Abstract
Background: NK T-cell lymphoma nasal type is an aggressive and rare form of non-Hodgkin’s lymphoma linked closely to Epstein-Barr virus and primarily involves and destroys mid-facial structures with a poor survival rate. The disease is insidious in onset with early non-specific symptoms obscuring an underlying neoplastic process.
Case description: A case of NK T-cell lymphoma presenting early with symptoms of chronic sinusitis. Infection of odontogenic origin suspected by primary care physician (PCP) based on the later presentation of associated dental pain. Referral and evaluation by oral care specialists ruled out infection of odontogenic origin but failed to recognize an underlying neoplastic process developing due to the unusual presentation in the absence of nasal congestion, epistaxis and swelling.
Clinical relevance: It must be recognized by clinicians that 10% of head and neck malignancies are non-squamous cell carcinomas (SCC) in origin and must be included in the differential diagnosis when symptoms and clinical signs are at variance. Prompt referral to specialists to rule out underlying malignant processes when conventional therapy fails to improve patient-reported symptoms should be made. Delay in diagnosis has a direct impact on treatment morbidity, cost of treatment, quality of life outcomes and on survival outcomes.
Keywords
Extranodal NK T Cell Lymphoma; Epstein Barr Virus; Nasal mass; Midline lethal granuloma; Radiotherapy; Chemotherapy; Head and Neck malignancy
Introduction
Natural Killer (NK) cells are cytotoxic cells that develop from lymphoblastic pluripotent stem cells in the bone marrow. NK cells represent a lineage of lymphocytes distinct from T-Lymphocytes [1,2]. NK cells protect the host by targeting and lysing developing tumor cells and cells infected with either viruses or bacteria [1].
Current World Health Organization (WHO) classification [3,4] recognizes two forms of natural killer cell lymphomas: extranodal NK/T-cell lymphoma and aggressive NK-cell leukemia (ANKL). Extranodal NK/T-cell lymphoma, (Nasal type), is a rare, aggressive form of non-Hodgkin T-cell lymphoma [5,6] that involves primarily the nasal cavity and paranasal structures in more than 70% of cases [6,7]. It is prevalent in individuals of East Asian, Native American, and South American ethnicity and follows an aggressive clinical course with a high mortality rate [7,8]. The adjacent paranasal structures of the palate, orbit, and paranasal sinuses are frequently destroyed to devastating effect by local extension with or without bone erosion. NK/T-cell lymphoma, nasal type, was once thought to be in the spectrum of a midline lethal granuloma, but immunohistochemistry techniques have allowed a better understanding of the malignant nature of this particular disease presentation. Its recognition as a distinct entity from other granulomatous diseases such as sarcoidosis and Wagener granulomatosis that have a similar destructive presentation but a different clinical course in the mid-palate has led to better management protocols for this devastating and deadly disease. A distinctive feature of this condition is that Epstein-Barr virus is always invariably associated with NK/T-cell lymphomas and is thought to a play a yet to be determined role in lymphomagenesis and represents an important diagnostic criterion [9].
Because squamous cell carcinoma (SSC) accounts for approximately 90% of malignancies of the head and neck, its presentation such as non-healing ulceration, bleeding, pain, rolled or raised margins, induration etc. is well recognized by dentists and physicians prompting early specialist referral. However, recognition should be given to the fact non-SSC could present with unfamiliar obfuscating signs and symptoms not distinctive of an underlying neoplastic process leading to a delay in diagnosis thus increasing morbidity and mortality.
The presented case highlights the importance of including a neoplastic process in the differential diagnosis for patients who present with non-specific symptoms not responsive to conventional therapy. Irrespective of the benign nature of the initial presentation, such cases should prompt early referral by the general dentist or primary care physician to an oral and maxillofacial surgeon or ear, nose, and throat (ENT) specialist for additional imaging and diagnostic workup.
Case Description
A 43-year-old Hispanic man presented to the oral oncology and maxillofacial prosthodontic service at The University of Texas, MD Anderson Cancer Center in late November 2016, as a referral from the Department of Leukemia. He presented with amid-facial mass involving the nasal cavity with intraoral extension and erosion but no perforation of the hard palate. Additionally, there was an extensive lymphomatous infiltration involving the maxillary left labial gingiva.
The patient’s history of presenting symptoms started in midOctober 2016 with the patient presenting to his primary care physician with persistent nasal congestion and an itchy nose of 2 weeks’ duration. His primary care physician prescribed a 1-week course of systemic antibiotic therapy and a steroid-based nasal decongestant as initial therapy as the patient worked as a landscaper. The symptoms did not respond to initial therapy persisting with progression to severe left-side maxillary sinus pressure and pain on occluding of the maxillary left posterior teeth within 2 weeks of presenting to his primary physician. Based on new presentation a referral was made by the PCP to his dentist to identify and manage to present symptoms of odontogenic origin.
The patient was seen at his local dentist’s office in early November 2016 within a day of his second primary care physician visit. A comprehensive clinical evaluation and imaging (Figure 1) were performed. The patient presented with no facial asymmetry or changes in the skin of the face. Intraoral examination revealed normal and intact mucous membranes of the oral cavity with normal anatomy of intraoral structures. Thermal tests on teeth of the posterior maxillary left quadrant responded negatively following stimulation and percussion test responded with non-localized mild tenderness. The patient’s periodontal health and oral hygiene were good. No carious lesions evident clinically except for an asymptomatic retained maxillary left second premolar root (#13). Orthopantomogram imaging revealed the absence of clouding bilaterally of the maxillary sinuses, maxillary alveolar bone levels were within normal limits, the absence of intra-coronal radiolucency’s indicative of caries or associated periapical radiolucency’s. Normal presenting root apices anatomy with no resorption, flaring or displacement. Retained root #13 was identified on radiograph with no associated periapical radiolucency
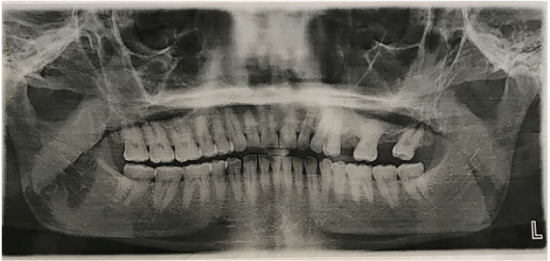
Figure 1: Pretreatment orthopantomogram revealing clear maxillary sinuses with no bony radiolucency in the region of the left maxillary posterior alveolar bone segment. No intra-coronal or periapical radiolucency. Alveolar bone levels within normal limits.
Following clinical examination and appropriate imaging, it was determined to presenting symptoms was of non-odontogenic origin with a likely maxillary sinus origin. Treatment recommendation was for surgical extraction of retained root #13 by an oral and maxillofacial surgeon. A 1-week course of antibiotics (Amoxil 500 mg b.i.d × 7 days) was prescribed to be completed prior to extraction. The retained root of #13 was extracted uneventfully (Figure 2) and the patient advised to seek further evaluation with an ENT specialist in the event of persisting symptoms.
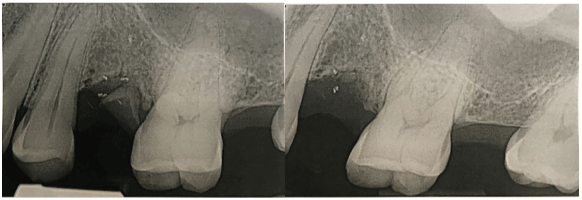
Figure 1: (Left) Pre-extraction and (right) post-extraction periapical radiographs of the retained #13 root tip. Normal trabeculation architecture of the surrounding alveolar bone.
2-weeks following the retained root extraction procedure, the patient presented to an ENT surgeon with a progressive rapidly enlarging symptomatic mid-facial mass and intraoral atypical tissue proliferation of the maxillary gingiva and palate. A nasopharyngoscopy revealed a sinonasal mass and a biopsy of the abnormal tissue sample was obtained and submitted for histologic evaluation. The abnormal diffuse proliferation of lymphocytes was identified and additional immunohistochemical staining revealed positive staining to CD3, CD30, CD56 perforin, granzyme B, ALK-9 negative markers indicative of NK T-cell lymphoma.
On histologic confirmation of high suspicion for extra-nodal NK/Tcell lymphoma, the patient was referred to a local hospital for further workup and treatment recommendations. Because of the complexity of his presenting symptoms, his care was referred to MD Anderson Cancer Center Houston Texas for multidisciplinary management under the Leukemia/Lymphoma department. A further surgical biopsy with immunohistochemical testing confirmed lymphoma and In-situ hybridization for Epstein Barr Virus encoded RNA (EBER) (Figure 3) was positive in malignant cells confirming the diagnosis of extranodal NK T-Cell lymphoma (Nasal Type).
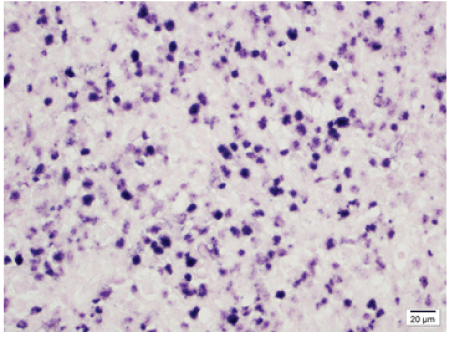
Figure 3: Pathology slide demonstrating EBER positive NK/T-cells.
Computed tomography with the contrast of the maxillofacial area and base of the skull revealed an extensive soft tissue mass measuring 5.5 × 5.3 × 5.4 cm, involving the left nasal cavity and extending into the left anterior ethmoid air cells, with local extension and bony destruction of the medial wall into the left maxillary sinus. Superior extension of the mass involved the left orbit and nasolacrimal duct. Imaging revealed bilateral neck lymphadenopathy with more prominence on the left; some nodes demonstrated central necrosis.
Treatment recommended at leukemia/Lymphoma tumor board was for combination chemotherapy and targeted radiation therapy to the head and neck for local disease control. Radiation treatment planning included in clinical treatment volume (CTV) organs at risk such as the salivary glands and associated structures of the jaws due to the extent of the tumor. A consultation with oral oncology and the maxillofacial prosthodontic department was requested to provide a baseline pre radiation maxillofacial evaluation.
The objective of the consultation with oral oncology was twofold; 1. To identify and manage local infection and teeth of hopeless prognosis prior to initiation of radiation therapy to reduce the risk of developing osteoradionecrosis (ORN) of the jaws. 2. To assess the need for a maxillary obturator prosthesis due to the high risk of developing an oro-nasal/sinus communication from perforation of the nasal floor and hard palate by the locally destructive tumor. This complication would lead to impairment of speech and swallowing (oral phase) and the nasal regurgitation of foods and fluids while eating with detrimental functional and psychosocial impact.
The patient was ambulatory to the oral oncology service and in obvious signs of distress from the painful presentation of the locally invasive tumor. His history revealed up until cancer diagnosis, he was in relatively good health though slightly obese. He had no underlying systemic disease and not on long-term medications. He had no personal or family history of cancer. He did not smoke or report recreational drug use only consuming alcohol socially averaging 1unit per week. He worked as a landscaper.
Extra oral examination revealed asymptomatic mid-facial asymmetry involving the left nasal cavity confluent with the left cheek, infraorbital region, and superior buccal space (Figure 4). There was associated bilateral neck lymphadenopathy at levels II and III. Intraorally, the patient presented with an intraoral mass involving the hard palate prominent on the left side, with a mid-palatal necrosis of the overlying keratinized mucosa with palatine bone exposure but no perforation (Figure 5).
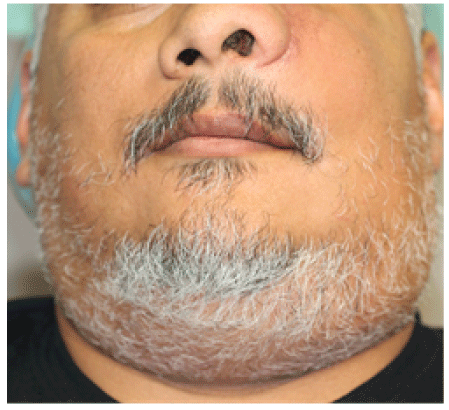
Figure 4: Facial asymmetry with prominent left-side swelling distorting left alae of nostril and malar and infraorbital rim. Bilateral neck metastatic nodal disease evident and on palpation.
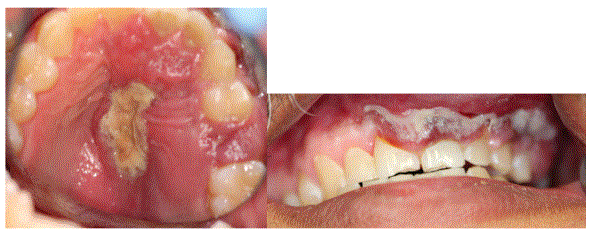
Figure 5: (Left) Intraoral presentation with a necrotic mid-palate and generalized erythematous swelling of the left palate. (Right) Lymphomatous infiltration of the maxillary left labial alveolar mucosa with overlying necrotic slough extending to the midline.
The patient was cleared from an oral oncology perspective following evaluation to begin radiation therapy for tumor control as he presented with low risk of developing ORN due to oral tissues absent of dental disease. It was determined not to capture records of dental anatomy with preliminary impressions for the fabrication of maxillary obturator prosthesis at this appointment as there was no oro-antral communication and the likelihood for changes to oral tissues was high rendering any records captured inaccurate for preciseness of fit for future obturator prosthesis fabrication.
Concurrent chemotherapy DeVIC (dexamethasone, etoposide, ifosfamide, and carboplatin) and intensity-modulated radiation therapy (IMRT) targeting the nasal lesion and bilateral supraclavicular nodes was initiated in early December 2016 for curative intent as standard algorithm regimen.
In the first week of January 2017, 4 weeks after initiation of therapy he presented to the emergency room at MD Anderson cancer center with respiratory distress with symptoms of severe dyspnea and stridor on respiration. A chest x-ray revealed multiple discrete lung masses that were initially thought to be a pulmonary fungal infection. A biopsy of the lung masses revealed distant pulmonary metastasis of NK/T-cell lymphoma. Computed tomography of the head and neck confirmed refractory and progressive disease with brain metastases following initial response to first-line therapy. Due to widespread fulminating disease, treatment rational was amended for a palliative goal utilizing immunotherapy Brentuximab and dexamethasone. The patient died 3 weeks later from complications of his disease.
Discussion and Conclusion
Extranodal NK/T-cell lymphoma (ENKL) is an aggressive rare form of non-Hodgkin lymphoma accounting for 7-10% of non-Hodgkin lymphomas in Asia and Central America [9]. ENKL due to its nonspecific early presentation, early diagnosis of this disease process is fraught with difficulty owing to the wide variety of symptoms. Irrespective of specialty, all dentists must be at the forefront of cancer prevention and include in their scope of clinical practice a routine and systematic periodic evaluation of all new and established patients’ head, neck and oral tissues. This clinical examination must be accompanied by specific questions that may reveal subtle early symptoms of an underlying disease process such as slow healing ulcerations, lumps, dysphagia, dysphonia, and otalgia. If such presenting symptoms persist for greater than two weeks after conventional therapy, prompt referral and further evaluation is warranted by appropriate specialists in either oral medicine, oral and maxillofacial surgery or otolaryngology.
The pathogenesis is unclear but has a strong association with Epstein-Barr virus, which probably acts as an oncovirus. The World Health Organization criteria require identification of EpsteinBarr–encoded RNA (ribonucleic acid) within samples to establish a diagnosis of NK/T-cell lymphoma [8]. Immunohistochemical markers with antibodies against NK-cell CD56 or T-lymphocyte CD3 antigens help confirm the diagnosis.
The pain of odontogenic origin is an unusual initial presentation as seen in this case with nasal involvement and swelling being more common [2]. This disease depending on its presentation be misdiagnosed as one of the other midline destructive diseases of the hard palate such as Wegener granulomatosis, sarcoidosis or cocaineinduced mid-palatine destruction [10]. ENKL of the orbit has also been reported in the literature described as being equally lethal and often misdiagnosed as an orbital cellulitis in the initial stages leading to blindness as a result of the delay in diagnosis [6].
The last decade has seen a marked improvement in the overall survival rate for early presenting ENKL. This is attributed to a change in treatment protocol from the refractory anthracycline containing chemotherapy regimens such as CHOP (Cyclophosphamide, Hydroxydaunomycin (Doxorubicin), Oncovin (Vincristine) and Prednisolone) conventionally used in lymphomas/leukemia to platinum containing regimens such as DeVIC (dexamethasone, etoposide (VePesid), ifosfamide, cisplatin) combined with concurrent radiation (CCRT) [11]. The refractoriness to anthracycline based chemotherapy regimens is due to the presence of P-glycoproteina product of multi-drug resistant gene (MDR1) expressed in tumor cell membrane that actively pumps anthracycline out of cell cytoplasm rendering it ineffective. P-glycoprotein, however, has no effect against platinum (cisplatin) based or L-asparaginase containing regimens such as SMILE (steroid, methotrexate, ifosfamide, L-asparaginase and etoposide) hence effective against extranodal NK lymphoma. Jimenez-Perez et al. reported an overall response rate (RR) 82% and complete response rate of 79% in patients treated with combined chemo-radiation in patients with stage 1 and 2 disease6.In another paper by Tse et al, a higher ORR of 89.7% with a lower CR rate of 69% as reported [2]. Another approach to therapy is targeting PD-1/PDL1 (programmed death ligand) and CTLA4 (Cytotoxic T-lymphocyte associated protein 4) upregulated by EBV in lymphoma cells with checkpoint inhibitors such as Pembrolizumab or nivolumab [12,13], a humanized anti-PD-1 monoclonal antibody. These specific molecules PD-1/PDL1 and CTLA4 are responsible for tumors ability to mount a negative immune response and resist detection and promote proliferation.
Extranodal NK/T-cell lymphoma is highly aggressive, with a poor prognosis and a high mortality rate if not managed promptly and especially if late presentation. Symptoms not responsive to conventional treatment in the absence of obvious odontogenic origin or dentoalveolar infection should alert the primary care physician or general dentist to a more insidious disease process and prompt early referral for specialist evaluation and appropriate imaging.
Conflict of Interest
None
Article Information
Article Type: CASE REPORT
Citation: Otun A, Qazali AA, Won A, Chambers M (2018) Natural Killer T-Cell Lymphoma (Nasal-Type) Presenting Early as Pain of Odontogenic Origin. Int J Dent Oral Health 4(3): dx.doi. org/10.16966/2378-7090.261
Copyright: © 2018 Otun A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
Received date: 09 May, 2018
Accepted date: 20 Jun, 2018
Published date: 27 Jun, 2018





