transfusion after hip arthroplasty [18,19]. Furthermore, blood transfusion, the occurrence of intra-operative incidents and increased operative time were associated with the practice of general anesthesia after a multivariate analysis [16]. In our study, age ≥ 60 years (OR=2.04, 95% CI: 1.13 to 3.68, p=0.01), duration of surgery (OR=1.02, IC 95% from 1.01 to 1.03, p<0.0001), the presence of intra-operative events (OR=6.69, 95% CI: 3.77 to 11.90, p<0.0001), regional anesthesia (OR=2.19; 95% CI: 1.10 to 4.34; p=0.02) were risk factors for transfusion blood cells in a simple logistic regression model. General anesthesia (OR=0.43, 95% CI: 0.22 to 0.82, p=0.01) had rather a protective effect (Table 2). In the multiple regression model, age ≥ 60 years (OR=5.33, 95% CI: 2.11 to 13.42, P=0.0004), duration of the surgery (OR=1.02, 95% CI: 1.01 to 1.03, p <0.0001) and intra-operative events (OR=5.07, 95% CI: 2.34 to 11.00, p<0.0001) were independent risk factors determining blood cells transfusion. Long-term treatment (OR=0.77, 95% CI: 0.20 to 2.93, p=0.71) and general anesthesia (OR=0.63, 95% CI: 0, 10 to 3.94, p=0.62) were non-significant protective factors. There were no similar data available in Africa for comparison.
Anesthesia in orthopedics in the elderly aged 60 or higher highlights a high frequency of comorbidities, a propensity for implementing loco-regional anesthesia techniques and a frequent tendency towards blood transfusion. Age ≥ 60 years, duration of the surgery and intraoperative events are clinical factors associated with intra-operative blood transfusion.
The authors declare no conflict of interest related to this article.
Download Provisional pdf here
All Sci Forschen Journals are Open Access