Abstract
Background: In the recent years new techniques were developed in plastic surgery and especially in aesthetic craniofacial microsurgical reconstruction.
Methods: From 2009 to 2013 free-tissue transfer technique has performed in patients with craniofacial defects at the Cancer Institute, Tehran, Iran and the Surgical Hospital of Azerbaijan Medical University, Baku, Azerbaijan Due to the localization patients were classified. Patients were followed, complications recorded and illustrative cases selected for a retrospective cohort review.
Results: Selected patients’ average age were 57 and 39 of them were female, 85 were male. Most of the surgical operations have performed due to the cancer defects (92.5 %) and mostly fibula was used as free-tissue transfer (in 38 cases). Success and complication rates were 96.7 % and 11.2 % respectively.
Conclusion: Nowadays there are many advanced surgical techniques to manage orofacial defects better.
Keywords
Head and neck surgery; Aesthetic surgery; Craniofacial microsurgery; Tissue reconstruction
Introduction
Different tumor types may develop in head-neck region. In the past, to perform resection or reconstruction for these pathologies were impossible. But nowadays the operating microscopes, sophisticated imaging techniques, advanced surgical approaches; micro vascular composite tissue transplantation, interspecialty cooperation (e.g., neurosurgery, neuro-otology, radiation oncology, and medical oncology) and most of all experience give possibilities in difficult cases. Plastic surgeons develop themselves to head-neck-skull base surgeons.
Branches of aesthetic, craniofacial, and microsurgery were improved in the last decades. According to Fisher et al. aesthetic units are already combination of soft and hard tissue but not “skin deep”. In the fact, hard tissue should be with soft tissue to create the unit. For the better result revisionary procedures should be performed.
Materials and Methods
We collected data of patients with craniofacial defects which free-tissue transfer technique has performed from two centers which we noted above. Due to the localization patients were classified. Patients were followed, complications recorded and illustrative cases selected. : Selected patients’ average age were 57 and 39 of them were female, 85 were male.
Etiologies included: cancer (95.2 percent), trauma (0.8percent), congenital defects (1.6 percent), and benign tumor (2.4 percent) (Figure 1).
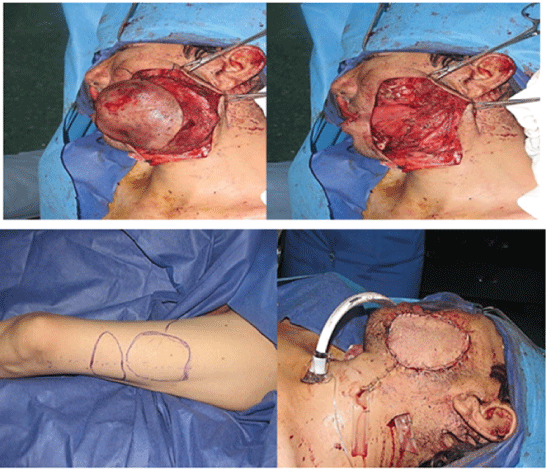
Figure 1: A 37 yrs male with history of recurrent dermatofibrosarcoma protuberance. The tumor resected with 3 centimeters margin. Then a double paddle anterolateral thigh free flap created which one paddle used for lining and another for coverage of the through and through defect.
Free-tissue transfers which we used in these patients: 38 fibula, 6 anterolateral thigh, 19 latissimus dorsi musculocutaneous flap, 12 latissimus dorsi muscle flap, 12 osteocutaneous radial, 16 fasciocutaneous, 14 rectus abdominis musculocutaneous, 6 rectus abdominis muscle, and 1 vastuslateralis flaps (Table 1).
| Etiology |
Percent % |
| Malignancy |
95.2 |
| Trauma |
0.8 |
| Congenital defects |
1.6 |
| Benign tumor |
2.4 |
Table 1: Etiologies of craniofacial surgery.
Free-tissue transfers that we used included: 38 fibula, 6 anterolateral thigh, 19 latissimus dorsi musculocutaneous flap, 12 latissimus dorsi muscle flap,12 osteocutaneous radial, 16 fasciocutaneous, 14 rectus abdominis musculocutaneous, 6 rectus abdominis muscle, and 1 vastuslateralis flaps (Table 2).
| Transferred Tissue |
Number of procedure |
| Fibula |
38 |
| Anterolateral thigh |
6 |
| Latissimus dorsi musculocutaneous flap |
19 |
| Latissimus dorsi muscle flap |
12 |
| Osteocutaneous Radial |
12 |
| Fasciocutaneous |
16 |
| Rectus abdominis musculocutaneous |
14 |
| Rectus abdominis muscle |
6 |
| Vastuslateralis flap |
1 |
Table 2: Kind of transferred tissue.
Results
Success and complication rates were 96.7 % and 11.2 % respectively. As secondary procedures fat injection, tissue resuspension, and cutaneous flap excision have performed which were followed by full-thickness skin grafting or tissue rearrangement.
So, with combination of critical concepts we demonstrate success rates of patients (Figure 2).
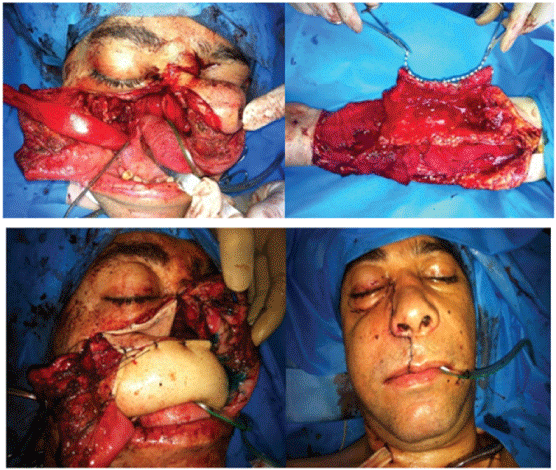
Figure 2: A 32 yrs male with history of SCC of maxilla. Post resection defect is a type 3b. Following creation of an osteocutaneous free fibula flap, the fibula bone sandwiched by the skin paddle and used for reconstruction for the palatal arch. The skin paddle used for repair of the bucal and oral lining.
Dental implants used to support orthopedic rehabilitation and routine reconstruction of subtotal defects of the mandible. In two patient’s preoperative virtual computer simulation used to help performing single stage surgical treatment with immediate orthopedic rehabilitation. Preoperative stage procedures included 3D analysis of pathological and donor sites, virtual simulation of tumor resection, localizing of the dental implants into fibula, virtual flap bending and transfer, virtual bending of fixing reconstruction plates, and fabrication of navigation templates and bridge prosthesis supported by dental implants. Then tumor resected, dental implants inserted into fibula and performed elevation of fibula osteocutaneous free flap, rigid fixation within recipient site and immediate loading by bridge orthopedic device. 10-month follow-up demonstrates acceptable functional and esthetic results. Radiologic examination showed suitable position and integration of dental implants. As a result we observed that we can achieve successful rehabilitation of the patients with extensive defects of the jaws via ablative tumor resection, dental implants insertion prior to flap elevation guided by navigation templates, further osteotomy, modelling of the flap according navigation template, flap transfer and rigid fixation within recipient site by prebended plates, with application of prefabricated prosthesis (Figure 3).
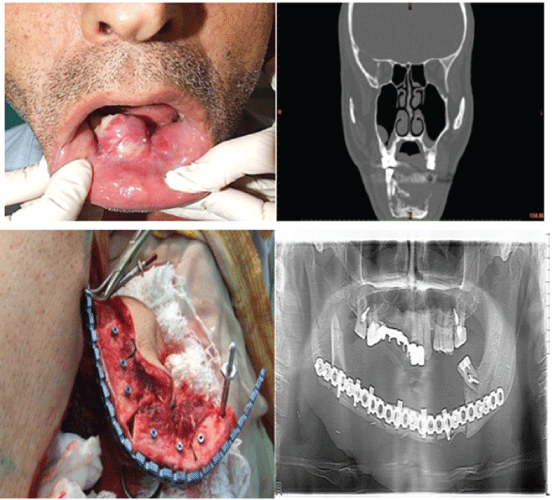
Figure3: The patient with clear cell carcinoma of mandible. Mandible was resected and free fibula reconstruction was done with immediate dental implantation.
Discussion
There is wide range of procedures in reconstructive maxillofacial surgery to repair soft or hard tissue defects of the maxillofacial region [1]. To repair of the jaw and mouth defects have challenges for the surgeon which is mostly indicated in patients with oral squamous cell carcinoma (SCC). Additionally reconstructive procedures used in defects due to benign tumors, trauma, osteoradionecrosis, infection, chronic non-union of bone, clefts, congenital deformities and old age [2,3]. Maxillofacial reconstructive surgery was developed by advanced antibiotics, improved diagnostic imaging and anesthesia [4]. In the last decades, maxillofacial reconstruction developed with improved bone technology, osseointegration and microsurgery and advanced dental prosthodontics. In here we can say that reconstructive surgeries aims are early wound closure and the restoration of form, cosmetics and function. And in this article you can see the role of modern methods in reconstruction and rehabilitation procedures with free tissue transfer, prosthodontics and dental implants [5,6].
In 1970s the craniofacial defects were repaired with soft tissue, and success rate at this method was nearly 60% [7]. Nowadays we can achieve better results with critical concepts in aesthetic craniofacial microsurgical reconstruction which are noted at below [8,9]:
- Knowledge on aesthetic units of face
- The size of defects
- Tissue requirements
- Bone and soft tissue support
- Soft tissue volume
- Timing
- Secondary revision
To perform the bone cuts and the bone shifts in osteotomies are already usual procedures. So, the term exposure by facial disassembly can fit better utterance [10]. The advantages of this concept include freedom from rigid boundaries and anatomic terms due to the development of modern methods of exposure which are newer and safer. By this method we can use ‘as benefit’ approach instead of ‘as required’ approach for patients [11,12]. By all of these new limits created and encountered. Although challenges remain, technologic developments in terms of advanced guidance systems, more punctual and effective radiation treatment, and new chemotherapeutic agents together with earlier diagnosis, improves the outlook for previously incurable conditions [13-16].
In the management of orofacial defects due to disorders such as neoplastic disease maxillofacial reconstruction has an important role [17]. The modern reconstructive techniques are discussed below. Free flap transfer, in the name of Vascularized Free Tissue Transfer (VFTT), now has gained wide acceptance in maxillofacial reconstruction [18-20]. In this procedure detaches from donor site with its blood and nerve supply and transfers to recipient site. In here estimated success rates changes between 90% and 94%. From such perspectives, as influences of postoperative radiation on the vascularized flap are less severity compared to the non-vascularized flap because of the transferred blood supply, VFTT is advantageous over non-vascularized transfer. Different donor sites used for VFTT due to the requirements [21].
Conclusion
Although, there are some harmful functional and psychological effects on the patient due to the orofacial defects, nowadays there are many advanced surgical and prosthetic rehabilitation techniques to manage defects better.
Advanced integration of microsurgery, osseointegration and bone technology to orofacial reconstruction have resulted in more treatment modalities and increased success. Maxillaofacial reconstruction continue to develop by created new techniques and due to these its future seems so bright.
Conflict of interest
The authors declare that they have no conflict of interest.
Article Information
Article Type: REVIEW ARTICLE
Citation: Fathi H, Davudov MM, Foroughiasl P, Rahimov RC, Sultanova NN (2018) Result of Free Flap Reconstruction and Dental Implant Rehabilitation in Patients with Advance Tumors of Maxillofacial Area. Int J Dent Oral Health 4(2): dx.doi. org/10.16966/2378-7090.255
Copyright: © 2018 Fathi H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Received date: 05 Apr, 2018
Accepted date: 23 Apr, 2018
Published date: 30 Apr, 2018




