
Figure 1: Maxillary RPD providing teeth as well as acting as an Appliance for increasing the vertical dimension


Harold S Cardash*
Department of Prosthodontics, Goldshleger School of Dental Medicine, Tel Aviv University, Israel*Corresponding author: Harold S Cardash, Department of Prosthodontics, Goldshleger School of Dental Medicine, Tel Aviv University, Israel, Tel: 098338613; E-mail: cardash@inter.net.il
This short article is designed to bring greater awareness to the Dentist and the Dental Team. A few points in the treatment of a partially edentulous patient. Self-care and the ability of the patients to fully understand the function of a removable prosthesis are critical influential factors which sometimes may be overlooked when constructing a removable partial denture.
The article concentrates on the lack of oral hygiene. After 50 years of RPDs in private dental practice it still seems to be still the most potent enemy of the restorative dentist.
Why does the patient clean well enough the first two weeks and then his enthusiasm wanes and he returns to his old habits. Even three monthly visits to the hygienist do not seem to help. Much work and attention for the long term success of the RPD’s should focus efforts to elicit best practices.
Removable partial denture; Oral surgery; Oral hygiene
Whilst the dental literature is replete with articles describing the designs and technique used in creating a removable partial denture (RPD), little has been written on the performance of the RPD in the aftermath. The RPD is delivered with brief instructions on hygiene and the patient dismissed with a “have to get used to it”. The RPD is not used today as often as in the past partly due to the advent of implants, but there (Figure 1) are still many patients who decline implants because of the high cost of treatment and necessity on some occasions to first surgically provide an adequate implant foundation; another group would be those who are medically unfit to undergo oral surgery.

Figure 1: Maxillary RPD providing teeth as well as acting as an Appliance for increasing the vertical dimension
As the price of gold has dramatically increased over the past few years most dentists have now switched from gold to chromium-cobalt for their RPD castings. Whilst chrome-cobalt has adequate strength to maintain the majority of major and minor elements, the retaining part of the clasp structure maybe liable to fracture because of failure at a lower stress level due to fatigue [1] above its proportional limit. Following designing the RPD the refractory model is scored about 1.5 mm deep which acts as a guide to the finishing line of the final RPD. Beading ensures tissue contact of the major connector with palatal tissue.
Bates [2]however found that the fatigue limit of cobalt chromium alloy is just above its proportional limit and fracture is also due to repeated distortion at lower stress levels.
The RPD has been likened to a bikini with minimum coverage of tissue and minimum retention.
If a long lip exists, the teeth and associated structures may be hidden (Figures 2 and 3) and even clasps placed on anterior teeth. The rigidity of the palatal part of the RPD may be strengthened if full coverage is used.
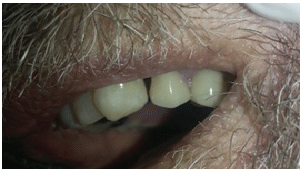
Figure 2: Long lip hiding RPD elements
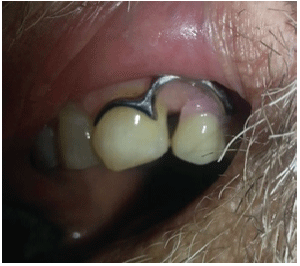
Figure 3: Clasp exposed by finger moving lip
However this may cause the patient to partially or temporarily lose his sense of taste or feel a metallic taste in the mouth.
RPD can be a potentially dangerous appliance especially in the mouth where there is periodontal disease. Treatment of the soft tissue is the same as for any patient suffering from chronic periodontitis; scaling, polishing and emphasis on methodical oral. The mouth must be cleansed after every meal as must the toothbrush and any other cleansing aids used. The RPD should be held by its major connector while each element is carefully cleaned. A bowl with water or a wet rag will soften the blow should the denture be dropped and avoid denture breakage or clasp deformation. The correct position for removal of the prosthesis is to place the fingernail medially or distally to the clasp, and not immediately apical to it. When seating the prosthesis it should carefully be positioned in place with the fingers. The tendency to approximately place the prosthesis and then bite it into place is to be condemned. The patient is not allowed to leave the surgery until competence is shown in placing the appliance.
The metal must be worked at high temperatures that may cause problems to the dental technician, so that some laboratories now refuse handling the metal and obliging the dentists to send their work abroad for casting thereby increasing time between appointments.
Download Provisional PDF Here
Article Type: Editorial
Citation: Cardash HS (2017) 50 Years of RPDs in Private Dental Practice. Int J Dent Oral Health 3(2): doi http://dx.doi.org/10.16966/2378-7090.e102
Copyright: © 2017 Cardash HS. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access