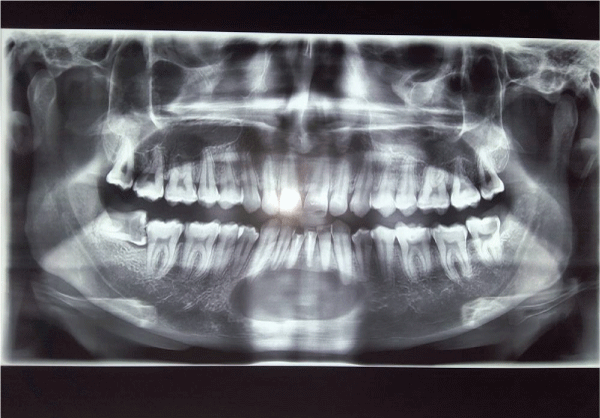
Figure 1: Orthopantamogram showing large radibular cyst in anterior mandible


N Dhineksh Kumar1* J Eugenia Sherubin1 Mathew Jose1 C Swaminathan2
1Professor, Department of Oral and Maxillofacial Surgery, Sree Mookambika Institute of Dental Sciences, Tamil Nadu, India*Corresponding author: N Dhineksh Kumar, Department of Oral and Maxillofacial Surgery, Sree Mookambika Institute of Dental Sciences, Tamil Nadu, India, E-mail: dhineksh@gmail.com
The Radicular cyst is the most common cyst occurring in the head and neck region. It is also called as root end cyst, periapical cyst and apical periodontal cyst. The causative factor of the radicular cyst is a non vital tooth. The radicular cyst is an odontogenic cyst formed due to the stimulation of cell rest of Malassez derived from the Hertwig epithelial root sheath. Similar to all odontogenic cysts it expands by hydrostatic theory and osmotic pressure theory. Smaller radicular cysts remain asymptomatic until they get infected. The large radicular cysts cause bone resorption, tooth displacement and if the inferior alveolar nerve is involved it causes paraesthesia. The management of radicular cyst is by conservative management or marsupialisation alone or enucleation alone or marsupialisation followed by enucleation. If the teeth involved in the cysts are salvageable, root canal treatment, apicoectomy and retrograde filling are done in order to salvage the teeth involved. To select an appropriate treatment plan from above the extent of the cystic lesion is an important factor. Thus it is clear that the selected diagnostic imaging modality should provide adequate information regarding the bony and soft tissue extent. Here we report a case of large radicular cyst of mandible involving all the six lower anterior teeth of the jaw successfully managed by enucleation followed by apicoectomy and retrograde MTA restoration of the six lower anterior teeth along with comments on diagnostic imaging.
Cyst is defined as pathological cavity filled with fluid, semisolid or gas except pus, covered by connective tissue which may or may not be lined by epithelium [1]. Radicular cyst is the most common odontogenic cyst with the incidence of 60.3% of odontogenic cysts and the mean age of occurrence is 37.5 years with male, maxillary predominance [2]. Radicular cysts form 52 to 68% of all the head and neck cyst [3]. Radicular cyst is an inflammatory odontogenic cyst derived from the remnants of Hertwig epithelial root sheath called as cell rest of Malassez [4]. Radicular cyst is a sequelae of apical periodontitis resulting from dental caries or periodontitis or from nonvital teeth due to trauma [5]. These cysts are commonly found around the apices of the teeth but can also occur lateral to it in relation to accessory root canals.
The radicular cyst causes buccal and palatal expansion in maxilla while in mandible it causes only buccal expansion and very rarely lingual expansion. It also causes teeth displacement and bone resorption extending into the soft tissues and rarely causes tooth resorption and nerve paraesthesia [6]. In the following case report we discuss the successful management of large radicular cyst by enucleation followed by apicoectomy and root end retro grade filling by MTA.
A 23 year old male patient reported with a complaint of painful swelling in the lower front region of the jaw for the past two weeks. The pain was continuous and aggrevated on mastication and relieved at rest and medication. Patient noticed the swelling two months back which started as a small swelling and grown gradually to reach the present size (3 × 4 cms). Patient had a history of trauma 10 years back and root canal treatment for the teeth in relation to the swelling 2 years back. On extra oral examination the swelling was 3 × 4 cm in size, surface normal with firm consistency and no mouth opening restriction with palpable and tender bilateral submandibular lymph nodes. On intraoral examination patient had swelling of size 3 × 4 cm in the mandibular symphysis region which extended from periapical region of 33 to 43 regions obliterating the labial vestibule. The surface of swelling was normal without any scars and sinuses. Margins were well defined. On intra oral palpation the swelling was tender and firm in consistency. The aspirate from cyst revealed a straw colored fluid with protein estimation of about 10.2 g/dl. The teeth 31,32,33,41,42,43 were non vital.
Orthopantamogram (Figure 1) showed well demarcated unilocular radiolucency with sclerotic borders in the intercanine region of the mandible (i.e. extending from 33 to 43). As the OPG is two dimensional modality of imaging the interference of vertebral column is seen over the region of the central mandible. Thus the three dimensional Computerized Tomography was opted for knowing the antero posterior extension and integrity of buccal and lingual cortical plate of the mandible. The CT images (Figures 2-4) revealed intact lingual cortex except for some small perforations, with complete loss of buccal cortex in relation to the anterior mandible. The total dimension of the cyst was 5x4x3 cm extending from the bone to the soft tissues. After systemic examination and blood routine workup, the treatment plan of cyst enucleation with apicoectomy and retrograde filling with Mineralised Trioxide Aggregate for all the six involving teeth under local anesthesia was proposed. The patient underwent root canal treatment for all six involved teeth 31,32,33,41,42,43 prior to the surgery.

Figure 1: Orthopantamogram showing large radibular cyst in anterior mandible
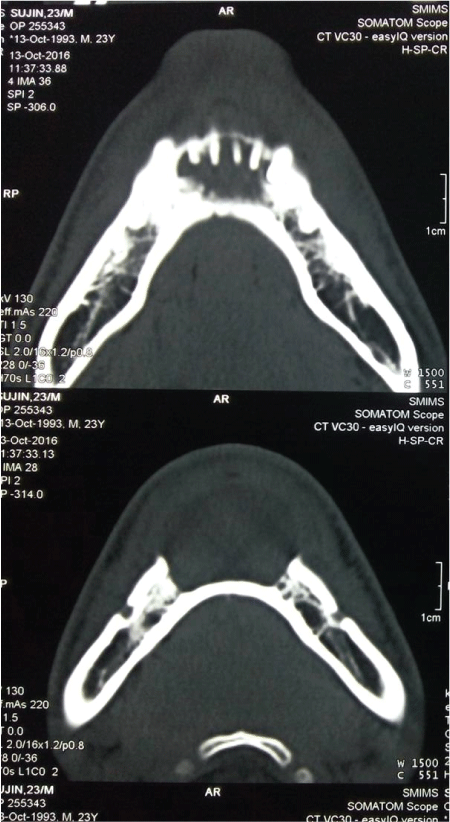
Figure 2: Axial view of cyst in CT showing involvement of teeth apices and resoprtion of buccal cortical bone and soft tissue extension
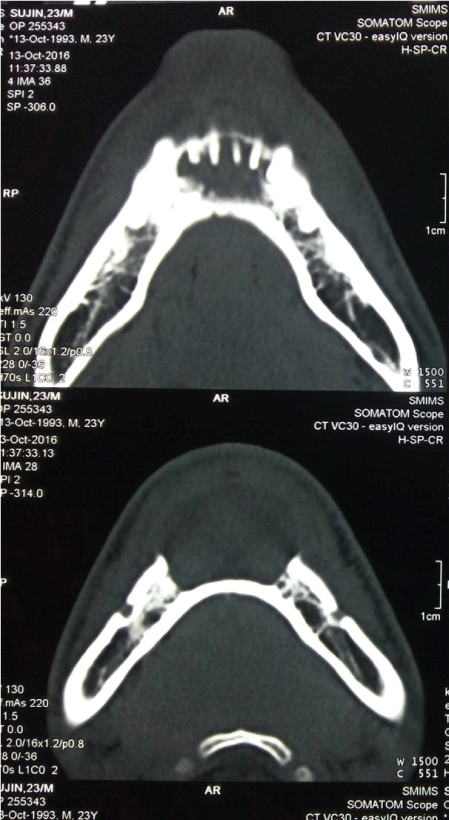
Figure 3: Coronal view of Cyst in CT showing soft tissue involvement and intact lower border of the mandible
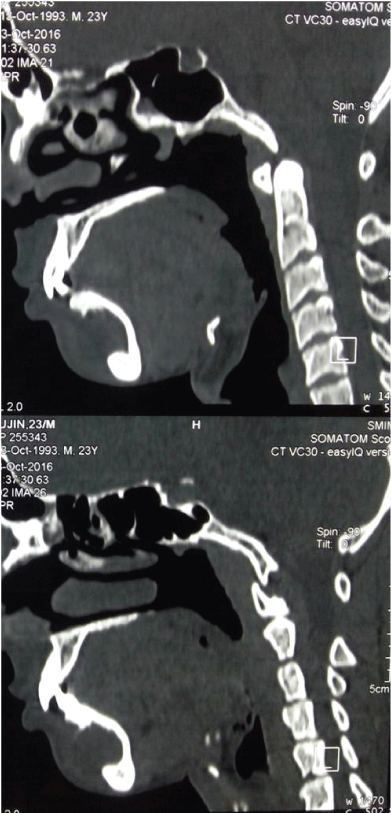
Figure 4: Saggital view of cyst in CT showing complete loss of buccal cortex with intact lower border
Under local anesthesia and aseptic condition, crevicular incision was placed on the buccal aspect from 36 to 46 regions for adequate exposure. The mucoperiosteal flap was elevated off from the cystic lining by blunt dissection without puncturing the cystic cavity (Figure 5). After exposing the circumferential bony margins of the cyst, the cyst lining is elevated out from the cystic cavity using peanut gauze to avoid rupture of the cyst (Figure 6). Once all the margins of the cyst have been elevated from the bony attachment, the cystic lining is curetted out from the cavity. Peripheral ostectomy with 703 bur was done around the corners of the bony margins to ensure the complete removal of the cyst and to expose the apices of the six anterior teeth for apicoectomy and retrograde filling. After the exposure of the apices (Figure 7), 3mm of apices were resected with the angulation of 90 degree from the tooth approaching it through the cystic cavity (Figure 8). Apical cavity preparations were made using hand instruments and after obtaining complete hemostasis, Mineralised Trioxide Aggregate is packed into the prepared cavity in the apical region (Figure 9) and the surgical site is closed primarily with the flap recovered over the bone cavity. The Post operative phase of the patients was uneventful and the six months post operative OPG (Figure 10) shows good bone formation without using any bone graft material.
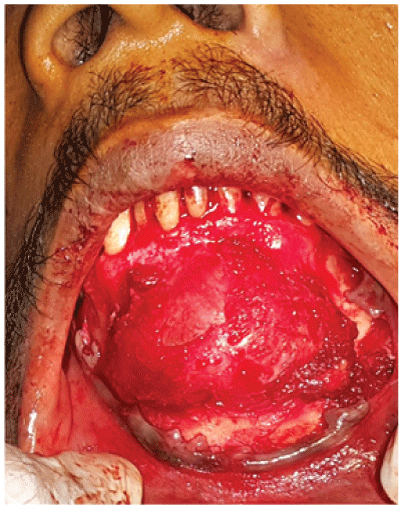
Figure 5: Cyst after exposure
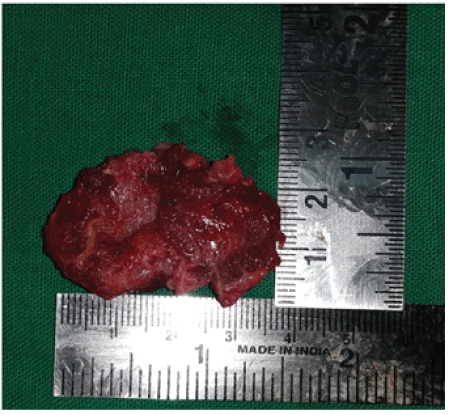
Figure 6: Enucleated specimen
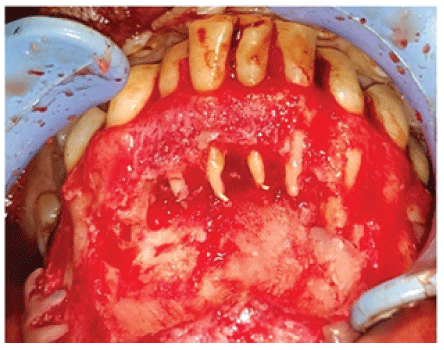
Figure 7: Cystic cavity showing Gutta Percha in root apexes
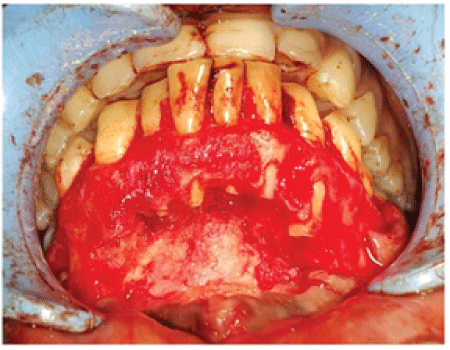
Figure 8: Post apicoectomy
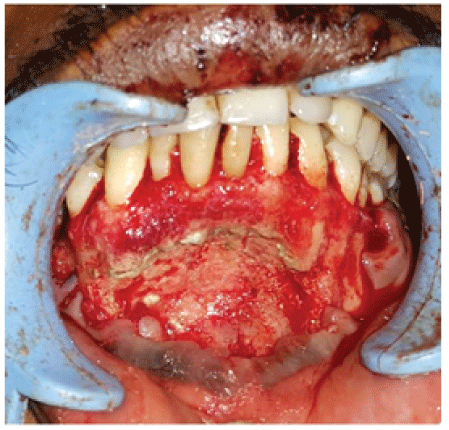
Figure 9: MTA retrograde filling
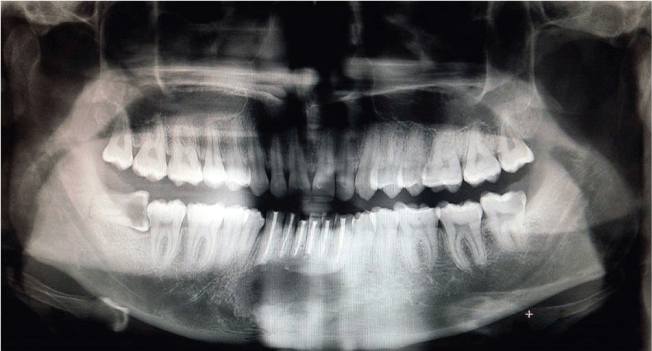
Figure 10: Post operative OPG after 6 months
The pathogenesis of radicular cyst is initiated by the activation of proliferation of cell rest of malassez by the microbial antigens, endotoxins and the cytokines from the apical foramen of the tooth. Complement fixation and antigen antibody complex formation are the two mechanism involved in the initiation of cell rest proliferation [7]. Later the growth factors like TGF-Beta, IL 1, IL6 and IL8 play an important in fibroblastic proliferation phase of the cell rest to form a periapical granuloma [8]. The two main theories for cyst formation is that the epithelial cell proliferates around the connective tissue surface of the periapical abcess cavity to form cyst or the cyst is formed from the central degeneration of the epithelial proliferations of periapical granuloma [9]. The central cystic degeneration was believed to be from a vascular compromise but later it was proved to be an immunologic reaction causing the epithelial clefts formed by intercellular fluids to collide forming a cavity leading to formation of cyst [10]. The cystic contents are a straw colored fluid with numerous cholesterol crystals formed from degenerated Red blood corpuscles. Histologically the cyst is lined by stratified squamous epithelium the thickness of lining increases with the duration. Hyaline bodies otherwise called as Rushtom bodies which are derived from the degeneration of epithelial lining are also present in radicular cyst [11]. Two types of radicualr cysts are described in literature type in which the epithelial lining is in continuous with the apical foramen and other type in which the epithelial lining is distinctly separated from the apical foramen [12]. The osmolality of the content was 290 ± 14.93 mOsm which is greater than the serum osmolality of 79 ± 4.68 mOsm [13].
Being a self sustaining lesion, former literatures considered conservative management by only root canal treatment sufficient for the treating the radicular cyst [14]. But this theory can be applied for smaller cyst but not to be applied for larger cyst which requires surgical intervention apart from root canal treatment [15]. Thus for knowing the extent of the cyst in the bone and surrounding soft tissue the diagnostic imaging plays an important role. The treatment of radicualr cyst depends upon size, integrity of cystic walls, approximity to vital structure and localisation of lesion [16]. The extent of radicular cyst can be studied by ultrasonography, Orthopantamogram, Compuerised Tomography and Magnetic Resonance Imaging. In this scenario the cost effective option of OPG was chosen which revealed the medial and lateral extent but for the anterio posterior extent, a computerised tomography was necessary to show the extent in axial, coronal and saggital planes and was cost effective than MRI. Other advantages of CT are
The radicular cyst can be managed by marsupialisation alone when it is no associated with periapical region and not associated with teeth otherwise known as Partch I procedure [18]. In larger cysts in atrophic mandible the radicular cyst is treated by marsupialisation to reduce the size of the cyst later followed by enucleation to prevent the pathological fracture and huge post excision deformity Also known as Partch II or Waldron’s procedure [19]. When cyst does not involve the teeth and occur as a residual cyst in edentulous area enucleation is done. When the cyst is involving the periapical region of the teeth and the teeth are salvageable, radicular cysts are treated by enucleation followed by periapical surgery [20].
The indications of periapical surgery are
The periapical surgery or root end surgery is the term used to procedure where root canal treatment to the involved teeth is done and after enucleation of the cyst, 3mm the apical portion of the root are resected [22] and after the periapical preparation which extend about 3mm into the root canal a biocompatible and well sealing material is filled using the retrograde approach using ultrasonic tips and specialised instruments [23]. The best material used for periapical restoration after apicocectomy is MTA – mineralised trioxide Aggregate when compared with intermediate restorative material and Amalgam [24]. The following are the advantages of the MTA.
The recent advances like using methylene blue application over the root after resection to stain the organic material of the cystic lining and the predominantly inorganic root portion is no stained by the solution is advocated [26]. After the invention of operative microscope to dentistry the micro endodontic surgery provides various advantage of accurate flap design, less bone removal for exposure, accurate root resection and periapical restoration without any spills of the radio opaque filling material [27].
Thus our current case was managed with enucleation followed by apicoectomy and retrograde filling of the root canal with MTA. This successfully managed case scenario highlights that Computerized Tomography is an irreplaceable tool for diagnosing maxillofacial lesions for its advantages like cost effectiveness, short duration procedure, reproducibility and patient friendly and higher resolution than orthopantamogram.
Download Provisional PDF Here
Article Type: Case Report
Citation: Kumar ND, Sherubin JE, Jose M, Swaminathan C (2017) Surgical Management of Large Radicular Cyst in Mandible. Int J Dent Oral Health 3(3): doi http://dx.doi.org/10.16966/2378-7090.236
Copyright: © 2017 Kumar ND, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Publication history:
All Sci Forschen Journals are Open Access