Incidence of Agenesis
If, during exfoliation, deciduous teeth do not erupt regularly or persist, patients and parents often discover agenesis of permanent teeth coincidentally. Ageneses exhibit a prevalence of 5.5% and are the most common congenital anomalies encountered in humans [1,2].
Agenesis is differentiated between solitary and multiple (Figures 1a-c and 2a-c). A difference is made between asymmetrical and symmetrical ageneses (Figures 3a-d and 2a-c) and, depending on the region, classified according to aesthetic or functional zones (Figures 4a,b and 2a-c). In case of persistence, a difference is made between the regular occlusion and infraclusion (Figures 3a-d) (quadrants IV and III).
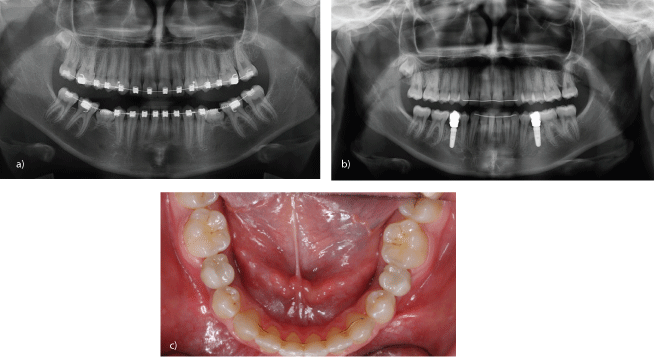
Figure 1a: Symmetrical ageneses 35,45 with persistent, infracluded deciduous teeth (orthopantomograph).
b: Implant-borne prosthetic restorations replacing ageneses 35,45 (orthopantomograph).
c: Occlusal screw-retained, modifiable implant-borne prosthetic restoration replacing ageneses35,45 (clinical image, from above).
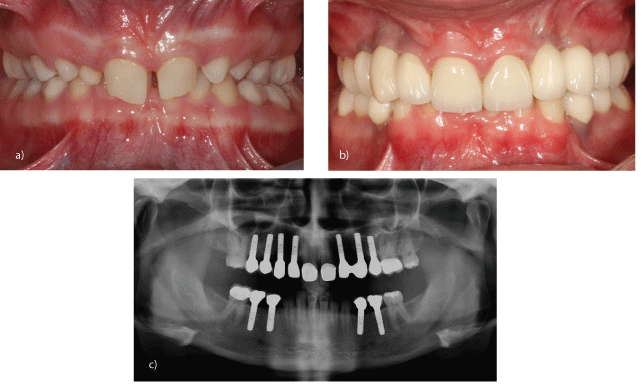
Figure 2a: Multiple ageneses and persistent, non-preservable teeth, closed bite due to lack of tertiary increase in vertical dimension.
b: Multiple ageneses-implant-borne prosthetic restorations.
c: Multiple ageneses-implant-borne prosthetic restorations (check-up X-ray).
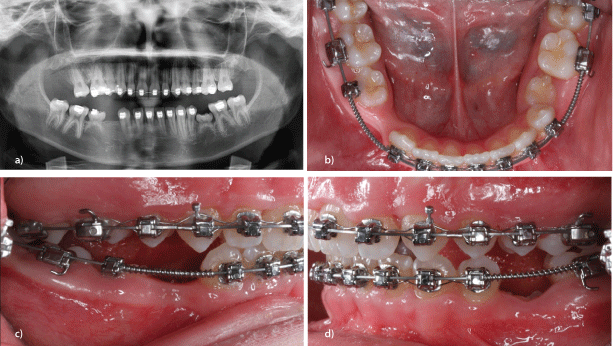
Figure 3a: Asymmetrical ageneses 15,35,44,45, orthodontic gap closure 15, persistent deciduous teeth 75 infraclusion and 85 normal occlusion (orthopantomograph).
b: Asymmetrical ageneses 15,35,44,45, orthodontic gap closure 15, persistent deciduous teeth 75 infraclusionand 85 normal occlusion (clinical view from above).
c: Asymmetrical ageneses 15, 35, 44, 45, orthodontic gap closure 15, persistent deciduous teeth 75 infraclusion and 85 normal occlusion (lateral view, quadrant IV).
d: Asymmetrical ageneses 15,35,44,45, orthodontic gap closure 15, persistent deciduous teeth 75 infraclusion and 85 normal occlusion (lateral view, quadrant III).
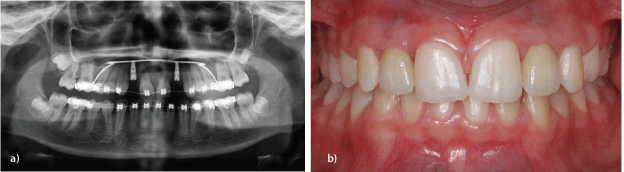
Figure 4a: Implant-borne prosthetic restoration of symmetrical ageneses in the aesthetic zone 12,22 (orthopantomograph).
b: Implant-borne prosthetic restoration of symmetrical ageneses in the aesthetic zone 12,22 (clinical status).
The exact formation mechanism has yet to be fully explained but hereditary causes are considered important (co)factors during the formation of non-syndromal dental ageneses [3]. Scandinavian studies indicate a familial connection as more than half of siblings and other family members of hypodontia patients also exhibit ageneses [4]. They result from point mutation within a closely linked polygonal system [5]. This almost always only affects the permanent dentition [6,7]. Depending on the extent of the anomaly, especially during puberty the affected patients and often their parents suffer immensely whereby a single missing tooth is sufficient to adversely affect the quality of life.
Aplasia is slightly more common in the maxilla than in the mandible [8]. It is usually the second tooth within a group which is missing. The wisdom teeth are the most affected, followed by the lower second premolars, upper laterals and upper second premolars. In isolated cases, dental aplasia may be non-syndromal or syndromal. Where ageneses occur together with syndromes, they are often in conjunction with one of the many forms of ectodermal dysplasia [9].
The degree of suffering caused by ageneses in children and adolescents differs from that of adults. Functionally, occlusal teeth are only missing temporarily from the mixed dentition, which only impedes adolescents minimally. Following puberty, missing teeth not only impede functioning, but the resulting abnormal aesthetics may also affect psychosocial development. For this reason, the guideline recommends aiming at early masticatory functional and aesthetic rehabilitation immediately after the pubertal growth episode. In severe cases of oligodontia or an odontia, for masticatory and speech functional reasons there are grounds for commencing treatment even prior to puberty.
Growth: Craniofacial Growth Versus Alveolar Process Growth
Growth in body length is, like growth in size of the feet, linked to open epiphysial cartilages and their enchondral ossification. Due to closure of the epiphysial cartilages with commencement of menstruation, resp. increase in sexual hormones, growth in length is interrupted in both sexes [10].
Prior to this however, a pubertal growth episode commences in girls at 10 years of age and boys at 12 years which has an effect on the frontal facial height and therefore also the alveolar process [11-13]. In the tibia and humerus regions growth in length is interrupted in girls at an age of approx. 13 years whereas in boys this can last until about 14 years of age. After this point in time, remaining body growth is due to growth of the thorax and spine only [10].
The limits, resp, phases of body growth in length have been thoroughly examined and clearly defined. There is no clear termination in growth of the alveolar process. The alveolar process grows due to desmal ossification (without pre-cartilage stage). During development of the vertical facial height, the maxilla drifts from the cranial base, independent of the teeth, by resorption of cranial material and deposition caudally [6]. Apart from drift, further vertical growth results from continual eruption of the teeth to the occlusal plane. Whilst underway, the teeth in the mixed dentition transport their own bone with them and form the bone of the alveolar process in its final height and width. In case of dental aplasia, this physiological process is lacking thus leading to the typical, rudimentary monocortically formed alveolar process. Where solitary ageneses result in narrow gaps, for example with upper laterals, the height of the alveolar process appears to be influenced positively by the growth of the adjacent teeth [14] yet the width is always monocortical. This is referred to as hypoplasia of the alveolar process. Hypoplasia must not be confused with atrophy. Hypoplasiais a genetically-programmed condition not influenced by growth of the teeth and which remains in a poor condition. Atrophy involves loss of structure from a primarily, regularly formed alveolar process. The initial condition is good yet worsens, in accordance with the various stages of atrophy, due to lack of functioning [15-17].
Thilander determined growth in the alveolar process up until 32 years of age [18]. As implants undergo ankylotic integration, they do not grow with the jaw and may be the cause of infraclusion during continued growth. Where treatment commences at an early stage, modifiable prosthetic restorations should be placed to allow correction of the infraclusion. In the marginal region, if necessary, the residual growth should be planned and compensated for using augmentation during implant placement. This type of treatment is referred to as prospective implant positioning and plays an important role, particularly in the aesthetic zone [19].
The maxilla grows longer than the mandible whereby transversal growth in width takes place until approx. 16 years of age. Vertical growth in the maxilla is special in that it takes place from 16 to 32 years of age [20,18]. Growth of the alveolar processes is governed by the development and extrusion of the permanent teeth. The space required for the tooth roots and expansion of the maxillary sinus provide for vertical growth toward the caudal aspect [21]. Depending on the age group, mean vertical growth is between 1.5mm and 5.7mm in women and 1.9mm and 7.1mm in men [18](Figure 5).

Figure 5: Frontal facial growth in height: The sum of desmal ossification and craniofacial growth.
In children craniofacial growth adds to the growth of the alveolar process. As the substance migrates, this part of growth also influences implants placed early. Therefore, one can reckon with an average pubertal growth episode of approx. 15.5mm in males and 12.5mm vertical facial development in females. The increase in height of the alveolar process must be added to this resulting in mean infraclusion amounts of 17.4mm in males and 14mm in females [13].
As the mean increase in vertical facial height is only approx. 1.4mm between the ages of 14-18 years, during adolescence (between 12-18 years) craniofacial growth is slowed. When the 1.7mm height of the alveolar process is added, and an implant is placed during adolescence the mean infraclusion is approx. 3.1mm (Figure 6).
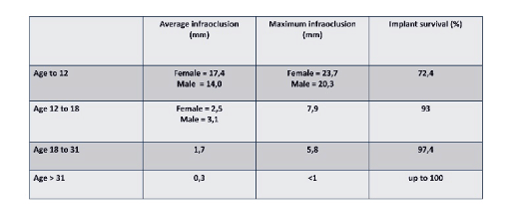
Figure 6: Values shown in literature indicating anticipated jaw growth and resulting infraclusion for implants placed in the relevant age groups and implant survival in the age group (Terheyden).
Once the age of 19 has been attained, it must be assumed that no further craniofacial growth takes place. Up to the age of 32 years, the mean vertical development of the alveolar process is a further 1.7mm. After the age of 32 years minimal infraclusions and changes to the alveolar process were observed. The average value was 0.3mm. Clinically speaking, this value is largely tolerated and a remake not considered until the values were >1mm [22,23].
Alternatives to Implant Placement
Long-term retention of the deciduous teeth
Retaining persistent deciduous teeth maintains masticatory functioning and prevents atrophy. The alveolar process is typically hourglass-shaped because its’ crestal region is retained [6]. Assuming the deciduous teeth drift to the occlusal plane without infraclusion, pocket-formation or harm to the adjacent permanent teeth, they are suitable for maintaining space long-term (Figures 7a-c). However, if the deciduous teeth are in infraclusion extraction is indicated in order to prevent harm to the adjacent teeth as well as vertical bone collapse [24].
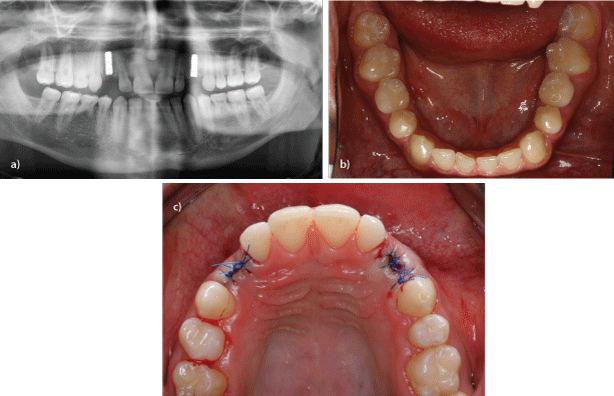
Figure 7a: Multiple ageneses 14,15,24,35,45, persisting deciduous teeth 55,75,85 in normal occlusion, distalisation of teeth 13,23 toward 14,24 and implant-borne prosthetic restoration of teeth 13,23 (orthopantomograph).
7b: Multiple ageneses 14,15,24,35,45, persisting deciduous teeth 55,75,85 in normal occlusion, distalisation of teeth 13,23 toward 14,24 and implant-borne prosthetic restoration of teeth 13,23 (mandible, viewed from above).
7c: Multiple ageneses 14,15,24,35,45, persisting deciduous teeth 55,75,85 in normal occlusion, distalisation of teeth 13,23 toward 14,24 and implant-borne prosthetic restoration of teeth 13,23 (maxilla, viewed from above).
Autografting of teeth
Autografting of teeth is better indicated in cases of traumatic tooth loss than for dental aplasia. Autografting of teeth is advantageous in that they can form their own alveolar process bone. They participate in growth of the jaw and, assuming no ankylotic integration has taken place, orthodontic treatment may be used to mobilise them as with natural teeth. However, the time frame for grafting is dependent upon the roots of the tooth graft having formed optimally (between ⅔ - ¾ of the prospective final length) [25]. A further problem is that a donor must be available and extracting the tooth creates a further gap which must be treated. This treatment is therefore not indicated for cases of multiple agenesis.
Conventional prosthetic restorations
Due to residual growth and limited preparation options due to the extensive pulpal horns, conventional bridgework can be ruled out for children and adolescents [23]. Splinted restorations are difficult where further growth is anticipated.
Assuming the teeth adjacent to the agenesis region are non-carious and the gap is not extensive, single-winged, resin-bonded bridgework may be placed. This appears to be an excellent, long-term type of treatment for replacing missing teeth in this age group. It can be carried out quickly and only causes minimal harm to the abutment teeth. As the restoration is not splinted, growth is not impeded and it can be modified atraumatically during the growth period. In cases of agenesis atrophy due to lack of function is not a problem. As this primarily involves hypoplasia, the condition of the non-functionally loaded region beneath the bridge pontic is not adversely affected (Figures 8a-c).

Figure 8a: Asymmetrical agenesis in the aesthetic zone, tooth 12 is missing, single-winged, resin-bonded bridge (facial view).
b: Asymmetrical agenesis in the aesthetic zone, tooth 12 is missing, single-winged, resin-bonded bridge (maxillary view, without resin-bonded bridge).
c: Asymmetrical agenesis in the aesthetic zone, tooth 12 is missing, single-winged, resin-bonded bridge (orthopantomograph).
Orthodontic Gap Closure
The decision to close a gap using orthodontic procedures should be taken patient-specifically and interdisciplinarily. Not only dental, but also dentofacial and skeletal factors are relevant when deciding on the treatment. There are advantages for cases with additional diagnoses such as lack of space or occlusal anomalies [26-28]. Despite the advantage that further costs for prosthetics are avoided, it has been shown that moving teeth using orthodontic measures is impeded in the atypical bone structure. Closing a gap always has an effect on the vertical jaw relationship. Mesialisation may close the jaw relationship and cause secondary CMD symptoms. Different specialist fields are frequently combined (Figures 9a-c).
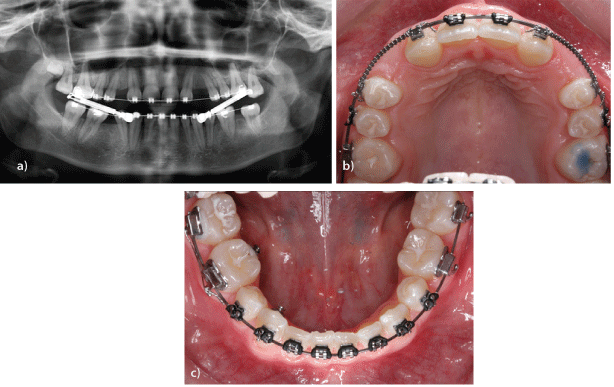
Figure 9a: Multiple ageneses 12,22,35,45, mesialisation of teeth 13,23 toward 12,22 and orthodontic gap closure 35,45 (orthopantomograph).
b: Multiple ageneses 12,22,35,45, mesialisation of teeth 13,23 toward 12,22 and orthodontic gap closure 35,45 (maxilla, viewed from above).
c: Multiple ageneses 12,22,35,45, mesialisation of teeth 13,23 toward 12,22 and orthodontic gap closure 35,45 (mandible, viewed from above).
It is often observed that, following orthodontic gap closure, patients are not satisfied with the aesthetics of the aesthetic zone [29]. The advantage of a biological natural restoration must be compared with the functioning and aesthetics. Diminishment of the dental arch together with mesialisation of the distal residual dentition results in loss of canine-guidance and closure of the vertical jaw relationship. This is frequently the cause of craniomandibular dysfunctioning. For this reason, widening the gap and an implant-borne prosthetic restoration is often the better approach (Figures 10a-c).
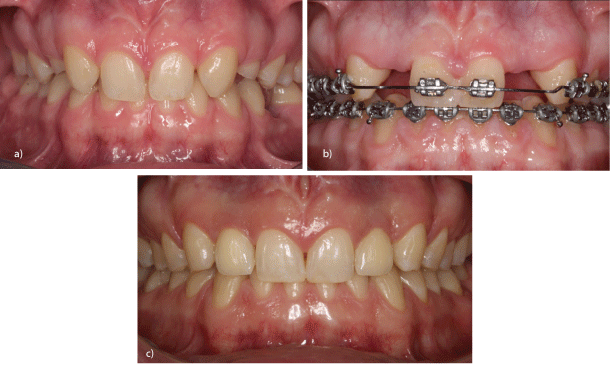
Figure 10a: 18-year-old patient with symmetrical ageneses 12,22, persistent, non-preservable deciduous teeth 53,63 and impacted tooth 35 (facial view).
b: 18-year-old patient with symmetrical ageneses 12,22, orthodontic pretreatment following extraction of teeth 53,63 and exposure of tooth 35 (facial view).
c: Implant-borne prosthetic restorations 12,22,5-year check-up (facial view).
Treatment Concept for Ageneses
Evaluation of the literature shows that the 95.3% survival rate for dental implants is higher than for the above-mentioned alternatives (retention of deciduous teeth 89.6%, autografting of teeth 94.4%, conventional prosthetics 60.2%) [6]. Therefore, implant treatment must be given more consideration for these patients.
Customised, age-independent treatment planning should be carried out interdisciplinarily. Implant rehabilitation during adolescence requires comprehensive diagnoses in order to influence factors such as infraclusion and implant-prognosis as positively as possible. These diagnoses include the body size of the patient and family as well as determination of growth potential and pattern [19]. Over the past years, analysis of the spinal maturity depicted in the lateral cephalometric radiograph has overtaken hand-root analysis for determining the growth potential.
Determining the ideal moment in time for implant placement requires interdisciplinary cooperation and appears to be after the pubertal growth episode [30-32]. Guidelines provide additional help for intensive planning and creating a custom treatment concept [14]. The treatment should be divided into different phases within the time frames of childhood (up to 12 years), adolescence (12-18 years) and young adult (18-30 years) [24].
Aesthetic Versus Functional Zones
While planning for implant placement, the region from which the tooth is missing plays an important role. Whereas functionality is in the foreground for the posterior region, the aesthetic zone is especially challenging. Achieving perfection not only involves contouring the emergence profile optimally, but also in reproducing it symmetrical to the contralateral tooth [33].
In case of dental agenesis, the alveolar process is always monocortical and minimally perfused. As the volume is usually created by the erupting tooth, it is lacking in cases of agenesis. Implant placement in such cases requires sufficient bone and soft tissue augmentation [24].
Asymmetrical Versus Symmetrical Ageneses
In cases of solitary agenesis, the second teeth of a tooth group are frequently affected. This applies particularly to the lower second premolars and upper laterals. Many cases of agenesis are bilaterally symmetrical with the exception of upper laterals which are more frequently missing on the left [34]. Often, the contralateral tooth is only a peg tooth (Figures 11a,b). Intermaxillary discrepancies and asymmetry lead to displacement of the upper midline which adversely affects the aesthetics. Both inclination and drifting of teeth adjacent to the gap result in hyper balanced contacts and incorrect loading. This disturbs the dynamic occlusion and, in case of aplasia of the mandible, may even lead to over closure and traumatisation of the gingival [35].
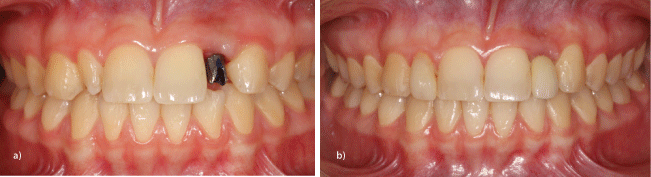
Figure 11a: Asymmetrical agenesis 22 with rudimentary developed tooth 12 (facial view).
b: Implant-borne prosthetic restoration 22 and non-prepared veneer 12 (facial view).
In cases of solitary agenesis, orthodontic procedures should be employed to slow the mesial thrust exerted by the residual distal teeth (Figures 12a-c). The objective is to prevent uncontrolled tooth mobility and commence creation of an adequately wide gap for implant placement [33].

Figure 12a: Symmetrical ageneses 12, 22 in the aesthetic zone-spontaneous tendency to mesialisation of teeth 13, 23 toward 12, 22 (facial view).
b: Symmetrical ageneses 12,22 in the aesthetic zone-spontaneous tendency to mesialisation of teeth 13, 23 toward 12, 22 (orthopantomograph).
c: Taking advantage of the growth episodes while the tooth is erupting for orthodontic pretreatment and widening the gap.
In cases with solitary agenesis, the alveolar process is usually of regular height. This was observed continually in the upper anterior region of the laterals. One of the causes may be the minimal gap between the central and canine which leads to the papilla peaks having considerable influence on the formation of the alveolar process [15]. However, due to the lack of tooth development and eruption of the permanent tooth, the gap does not attain full width but exhibits a monocortical, poorly perfused alveolar process. This must be taken into account during planning and for the augmentation technique.
Multiple Ageneses
In 50% of the agenesis patients more than one tooth was missing. More than 200 genes play an important role in tooth development whereby some of the genes are also responsible for the development of other organs. This fact explains why multiple ageneses usually occur together with syndromes [36]. They are often linked to ectodermal dysplasia [37]. The hereditary form and characteristics of this syndrome are frequently very multiple and often overlooked clinically. The picture shows patients with hardly any perspiratory glands, thin skin and sparse hair as well as a typically round-shaped face. Due to the facial shape, the bite is also closed. The few residual teeth are often smaller than normal and plump (taurodontia) [38](Figures 13a,b). It is advisable to refer patients with a conspicuous clinical appearance to an institute for human-genetics for diagnosis of the syndrome. If mutation can be proven, the parents at least have in Germany the option of applying for an exceptional indication for dental implants as described in paragraph 28 SGB V [24]. Further syndromes closely linked to hypodontia are orodigitofacial dysostose and trisomy 21. With cheilognathopalatoschisis the incidence of agenesis is approx. 30-50%. The larger the cleft, the higher the prevalence of hypodontia [39].
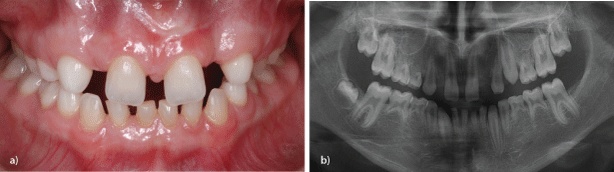
Figure 13a: 12-year-old multiple agenesis patient, persistent deciduous teeth and barrel-shaped permanent teeth (facial view).
b: 12-year-old multiple agenesis patient, persistent deciduous teeth and barrel-shaped permanent teeth (orthopantomograph).
Ageneses lead to a series of negative developments in the stomatognathic system: In addition, the muscle tone of the cheeks and tongue, resp. the failure to transfer the masticatory forces to the bone via the teeth cause advancing resorption of the jaw bone. Multiple ageneses not only adversely affect the function of the orofacial system but also the aesthetics, which often results in serious social impairment especially in younger patients. Further negative developments include tooth rocking, raising/lowering of the adjacent teeth, displacement of the midline and elongation of the non-supported teeth in the opposing jaw as well as over closure and atrophy of the alveolar bone together with the onset of habits and speech defects. For this reason, it is very important that the diagnosis be completed as early as possible and the treatment commenced in good time.
Depending on the degree of oligodontia, a conventional prosthetic restoration without implant-support is not feasible as the irregular positioning of and wide distances between the abutment teeth rule out placing a fixed restoration.
The wider the gap left by missing teeth, the lower and narrower the alveolar process. The clinical appearance of patients with agenesis of more than four teeth also exhibits over closure [40] (Figures 14a,b) which is enhanced if the tertiary physiological increase in vertical dimension due to aplasia of the 12-year molars has not taken place.
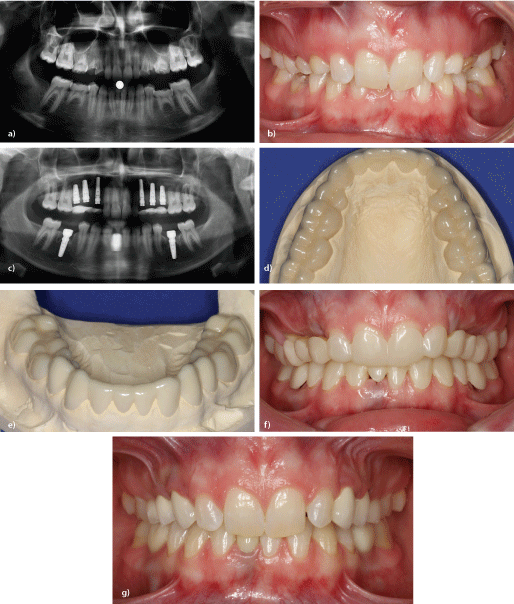
Figure 14a: 16-year-old multiple agenesis patient, non-preservable persistent deciduous teeth and lacking tertiary bite-raising (orthopantomograph).
b: 16-year-old multiple agenesis patient, non-preservable persistent deciduous teeth and lacking tertiary bite-raising (facial view).
c: 16-year-old multiple agenesis patient (post-implant placement orthopantomograph).
d: 16-year-old multiple agenesis patient-Long-term temporary restoration for the implant healing period, raises the jaw relationship (view on upper model).
e: 16-year-old multiple agenesis patient-Long-term temporary restoration for the implant healing period, raises the jaw relationship (view on lower model).
f: 16-year-old multiple agenesis patient-Long-term temporary restoration for the implant healing period, raises the jaw relationship (facial view).
g: Implant-borne prosthetic restoration of a multiple agenesis case-4-year check-up after placing the prosthetic restoration (facial view).
The treatment should compensate for the lack of increase in vertical dimension. During the implant healing phase, long-term temporary restorations can be used to set the vertical jaw relationship. The objective is to guide the TMJ and neuromuscular system to a neutral status and thus prevent CMD symptoms at a later stage (Figures 14c-g).
Where vertical bone deficits are involved, atrophy of the perioral soft tissue may occur. This reaches the point where patients have a positive lip ledge, accentuated nasolabial fold and a generally reduced lower facial third. With multiple syndromal ageneses, often only the cranial base is pronounced and only seldom is a narrow edentulous alveolar ridge present which is corticalised to the point where the buccal and oral compacta fuse. In cases with severe forms of agenesis, apart from a hypoplastic jaw, maxillary retroprognathism and mandibular prognathism often occur which, with additional rotation of the mandible, is referred to as pseudoprognathism [40].
Not only development of the alveolar process stems from erupting teeth, but also that of the masticatory attached gingiva. For this reason, agenesis regions often have insufficient attached gingiva.
When planning the restorations and required number of abutments similar prosthetic principles apply as when replacing teeth lost for other reasons.
Concomitant orthodontic treatment for guiding growth and the strategic positions of the existing abutment teeth are particularly important. Early planning and orthodontic treatment should prevent non-structured tooth movements. In fact, the growth stimulus should be used during implementation of the prosthetic concept in order to position the residual teeth strategically favourably and set the vertical jaw relationship optimally [19].
Conclusions
In cases of tooth aplasia, early interdisciplinary and customised planning/treatment appears to result in successful and lasting rehabilitation.
To achieve this objective, operators have numerous types of treatment at their disposal. As there is no generally valid concept for all patients, operators are confronted with great challenges. A structured treatment “timetable” is especially lacking for the rare cases of multiple agenesis.
For symmetrical solitary ageneses in the posterior region orthodontic treatment for closing the gap often makes sense whereby the vertical jaw relationship is maintained. In cases of asymmetrical agenesis, widening the gap and autografting or implant placement is recommended. Overcrowding of the teeth can be compensated by extraction and orthodontic treatment for closing the gap.
In the aesthetic zone, it has often been observed that orthodontic treatment for closing a gap results in patients considering the resulting aesthetics unsatisfactory. The loss of canine guidance with mesialisation of the distal group is also a drawback for correct functioning. The loss of vertical jaw relationship may often cause CMD at a later stage. For this reason, widening the gap and implant prosthetic rehabilitation is frequently the better approach.
Suspected agenesis should be clarified quickly in order to develop a treatment concept at an early stage. Firstly, it has to be decided whether the deciduous teeth should be retained or extracted. Not only the strategy and treatment planning are important, but also interdisciplinary coordination-accordingly, concomitant orthodontic treatment should commence at this stage at the latest.
In cases of more complex ageneses, dentoalveolar and skeletal anomalies, caused by the lack of growth induction, are corrected. The width of the gap required for the ensuing restoration is then determined. The interdisciplinary treatment takes place over a period of years and requires regular re-evaluation taking facial development into account. For multiple agenesis patients, depending on the number and locations of the natural teeth, prosthetic restorative, resp., implant retentive measures are carried out in order to place a temporary restoration. If one differentiates between the ages and follows the guidelines it is apparent that-heeding the developed concept of prospective implant positioning [41] in numerous cases the advantages of early implant placement outweigh the disadvantages. However, only in absolute exceptions (e.g. anodontiaor severeoligodontia) should they be carried out prior to the pubertal growth episode. The treatment concept should not only be aimed at the type of teeth missing, but also take the entire craniofacial system into account holistically. This requires closely timed recall appointments for evaluating growth tendency and adapting the restoration regularly to the jaw growth.
Whereas success parameters and survival rates are important for the operator and team, the patient-orientated parameters indicate that self-confidence, satisfaction, masticatory functioning and quality of life have increased thanks to the treatment. Studies indicated that patients were most satisfied with dental implants (93.4%), followed by conventional restorations (76.6%), autografted teeth (75%) and orthodontic gap closure (66.5%) [29].
This type of treatment is not only complex and demanding, but also risky in that the residual growth may be miscalculated and should, therefore, in order to rule out failures, only be carried out by experienced operators and dental centres. Once growth has been completed, corrections are only partly possible [41]. Conventional treatments rarely lead to the desired success. In fact, this type of treatment demands far-sighted cooperation between orthodontics, prosthetics, oral surgery and implantology.















