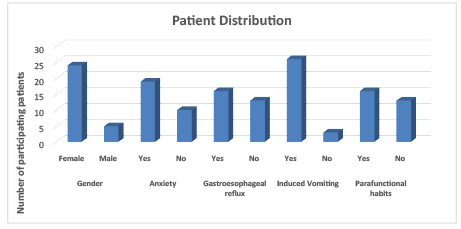
Graph 1: Patient distribution in terms of gender, the presence of anxiety, gastro esophageal reflux, induced vomiting and Para functional habits among bariatric patients (N=29).

Ilma Carla de S Porcelli1,* Carla C Roma2 Margareth CP Nunes3 Sandra Mara Maciel3 Renata C Pascotto3
1Master Student in Integrated Dentistry, Dentistry School, State University of Maringá, Brazil*Corresponding author: Ilma Carla de S Porcelli, Dentistry School, State University of Maringá Av. Mandacaru 1.550, 87080-000–Maringá, PR, Brazil, Tel: 55 44 3305-8617; E-mail: ilmacarlaics@gmail.com
Objective: The objective of this prospective cross-sectional study was to analyze the effects of bariatric and metabolic surgery on the oral health of patients.
Methods: Twenty-nine patients answered a questionnaire after undergoing bariatric surgery. Of these,18 accepted to have their dental condition clinically assessed as well. Mean postoperative time was 4 years. Oral and eating habits were assessed in order to detect the impact of gastroplasty on patients’ lives and on their dental status. The Eccles index was usedto assess the level of dental erosion.
Results: Bariatric surgery complications such as gastroesophageal reflux (55%), induced vomiting (90%), anxiety (65%), and systemic diseases such as anemia, high blood pressure, allergies or a combination of these (59%) were observed. Additionally, changes in eating habits such as craving for candies, ice, beer, finger foods, and sodas (59%), as well ashyposalivation (27%), parafunctional habits (55%), and dentin sensitivity (48%) were also reported. Among the patients submitted to the clinical examination, 55% demonstrated caries and 28% tooth wear Grade 1.
Conclusion: Bariatric surgery had a negative effect on oral health, making the patient more susceptible to dental erosion. The integration of dentists into multidisciplinary teams is essential to early diagnosis and treatment of injuries caused by dental erosion. Dentists’ awareness of the effects of bariatric surgery on the oral health can assist them to improve the quality of life of bariatric patients.
Bariatric surgery; Oral health; Tooth erosion; Dentalcaries
Morbid obesity can increase the risk of chronic diseases and mortality by 50% to 100% when compared to non-obese patients, which explains the significant increase in the number of referrals to bariatric surgery [1]. In 2013, the number of bariatric surgeries reached 468,609 worldwide [2]. In the United States, the number one country in the gastroplasty ranking, about 179,000 procedures were performed in 2013 alone [3].
The impact of the complications of bariatric surgery on oral health has not been fully reported in the few longitudinal studies found in the medical and dental literature [4]. In addition, there is a lack of studies linking oral diseases such as dental erosion with eating and parafunctional habits associated with the emotional aspects of bariatric patients.As a result, in order to better ensure the oral healthof bariatric patients, further research that may bring to light relevant information on the matter is warranted.
Surgery for the treatment of morbid obesity positively affect the treatment and control of comorbidities such as diabetes, sleep apnea, hypertension, dyslipidemia, coronary heart diseases, osteoarthritis, among others.Additionally, it also provides significant improvement in the self-esteem and anxiety of bariatric surgery patients [5], decreasing their susceptibility to depression [6]. However, due to the intake of simple carbohydrates, gastroplasty can also lead to several negative impacts such as nausea, vomiting, flushing, epigastric pain, and symptoms of hypoglycemia, also known as the “dumping” syndrome [7].
Moreover, eating disorders such as anorexia nervosa, bulimia nervosa and binge eating, can also directly affect the oral cavity[8]. Gastroplasty has been correlated with dental problems such as periodontal disease [9], significant increase in dental caries [10], dehydration [11], hyposalivation [12], dental erosion [13], as well as mouth ulcers, dentin sensitivity [14], and halitosis [15]. Complications like osteoporosis, which may also affect the oral cavity in the form of alveolar bone loss [16], secondary hyperparathyroidism [17] and nutritional deficiencies [18] are also other possible complications.
Studies have shown a correlation between low salivary flow and oral diseases such as dental caries, periodontal disease and dental erosion [19]. Typically, due to the gastric changes produced by the surgery, bariatic patients present difficulties ingesting liquids [20], leading to low salivary flow [21]. Furthermore, the buffer effect of saliva is also negatively affected, increasing the risk of dental caries [10] and tooth wear [6] in bariatric patients.
Therefore, the objective of this study was to evaluate the effects of Bariatric and Metabolic Surgery surgery on the oral health of patients, particularly in relation to the development of dental erosion.
This study was submitted and approved by the Local Research Ethics Committee (Protocol no CAAE: 43114215.7.0000.0104).
The target population in this study was obtained through a list of patients submitted to bariatric surgeryat the Morbid Obesity Surgery Centre. As part of the pre-operative routine, all patients were submitted to a complete psychological, medical and oral health examination. Only patients whose records demonstrated goodoral health, ie.,absence of active carious lesions, dental erosions or periodontal disease before surgery were selected for the study.
Patients were initially contacted by phone, when they were informed on the objectives of the study. Patients who accepted to participate were scheduled a visit by the researcher, when any doubts were further clarified and patients were asked to sign an Informed Consent. All participating patients were then asked to answer a questionnaire on the effects of bariatric surgery in their lives, and were invited to have their oral health and dental condition clinically examined.
Any queries concerning any of questions were clarified at the moment the questionnaire was being filled out. The first part of the questionnaire consisted of questions related to patient identification, registration data and socioeconomic status. The second part of the questionnaire consisted of structured multiple choice questions on the effects of bariatric surgery on their daily routine, eating habits and oral hygiene, in order to detect the risk of tooth wear.
In the Morbid Obesity Surgery Centre all patients who accepted to undergo the clinical examination were evaluated by a single examiner, who observed the presence of caries and tooth wear. The examinations were conducted with the use of an explorer, a dental mirror 5 and clinical tweezers [22]. After the examination, patients received professional prophylaxis and were thoroughly instructed on oral health and hygiene, and on the prevention of dental erosion.
For the evaluation of tooth wear in bariatric patients the Eccles index for dental erosion was used [23], through which the chemical dissolution of dental tissues are classified. The index proposes that all the teeth are assessed and adopt scores ranging from 0 to IV, as follows: Class 0 - no wear, when dental surface present no visible wear; Class I - superficial lesions, when the lesion involves only the enamel; Class II - localized lesions, when the lesion reaches 1/3 of the dentin; Class III - extensive lesions, when the lesion covers more than 1/3 of the dentin; and Class IV – restored surface, when tooth surface is restored due to tooth wear.
Data were entered into a Microsoft Excel spreadsheet and descriptive statistical analysis was presented in terms of percentages and graphs.
Thirty-three bariatric patients were contacted, of which 29 accepted to participate in the study. The age of the participants ranged between 20 and 70 years, with a predominance of women (82.76%). All the 29 participating patients answered the questionnaire. Of these, 18 underwent oral clinical examination and prophylaxis. Eleven patients refused to undergo clinical examination, claiming that it was unnecessary, and were referred to their dentists. The mean time since patients had undergone bariatric surgery was 4 years.
Concerning the different types of surgery, 79% of patients was submitted to gastric banding, 14% to Roux-en-Y gastric bypass (FobiCapella surgery), while 7% did not know for sure the type of surgery. Regarding the emergence of systemic diseases after bariatric surgery, 41% of patients reported no disease, while 28% reported having anemia, 10% high blood pressure, 4% allergies, and 17% a combination of two or more of these conditions (anemia, high blood pressure and allergy).
Bariatric surgery had a relevant impact on the eating habits of the individuals as they were prevented from eating in large quantities. Changes in the type of compulsion were identified, where 38% reported having cravings for sweets, 7% for alcoholic drinks (beer), and 14% for one or more types of food and drink (sweets, beer, ice, finger food, and sodas), while 41% reported no compulsion. Moreover, 41% of patients reported not consuming acidic foods and drinks, while 14% reported consuming both, 21% eating acidic food only, and 24% drinking acidic drinks only. Predominance regarding the use of vitamins (72%) was also observed, while 59% reported making use of calcium.
Regarding anxiety, 65.5% of patients reported experiencing the condition, while 34.5% did not. Most of the patients (55%) presented gastroesophageal reflux. The vast majority of participants (90%) reported induced vomiting due to the feeling of food being “stuck” in their stomachs. Most of the patients (55%) presented some sort of parafunctional habit: bruxism (21%), abrasion (14%); clenching and bruxism (10%); abrasion, bruxism and clenching (10%), while 45% did not present any parafunctional habit (Graph 1).

Graph 1: Patient distribution in terms of gender, the presence of anxiety, gastro esophageal reflux, induced vomiting and Para functional habits among bariatric patients (N=29).
Patients were also asked in regard to the time they had last visited the dentist, with a reported mean time of 2 years. Concerning oral status, 69% of patients reported brushing their teeth and 55% rising their mouths after episodes of vomiting, 48% also reported tooth sensitivity, while most (72%) did not feel any decrease in their salivary flow. (Graph-2).
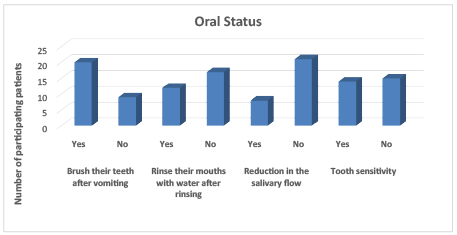
Graph 2: Distribution of oral status variables reported by bariatric patients (N=29).
Among the 18 patients that accepted to be clinically evaluated, 55% presented dental caries, while 72% did not present any visible signs of dental acid erosion. All of the patients with dental acid erosion (28%) were classified as being Class I according to the ECCLES index for dental erosion. The the most affected surfaces were the occlusal surfaces of the lower molars, with slight rounding of the cusps (Graph 3).
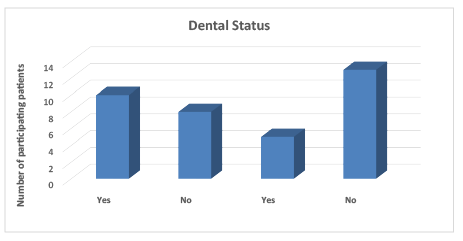
Graph 3: Distribution of the dental status variables among the clinically evaluated bariatric patients (N=18).
Bariatric surgery is the most effective treatment for morbid obesity, resulting in significant weight loss to millions of bariatric patients worldwide [24]. Surgical treatment and long-term weight loss bring improved quality of life and reduce comorbidities [25]. However, several negative effects also exist, which can impact some aspects of oral health, such as dental erosion [26].
Although some previous studies have alsoevaluated the effects of bariatric surgery on dental health [4,27], they are different in design. In the study performed by Heling et al. [27], dental hypersensitivity was self-reported, and tooth wear was not directly assessed. Marsicano et al. [4] evaluated oral changes, such as dental caries, periodontal disease, dental wear and salivary flow, and assessed the impact of oral health on quality of life in a group of bariatric patients before and after the surgery. In the present study, however, an association between dental erosion with parafunctional and eating habitsin bariatric patients was performed. Furthermore, this study also attempted to address those eating disorders triggered by important psychological factors that might have an effect on dental health. The understanding of this correlation is essential for the formulation of strategies to improve the quality of life of bariatric patients.
In the present study, 55% of the bariatric patients presented gastroesophageal reflux, and 90% reported induced vomiting when they felt food was “stuck” in their stomachs, which are common causes of dental erosion due to the created acidic environment with pHs under 2.0. Acidic substances with pH below the critical level for enamel (5.5) and dentine (4.5) can dissolve the crystals of hydroxyapatite [28], and lead to dentin hypersensitivity [13].
Moreover, dentin sensitivity was reported by 48% of patients, a result slightly above that obtained by Heling et al. [27], who observed increased hypersensitivity in 37% of their bariatric patients. Eccles Class I noncarious dental lesions (NCDLs) were observed in 28% of the bariatric patients examined. According to Alves et al. [24], bariatric patients have higher prevalence and risk of NCDLs when compared to patients with morbid obesity but under control. West and Joiner [29] define dental erosion as the loss of tooth structure caused by a chemical process that does not involve bacterial action, caused by acids that may have extrinsic origin, such as acidic foods and drinks, or intrinsic, such as stomach liquids or gases due to eating disorders. The location of the lesions will depend on the etiology: when extrinsic, on the facial surface, and when intrinsic, wear mostly occurs on the palatal and occlusal surfaces [30].
Regarding their food habits, many patients reported either eating or drinking acidic foods (58%) or the association of both (14%). The consumption of acidic foods and especially acidic drinks by bariatric patients is the most likely cause of dental erosion in patients predisposed to enamel dissolution due to the decreased buffer capacity of saliva [28]. Saliva significantly influence the demineralization and remineralizationprocess. According to Dodds [31], patients with small amounts of saliva tend to have more severe injuries due to impaired remineralization. When acidic substances are frequently present, a demineralization-remineralization imbalance tends to occur, promoting the development of dental erosion lesions.
A common symptom in bariatric patients is dehydration, which occurs due to difficulties in fluid intake, exacerbated by vomiting and diarrhea [11]. Greenway and Greenway [32], noted that the flow of saliva decreases in patients with dehydration, and also the buffer capacity of saliva tends to be reduced by the constant presence of stomach acids in the oral cavity. Nevertheless, although previous studies have shown a decrease in stimulated salivary flow in bariatric patients [7,29], most of the participants in this study (73%) reported feeling no change in their salivary flow.This may be explained by the mean time since the bariatric surgery (4 years). Marsicano [4], showed that hyposalivation tends to regress to normal six months after gastroplasty, accounting for the data found in this study.
Greater involvement of the occlusal surfaces of the lower molars with slight rounding of the cusps was also found, which is in agreement with the findings of Mehta et al [33]. Barron et al [34] also observed tooth wear on the lingual and palatal surfaces of the front teeth, which are the areas in greater contact with the acid content of vomit and gastroesophageal reflux. Since the incidence and severity of dental wear significantly increase over time after surgery [34], Bartlett et al. [30] pointed out that greater importance should be given to the prevention and monitoring of lesions for oral health maintenance, rather than to the restorative procedures. Most bariatric patients (69%) reported brushing their teeth after vomiting, a habit that contributes to the loss of dental hard tissues [24]. The temporal proximity between the intake of acidic food and oral hygiene may influence the dental erosion process due to its association with abrasion caused by the toothbrush [35].
Most patients in this study had some kind of parafunctional habit (55%) or a combination of them (20%). For Grippo et al. [36] noncarious lesions has a multifactorial etiology, with the combination of chemical and mechanical factors being commonly present. For them, apart from the acidic diet and gastroesophageal reflux, these injuries also suffer influence of deleterious habits. According to Kwak [37], bruxism, which may be defined as the rhythmic activity of grinding and/or clenching teethprobably associated with emotional stress, is characterized as the most problematic parafunctional habit. A common sign of bruxism is the presence of dental veneers with flat and bright areas that are not part of the natural shape of the teeth, and misaligned centric occlusion [38].
This study revealed a predominance of women (83%) compared to men, similarly to the findings of et al. [39], who also found 81.58% of women in their sample of bariatric patients. This result, the authors noted, testify to the concern females have to seek surgical procedures to achieve not only better quality of life, but also esthetic standards dictated by society. According to Aarts et al. [40], morbidly obese patients are predisposed to anxiety. A fact that was confirmed in the present study, where 65% of patients reported the condition. Furthermore, according to Pataky et al. [41], although longitudinal studies show a trend to a improved psychological status after bariatric surgery, some psychiatric and eating disorders may emerge in this period. Morbidly obese patients demonstrate a higher prevalence of binge eating disorders, which may remain active after surgery [42]. This study showed the impact of surgery in binge eating habit changes, with patients developing compulsion for sweets (38%), alcohol (7%), or a combination of food and/or drinks (4%).
Bulimia is a common form of eating disorder to reduce body weight characterized by overeating followed by induced vomiting [43]. According to Uhlen et al. [44], psychosomatic disorders such as anorexia and bulimia nervosa can result in typical dental erosion lesions. Some medications used to treat bulimia such as antidepressants, can also cause salivary hypofunction, acting as a supporting factor in dental erosion. Moreover, gastric reflux is frequently present in patients with alcohol problems, due to frequent vomiting caused by alcohol abuse [45]. For White et al. [46], it is impossible to predict when eating or other psychiatric disorders may occur in the postoperative period in all cases. However, the early diagnosis of such conditions preoperatively would reinforce the need for carers to keep patients under observation after the surgery. According to the authors, previous eating disorders tend to stop temporarily or undergo change. A good example is when patients replace preoperative binge eating habits by eating small amounts of food for long periods of time (grazing) postoperatively [47].
In the present study, dental caries were detected in 55% of the clinically examined patients. According to Hague e Baechle [10], the increased frequency of food intake (grazing), concomitant with inadequate oral hygiene, could result in a serious frame for the development of carious lesions. Marsicano et al. [4] show that patients after gastroplasty have their gastric capacity reduced by 15 to 50 ml, justifying medical recommendations to increase the number of small meals for longer periods of time, slow chewing and sipping small amounts of liquids all day long. However, the authors point out that, frequently, there is sharp increase in the intake of sweet liquids, leading to a significantly increased risk of dental caries. For Moura-Grec et al. [14], bariatric patients make use of sugary and acidic diets usually at nightwhen saliva is more viscous. When not followed by proper oral hygiene, the host becomes more susceptible to bacterial fermentation.
Overall, bariatric surgery results demonstrate improvements in the systemic health of patients, reducing comorbidities (such as diabetes and hypertension) and the daily ingestion of drugs [48]. In the present study, although 41% of bariatric patients did not report the emergence of any type of systemic diseases after the surgery, 27% presented anemia. For MouraGrec et al. [14], malabsorption of macro- and micronutrients is a common sequelae in patients undergoing bariatric surgery, particularly the Rouxen-Y gastric bypass, where changes in the anatomical characteristics of the gastrointestinal tract, followed by the adoption of restrictive diets, reduce the volume of food intake and may modify the characteristics of the ingested nutrients. According to the authors, the macronutrients found at suboptimal levels can include proteins and lipids, while the micronutrients most often related to nutritional impairments are vitamin B12, iron, calcium and vitamin D3. According to Gesquiere et al. [18], Y- Roux-en gastric bypass (Capella surgery) can reduce the absorption of iron, but the exact amount is still largely unknown. Food habit changes after surgery can also contribute to the development of iron deficiency, which can be caused by the reduced consumption of iron-rich foods (red meat) or by impaired absorption due to decreased production of gastric secretions after surgery [48].
Nutritional counseling, combined with vitamin and mineralsupplementation, should be used by patients in the prevention and treatment of the metabolic effects arising from bariatric surgery [17]. In this study, the vast majority of bariatric patients (72%) reported the regular use of vitamins. However, 41% reported not taking any calcium supplement, which in the long run may negatively affect the health of these patients. Fleischer et al. [49] demonstrated the presence of bone loss associated with bariatric surgery. According to Grec et al. [14], these findings demonstrate the need of further studies to assess the status of maxillary and mandibular bone. When these bone structures are affected, it may lead to tooth loss and compromise the periodontal supporting structures.
One important limitation of the present study concerns the small number of patients that accepted to be clinically examined, which could result in selection bias. The reason why 11 of the 29 patients (38%) did not accept being examined may be accounted by the difficulty some patients have in exposing sensitive aspects of their lives. Thus, had these patients being examined, a greater number of cases of caries and acidic dental erosions, possibly more severe cases, might have been identified. Nonetheless, based on the findings of this study, it is clear that gastroplasty can negatively affect the oral health of bariatric patients. Further studies are required in order to develop protocols for the prevention and treatment of oral diseases of patients that undergo bariatric surgery.
Due to the susceptibility of bariatric patients to tooth erosion and dental caries, the integration of dentists into multidisciplinary teams would be essential for the early diagnosis and treatment of oral conditions. The dental professional is suitably qualified and capable of identifying dental conditions at very early stages. This would be important, as acidic dental erosion and caries can result in extensive health problems in the long term.
Moreover, dentists can also assist in the recognition of other conditions that need to be addressed, among which bulimia and xerostomia, and refer the patient to multidisciplinary treatment by physicians, psychiatrists, psychologists and nutritionists, whenever deemed necessary. Dental care associated with medical treatment can benefit bariatric patients, not only in terms of promoting oral health but also in making patients more aware of the effects of bariatric surgery on oral health, ensuring them better quality of life.
The authors would like to thank the Morbid Obesity Surgery Centre, for allowing the contact with their bariatric patients. The authors would also like to thank Mr. Antonio Carlos Correa for the English version of the paper.
Download Provisional PDF Here
Article Type: Research Article
Citation: de S Porcelli IC, Roma CC, Nunes MCP, Maciel SM, Pascotto RC (2016) Effects of Bariatric Surgery on The oral Health of Patients. Int J Dent Oral Health 2(2): doi http://dx.doi. org/10.16966/2378-7090.181
Copyright: © 2016 de S Porcelli IC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access