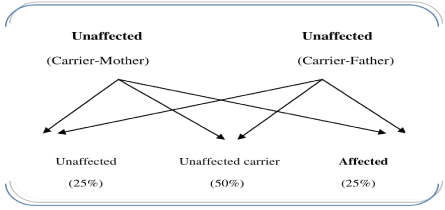
Figure 1: Inheritance of Thalassemia Disease
Sapna Thakur* SN Raw
National Institute of Technology, Raipur, India*Corresponding author: Sapna Thakur, National Institute of Technology, Raipur, India, Tel: 9425550550; E-mail: sapnarajput85@gmail.com
Thalassemia disease (TD) is the most common genetic blood disorder in the world and represents a significant public health problem in India. Currently different forms of the disease identified in many states of India. Beta-Thalassemia form of Thalassemia disease has been identified among the population of Chhattisgarh state. Chhattisgarh state of India is one of the growing states with 25 million populations (census, 2011) and a resource-rich state; it is a source of electricity and steel. The aim of this paper is to present a basic structure of Thalassemia disease and create a short review of the disease prevalent in different parts of Chhattisgarh.
Thalassemia; Abnormal hemoglobin; Bone marrow transplantation; Blood transfusion
Beta-Thalassemia carrier frequencies included India, varying from 1 to 20%, and rarely may be higher. Also, AlphaThalassemia carrier frequencies are much greater, varying from 10 to 20% [1]. It is a genetic condition in which the red blood cells (RBCs) contain abnormal hemoglobin, an abnormal form of the oxygen-carrying protein. Approximately 10,000-12,000 Thalassemia Major (Beta-Thalassemia Major) infants are born each year in India, and the incidence instead of it has been increased year by year [2].
If both parents are Thalassemia carrier have a child, there is a 25%, chance with each pregnancy, with a one to four, that the coming child will have Thalassemia major. In other words 25% chance of having a child with Thalassemia major; 50% chance of having a child with Thalassemia minor; 25% chance of having a normal child [3]. This form of inheritance is medically referred as an autosomal recessive pattern (Figure 1).

Figure 1: Inheritance of Thalassemia Disease
The Thalassemia disorders are the commonest clinically serious single gene disorders. It is estimated that over 300,000 affected children are born every year globally. Around 60,000 of these will have a Thalassemia syndrome and the rest will suffer from sickle cell disease [4,5]. The following section describes the ranges for classification of Thalassemia disease: The Normal range of Hemoglobin (Hb) varies between adult males is 13.0-15.0 g/dL and 11.5-13.5 g/dL in adult, nonpregnant females [6,7]. The following Table 1 characterized the Hb ranges for different types of TD [8].
| Haemoglobin Type | Normal | Carrier | Intermediate | Major |
| HBA | 96%-98% | 92%-95% | 10%-30% | 0% |
| HBF | <1 | 0.5%-4% | 70%-90% | 95%-98% |
| HBA2 | 2%-3% | >3:5% | 2%-5% | 2%-5% |
Table 1: Haemoglobin (Hb) concentration in classification of Thalassemia disease
The Table 1 represents the values of hemoglobin components such as HbA, HbF and HbA2 that are essential to characterize the severity involved in a patient with Thalassemia diagnosis. Thalassemia Minor, Thalassemia Intermedia and Thalassemia major are characterized by reducing Hb levels, Mean Corpuscular Volume (MCV) and Mean Corpuscular Hemoglobin (MCH) [9].
The symptoms are different depending on what state the patient is in. Common symptoms of Thalassemia in Major stage include Yellow discoloration of the skin (jaundice) or whites of the eyes, Weakness, Abdominal swelling, Dark urine (a sign that red blood cells are having problems), Poor appetite. Thalassemia children are normal at the birth and after the six months, they started to generate the different symptoms of Thalassemia disease.
The treatment goals for Thalassemia disease aim to relieve pain, prevent infections, and manage complications. Patients should seek care from a doctor who specializes in blood disorders (hematologist) or a clinic that is experienced in treating Thalassemia disease. Bone marrow transplantation is the only potential cure, but it is used in only a small number of cases as few patients are able to find donors who are suitable genetic matches. Blood transfusions are given to prevent worsening anemia and prevent stroke [10-14]. Drug treatments for Thalassemia disease include: Antibiotics, usually penicillin, are commonly given to infants and young children, as well as adults, to help prevent infections. Patients consider pain relief medication to control pain during the blood transfusion. Hydroxyurea is prescribed for patients with moderate-tosevere Thalassemia disease to help reduce the frequency of pain episodes and acute chest syndrome. The cost involved in the treatment of Thalassemia disease varies from a few thousand rupees to lacks per year, depending upon the kind of treatment considered for the patients [15,16].
Chhattisgarh is one of the growing states of India; the population growth rate is 22.61% [17]. Health sectors of Chhattisgarh Government have worked with various diseases such as Dengue, Malaria, Cancer and Sickle Cell Disease to reduce the complications combined with each disease. However, Thalassemia screening programs have not been considered to identify the affected population. Therefore, Thalassemia Major is the most severe form of the disease and due to lack of awareness and it seems to increase from year to year (Thalassemia welfare society Bhilai, Chhattisgarh). Therefore, we need to generate an initial structure of Thalassemia disease in this population to provide a baseline study for new researchers in this field and as a source for the future implementation of public health measures.
Chhattisgarh is one of the growing states of India where state-level population based screening for Thalassemia disease is not done. Figure 2, shows that in 2012 Thalassemia carrier was 10.61% in screened population and in 2013 it is increased at 14.65% and finally in 2014 it is turned into 17.95% (SourceThalassemia Welfare Society, Bhilai, Chhatisgarh). The data of the study, considered from different parts of Chhattisgarh such as Raipur, Durg, Rajnandgaon, Mungeli, Raigarh, Tilda Bhatapara, Chakarbhata. Also, another type of genetic diseases like SCD and G6PD deficiency is prevalent in this region and studied more than Thalassemia disease [18].
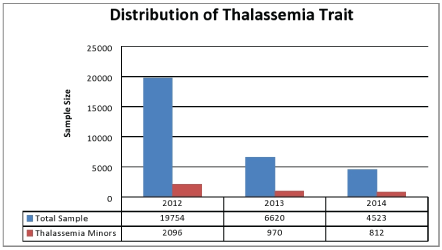
Figure 2: Year-wise Distribution of Thalassemia Trait in Chhattisgarh, India
The present study essentially evaluated the current status of Thalassemia disease in Chhattisgarh in terms of its prevalence, symptoms, diagnosis and treatment. The side effects of multiple blood transfusions in the patient create the damage to various organs. In Chhattisgarh state, there is a need to define what facilities must be identified for the rescue of preventive, primitive and medicinal services with regard to Thalassemia disease and the principles with regard to equipment, consumables, skills and protocols of care needed to ensure this. In the absence of a clear policy articulated, many patients with Thalassemia disease are unable to access the treatment they need in the healthcare facilities.
Download Provisional PDF Here
Article Type: REVIEW ARTICLE
Citation: Thakur S, Raw SN (2018) Thalassemia prevalence in the state of Chhattisgarh: A short-review of the Literature. J Blood Disord Med 3(1): dx.doi.org/10.16966/2471-5026.121
Copyright: © 2018 Thakur S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access